Abstract
Multifetal reduction is the termination of one or more fetuses in a multifetal pregnancy to decrease the likelihood of maternal and fetal morbidity and mortality. Before the procedure, an ultrasound exam should be performed to assess the fetal number and chorionicity and to screen for fetal anatomic abnormalities. Genetic screening/testing should also be offered as the findings may lead to the selective termination of an anomalous fetus. Fetal reduction is achieved through intracardiac instillation of potassium chloride or, in the case of monochorionic fetuses, radiofrequency cord ablation. This procedure should be performed under ultrasound guidance and is mostly commonly performed through a transabdominal approach. Fetal and neonatal outcomes are dependent on the starting and finishing fetal numbers. Triplet pregnancies reduced to twins have lower total pregnancy loss rates, preterm delivery <28 weeks, NICU admission, and perinatal mortality. Although there appears to be a benefit to reducing higher-order multiples to a twin gestation, the benefit of reducing a twin pregnancy to a singleton less clear. The maternal benefits of fetal reduction include decreased rates of hypertensive diseases of pregnancy, gestational diabetes, and cesarean delivery.
Keywords
multifetal pregnancy reduction, selective termination, multiple gestation
Introduction
Multiple gestations are at risk for perinatal morbidity and mortality that increase with higher-order pregnancies, primarily caused by complications of prematurity. The risk of preterm delivery increases as the number of fetuses increases. In 2014, preterm delivery <32 weeks occurred in 1% of singletons, 11% of twins, 39% of triplets, and 72% of quadruplets. Infant mortality increases fourfold in twins, 12-fold in triplets, and 26-fold in quadruplet births.
In addition to perinatal concerns, maternal risk is also significantly increased in higher-order pregnancies. Compared with twins, triplet pregnancies were at higher risk for pregnancy-associated hypertension (odds ratio [OR], 1.22; 95% confidence interval [CI], 1.15–1.30), eclampsia (OR, 1.69; 95% CI, 1.46–19.4), cesarean delivery (OR, 6.55; 95% CI, 6.15–6.97), and excessive bleeding in labor and delivery (OR, 1.41; 95% CI, 1.25–1.56).
The incidence of multifetal pregnancies has increased significantly over the past 3 decades, primarily because of the success of assisted reproductive technologies. The twin birth rate increased by 76% from 1980 to 2009, and accounted for 3.39% of live births in 2014. Triplet or higher-order pregnancies increased by 400% between 1980 and 1998. However, the rate of higher-order pregnancies had declined by 40% by 2009 as a result of primary prevention such as guidelines advocating the transfer of fewer embryos and secondary prevention with multifetal pregnancy reduction (MFPR).
In the 1980s several authors reported on MFPR as a method to improve maternal and fetal outcomes in high-order multiple pregnancies. This procedure involves the termination of one or more presumably normal fetuses to increase the overall likelihood of survival, and to decrease the long-term morbidity of the remaining fetus or fetuses. MFPR increases the rate of live birth, while decreasing the risk of pregnancy loss, preterm delivery, neonatal/infant demise, preeclampsia, and gestational diabetes.
Procedure
Setting
MFPR is performed as an outpatient procedure in an ultrasound (US) unit in the late first or early second trimester.
Counseling
The American College of Obstetrics and Gynecology recommends nondirective counseling when reviewing the details of a patient’s multifetal pregnancy (maternal health issues/risks, number of fetuses, and potential outcomes of pregnancy continuation versus reduction). The psychologic, economic, social, and health risks should be addressed before the procedure. The risks of the procedure should be reviewed, as well as the expected prognosis.
US should be performed before counseling to determine fetal number, chorionicity, and screen for possible genetic, growth, or anatomic abnormalities. The chorionicity of the pregnancy should be identified as early as possible, as this will affect the counseling relating to fetal selection for termination. Monochorionic twins are fraught with potential concerns, such as twin-twin transfusion syndrome and unequal placental sharing. Potassium chloride (KCl) termination of one fetus is contraindicated in a monochorionic twin gestation, as the anastomoses in the shared placenta may cause an inadvertent termination of the co-twin. Radiofrequency cord ablation can be used to selectively terminate one fetus in monochorionic twins, but this is associated with a higher risk of preterm labor, delivery in the periviable period, and loss of the pregnancy. Consideration should be given to reducing both monochorionic twins when present in a higher-order multiple pregnancy.
