Introduction to Nuclear Medicine
David K. Shelton
Introduction
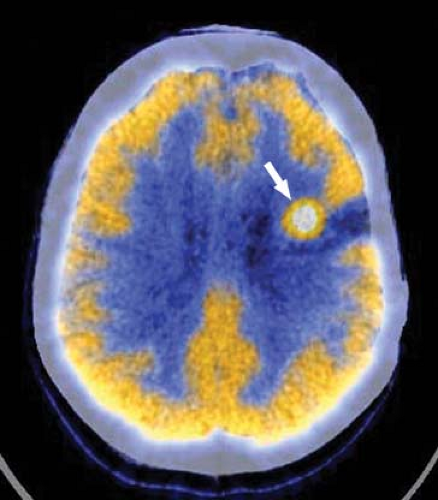
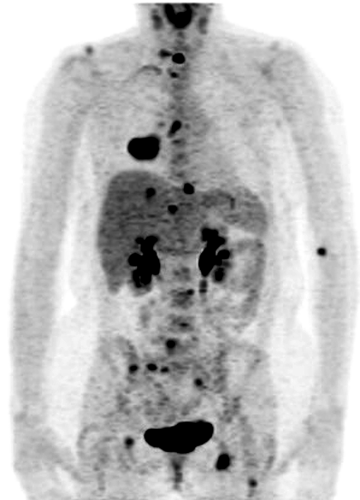
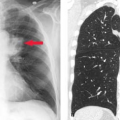
Nuclear medicine encompasses both therapeutic and diagnostic modalities that support practically every field of medical endeavor. Despite changes in referral patterns and the advent of managed care, nuclear medicine studies remain among the most cost-effective for the diagnosis and management of a variety of diseases. Radiographic, ultrasonographic, and MR studies provide high spatial resolution and important anatomic or structural information from which pathologic processes are inferred. On the other hand, nuclear medicine studies provide high functional resolution and provide physiologic and functional information not otherwise available. Anatomic imaging can measure the dimensions of a spot, but functional imaging can show whether it is active and whether it is malignant or not (Fig. 52.1). With this being the decade for advancing functional imaging, many new, important techniques have become commonplace in the clinical environment. PET-CT and now SPECT-CT have improved the sensitivity and specificity for neural, cardiac, and oncological imaging. PET-CT has greatly improved patient throughput, tumor staging, and evaluation of tumor response to therapy (Fig. 52.2). Molecular medicine and molecular imaging promise to bring applications of genomics and protein messaging quickly into the clinical arena. We now have the ability to follow gene therapy as well as stem-cell therapy through their introduction into the patient. Lymphoscintigraphy is helping surgeons to better stage melanoma and breast cancer and has significantly decreased patient morbidity following nodal staging procedures. Hand-held probes allow better localization of sentinel nodes as well as of small difficult lesions identified on PET FDG scans. New therapies include antibody therapy for lymphoma, and research is being advanced for breast cancer antibody therapy, I-131 MIBG and yttrium (Y-90)-labeled octreotide.
The material in this section is intended to provide an overview of the specialty and at the same time serve as the basis of review for those residents preparing for board examinations. The information should also be useful to those who may not practice nuclear medicine regularly or may not have done so recently.
Imaging Principles
The basic principles of diagnostic nuclear radiology are simple to grasp, yet somehow seem to elude first-year residents as they are overwhelmed with information at the outset of their training. The concept of nuclear imaging is based on the external detection and mapping (emission image) of the biodistribution of radiotracers that have been administered to a patient. The knowledge of the normal patterns of uptake, distribution, and excretion permits us to make decisions concerning the presence or absence of disease.
Sometimes a radionuclide or radioisotope of a naturally occurring element essential to normal biologic function (e.g., Iodine-123) or an analog (e.g., Technetium-99m Pertechnetate, Tc-99m-O4) is used without additional chemical alteration (Fig. 53.3). More commonly, a radioactive isotope is combined with a physiologically “active” compound to create a radiopharmaceutical which can be administered intravenously, orally, or via direct injection. Thus Tc-99m-O4 may be combined with a diphosphonate compound for skeletal imaging. If the same radioisotope is combined with an iminodiacetic acid derivative, the biologic distribution reflected by the images will be that of a biliary scan. This simple concept is the foundation for imaging the biodistribution of radiolabeled blood cells, monoclonal antibodies, peptides, and energy substrates such as glucose and fatty acids. If this unifying principle can be kept in mind while reading the various sections on nuclear imaging, the diverse number and types of studies may seem somewhat less bewildering.
Radiotherapy
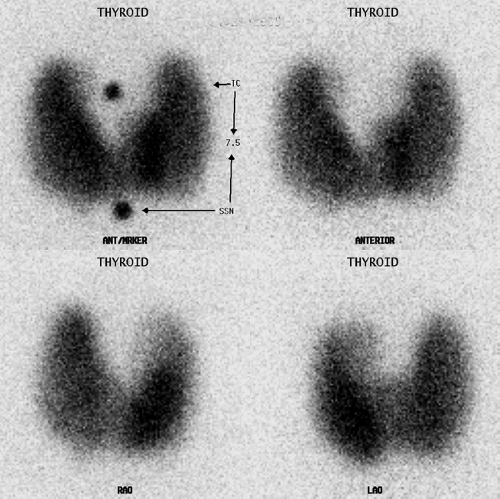
Radiotherapy is an extremely important arm of nuclear medicine and is critical to several areas of clinical medicine. The distinguishing feature of therapeutic radioisotopes and radiopharmaceuticals is that they are particulate emitters, with beta emitters being utilized much more commonly than alpha emitters. Beta particles only travel a short distance through tissues, depositing most of their energy within a couple of millimeters. I-131 is utilized for benign thyroid conditions such as Graves’
disease, toxic adenoma, and Plummer disease or toxic multimodular goiter (Fig. 52.3). I-131 is also the primary treatment of choice for thyroid remnant ablation and metastatic thyroid cancer. I-131 MIBG and Y90 octreotide are under evaluation for treatment of metastatic neuroendocrine tumors as well.
disease, toxic adenoma, and Plummer disease or toxic multimodular goiter (Fig. 52.3). I-131 is also the primary treatment of choice for thyroid remnant ablation and metastatic thyroid cancer. I-131 MIBG and Y90 octreotide are under evaluation for treatment of metastatic neuroendocrine tumors as well.
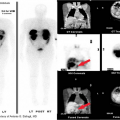
P-32 can be given intravenously for hematological disorders such as essential thrombocytosis, or in colloidal form for localized installation in arthritic joints for radiosynovectomy, in cystic tumors or into malignant fluid collections. Strontium-89 and Samarium-153 have proven effective in palliative pain management for patients with osteoblastic bone metastases. Radioimmunotherapy (RIT) with monoclonal antibodies is now being utilized for refractory lymphoma treatment with ibritumomab tiuxetan (Yttrium-90 Zevalin©) and tositumomab (I-131 Bexxar©) (Fig. 52.4). RIT is also being studied for refractory metastatic breast cancer. A new form of radioembolotherapy (RET) is being utilized in conjunction with interventional radiology. After careful planning and dosimetry calculations, Y-90 microspheres are injected directly into selected hepatic arteries for treatment of unresectable hepatocellular or for metastatic liver disease.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree