How to Image the Hips and Pelvis
See the hip and pelvis protocols at the end of the chapter.
- •
Coils and patient position: Generally, when evaluating the hips for entities such as avascular necrosis (AVN) or fractures, it is possible in many patients to use a torso phased array coil. For larger patients, the body coil is necessary. Both hips and the entire pelvis are imaged simultaneously for most clinical indications. The patient is placed supine in the magnet. For evaluation of smaller structures in the hip joint, such as the labrum or cartilage, a surface coil, such as a flexible wrap coil, is recommended, and then only the symptomatic hip is evaluated with thinner slice thickness and smaller interslice gap. The addition of intra-articular contrast material, such as a dilute gadolinium solution, is helpful for additional evaluation of the labrum.
- •
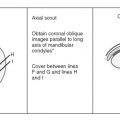
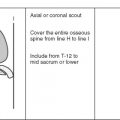
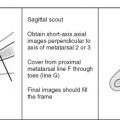
Image orientation ( Box 14-1 ): The most useful information for evaluating hip pathology can be obtained in the axial and coronal planes. Sagittal images sometimes can be difficult to interpret because the fovea centralis may mimic pathology, and these images generally give no additional information. For evaluation of labral tears and femoroacetabular impingement, oblique coronal and oblique axial images are helpful.
BOX 14-1
Structures to Evaluate in Different Planes
Coronal
- •
Osseous structures
- •
Acetabulum
- •
Femoral head, neck
- •
Greater, lesser trochanter
- •
Sacrum
- •
Ilium
- •
Sacroiliac joints
- •
- •
Muscles
- •
Gluteal muscles
- •
Adductors
- •
Abductors
- •
Hamstrings
- •
Quadriceps
- •
- •
Labrum
- •
Pulvinar
Axial
- •
Osseous structures
- •
Acetabulum
- •
Femoral head, neck
- •
Greater, lesser trochanter
- •
Sacrum
- •
Ilium
- •
Sacroiliac joints
- •
- •
Muscles
- •
Gluteus maximus, medius, and minimus
- •
Sartorius, rectus femoris
- •
Gracilis, pectineus, adductor longus, brevis, and magnus
- •
Tensor fascia lata
- •
Piriformis
- •
Obturator internus, externus
- •
Gemelli superior and inferior
- •
Quadratus femoris
- •
- •
Labrum
- •
Pulvinar
Sagittal
Not standard or necessary to perform
- •
- •
Pulse sequences and regions of interest: A large field of view (24-30 cm) is necessary when evaluating both hips and the pelvis simultaneously, as is done for AVN or trauma. Especially in the setting of trauma, the entire osseous pelvis should be evaluated. We routinely scan from the iliac crest to the lesser trochanter. To scan the pelvis in a timely fashion, a slice thickness of 6 or 7 mm with an interslice gap of about 3 mm is reasonable. When assessing joint pathology, such as labral detail, a smaller field of view is recommended (14-24 cm), with a smaller slice thickness. We have found that 3-mm slice thickness with a 10% interslice gap (0.3 mm for those who do not wish to do the math) is satisfactory. The coverage for a dedicated hip MRI examination should include the supra-acetabular location through the bottom of the lesser trochanter. A T1W sequence is necessary for showing anatomic detail. Some type of T2W image in the same planes also is recommended. T2W images show edema or fluid that may not be appreciated on T1W images. Fast spin echo T2W images with fat suppression and (fast) STIR images show fluid and edema with increased conspicuity compared with other types of T2 sequences.
- •
Contrast: Intravenous contrast administration is generally unnecessary except to differentiate a cystic from a solid mass. Intra-articular contrast administration is of great benefit, however, when assessing labral pathology. The dilution technique is the same as for the shoulder or any other joint. A 1/200 dilution of gadolinium in normal saline is injected into the joint after confirmation with a small amount of radiopaque contrast material. The high signal contrast (gadolinium) compared with the low signal labrum makes identification of tears easier. Additionally, we recommend fat suppression with T1W and T2W images after intraarticular contrast injection to make the gadolinium more conspicuous.
Normal and Abnormal
OSSEOUS STRUCTURES
Osseous and ligamentous structures and the musculotendinous components help to characterize and constrain the dynamic movements of the hip. The hip is important in the transfer of weight and energy between the appendicular and axial skeleton but is crucial in the execution of lower limb motion, such as walking, running, jumping, and kicking. Despite its importance in everyday maneuvers, the hip is less understood than other joints.
Normal Osseous Structures
The hip is a ball-and-socket joint, allowing for considerable motion with flexion and extension, internal and external rotation, and abduction and adduction. The acetabulum covers 40% of the femoral head and is formed from ilium, ischium, and pubic bones. At birth, these three bones are separated by the triradiate cartilage, a Y-shaped physeal plate. The acetabulum is tilted anteriorly, which explains the greater potential for flexion of the hip compared with extension. Because of the concave shape of the acetabulum, the hip is inherently stable. The depth of the acetabulum is increased by the dense fibrocartilaginous labrum that surrounds it. The combination of the labrum and transverse acetabular ligament makes a complete ring around the acetabulum.
The femur is the longest and strongest bone in the body. The proximal femur comprises a head, neck, and greater and lesser trochanters. The femoral head is spherical in shape, but is slightly flattened anteriorly and posteriorly. With the exception of the fovea, it is covered by articular cartilage that ends approximately at the level of the epiphyseal plate at the femoral head-neck junction. The fovea is seen as an indentation in the normal round contour of the femoral head on its medial aspect and is the site of attachment of the ligamentum teres.
The trochanters are apophyses, which add to the width of bone. The greater trochanter serves as the insertion site for the tendons of the gluteus medius and minimus, the obturator internus and externus, and the piriformis muscles. The lesser trochanter receives the iliopsoas tendon ( Fig. 14-1 ).

