Functions
• Special visceral efferent (SVE). Branchial motor to stylopharyngeus muscle.
• General visceral efferent (GVE). Visceral motor (parasympathetic) to the parotid gland (via lesser superficial petrosal nerve, LSPN).
• General sensory afferent (GSA). Somatic sensory from posterior external ear, tragus, posterior one third of the tongue, soft palate, nasopharynx, tympanic membrane, eustachian tube, and mastoid region.
• Visceral afferent (VA). Visceral sensory from carotid body (O2, CO2 chemoreceptors) and carotid sinus (baroreceptors) .
• Special afferent (SA). Special sensory for taste from posterior one third of tongue.
Anatomy
• The glossopharyngeal nerve leaves the medulla between the olive ventrally and the inferior cerebellar peduncle dorsally (postolivary sulcus) as the most rostral three to five of the group of rootlets that will form cranial nerve (CN) IX, X, and the cranial root of XI (Figs. 9.1, 9.2, 9.3). In its short (~15 mm) subarachnoid course, it traverses the cerebellomedullary cistern. The nerve sends off a tympanic branch (tympanic nerve or Jacobson nerve) to the middle ear before exiting the skull through the jugular foramen. In the jugular foramen, it lies anterior (in the pars nervosa) to CNs X and XI (which lie posterior in the pars vascularis). The superior and inferior (petrosal) glossopharyngeal ganglia are located in the jugular foramen. The nerve exits the jugular foramen posteromedial to the styloid process, then descends lateral to the pharynx between the internal carotid artery (ICA) and IJV (internal jugular vein) in the carotid space. It supplies the stylopharyngeus muscle and then penetrates the pharyngeal constrictor muscles (above the level of the middle constrictor) to reach the posterior aspect of the tongue.
• Tympanic nerve (Jacobson’s nerve) (parasympathetic + sensory). Parasympathetic innervation of parotid gland and sensory information from tympanic membrane and eustachian tube. The tympanic nerve arises from the inferior ganglion within the jugular foramen and reaches the tympanic cavity through a small canal (inferior tympanic canaliculus) on the undersurface of the petrous temporal bone. There it divides into branches that, together with the superior and inferior caroticotympanic nerves (from the ICA sympathetic plexus), create the tympanic plexus. The tympanic plexus in turn gives off (1) the LSPN; (2) a branch to join the greater superficial petrosal nerve (GSPN); and (3) sensory branches to the mucous membranes of the tympanic cavity, mastoid air cells and eustachian tube.
• Motor branch to stylopharyngeus muscle.
• Carotid sinus nerve (Hering’s nerve). To carotid sinus and carotid body (visceral sensory).
• Pharyngeal branches. To oro- and nasopharynx.
• Tonsillar branches. To palatine tonsil and soft palate.
• Lingual branch. To posterior one third of the tongue (sensory and taste).
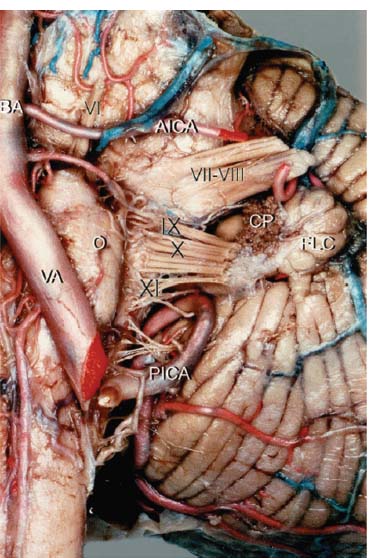
Fig. 9.1 Anterior view of the left cerebellopontine angle showing the origin of CN IX at the postolivary sulcus of the medulla. (AICA, anterior inferior cerebellar artery; BA, basilar artery; CP, choroid plexus; FLC, flocculus; PICA, posterior inferior cerebellar artery; O, olive; Roman numerals, cranial nerves; [VA], vertebral artery.) (From Ozveren MF, Ture U, Ozek MM, et al. Anatomic landmarks of the glossopharyngeal nerve: a microsurgical anatomic study. Neurosurgery 2003;52:1400–1410. Reprinted with permission.)
