INFECTIOUS AND NONINFECTIOUS INFLAMMATORY DISORDERS: SARCOIDOSIS AND INFLAMMATORY PSEUDOTUMOR
KEY POINTS
- Sarcoidosis is a systemic disease that may have more than one type of head and neck presentation, and it may mimic systemic disease such as Sjögren syndrome and lymphoma.
- Sarcoidosis has important intracranial as well as extracranial manifestations, including those of an infiltrating leptomeningeal and pachymeningeal process.
- Inflammatory pseudotumor may occasionally occur outside the orbit and wherever it occurs may mimic malignancy, especially lymphoma.
- Inflammatory pseudotumor is a diagnosis of exclusion whenever biopsy of an infiltrating mass returns “nonspecific granulomatous” or “inflammatory process.”
SARCOIDOSIS
Etiology, Prevalence, Pathologic Diagnosis, and Distribution of the Disease
Sarcoidosis is a systemic disease of unknown etiology. It is likely an immunologic response to a mycobacterial infection, but this is not proven. In such a possible model of pathophysiology, it is can reasonably be considered as an infectious disease or at least a “not obviously” infectious inflammatory disease. There is an inverse relationship to inherent mycobacterial susceptibility and the incidence of sarcoidosis in some ethnic populations.1–3 Depressed T-cell or B-cell function seems to be a predisposing factor in a significant percentage of patients. The disease is most prevalent in the southeastern United States and is most frequently seen in the 20- to 50-year age bracket.
Histopathology in sarcoidosis shows noncaseating granulomas. The diagnosis of sarcoidosis is made clinically by excluding other granulomatous processes while having the appropriately confirmatory laboratory studies, including a positive angiotensin-converting enzyme (ACE) test, Kveim test, and consistent histopathology.2–4 Imaging is supportive in most cases but in some circumstances may be the first study that actually suggests sarcoidosis as a differential possibility because of the gross morphology and anatomic distribution of findings.
Head and neck manifestations of sarcoidosis are common at the time of presentation and may be categorized into nodal and extranodal groups.
Lymphadenopathy
Lymphadenopathy is a prominent component of sarcoidosis in many patients.5 It involves all major cervical groups bilaterally (Fig. 18.1). With adenopathy as the predominant or exclusive head and neck presentation, the disease must be distinguished histopathologically from the other ubiquitous malignant and nonmalignant adenopathies.6
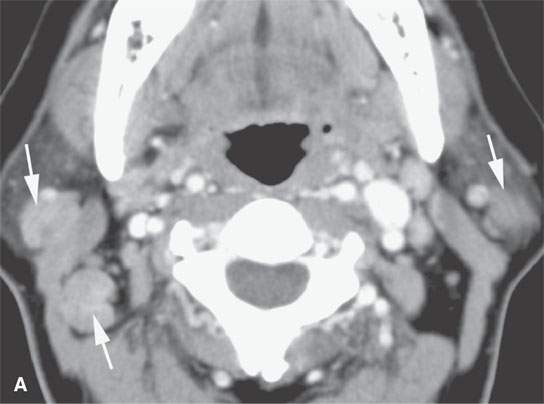
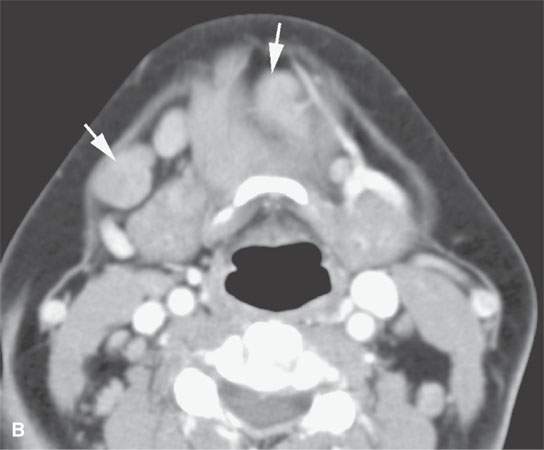
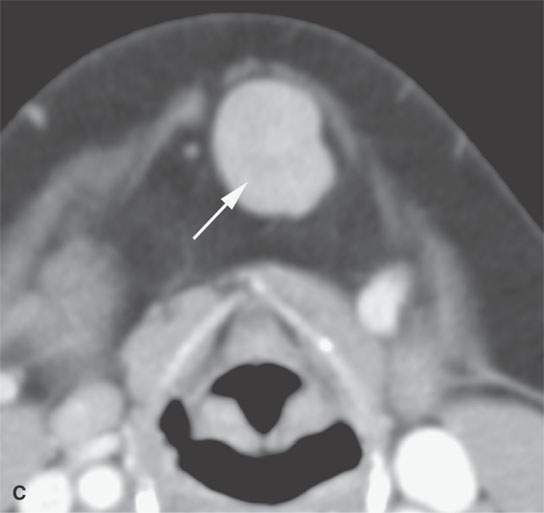
FIGURE 18.1. Contrast-enhanced computed tomography shows that nodes related to sarcoidosis cannot be differentiated from those due to lymphoma or reactive nodes morphologically.