The bone marrow of the pelvis and hips is generally diffuse or patchy intermediate signal (but higher signal than muscle on T1W images) because of the large amount of red marrow that persists in this region throughout life. The epiphyses and apophyses should have high signal fatty marrow on T1W images. Occasionally, a small rim of red marrow may parallel the subchondral bone of the femoral epiphysis; this is considered normal. Thick stress trabeculae in the femoral neck (calcar) can be seen as low signal lines on MRI, as can linear physeal scars at the femoral head-neck junction.
Vascular Abnormalities of Bone
Osteonecrosis (Avascular Necrosis) ( Box 14-2 ).
One of the major indications for MRI of the hip is for detection of osteonecrosis of the femoral head. The presumed mechanism of mechanical failure of the femoral head is accumulated stress fractures of necrotic trabeculae that are not repaired. MRI is capable of detecting the early stages of ischemic necrosis, which is important clinically so that therapy can be instituted before the onset of femoral head collapse, fragmentation, degenerative change, and hip replacement. Early diagnosis can lead to joint-sparing techniques, such as core decompression, rotational osteotomy, or free vascularized fibular graft.
Cause
- •
Trauma
- •
Steroids
- •
Hemoglobinopathies
- •
Alcoholism
- •
Pancreatitis
- •
Gaucher’s disease
- •
Radiation therapy
- •
Idiopathic
MRI
- •
Diffuse edema (low T1, high T2) early
- •
Focal serpiginous low signal line with fatty center (most common appearance)
- •
Double-line sign
- •
Focal subchondral low signal lesion on T1 with variable signal on T2
Location
- •
10-o’clock to 2-o’clock position on coronal images
- •
Anterior femoral head affected first
Numerous causes of AVN have been cited, including trauma, steroids, hemoglobinopathies, alcoholism, pancreatitis, Gaucher’s disease, and radiation. AVN is considered idiopathic when no cause can be identified. Anabolic and catabolic steroid use can result in AVN.
AVN is bilateral in 40% of hips, so both hips should be imaged simultaneously for this indication. The classification scheme for AVN observed on radiographs cannot be used for MRI. MRI is most useful when plain films are negative. MRI also is more sensitive than computed tomography (CT) or radionuclide bone scintigraphy. Additionally, MRI can provide information regarding articular cartilage, marrow conversion, joint fluid, and associated insufficiency fractures, which also are common in patients taking steroids.
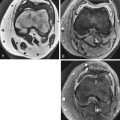
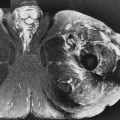
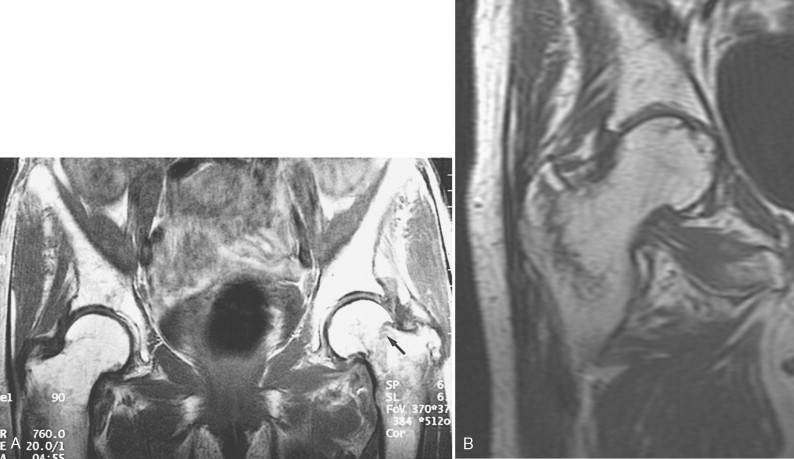
The appearance of AVN on MRI includes a diffuse pattern of bone marrow edema early (similar in appearance to transient bone marrow edema), subsequently becoming more focal in the femoral head; a serpiginous line of low signal intensity surrounding an area of fatty marrow in the femoral head between the 10-o’clock and 2-o’clock positions on coronal images (usually anterior in the femoral head) is characteristic for AVN ( Figs. 14-2 and 14-3 ). This is the typical geographic pattern of AVN that is seen most often. Collapse of bone and sclerosis may result in a focal area of low signal on T1W images that is variable signal on T2W images ( Fig. 14-4 )—in other words, not a fatty center. This latter appearance is uncommon and is less specific than the geographic pattern.



