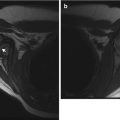
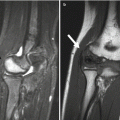
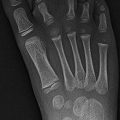
Fig. 27.1
Posterior spinal fusion (PSFI) with instrumentation. (a, b) There are hooks (white arrows) above the laminae of T2, and screws (black arrows) have been inserted through the pedicles and then into the vertebral bodies at multiple levels. Vertical rods connect the instrumentation
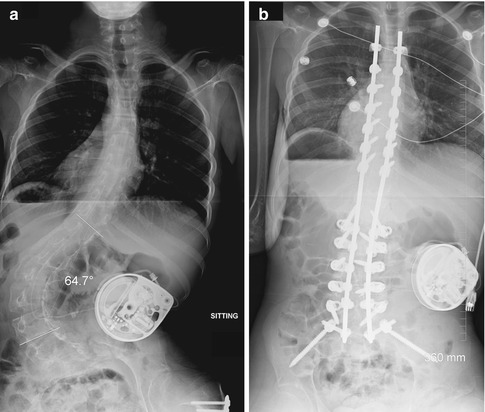
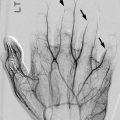
Fig. 27.2
PSFI anchored in iliac bones in patient with cerebral palsy (CP). (a) Preoperative image shows a neuromuscular-appearing curve, along with a baclofen pump and hardware from prior femoral varus derotational osteotomy. (b) This flexible curve almost straightens with posterior fusion. Hardware is anchored in the iliac bones (Courtesy of Rebecca Stein-Wexler)
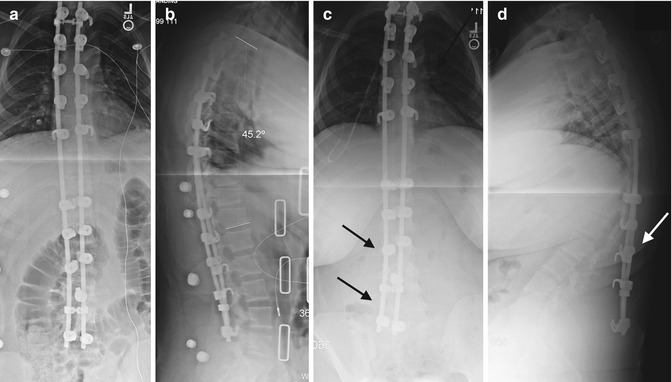
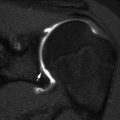
Fig. 27.3
PSFI failure due to pullout of the hooks. (a, b) Perioperative images demonstrate hooks at multiple levels, with mild wedging of multiple lower thoracic vertebral bodies due to underlying Scheuermann disease. (c, d) The three distal pairs of hooks have detached from the laminae, and the rods now arc to the right of (black arrows) and posterior to (white arrow) the lumbar spine (Courtesy of Rebecca Stein-Wexler)
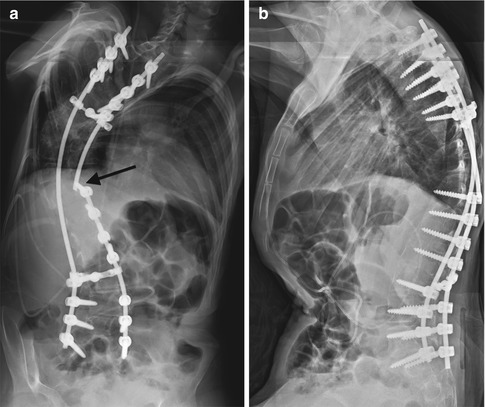
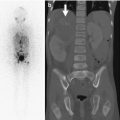
Fig. 27.4
PSFI with rod fracture. (a, b) The rod on the left has fractured (black arrow) just above a pedicle screw (Courtesy of Leslie E. Grissom)
Clinical Application
Idiopathic scoliosis, neuromuscular scoliosis.
Specific Indications
This procedure is used to halt progression of scoliosis, to restore coronal and sagittal balance, and to improve the appearance of chest wall deformity.
Surgical Technique
Hooks are placed around the pedicles or laminae, or pedicle screws are inserted through the pedicles into the vertebral body (Fig. 27.1). Vertical rods are then inserted through this hardware. The posterior spinal elements are decorticated, the facet joints removed, and bone graft applied. For patients with neuromuscular scoliosis, the distal extent of hardware may be embedded in the iliac bones, in order to improve spine stability (Fig. 27.2).
Postoperative Evaluation
Hooks, screws, and rods are visible on the right and left sides of the spine. Bone graft is usually visible primarily on the concave side of the curve.
Complications
Hooks may erode the spine and subsequently pull out (Fig. 27.3). Pullout of pedicle screws is extremely rare. Pedicle screws may be malpositioned, potentially damaging the spinal cord, nerve roots, or soft tissues adjacent to the spine. If pedicle screws are positioned too far to the left, the aorta may be endangered (this is generally seen on the concave side, near the apex). A major increase in scoliosis implies failed fusion. Rod breakage (Fig. 27.4; see also Fig. 3.69) indicates motion, which may signify incomplete fusion or pseudarthrosis.
1.3 Growing Rod Technique [2] (Figs. 27.5–27.9)
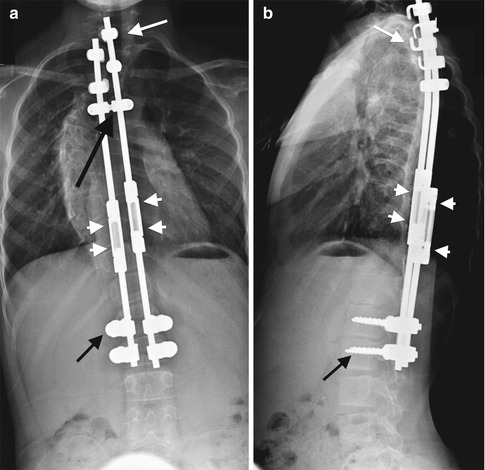
Fig. 27.5
Growing rod technique. (a, b) There are hooks (short white arrows) and pedicle screws (short black arrows) at the foundation sites. The two expandable growing rods are connected by a transverse connector (long black arrow). The expandable growing rod is extended through the tandem connector (arrowheads)
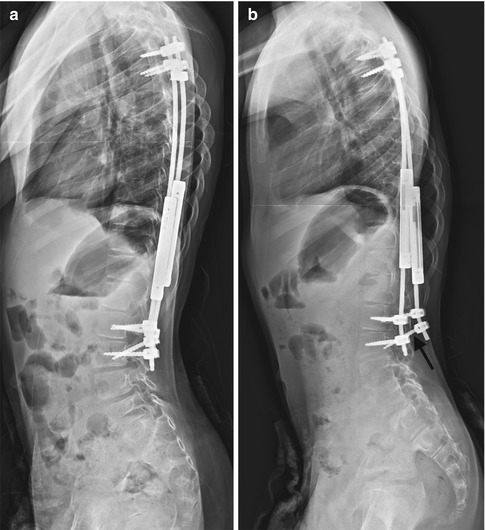
Fig. 27.6
Screw retraction from growing rods. (a) After surgery, one of the four distal foundation pedicle screws is angled and may not adequately engage with the pedicle. (b) Later, both the angled screw (arrow) and the screw above are dorsally displaced, no longer engaged with the pedicle. The associated rod arcs posteriorly (Courtesy of Leslie E. Grissom)
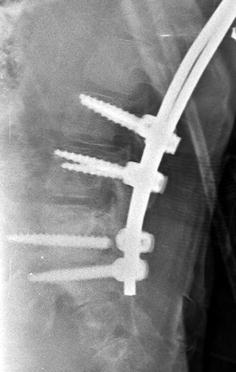
Fig. 27.7
Growing rods with screw fracture. There is an obvious break in one of the two most distal foundation screws. Furthermore, ill-defined lucency surrounds both distal screws, suggesting loosening (Courtesy of Leslie E. Grissom)
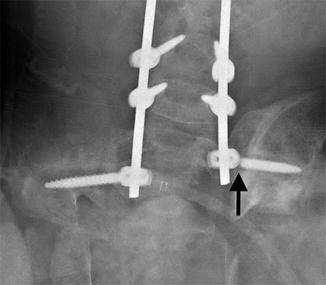
Fig. 27.8