Extranodal Disease
The extranodal manifestations of sarcoidosis are relatively common. Significant numbers of patients have involvement of the visual pathways, including the optic nerve–optic sheath complex, uveal tract and the retina, parotid glands, and lacrimal glands (Fig. 18.2). The glandular changes are virtually always bilateral and roughly symmetric (Figs. 18.3–18.8). Submucosal masses or a more diffuse infiltrative submucosal process may be present anywhere in the upper aerodigestive tract, with the most common area involved being the sinuses and nasal cavity (Fig. 18.9A,B) followed distantly by the larynx and trachea (Fig. 18.10). The sinus disease may manifest as a necrotizing process that cannot be distinguished from Wegener granulomatosis (WG) and angiocentric lymphoma, discussed in Chapter 17, or cases of advanced cocaine abuse (Fig. 18.9C,D).
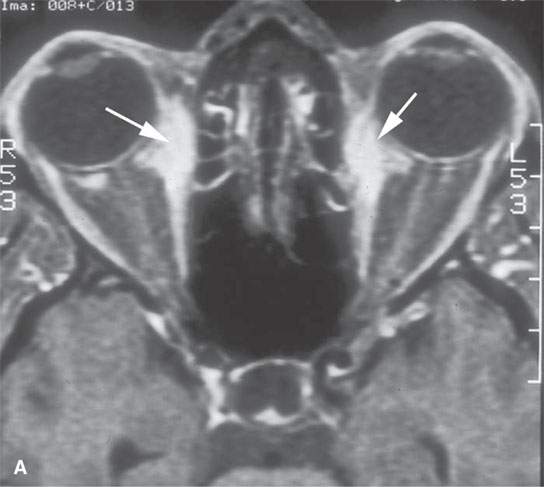
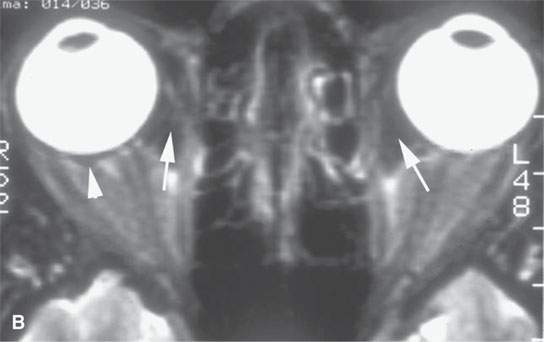
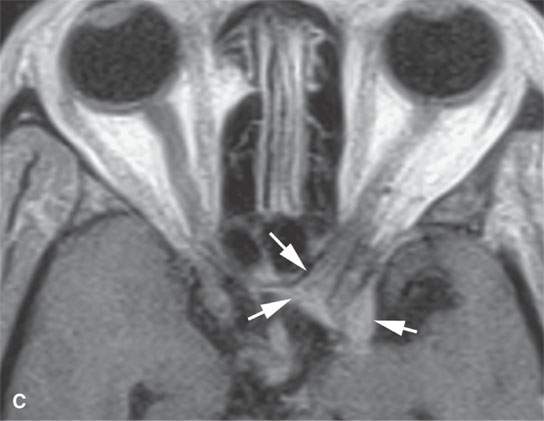
FIGURE 18.2. Contrast-enhanced (CE) magnetic resonance in two patients with an unusual orbital involvement relatively late in the evolution of the disease. CE fat-suppressed T1-weighted (T1W) image (A) shows both intraconal and extraconal enhancement (arrows), and the T2-weighted image (B) shows the process to be lower in signal intensity than muscle (arrows), as is the perisclerotic component (arrowhead), suggesting a fibrous component perhaps related to healing. The second patient presented with orbital apex syndrome, with the CE T1W image in (C) showing meningeal involvement (arrows) at the orbital apex and in the optic canal.