On spin echo T2W images, the “double-line sign” has been described as an appearance typical of ischemic necrosis. The double line is a line of low signal that surrounds an inner line of high signal on spin echo T2W images. The double-line sign represents a chemical shift artifact and is not currently seen with the updated high field MRI scanners because of the spectral presaturation fat suppression that is always applied with the T2W FSE/TSE sequences to eliminate the high signal of the fatty tissue. MRI signal abnormalities such as the double-line sign initially were thought to be helpful in staging osteonecrosis because they corresponded to histologic findings ; however, because the prognostic significance is unclear, staging based on signal characteristics generally is not recommended.
Important additional findings necessary to report to the clinician include the volume of the head that is involved with AVN; this is best determined with axial imaging. Additionally, findings of degenerative disease, such as joint space narrowing and osteophytes, are important to report because this helps with staging of the disease. Similarly, it is important to report collapse of the femoral head (see Fig. 14-4 ). The presence and amount of a joint effusion often correspond to the severity of clinical pain symptoms.
Misinterpretation of osteonecrosis may occur if one is unfamiliar with a few potential pitfalls ( Box 14-3 ). Occasionally, normal hematopoietic marrow can be identified in the femoral head. The signal intensity of hematopoietic marrow is higher in signal than AVN on T1W images. A synovial herniation pit, which represents a tiny defect in the bone that allows joint fluid to fill this space (analogous to a subchondral cyst, but removed from the articular surface), can erroneously be interpreted as an area of AVN ( Fig. 14-5 ). The fovea centralis, a normal anatomic finding, inadvertently may be diagnosed as a site of AVN with subchondral collapse ( Fig. 14-6 ). Subchondral cysts from degenerative joint disease of the hip may appear similar to AVN, but the low signal margins of the cyst are smooth and regular, rather than serpiginous as with AVN. Also, abnormalities on both sides of the joint usually are present, with evidence of degenerative cysts and degenerative cartilage loss and osteophytes. Metastases occasionally may have an appearance similar to AVN that is diffusely low signal on T1W images.
- •
Hematopoietic marrow
- •
Synovial herniation pit
- •
Fovea centralis


Legg-Calvé-Perthes disease is an idiopathic AVN of the growing femoral epiphysis that results in a progressive deformity and outward displacement of the femoral head; it occurs in children 4 to 10 years old ( Box 14-4 ). MRI has been reported to be useful for assessing Legg-Calvé-Perthes disease. Diffuse low signal in the femoral head on T1W and T2W images is the most common finding. Collapse of the femoral epiphysis also can occur. Jaramillo and associates showed that physeal bridging and deformity of the femoral head with abnormal low signal in the head on MRI were statistically significant predictors of growth arrest. Abnormalities of the epiphysis did not relate to growth arrest. Depiction of physeal bridging at MRI was the best predictor of growth arrest in their study. MRI allows earlier diagnosis and diagnosis of coexistent contralateral disease and monitoring of therapy ( Figs. 14-7 and 14-8 ).
- •
Idiopathic avascular necrosis of femoral head
- •
Age 4-10 years
- •
May lead to growth arrest
- •
MRI findings: Diffuse low signal on T1W and T2W images ± collapse of femoral head
- •
MRI predictors of growth arrest
- •
Physeal bridging
- •
Signal change in physis/metaphysis
- •


Idiopathic Transient Osteoporosis of the Hip (Transient Painful Bone Marrow Edema) ( Box 14-5 ).
Idiopathic transient osteoporosis of the hip (ITOH) also has been referred to as transient painful bone marrow edema . The first well-documented description was reported in three women during the last trimester of pregnancy. ITOH is an uncommon and usually self-limited clinical entity of unknown cause that primarily affects middle-aged men (40-55 years old). Although the underlying cause is uncertain, a vascular basis almost certainly exists. When women are affected, it is usually during the third trimester of pregnancy. There are anecdotal reports of ITOH occurring in early pregnancy with resolving hip pain after spontaneous or therapeutic abortions. The male-to-female ratio is 3:1. This condition is rare in children, and there are no known predisposing factors except pregnancy. Generally, only one hip is affected at a time. Recurrence in the same hip can occur. This entity is known as regional migratory osteoporosis when it migrates to other joints.
- •
Middle-aged men
- •
Pregnant women
- •
Male-to-female ratio 3 : 1
- •
No history of trauma
- •
Spontaneous resolution (6-8 mo)
- •
MRI: Low T1 signal; high T2 signal femoral head to intertrochanteric region
- •
Differential diagnosis: Septic hip, avascular necrosis (early), osteoid osteoma (younger age group)
Clinically, patients present with disabling pain without a history of trauma. Conventional radiography shows osteopenia isolated to the affected hip. It is important to make the proper diagnosis so that correct treatment can be instituted. ITOH generally resolves spontaneously in 6 to 8 months after protected weight bearing and symptomatic support. Insufficiency fractures of the hip may occur without protected weight bearing because of the severity of the localized osteoporosis. MRI in ITOH shows decreased signal on T1W images and increased signal on T2W images extending from the femoral head to the intertrochanteric region ( Fig. 14-9 ). These findings have been attributed to bone marrow edema. The signal intensity in the acetabulum is normal. These characteristics have been reported within 48 hours after the onset of symptoms of ITOH.

Because early AVN can have a similar appearance on imaging, and the treatments are different, it is important to differentiate ITOH from AVN. There is some controversy as to whether ITOH represents a very early, reversible stage of AVN. VandeBerg and colleagues developed criteria to increase sensitivity and specificity of irreversible changes of ITOH that would lead to a diagnosis of AVN. They suggested that the absence of a subchondral low signal intensity on T2W images or postcontrast T1W images suggests a favorable outcome (reversible disease). The presence of a low signal subchondral area measuring more than 4 mm in thickness and greater than 12.5 mm in length on T2W images or postcontrast T1W images suggests an irreversible lesion (AVN). An intra-articular osteoid osteoma of the hip can cause marrow edema in a similar distribution as ITOH, and a cortically based, small, round lesion should be carefully searched for to exclude this; however, different age groups generally are affected by these two disease processes. Infection of the proximal femur with a septic joint also should be considered in the differential diagnosis based on the MRI appearance.
Fractures ( Box 14-6 )
Fatigue Fractures.
Stress fractures occur commonly around the hips and in the pelvis. Stress fractures are divided into fatigue fractures and insufficiency fractures. Fatigue fractures result from increased or abnormal stress applied to normal bone. MRI is superb for evaluating this abnormality and may be positive when conventional radiography is negative. Bone scintigraphy is sensitive but not specific for stress fractures or stress reactions. MRI is sensitive and specific because it can show the linear fracture or marrow edema from a stress reaction ( Figs. 14-10 to 14-12 ). Because of the exquisite contrast and intrinsic spatial resolution of MRI, this abnormality can be diagnosed early, leading to early appropriate treatment.
- •
Stress fractures—abnormal stress across normal bone
- •
Insufficiency fractures—normal stress across abnormal bone
- •
Femoral neck
- •
Sacrum
- •
Supra-acetabular
- •
Pubic bones, superior and inferior pubic rami
- •
- •
MRI appearance
- •
Linear low signal T1 with low signal edema
- •
Increased signal (edema) T2 with linear low signal (fracture line)
- •
- •
Salter fracture of the hip—medial, inferior, posterior slip of femoral head
- •
Widened physis with edema
- •



Stress reactions occur typically in the femoral neck along the medial aspect (compressive surface) or the superior lateral surface (tensile surface). Additional locations of stress fractures in the pelvis include the pubic rami (superior and inferior) and sacrum. Sacral stress fractures are most often seen in athletes, especially runners. Patients often present with low back pain, and lumbar spine MRI is ordered. The sacrum should be evaluated for this abnormality. The diagnosis can be overlooked because the bone marrow edema may not be conspicuous on non–fat-suppressed T2W images ( Fig. 14-13 ). Stress fractures image as linear low signal surrounded by bone marrow edema.