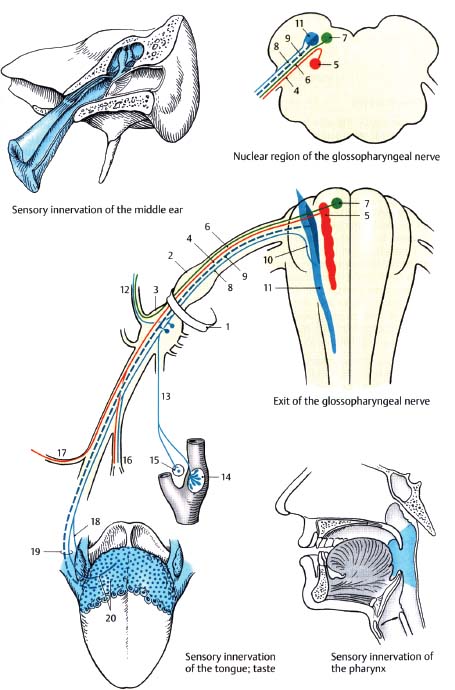
Fig. 9.2 Glossopharyngeal nerve. (1, jugular foramen; 2, superior ganglion; 3, inferior [petrosal] ganglion; 4, branchial motor fibers; 5, nucleus ambiguus; 6; parasympathetic fibers; 7, inferior salivatory nucleus; 8, visceral sensory fibers; 9, special sensory fibers [taste]; 10, tractus solitarius; 11, nucleus solitarius; 12, tympanic nerve; 13, carotid sinus nerve [of Hering]; 14, carotid sinus; 15, carotid body; 16, pharyngeal branches; 17, nerve to stylopharyngeus muscle; 18, tonsillar branches; 19, lingual branches; 20, taste fibers.)
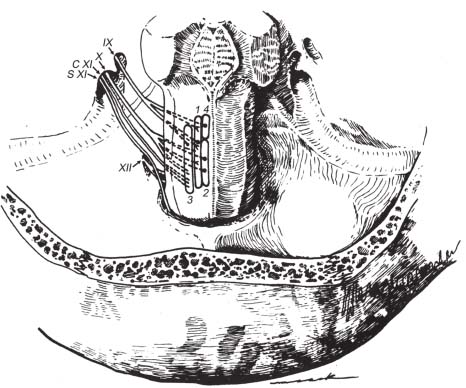
Fig. 9.3 Origin and cisternal courses of glossopharyngeal, vagus, spinal accessory, and hypoglossal nerves. Note that the glossopharyngeal nerve is made up of three to five rootlets (only two shown on this schematic). The glossopharyngeal nerve passes through the more anterior part of the jugular foramen (pars nervosa), whereas the vagus and spinal accessory nerves pass through the posterior part (pars vascularis). The hypoglossal nerve passes through the more inferiorly located hypoglossal canal. (1, nucleus solitarius; 2, dorsal motor nucleus of X; 3, nucleus ambiguus; 4, superior salivatory nucleus; C XI, cranial root of CN XI; S XI, spinal root of CN XI.) (From Harnsberger HR. Handbook of Head and Neck Imaging (2nd ed.) St. Louis, MO: Mosby, 1995. Reprinted with permission.)
Distinct Branches of the Glossopharyngeal Nerve (Fig. 9.4)

Fig. 9.4 Schematic drawing demonstrating the portions and branches of the glossopharyngeal nerve. (From Ozveren MF, Ture U, Ozek MM, et al. Anatomic landmarks of the glossopharyngeal nerve: a microsurgical anatomic study. Neurosurgery 2003;52:1400–1410. Reprinted with permission.)
Functional Pathways of the Glossopharyngeal Nerve
• The glossopharyngeal nerve is complex, supporting five separate functions with a complex anatomical course. It is helpful to think of each pathway and its associated anatomy separately as detailed here.
• SVE (branchial motor) pathway. The rostral portion of the nucleus ambiguus (in medulla) innervates the stylopharyngeus muscle and part of the superior pharyngeal constrictor.
• GVE (visceral motor) pathway. Parasympathetic preganglionic fibers from the inferior salivatory nucleus in the rostral medulla travel with CN IX and join the tympanic nerve to enter the tympanic plexus (no synapse here), from which the LSPN arises. The LSPN reenters the cranium through a small canal in the petrous temporal bone lateral to the canal for the GSPN, then travels back out through the foramen ovale to synapse in the otic ganglion (below the foramen ovale). Postganglionic fibers then travel with the auriculotemporal nerve (branch of CN V3) to the parotid gland to cause salivation and vasodilation.
• GSA (somatic sensory) pathways. Sensation from the back of the ear, tragus, posterior one third of the tongue, soft palate, oro- and nasopharynx (e.g., for gag reflex) travels via lingual, tonsillar, and pharyngeal branches to the superior ganglion (location of cell bodies of sensory neurons) and then to the caudal spinal trigeminal nucleus. Sensation from the tympanic membrane, eustachian tube, and mastoid region travels via the tympanic plexus to the tympanic nerve to the inferior ganglion to the spinal trigeminal nucleus.
• VA (visceral sensory) pathway.