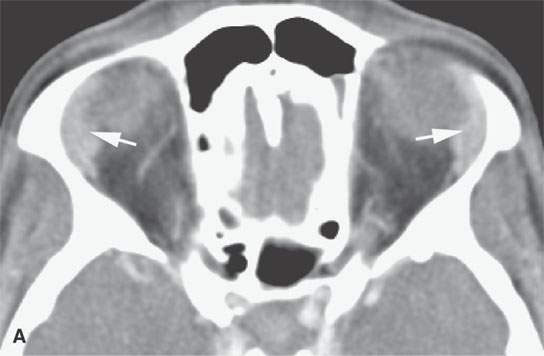
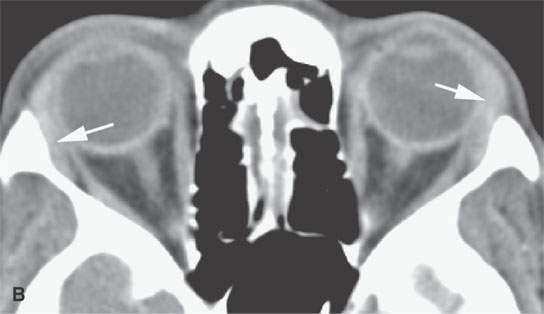
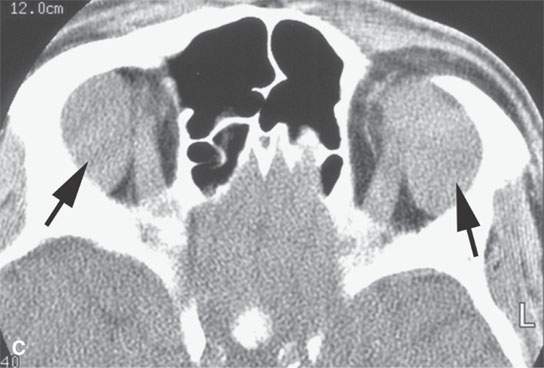
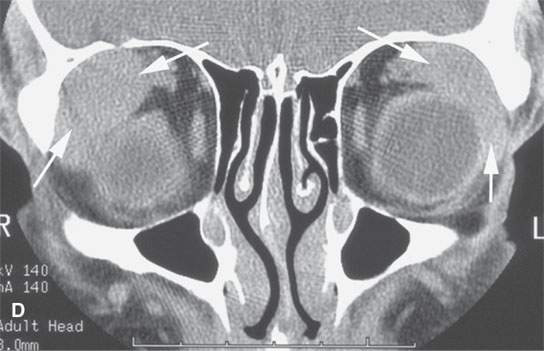
FIGURE 18.3. Contrast-enhanced computed tomography in two patients showing the range of size possible in lacrimal gland sarcoidosis. A, B: Glands are slightly enlarged and enhance slightly (arrows). C, D: Glands are about as large as they get in sarcoidosis(arrows).
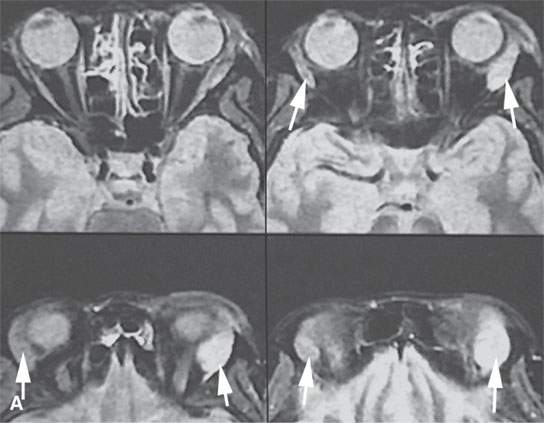
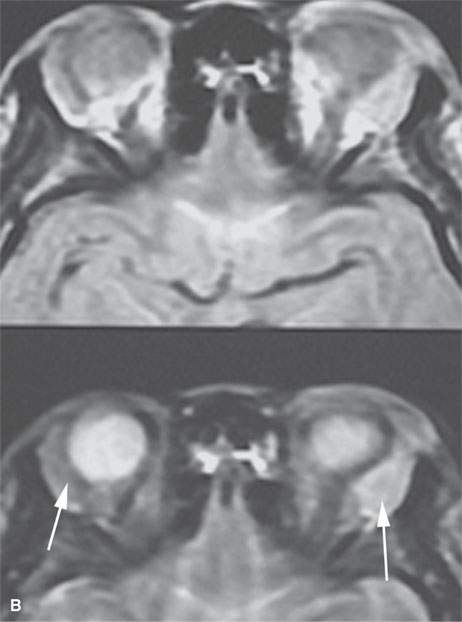
FIGURE 18.4. Magnetic resonance imaging of a patient with lacrimal gland sarcoidosis (arrows). A series of short T1 inversion recovery (STIR) images in (A) show the left gland to be larger and brighter than the right. The density and T2-weighted images in (B) show the left gland to be brighter than the left, although both are involved (arrows).