Insufficiency Fractures.
Insufficiency fractures may occur in osteoporotic patients. These are fractures that occur from physiologic stresses on bone weakened by osteoporosis. In the clinical setting of a painful hip in an osteoporotic patient (even with no significant history of trauma, and despite the fact that the patient may be able to bear weight), a radiographically occult fracture may exist. MRI is the fastest, most cost-effective, and most sensitive and specific method for making the diagnosis in this setting. A limited MRI examination consisting of coronal and axial images of the entire pelvis using T1W and fat-suppressed T2W sequences can be done to evaluate for this entity. Any marrow sequence would suffice. Sometimes the fracture is more readily appreciated on T1W images, and sometimes T2W images are better, so both are recommended for screening.
MRI shows linear low signal with surrounding bone marrow edema on T1W images ( Fig. 14-14 ). The fracture remains low signal on T2W images, but surrounding bone marrow edema is high in signal intensity. Images of the entire pelvis with larger field of view are recommended because hip pain may be referred from abnormalities outside of the hip, such as sacral insufficiency fractures. Multiple fractures often coexist. The most common locations for insufficiency fractures around the pelvis are subcapital, intertrochanteric, sacral, supra-acetabular, pubic bones, and superior or inferior pubic rami.
A sacral insufficiency fracture has a pathognomonic appearance on MRI. T1W images show linear low signal (representing the fracture), usually paralleling the sacroiliac joint with surrounding bone marrow edema (low signal on T1W images and high signal on T2W images). Generally, the bone marrow edema is confined to the sacral ala with the fracture and does not extend across the midline, unless the fracture is bilateral ( Figs. 14-15 and 14-16 ). If the linear component of the fracture is not evident, the abnormality of the sacral marrow may mimic metastatic disease.


Supra-acetabular insufficiency fractures are reliably diagnosed with MRI by noting a curvilinear (eyebrow-shaped) low signal fracture line that parallels the roof of the acetabulum, accompanied by surrounding bone marrow edema (low signal on T1W images that becomes high signal on T2W images) ( Fig. 14-17 ). These fractures are seen in the same patient population with sacral insufficiency fractures (ie, patients with osteoporosis and especially patients who had previous pelvic radiation, which significantly weakens the bone). The characteristic curvilinear low signal fracture line should be identified, along with the geographic appearance of the bone marrow edema, so that insufficiency fractures are not confused with metastatic disease, which generally has diffuse edema and perhaps an associated soft tissue mass with destruction of the acetabulum.

Insufficiency and fatigue fractures have a predilection for the femoral neck and pubic bones (although they have been reported in the sacrum). Supra-acetabular and sacral fractures are almost exclusively of the insufficiency type in osteoporotic individuals.
Salter Fractures ( Box 14-7 ).
Traumatic epiphyseal slip can occur in skeletally immature individuals as a result of birth trauma or accidental or nonaccidental trauma. If the femoral head ossification center is not mineralized, conventional radiography may suggest developmental dysplasia of the hip (DDH) (owing to lateral displacement of the femoral shaft). A T2W sequence, particularly fast spin echo with fat suppression or (fast) STIR imaging, shows edema and hemorrhage through the physis and is diagnostic of a shear injury.
- •
Age 10-17 years (males), 8-15 years (females)
- •
Male > female
- •
Increased incidence in overweight children
- •
MRI: Widened growth plate with high T2 signal
- •
Epiphyseal slip
- •
Slipped capital femoral epiphysis is predominantly an adolescent occurrence, typically observed in boys 10 to 17 years old and in girls 8 to 15 years old. Boys generally are more frequently affected than girls, and this entity is more common in blacks than whites. The incidence is especially high in overweight children. Proposed causes include adolescent growth spurt, hormonal influences, increased weight, and activity, all of which result in repetitive stresses, resulting in a Salter 1 fracture of the proximal femoral growth plate.
If conventional radiography is equivocal, MRI can be used to assess the relationship of the femoral head and neck. MRI shows a widened growth plate with abnormal high signal on the T2W image through the growth plate, with medial and posteriorly located femoral epiphysis with respect to the metaphysis. On the coronal T1W image, the growth plate appears wider than normal, as evidenced by increased width of the low signal physis ( Fig. 14-18 ). These findings can aid the surgeon with operative planning. An additional important advantage of MRI is its ability to identify early osteonecrosis, which can be seen in 15% of children with this entity.