1. Baroreceptors in carotid sinus. Baroreceptors at the carotid bifurcation sense an increase in blood pressure that travels via the carotid sinus nerve to the inferior (petrosal) ganglion to the tractus solitarius and then to the caudal nucleus solitarius (site of synapse). Interneurons then synapse on the dorsal nucleus of CN X to cause a vagal response (decreased blood pressure and heart rate and force of cardiac contraction) (carotid sinus reflex).
2. Chemoreceptors in carotid body. Carotid body chemoreceptors detect blood O2. and CO2. concentrations, and transmit information via Hering’s nerve to the inferior (petrosal) ganglion to the tractus solitarius and to the caudal nucleus solitarius. Interneurons then synapse on the respiratory center in the medulla to control respiratory rate and depth.
• SA (special sensory) pathway. Taste fibers in the posterior one third of the tongue, posterior pharynx and eustachian tube transmit information to the inferior (petrosal) ganglion to the rostral nucleus solitarius to the reticular formation and via the central tegmental tract to the contralateral thalamic VPM .
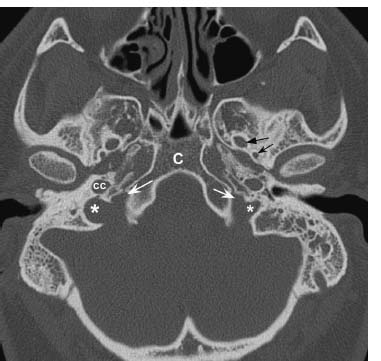
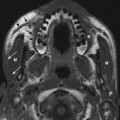
Fig. 9.5 Axial CT image in bone window through the skull base demonstrates normal jugular foramina bilaterally. The jugular vein and CN X and XI exit via the pars vascularis (*). The glossopharyngeal nerves pass through the pars nervosa (white arrows), which is located anteromedially. The right jugular foramen is larger than the left, a typical and normal finding. The normal carotid canals are seen just anteriorly (CC). Note the normal clivus (C), foramen ovale, and foramen spinosum (straight black arrow and concave black arrow, respectively).
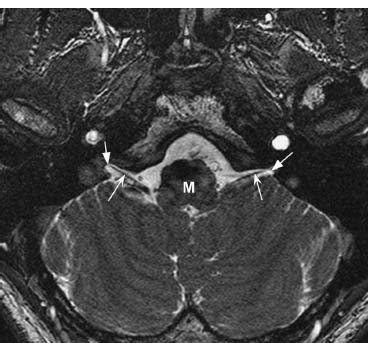
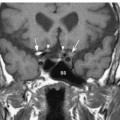
Fig. 9.6 Thin-section axial fast imaging employing steady-state acquisition (FIESTA) image through the skull base demonstrates the cisternal portions of the glossopharyngeal nerves (concave arrows) exiting the dorsolateral medulla (M). The nerves course anterolaterally toward the pars nervosa of the jugular foramina (straight arrows).
Glossopharyngeal Nerve: Normal Images (Figs. 9.5, 9.6)
Glossopharyngeal Nerve Lesions
Evaluation
• Sensory evaluation. Ipsilateral loss of taste over posterior one third of tongue. Loss of sensation over soft palate, posterior one third of tongue, and nasopharynx. Alternatively, otalgia due to referred pain along the tympanic branch to the ear may be observed.
• Motor evaluation. Usually no obvious deficit results from loss of Stylopharyngeus function; however, mild dysphagia may occur.
• Reflex evaluation.
 Gag reflex. Light touch to pharynx, tonsillar area, or base of tongue should lead to gagging (tongue retraction along with elevation and constriction of pharyngeal muscles). Afferent arc is CN IX sensory (pharynx) to caudal nucleus solitarius. Efferent arc is nucleus ambiguus via CN IX/X to pharyngeal muscles.
Gag reflex. Light touch to pharynx, tonsillar area, or base of tongue should lead to gagging (tongue retraction along with elevation and constriction of pharyngeal muscles). Afferent arc is CN IX sensory (pharynx) to caudal nucleus solitarius. Efferent arc is nucleus ambiguus via CN IX/X to pharyngeal muscles.
 Palatal reflex. Light touch to soft palate should lead to ipsilateral deviation of the uvula and elevation of the soft palate (swallowing reflex). Afferent arc is CN IX sensory and efferent arc is nucleus ambiguus to CN X to palatal and pharyngeal muscles.
Palatal reflex. Light touch to soft palate should lead to ipsilateral deviation of the uvula and elevation of the soft palate (swallowing reflex). Afferent arc is CN IX sensory and efferent arc is nucleus ambiguus to CN X to palatal and pharyngeal muscles.
• Autonomic evaluation. Ipsilateral alteration in parotid salivation (difficult to test). Carotid sinus nerve dysfunction may lead to tachycardia/bradycardia and/or hypotension.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree