Abstract
Fetal hydrothorax is an intrathoracic effusion that arises in the fetus, may occur unilaterally or bilaterally, and may be primary or secondary. It constitutes a nonspecific finding, because it generally is the clinical manifestation of subjacent pathology. Primary fetal hydrothorax is a diagnosis of exclusion; there is a wide range of potential etiologies, thus cardiovascular disease, fetal arrhythmias, structural malformations, and chromosomal abnormalities must be excluded. Detailed ultrasound and karyotyping is recommended. Prenatal evolution is variable, with 10% to 20% of isolated hydrothorax resolving spontaneously; mild to moderate effusions may remain stable during pregnancy, presenting a good outcome with postnatal treatment. Invasive fetal therapy for fetal hydrothorax should be reserved for severe isolated cases with high risk of developing hydrops due to mediastinal shift, aiming to reduce the risk of lung hypoplasia. In general, unilateral mild cases are primary abnormalities of the lymphatic drainage system and have good prognosis, while severe cases are associated with a poor prognosis and pleuroamniotic shunting should be offered to improve survival rates.
Keywords
hydrothorax, chylothorax, fetal pleural effusion
Disease
Definition
Fetal hydrothorax (also pleural effusion) is an intrathoracic effusion, which may occur unilaterally or bilaterally. It constitutes a nonspecific finding, since it generally is the clinical manifestation of subjacent pathology. If primary and isolated, it is termed primary fetal hydrothorax , and postnatally chylothorax.
Prevalence and Epidemiology
An uncommon finding, occurring in 1 : 8600 to 1 : 15,000 pregnancies, with male fetuses affected more frequently than female (2 : 1).
Etiology and Pathophysiology
There is a wide range of potential etiologies. Hydrothorax is more commonly part of a more complex disease, and frequently associated with hydrops:
- •
cardiovascular disease (50%) and fetal arrhythmias
- •
structural malformations (25%), particularly pulmonary abnormalities such as congenital cystic adenomatoid malformation (CCAM), bronchopulmonary sequestration (BPS), or congenital diaphragmatic hernia (CDH)
- •
chromosomal defects (6%–17%), most commonly trisomy 21 and Turner syndrome
- •
hematologic conditions (alloimmunization)
- •
infections (toxoplasmosis, rubella, cytomegalovirus, syphilis, herpes, and parvovirus B19)
- •
lung and digestive disorders
- •
metabolic disorders (congenital goiter)
- •
anomalies in the umbilical cord and placenta
The main pathophysiologic consequences of hydrothorax are lung hypoplasia and hydrops due to mediastinal shift, caused by compression of the heart and obstruction of venous return. Additionally, compression of the esophagus may lead to polyhydramnios.
The diagnosis of hydrothorax warrants a thorough investigation of potential causes. Detailed ultrasound (US) and karyotyping, primarily looking for trisomy 21, Turner syndrome, and other aneuploidies, are mandatory. More advanced genetic testing may help in isolated cases, and potential genes associated with the disease have been described. As mentioned, primary hydrothorax is an exclusion diagnosis that can only be confirmed postnatally.
Manifestations of Disease
Clinical Presentation
The diagnosis can be made by identification of isolated fluid effusion surrounding one or both fetal lungs, under variable forms, from a mild unilateral effusion to massive bilateral effusion. A proportion of cases present as fetal hydrops, which may hamper discerning whether hydrothorax was first, and thus the cause of hydrops, or whether it is part of a general problem.
For isolated hydrothorax, when the onset is in the form of a mild pleural effusion, the evolution is hard to predict. Some cases remain stable for the remainder of the pregnancy whereas some evolve to severe hydrothorax. Severe cases virtually always evolve to hydrops.
One of the main concerns is the underlying disease causing the problem. Bilateral effusions, severe hydrothorax with significant lung/mediastinal compression and hydrops constitute poor prognostic signs. Parents must be warned that even in the event of successful prenatal therapy, there remains a risk of underlying potentially severe diseases, which will become evident only after birth. Chylothorax has been associated with mosaicism and various genetic disorders, some of which have recently been described, associated to gene mutations.
Imaging Technique and Findings
Ultrasound.
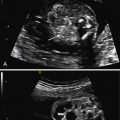
The diagnosis is made based on the presence of free fluid in the thoracic cavity, unilaterally or bilaterally. The lung floats freely in the pleural cavity. In severe cases, the lung is much reduced in size and has a characteristic butterfly appearance, floating in free fluid and moving with the heart beats. Unilateral severe cases present with severe mediastinal shift and compression of the contralateral lung. Defining hydrothorax as mild, moderate, or severe is based on subjective factors including the degree of lung compression and mediastinal shift ( Figs. 4.1 and 4.2 ).


As mentioned, when the diagnosis is first made in the context of fetal hydrops, it is difficult to discern whether the thoracic effusion is the cause or consequence of hydrops.
Magnetic Resonance Imaging.
Magnetic Resonance Imaging (MRI) does not provide additional information in primary fetal hydrothorax, but it may help ruling out associated abnormalities, such as CCAM, BPS, or CDH, where the primary pathology dictates management.
Presence of free fluid surrounding the lung, either unilaterally or bilaterally.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree