Clinical Presentation
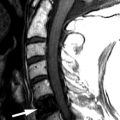
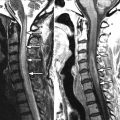
The patient is a 39-year-old otherwise healthy woman who developed a papulopustular skin eruption/infection attributed to MRSA (methicillin-resistant Staphylococcus aureus ). One month later, she developed pleuritic chest pain and a cough and was diagnosed with pneumonia. The symptoms resolved, but pleuritic chest pain recurred along with back pain. The patient was afebrile. Magnetic resonance (MR) imaging of the thoracic spine was ordered.
Imaging Presentation
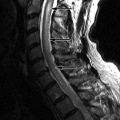
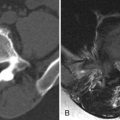
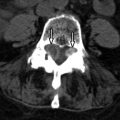
MR imaging of the thoracic spine revealed signal abnormalities consistent with T5-6 discitis and vertebral osteomyelitis ( Figs. 56-1 to 56-4 ) . A paraspinal phlegmon was also demonstrated ( Fig. 56-5 ) . A percutaneous paraspinal computed tomography (CT)–guided biopsy was performed at the T5-6 level, which yielded no viable organisms ( Fig. 56-6 ) . This was followed with a percutaneous transpedicular biopsy ( Fig. 56-7 ) . A diagnosis of MRSA osteomyelitis and discitis was made based on the culture of biopsy tissue.







Discussion
Spondylodiscitis is an infectious process involving the vertebra ( osteomyelitis ) and adjacent intervertebral disc ( discitis ). Rarely, tuberculosis and other granulomatous infections can cause vertebral infection without invading the intervertebral disc, but the vast majority of cases of osteomyelitis penetrate the vertebral endplate to involve the intervertebral disc. The vertebral-disc infection frequently extends into the paraspinal and epidural space forming a phlegmon, which may cavitate to form an abscess. Rarely, the infection infiltrates the thecal sac where it can cause arachnoiditis, meningitis, or an intramedullary spinal cord abscess.
Pyogenic and granulomatous spondylodiscitis occurs more frequently in patients with a chronic illness, including patients with diabetes mellitus, chronic renal failure, or chronic liver disease; immunocompromised patients; and IV drug abusers. Spondylodiscitis also occurs in patients with chronic nutritional deficiencies such as those in chronic alcoholics.
Most vertebral infections occur from blood-borne pathogens that preferentially settle in the hypervascular marrow adjacent to the vertebral endplates. In adults, the disc is an avascular structure and becomes secondarily involved after the infectious process destroys the vertebral endplates. The vertebral cortical and cartilaginous endplates represent the nutritional conduit for the intervertebral disc. When the cortical and cartilaginous endplate becomes disrupted, the infection can enter directly into the disc. In children, the intervertebral disc may still be vascularized, so the infectious process can begin primarily within the disc. Infections can also invade the vertebra by direct extension from infections in adjacent organs such as infections originating in the genitourinary or gastrointestinal tract. Infections may also occur in the vertebra after trauma, surgery, or percutaneous spine interventional procedures.
Vertebral infections are most commonly caused by pyogenic bacteria. The most common pathogen is Staphylococcus aureus (see Figs. 56-1 to 56-5 ). However, other organisms may cause pyogenic spine infections, including coagulase negative Staphylococcus ( Figs. 56-8 and 56-9 ) , Streptococcus, Pneumococcus, Hemophilus, Enterococcus, Escherchia coli, Salmonella, and rarely anaerobic organisms. Granulomatous spinal infections are seen with increasing frequency, especially in immunocompromised patients. Granulomatous spondylodiscitis is most commonly produced by Mycobacterium tuberculosis ( Fig. 56-10 ) . However, atypical mycobacteria ( Figs. 56-11 to 56-13 ) , Brucella, Streptomyces , parasites, and fungal organisms can also cause granulomatous spine infections. Fungal spondylodiscitis is a rare spinal infection, usually occurring in immunocompromised patients. Infections produced by both common and uncommon pathogens more frequently occur in immunocompromised patients.






The diagnosis of spondylodiscitis should be made based on clinical information and the imaging appearance. Patients with spine infections typically present with acute or progressively worsening back pain. The pain tends to have an acute onset with pyogenic infections and a more insidious onset in granulomatous infections, but in both cases, the pain becomes progressively worse. Constitutional symptoms may be present including fever, chills, malaise, and night sweats. These patients may present with myelopathic symptoms if the cord is compressed by epidural phlegmon or abscess. If the phlegmon extends into the neural foramen or paraspinal soft tissues, they may have radicular symptoms.
Leukocytosis with a high neutrophil count, markedly elevated ESR (erythrocyte sedimentation rate), and C-reactive protein levels are strongly suggestive of a pyogenic infection. In granulomatous infections (e.g., tuberculosis, Brucella ), the ESR is usually elevated out of proportion to the degree of leukocytosis.
If a disc infection is suspected, it is important to perform percutaneous needle aspiration biopsy of the disc, adjacent vertebra, and/or phlegmonous tissue to culture the offending organism and determine the most effective antibiotic for treatment (see Figs. 56-6 and 56-7 ). However, one should not rely on a positive culture after aspiration biopsy to initiate therapy because the results are commonly negative for a variety of reasons. The disc aspiration may yield negative results if the patient has already received antibiotic therapy or if samples are taken only from the disc center, which may contain only noninfectious liquid and necrotic debris. It is important that aspiration samples be obtained from inflamed, contrast-enhancing tissue in the involved vertebral body, adjacent to a bony sequestrum or in a paravertebral phlegmon. Disc aspiration biopsy often yields negative results in patients with mycobacterial infections, so it is important to always consider tuberculosis as a possible cause of the infection.
It requires about 4 weeks to culture M. tuberculosis, so it is not practical to withhold therapy while waiting for culture results. However, the diagnosis of tuberculosis can also be made if acid-fast bacilli are detected in the tissue samples (using an enzyme-linked immunosorbent assay for tuberculous bacilli) or if characteristic Langhans giant cells are seen in the tissue. If tuberculosis is suspected, a positive Mantoux (purified protein derivative [PPD]) skin test supports the diagnosis of tuberculosis. A PCR (polymerase chain reaction) test should be performed on the biopsy tissue samples. PCR is a quick, reliable DNA test that is used to confirm the diagnosis of tuberculosis. However, the PCR may be, in a minority of cases, falsely negative, so a negative PCR does not exclude the diagnosis of tuberculous spondylitis. If caseating granulomas are observed histologically in the tissues, this indicates either tuberculosis or brucellosis.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree