Etiology, Prevalence, and Epidemiology
Inflammatory pseudotumor, also known as inflammatory myofibroblastic tumor, is a quasineoplastic lesion that clinically and radiologically tends to mimic a malignant neoplasm and that histologically consists of a mixture of inflammatory cells, myofibroblastic spindle cells, and plasma cells. The proportion of the various cells varies considerably from pseudotumor to pseudotumor. Pseudotumors with a predominance of plasma cells are commonly referred to as plasma cell granulomas, and pseudotumors with approximately equal numbers of fibroblasts, and histiocytes are referred to as fibrous histiocytomas.
In most cases the etiology is unknown, although infection, infarcts, and radiation have been implicated as risk factors. Up to a half of pseudotumors demonstrate abnormality at the anaplastic lymphoma kinase receptor tyrosine kinase gene (2p23 locus), suggesting an underlying genetic defect. Organisms found in association with pulmonary inflammatory pseudotumor include various bacteria and Mycoplasma .
Inflammatory pseudotumors are rare. They may affect individuals of any age but have a predilection for children and young adults. They are the most common primary lung mass seen in children.
Pathophysiology
Inflammatory pseudotumors are fibroinflammatory lesions that are believed to result from an exaggerated response to tissue injury. Histologically, they consist of a mixture of inflammatory cells, myofibroblastic spindle cells, and plasma cells. The proportion of these cells varies, but it is believed that the progenitor cell of the various pseudotumors is the myofibroblast. These lesions also are commonly referred to as inflammatory myofibroblastic tumors.
On the basis of the predominant histopathologic features, inflammatory pseudotumors can be divided into three histologic types: (1) focal organizing pneumonia pattern, characterized by small airways and adjacent parenchyma filled with fibroblasts and foamy histiocytes; (2) fibrous histiocytic pattern, characterized by spindle-shaped myofibroblasts arranged in whorls; and (3) lymphohistiocytic pattern, characterized by a mixture of lymphocytes and plasma cells with only minimal fibrous connective tissue.
Manifestations of the Disease
Radiography
The most common radiologic manifestation consists of a solitary peripheral sharply circumscribed lobulated nodule or mass. The lesion may have smooth or spiculated margins and range from 1 to more than 6 cm in diameter ( Fig. 21.1 ). Calcification is present occasionally, particularly in children, and cavitation is present rarely. Endobronchial tumors can cause obstructive pneumonitis and atelectasis. Hilar or mediastinal lymph node enlargement and pleural effusion occur occasionally.

Computed Tomography
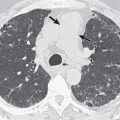
Inflammatory pseudotumors may have smooth or spiculated margins ( Fig. 21.2 ; see Fig. 21.1 ), homogeneous or heterogeneous attenuation, and either no enhancement or variable enhancement after intravenous administration of contrast medium. On computed tomography (CT) the nodules are usually closely associated with a bronchus. Multiple lesions are seen in 5% of cases. Approximately 10% of inflammatory pseudotumors manifest as endobronchial masses. Occasionally, they may be endotracheal.