Risks of the procedure are similar to the risks of amniocentesis, including amniotic fluid leakage from the sac of a viable fetus, placental abruption, infection (chorioamnionitis), and pregnancy loss.
Genetic Testing
Multifetal pregnancies are more common with increasing maternal age. Advanced maternal age and assisted reproductive technology are known to increase the risk of fetal malformations and, therefore chromosomal analysis should be considered. As a consequence, patients should be counseled on the risks and benefits of prenatal screening and testing before fetal reduction, as the findings may lead to selective termination of an anomalous fetus. Screening for aneuploidy with nuchal translucency alone in twin pregnancies has a detection rate of approximately 70% for trisomy 21 with a 5% false-positive rate. When nuchal translucency was combined with first-trimester serum screening and nasal bone in a retrospective analysis of 4188 twin fetuses, the detection rates were 79% for nuchal translucency combined with serum analysis and 89% if the nasal bone was also included. For triplet pregnancies, screening options are limited. Serum screening, including cell-free fetal DNA and biomarker testing, has not been validated for triplets and higher-order multiples. The use of nuchal translucency has not been established, as the limited studies on this subject are conflicting.
Invasive prenatal diagnosis with chorionic villus sampling (CVS) has the advantage of reassuring the parents by confirming that the remaining fetuses are chromosomally normal; this is especially important in cases where the pregnancy is reduced to a singleton. At our institution, we offer karyotyping, microarray, and targeted diagnostic testing based on pregnancy risk factors. In recent years, several studies have shown the accuracy and safety of performing CVS in multifetal pregnancies before MFPR. One study documented successful performance of the procedure in 98.8% (85 of 86) of patients, with detection of an abnormal karyotype in 1.8% (3 of 165 fetuses) and an error rate of 1.2% (2 of 165). A larger study comparing patients who had CVS before MFPR ( n = 437) with those who did not ( n = 321) reported that women who underwent CVS had the reduction performed on average 1 week later (12.6 weeks) than those who did not (11.6 weeks). There was no difference in the overall loss rate, reported at 4% (17 of 437) in the CVS group versus 7% (21 of 321) in the non-CVS group ( P = .098). In that series, CVS was associated with a reduction in the pregnancy loss rate by 76% in women who reduced to a singleton; the loss rate was 2% (4 of 192) in the CVS group versus 9% (6 of 90) in the non-CVS group. These authors concluded that CVS before MFPR does not increase the risk for pregnancy loss and possibly may reduce the risk for adverse outcomes before reduction to a singleton. On the basis of recent series that indicate a growing rate of MFPR procedures to a singleton, first-trimester screening and CVS should be offered to all women who are considering undergoing MFPR..
Technique
At our institution, MFPR procedures are ideally performed between 11 and 13 weeks’ gestation. At this gestational age range, most spontaneous losses will already have occurred, the procedure is technically easier to perform, and US screening/invasive testing can be performed. The procedure is most commonly performed transabdominally because transvaginal and transcervical approaches have been reported to be associated with higher pregnancy loss (13.3% versus 3.5%, P = .04) ( Fig. 117.1 ).

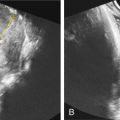
Before performing an MFPR, a US exam should be performed to identify the position and chorionicity of the pregnancy. The decision of which fetus or fetuses to reduce should take into consideration the outcomes of available screening/testing results or other US evidence of early intrauterine growth restriction or detection of a major fetal anomaly. If all prenatal diagnostic tests are normal, the most easily accessible fetuses are targeted for reduction, and the fetus overlying the internal cervical os is spared ( Fig. 117.2 ) because of the theoretic risk of infection or preterm delivery if that fetus were reduced. This should be differentiated from selective termination, in which a fetus is reduced based on genetic or structural abnormality regardless of its position.