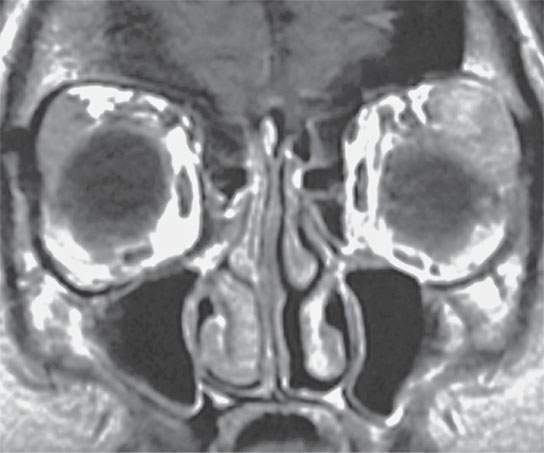
FIGURE 18.5. Contrast-enhanced T1-weighted image showing bilateral lacrimal gland sarcoidosis, but the left gland is large and enhances to the right.
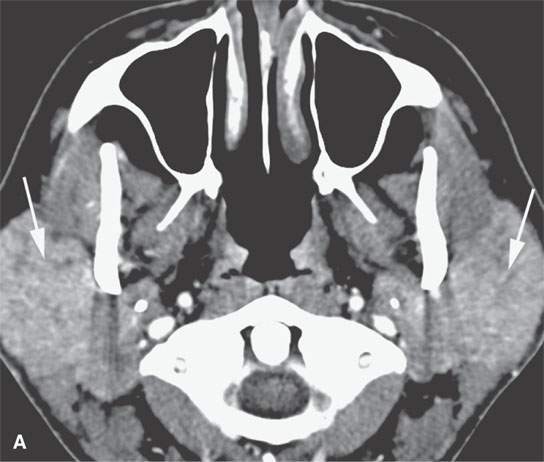
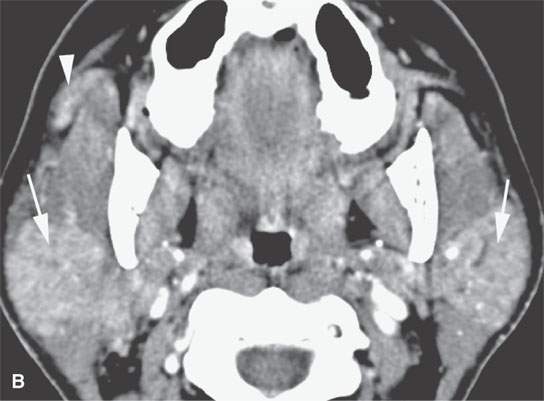
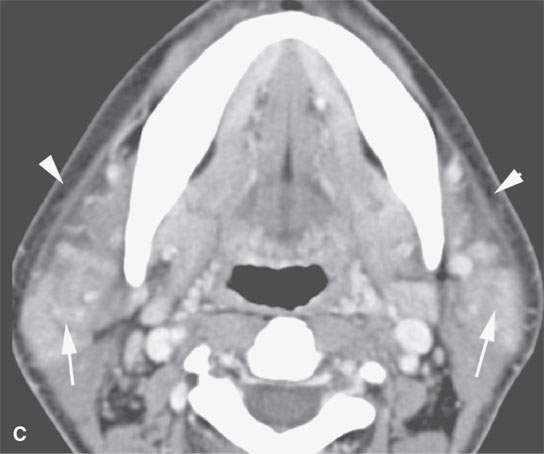
FIGURE 18.6. Contrast-enhanced computed tomography of active parotid sarcoidosis. A:The glands are enlarged bilaterally (arrows), including the accessory lobe on the right (arrowhead in B). The periparotid soft tissue edema (arrowheads in C) is an unusual feature.