Growing rods with screw fracture and loosening. One of the distal anchoring screws at the iliac bone has fractured (black arrow) near its base. Ill-defined lucency surrounds that screw as well as its counterpart on the right, indicating loosening (Courtesy of Leslie E. Grissom)
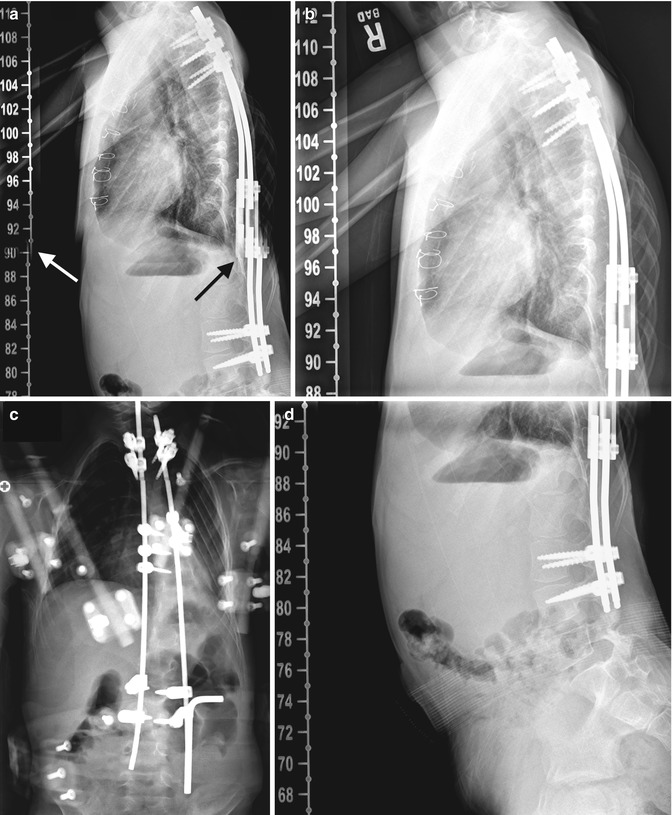
Fig. 27.9
PSFI with rod breakage simulated by stitching artifact. (a) On the lateral view, the more anterior rod appears fractured (black arrow). However, duplication of the measurement numbers (white arrow) indicates that this break results from stitching artifact. (b, d) Review of the source images shows no evidence of rod fracture. (c) On the frontal projection, the rods appear intact (Courtesy of Leslie E. Grissom)
Clinical Application
Progressive early-onset scoliosis.
Specific Indications
This procedure is employed in young children with progressive deformity that (in general) exceeds 50°, who have failed nonoperative measures. The goal is to postpone definitive spinal fusion in order to allow the child to achieve maximal spinal growth, overall growth of the entire thoracic cavity, and optimal lung maturation.
Surgical Technique
Distal and proximal foundation sites are prepared by exposing the subperiosteal bone. Hooks or screws may be used at either site. Each foundation is composed of four anchors (hooks and/or screws), which are attached to vertical rods (Fig. 27.5). These rods are placed by a solely subcutaneous or subfascial approach. This is important, since premature spine fusion is avoided by not disturbing the remainder of the spine. Rods are connected transversely by a subcutaneous transverse connector. The vertical rods are lengthened at the tandem connector about every 6 months to accommodate growth.
Postoperative Evaluation
Hooks and/or screws are attached to the spine at each foundation site. Elongation of the rods is best appreciated by evaluating the length of the rod distraction gap.
Complications
If the foundation sites are not stable enough to accept corrective loads, hooks and/or screws may dislodge (Fig. 27.6). Pedicle screws and hooks may also pull out during growth. Rod breakage may occur. Screws may loosen and fracture (Figs. 27.7 and 27.8). With this and other procedures, improper alignment of pasted images may give the false impression that rods are fractured (Fig. 27.9). Although infection is a risk with any surgical procedure, the manipulation involved with lengthening increases the likelihood of infection with this procedure.
1.4 Vertical Expandable Prosthetic Titanium Rib (VEPTR) [3, 4] (Fig. 27.10; See Also Fig. 3.66)
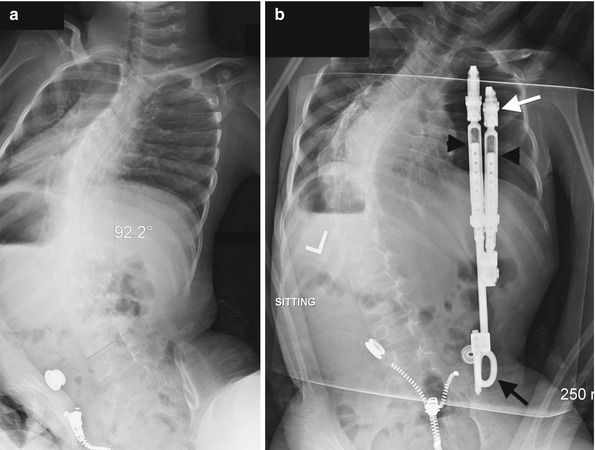
Fig. 27.10
Vertical expandable prosthetic titanium rib (VEPTR) technique. (a) Preoperative image demonstrates severe neuromuscular scoliosis and a small thoracic cage. (b) The VEPTR device is attached proximally to the ribs via a cradle (white arrow). The distal portion of the device is attached to the iliac bone (black arrow). The device is expanded through the tandem connector (arrowheads)
Clinical Application
Patients with thoracic insufficiency syndrome due to a primary spine or rib deformity.
Specific Indications
This procedure is used to treat thoracic insufficiency syndrome in children who have fused ribs and severe scoliosis, flail chest, or a hypoplastic thorax.
Surgical Technique
The proximal portion of the VEPTR device is attached to the ribs via a cradle. The distal portion is attached to the ribs, lumbar spine, or ilium (the ilium is usually used if the patient has neuromuscular impairment). No spinal fusion is performed. The device is expanded twice per year to accommodate patient growth.
Postoperative Evaluation
The VEPTR should be securely attached both proximally and distally. Expansion is apparent at the tandem connector (see Fig. 3.66).
Complications
Cradle detachment and VEPTR displacement are not uncommon. The device is bulky and may induce soft tissue complications such as skin breakdown. Manipulation of the rods increases risk of infection.
1.5 Anterior Spinal Fusion [5–9] (Fig. 27.11; See Also Fig. 3.67)
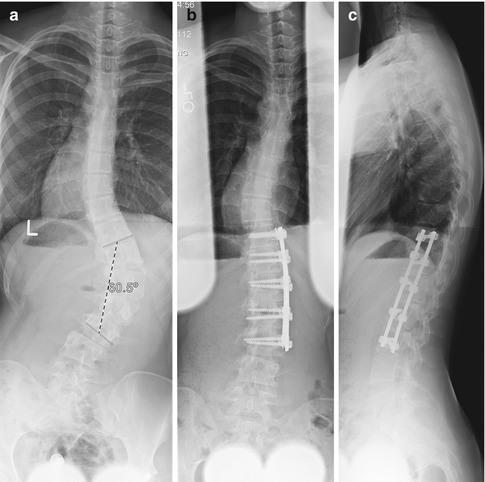
Fig. 27.11
Anterior spinal fusion. (a) Preoperative image shows focal lower thoracic/upper lumbar dextroscoliosis. (b, c) Screws traverse each vertebral body and are linked together by vertical rods. Grafting material fills the disk spaces
Clinical Application
Thoracolumbar or lumbar curves in patients with idiopathic scoliosis, kyphosis, and dysplastic spinal instability.
Specific Indications
Anterior spinal fusion with instrumentation is used to treat certain curve patterns in adolescent idiopathic scoliosis, usually in the thoracolumbar spine. Applying anterior as well as posterior fusion may make it possible to decrease the extent of distal fusion, preserving more spine mobility. Anterior spinal fusion is also usually combined with posterior fusion in cases with deficient posterior structures, such as myelodysplasia, or dystrophic healing, as in neurofibromatosis. In addition, by restricting anterior growth in young children who also undergo PSFI, anterior spinal fusion may prevent the “crankshaft” phenomenon, which occurs when abnormal spinal curvature develops due to continued anterior growth after posterior fusion.
Surgical Technique
Disks are removed from an anterior approach, which in some cases adequately corrects the abnormal curvature. In cases that also require instrumentation, screws are placed across the vertebral body and then linked together by rods. Bone graft and/or a structural cage is placed in the disk space to facilitate fusion and maintain lordosis.
Postoperative Evaluation
Hardware is clearly visualized. Eventually the disk spaces are obliterated by mature bone, although if a structural cage has been placed, it will remain evident.
Complications
Screw loosening, hardware failure, and pseudarthrosis may occur.
2 Pelvic Acetabuloplasty
2.1 General Considerations
Pelvic acetabuloplasty procedures reorient or change the depth or version of the acetabulum to improve hip joint congruence and to achieve a more normal weight-bearing surface. These surgeries are performed in patients with developmental dysplasia of the hip (DDH), Legg-Perthes disease, cerebral palsy, and other disorders that contribute to the development of a dysplastic acetabulum.
There are three general types of acetabuloplasty procedures: rotational acetabuloplasty, reduction acetabuloplasty, and augmentation acetabuloplasty. Each is performed by cutting the pelvis to reorient the articular surface over the femoral head. The indications for each depend on the degree and direction of acetabular deficiency, as well as the age and skeletal maturity of the patient.
Rotational acetabuloplasties, such as the Salter, Steel triple osteotomy, and periacetabular osteotomy, rotate the dysplastic acetabulum around a concentric femoral head after performance of a series of pelvic osteotomies. These procedures are generally used for patients with more significant deformity or for those whose hip dysplasia is not recognized until late childhood (or later).
Reduction acetabuloplasties, such as the Pemberton and Dega, redirect the acetabulum around a concentric femoral head, decreasing acetabular volume. These osteotomies are performed on the youngest patients, whose hips are best able to respond to decreased volume by continuing to grow and develop after the osteotomy.
Augmentation acetabuloplasties, such as the Chiari and shelf procedures, are generally utilized as salvage procedures, when additional acetabular coverage is needed but a concentric reconstruction cannot be achieved with other acetabuloplasties. These approaches are often employed in children with aspherical femoral heads or premature arthritis.
2.2 Rotational Acetabuloplasty with Innominate Osteotomy (Salter) [10, 11] (Figs. 27.12 and 27.13)
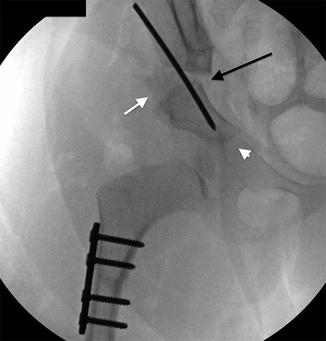
Fig. 27.12
Rotational acetabuloplasty with innominate osteotomy (Salter). There is a horizontal osteotomy of the ilium just above the acetabulum (long black arrow). A triangular-shaped bone graft (short white arrow), taken from the iliac crest, is held in the osteotomy site by a pin. The osteotomy is hinged medially without offset of the lower segment (white arrowhead). A varus femoral osteotomy has also been performed in this patient with developmental dysplasia of the hip (DDH)
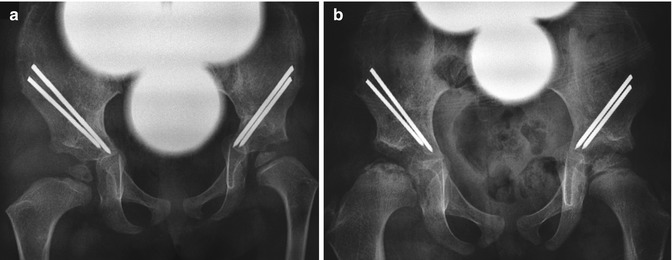
Fig. 27.13
Avascular necrosis (AVN) after rotational acetabuloplasties with innominate osteotomies. (a) Bilateral osteotomies have healed in this 2-year-old girl with history of bilateral DDH, and hardware is intact. Femoral heads are reduced. (b) 1.5 years later, the right femoral head is small and sclerotic; the metaphysis is broad and demonstrates subphyseal cysts. The left hip is developing normally (Courtesy of Rebecca Stein-Wexler; images copyright Shriners Hospital for Children, Los Angeles)
Clinical Applications
DDH and Legg-Perthes disease.
Specific indications: This procedure provides increased anterior and lateral coverage of the femoral head. It is performed in younger children whose pubic symphysis is still flexible. Congruent hip reduction and a spherical femoral head are prerequisites.
Surgical Technique
A horizontal osteotomy of the ilium is performed just above the acetabulum. The osteotomy is opened anteriorly and laterally by hinging and rotating the acetabular segment, using the pubic symphysis as the axis of rotation. A triangular-shaped bone graft is taken from the iliac crest and is held in the osteotomy site by transfixing pins.
Postoperative Evaluation
The osteotomy is hinged medially without offset of the lower segment. The lower ilia and obturator foramina should be asymmetrical on the two sides due to the rotation of the segment (bilateral symmetry is later regained through remodeling). Pins should not penetrate into the hip joint or pelvic basin. The bone graft donor site is usually identifiable.
Complications
Loss of angulation and rotation may occur in the immediate postoperative period. Pin extrusion, graft dislodgement, medial migration of the lower segment, and disruption of the ipsilateral sacroiliac joint are also possible. Avascular necrosis (AVN) may develop (Fig. 27.13).
2.3 Triple Innominate Osteotomy (Steel) [12, 13] (Fig. 27.14)
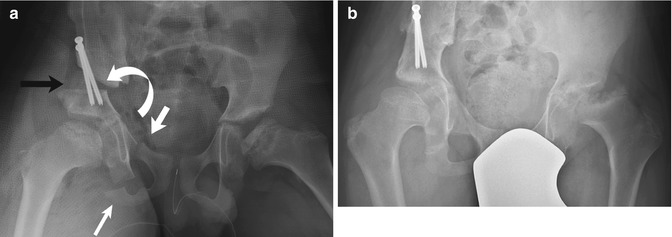
Fig. 27.14
Triple innominate osteotomy (Steel). (a) A perioperative image in a patient with bilateral AVN shows a supra-acetabular horizontal iliac osteotomy with bone graft (black arrow), a vertical osteotomy of the pubis (thick white arrow), and excision of a small segment of the ischium (thin white arrow). The acetabular fragment is rotated (curved arrow) to cover the femoral head. Transfixing screws hold the osteotomy in place. (b) Two years later, bone graft material is smoothly incorporated into a fully healed osteotomy
Clinical Applications
DDH, neuromuscular hip dislocation, AVN.
Specific Indications
As with the Salter procedure, a congruent hip joint is a prerequisite for this procedure. The triple innominate osteotomy is utilized to improve acetabular coverage in the older child whose pubic symphysis is no longer flexible.
Surgical Technique
A horizontal osteotomy of the ilium is performed just above the acetabulum. A vertical osteotomy of the pubis is also performed. A small segment of the ischium is excised. The acetabular fragment is completely free and is rotated where coverage is needed. Bone graft is placed into the gapped iliac osteotomy, and transfixing screws are used to hold the osteotomy in place.
Postoperative Evaluation
Femoral head coverage is improved, and there should be no pins or screws penetrating the pelvic basin or hip joint.
Complications
Pin or screw penetration, graft extrusion, and loss of correction may occur.
2.4 Pericapsular Iliac Osteotomy of Pemberton (Reduction Acetabuloplasty) [14–17] (Fig. 27.15)
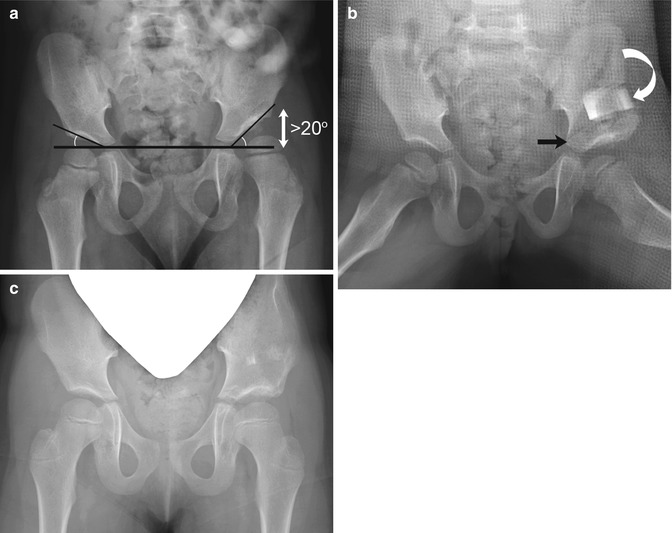
Fig. 27.15
Pericapsular iliac osteotomy of Pemberton (reduction acetabuloplasty). (a) Preoperative image shows a shallow left acetabulum with an acetabular angle of greater than 20° (double arrow) and left hip subluxation. (b) The ilium has been cut around the acetabulum, down to the triradiate cartilage (black arrow). The acetabular rim has been displaced downward and is held in place with a bone graft (curved arrow). The acetabular index is improved and the femoral head reduced. (c) Two years later, the osteotomy has healed, and the left iliac bone remains mildly distorted
Clinical Applications
DDH with acetabular dysplasia.