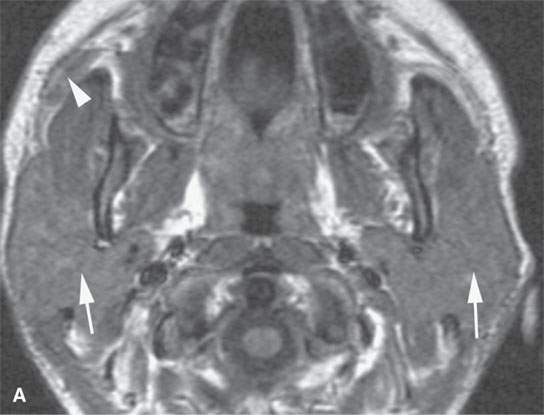
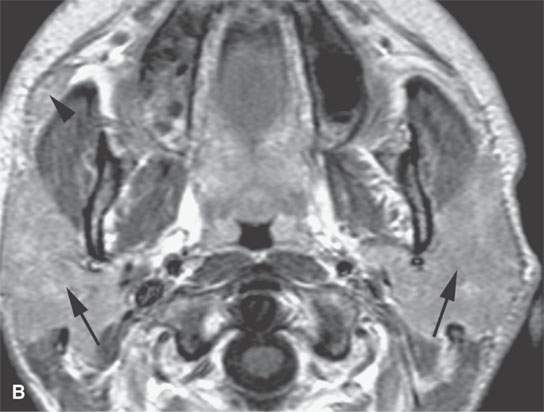
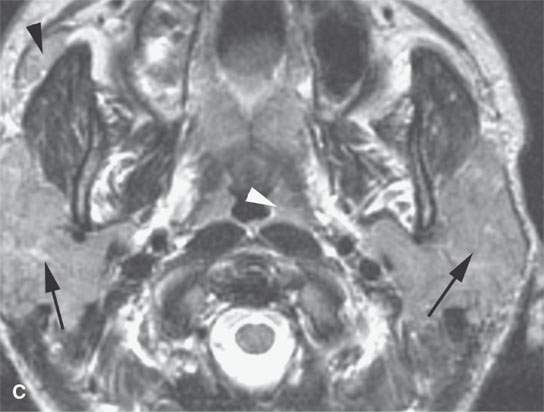
FIGURE 18.7. Non Contrast and contrast-enhanced magnetic resonance of active parotid sarcoidosis. The glands are enlarged bilaterally (arrows), including the accessory lobe on the right (black arrowheads). The enhancement is diffuse (compare the non–contrast-enhanced T1-weighted image in A with the postcontrast T1-weighted image in B). The T2-weighted image in (C) shows the inflamed/infiltrated parotid tissue to be isointense to the lymphoid tissue in the nasopharynx (white arrowhead), speaking to the lack of usefulness of signal intensity changes in differential diagnosis of these noninfectious inflammatory pathologies versus tumor and especially lymphoma.
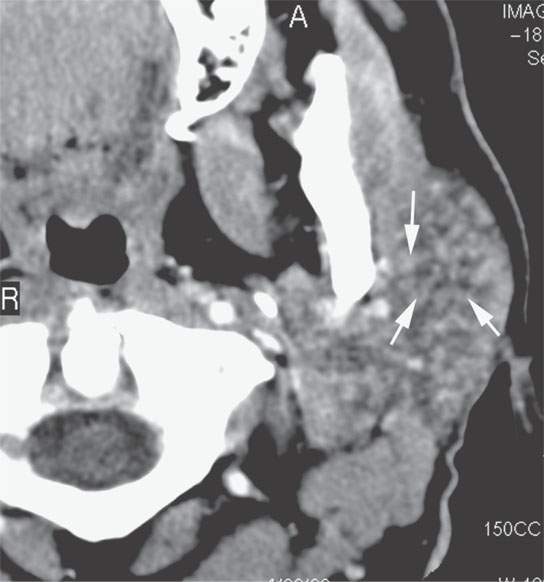
FIGURE 18.8. Contrast-enhanced computed tomography showing a multinodular parotid pattern (arrows) seen in sarcoidosis, as an outlier normal variant and in other diseases such as autoimmune sialoadenitis. This patient actually has Sjögren’s disease.
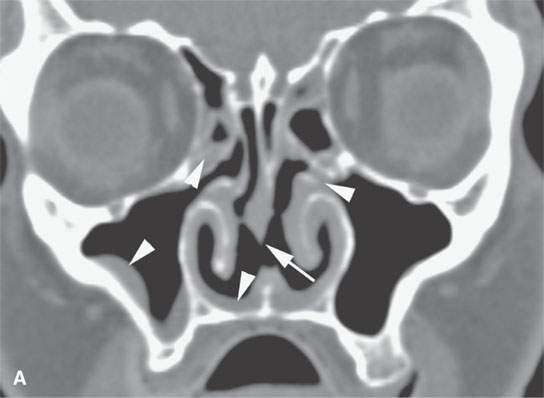
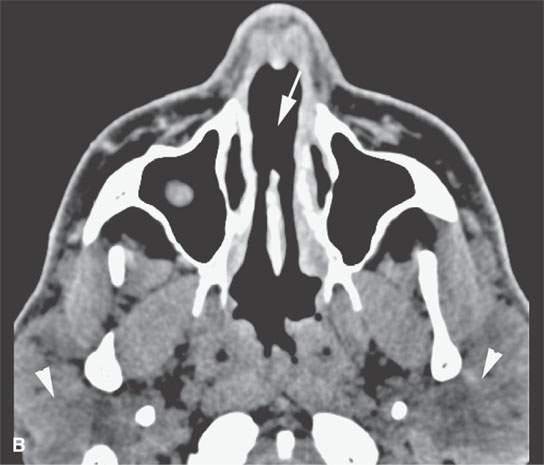
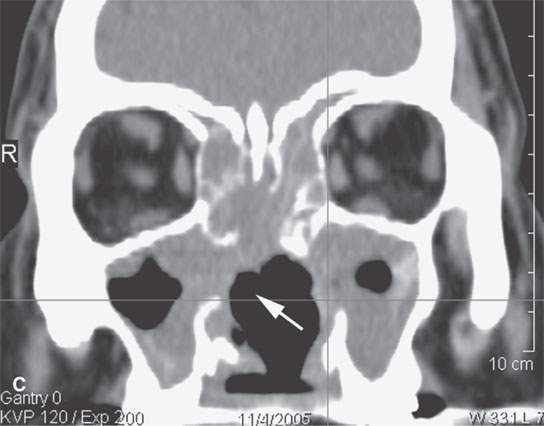
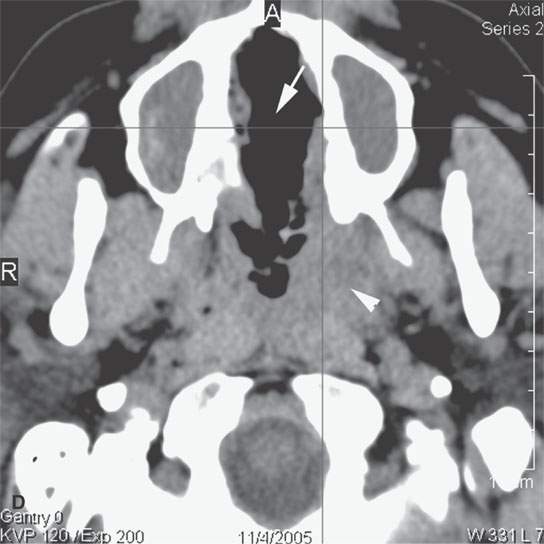
FIGURE 18.9. Sarcoidosis of the nasal cavity and sinuses in (A) and (B) shows septal necrosis (arrow) and mucosal thickening (arrowheads) in a pattern that is indistinguishable from Wegener granulomatosis, angiocentric lymphoma, and advanced changes due to cocaine abuse as shown in (C) and (D) with septal necrosis (arrows), mucosal thickening, and infiltration in the nasopharynx (white arrowhead in D). The parotid enlargement (arrowheads in B) is a clue to the correct diagnosis of sarcoidosis.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