Specific Indications
Acetabular dysplasia with a capacious acetabulum relative to the size of the femoral head. The acetabular index angle is larger than normal (>20° at age 2 or older). The triradiate cartilage must be open and mobile. The Dega procedure achieves the same goals as the Pemberton and appears radiographically similar.
Surgical Technique
The ilium is cut circumferentially around the acetabulum down to the triradiate cartilage. The acetabular rim is displaced downward and held with a bone graft. Unlike the Salter or Steel osteotomies, the bone graft is inherently stable and fixation is typically not needed.
Postoperative Evaluation
The femoral head is reduced and the acetabular index improved.
Complications
Intra-articular extension of the osteotomy, graft extrusion, and hip subluxation may occur.
2.5 Augmentation Acetabuloplasty: Medial Displacement Osteotomy (Chiari) [18–21] (Fig. 27.16)
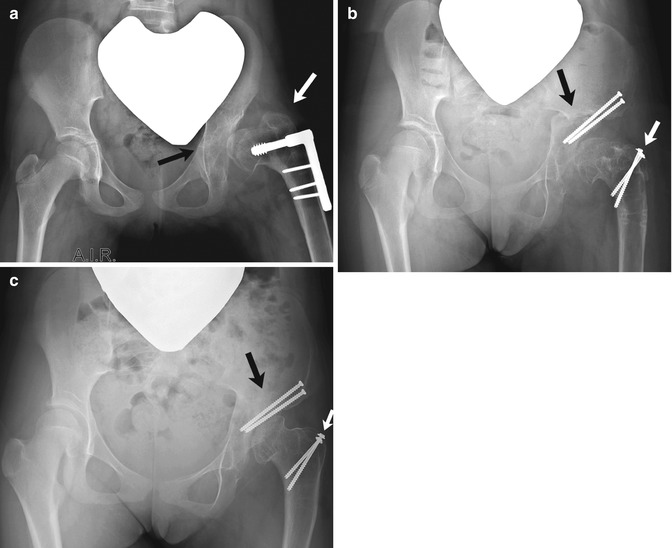
Fig. 27.16
Augmentation acetabuloplasty-medial displacement osteotomy (Chiari) with greater trochanter transfer. (a) Preoperative image obtained in abduction and internal rotation (AIR) shows a nonconcentric hip (black arrow) and a shallow acetabulum. The patient had already been treated with an unsuccessful varus derotational proximal femoral osteotomy, and the greater trochanter is higher than the femoral articulation (white arrow). (b) After surgery, the cut bony margin of the ileum forms a large neo-acetabulum that covers the medially shifted femoral head. Note offset (black arrow) at inner margin of the pelvis. Trochanteric advancement (white arrow) has also been performed, so that the greater trochanter is now distal to the level of the femoral articulation. (c) 1.5 years later, osteotomies have healed, and the pelvic offset has remodeled, with residual narrowing of the pelvic outlet. The contour of the femoral head is smoother
Clinical Applications
DDH, AVN
Specific Indications
This procedure is performed for symptomatic, nonconcentric hips that cannot be treated with concentric acetabuloplasty procedures. Since the bone and not the cartilage is placed over the femoral head, this is considered to be a salvage procedure.
Surgical Technique
A supra-acetabular osteotomy is performed, extending from the anterior ilium into the sciatic notch. The leg is then abducted, and axial pressure is applied to cause the acetabular fragment to displace medially underneath the ilium. Pins or screws are used to hold the pelvis in its corrected position.
Postoperative Evaluation
The supra-acetabular portion below the osteotomy is displaced medially, with offset at the inner margin of the pelvis. The femoral head is shifted medially and covered by the enlarged acetabulum. The procedure may be performed in conjunction with femoral procedures, such as trochanteric advancement or intertrochanteric osteotomy.
Complications
Loss of medial displacement, insufficient medial movement of the lower segment, over-displacement with loss of bony contact, and pin or screw migration may occur. Later, there may be narrowing of the pelvic outlet or degenerative arthritis of the hip, as the femoral head rests on interposed capsule.
2.6 Staheli Shelf Procedure [22–24] (Fig. 27.17)
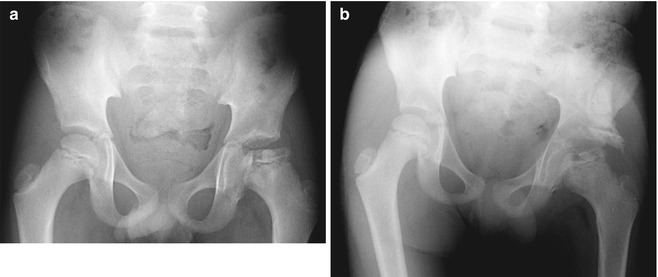
Fig. 27.17
Staheli shelf procedure. (a) Preoperative image shows the left femoral head is flat, broad, sclerotic, partially uncovered, and non-congruent after Legg-Perthes disease. (b) After surgery, a block of bone extends the acetabulum laterally, improving coverage of the femoral head. The inferior surface of the bone buttress is at the level of the lateral acetabular rim (Courtesy of Leslie E. Grissom)
Clinical Indications
DDH
Specific Indications
To increase the load-bearing area of the femoral head. This procedure is only performed if the acetabulum cannot be redirected to provide better coverage. Like the Chiari, this is a salvage procedure because the bone and not the cartilage is being placed over the femoral head.
Surgical Technique
A bone block is placed in a slot at the edge of the acetabulum and may be fixed with a pin or screw.
Postoperative Evaluation
The femoral head is reduced and laterally covered by bone buttress. The inferior surface of the bone block should be at the level of the lateral acetabular rim.
Complications
Displacement or pressure resorption of the bone block due to continued lateral subluxation of the femoral head may occur. Degenerative arthritis may develop.
3 Hip and Proximal Femur
3.1 General Considerations
Most operative procedures performed on the proximal femur correct abnormally increased rotation and angulation of the femoral neck by means of a varus or valgus derotational intertrochanteric ostetomy. In other cases screws may be placed across an acute or subacute slip of the proximal femoral epiphysis, intended to stabilize the epiphysis and prevent further displacement; proximal femoral osteotomies may be performed later on, in order to correct the position of the femoral head. Trochanteric transfer may be performed to shift the insertion of the abductor force distally in patients in whom shortening of the femoral neck has reduced the normal articular-trochanteric distance. Hip joint fusion is a temporizing measure, decreasing the symptoms of a degenerative joint in a child who is considered too young for joint replacement.
3.2 Varus Derotational Femoral Osteotomy [25] (Fig. 27.18)
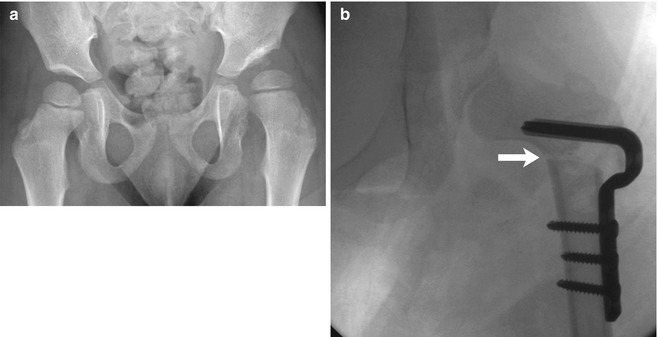
Fig. 27.18
Varus derotational femoral osteotomy. (a) There is bilateral coxa valga in this patient with CP. The left acetabulum is shallow, and the hip is subluxated. (b) Transverse femoral osteotomy at the level of the lesser trochanter (arrow) results in improved femoral head coverage. A blade plate holds the osteotomy fragments together
Clinical Applications
Cerebral palsy, Legg-Perthes disease, hip dysplasia, and increased femoral anteversion.
Specific Indications
This procedure is used to correct abnormally increased femoral anteversion and/or valgus deformity. It is also used to increase varus and contain the femoral head in some cases of AVN or Legg-Perthes disease.
Surgical Technique
A transverse femoral osteotomy is performed at the level of the lesser trochanter. A wedge of bone may be removed to achieve varus, but this is not always necessary. The desired amount of varus and anteversion is achieved and either a blade plate or a hip screw placed to hold the osteotomy together. Ideally, the distal shaft is positioned more medially in order to maintain normal weight-bearing forces.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree