Abstract
Other thoracic tumors can be found in fetal life, which are not described in previous chapters.
Bronchogenic cysts are masses derived from abnormal budding of the ventricular diverticulum that can appear in the mediastinum or the lung. It is a cystic duplication of the tracheobronchial tree, derived from an abnormal budding of the ventricular diverticulum of the foregut. Prenatal diagnosis is only possible in large, normally symptomatic cysts, showing a single, well-defined, unilocular, hypoechogenic intrathoracic mass within the lung parenchyma or mediastinum. Mediastinal and large cysts tend to compress the trachea and esophagus, with subsequent polyhydramnios and/or hydrops. Prenatal intervention is only indicated in massive cysts producing complications due to mediastinal shift.
Lymphangiomas arise from the lymphatic system and develop more frequently in the thorax, head, and neck. It is commonly described as a large singular or slightly multilocular fluid-filled cavity, located commonly in the neck and thoracic area. In 50% to 80% of patients affected by nuchal cystic hygromas, karyotypic abnormalities and various malformation syndromes are present, the most common being Turner syndrome. Prenatal imaging shows a thin-walled, multilocular or multiseptated cyst with variable echographic patterns, with no vascularization internally demonstrated by Doppler ultrasound. Size and shape may vary, although walls may appear multilobular at times.
Prognosis of these tumors will depend on precise location and size, and delivery must be planned based on individual characteristics of the lesion, in a tertiary center.
Keywords
pulmonary tumors, bronchogenic cyst, lymphangioma, thoracic hygroma
Introduction
Among rare thoracic tumors not described in previous chapters, two are the most common. Bronchogenic cysts are derived from abnormal budding of the ventricular diverticulum in the mediastinum or the lung. Lymphangiomas arise from the lymphatic system and develop more frequently in the thorax, head, and neck.
Bronchogenic Cyst
Definition
A bronchogenic cyst is a cystic duplication of the tracheobronchial tree, derived from an abnormal budding of the ventricular diverticulum of the foregut.
Prevalence and Epidemiology
Bronchogenic cysts account for about 20% to 30% of congenital bronchopulmonary foregut cystic malformations. Prevalence is reported as 1 : 42,000, although this could be underestimated because of the high rate of late diagnosis and hidden cases. Half of these cases are diagnosed after 15 years of age. Prenatal diagnosis is only possible in large cysts. A 70% detection rate has been suggested, although the small numbers of cases render any meaningful estimate difficult.
Etiology and Pathophysiology
Bronchogenic cysts result from abnormal budding of the ventral diverticulum of the primitive foregut. Most cysts develop between the 26th and 40th days of fetal life. If appearing during early bronchial development, the cyst is located in the mediastinum (30%), normally between the trachea and esophagus, and later it develops in the lung (70%). The cyst wall resembles a bronchus with ciliated respiratory epithelial lining, smooth muscle, cartilaginous structures, and bronchial mucus glands, usually filled with thick mucus.
Manifestations of Disease
Clinical Presentation
In children and adults, most cysts are asymptomatic and diagnosed at routine ultrasound or chest radiographs. Prenatally, clinical manifestations will depend on the size, presence of bronchial obstruction or mediastinal shift, and location. Rarely, bronchogenic cysts may obstruct a large bronchus creating a similar effect to bronchial atresia, with impaired fluid drainage distal to the obstruction leading to enlarged hyperechogenic lungs, mediastinal shift, and high risk of lung hypoplasia, polyhydramnios, and hydrops.
Imaging Technique and Findings
Ultrasound.
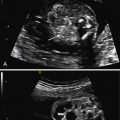
A single, well-defined, unilocular, hypoechogenic intrathoracic mass within the lung parenchyma or mediastinum. Mediastinal and large cysts tend to compress the trachea and esophagus, with subsequent polyhydramnios and/or hydrops. ( Fig. 7.1 ). Visualization of small mediastinal cysts can be challenging because of difficult differentiation from other structures, so they should be suspected in the presence of mediastinal enlargement without a clear mass.

Magnetic Resonance Imaging.
Magnetic resonance imaging (MRI) can be helpful for confirming large and detecting smaller bronchogenic cysts. It may aid in the differential diagnosis with other pulmonary malformations, providing better identification of congenital cystic adenomatoid malformation (CCAM) or bronchopulmonary sequestration, but reported error rates still range from 6% to 16%. The cyst is markedly hyperintense on T2-weighted MR imaging, and may show a hyperintense signal on T1-weighted images caused by mucoid or hemorrhagic contents.
- •
Single, well-defined, unilocular, hypoechogenic mass in the lung or mediastinum.
- •
Mediastinal shift may be associated, but is not mandatory for diagnosis.
Differential Diagnosis From Imaging Findings
The main differential diagnostic considerations are bronchopulmonary sequestration (BPS) and congenital cystic adenomatoid malformation (CCAM). Differentiation can be difficult or impossible prenatally with macrocystic CCAM lesions appearing as single cysts. Coexistence of these three separate anomalies in one lesion has been reported, suggesting a common embryologic link for these malformations.
The differential diagnosis must also include duplication cysts and neurenteric cysts. Duplication cysts are usually located in the middle or posterior mediastinum whereas neurenteric cysts are found in the posterior mediastinum and are associated with vertebral defects in the region where the cyst communicates with the spinal canal.
Synopsis of Treatment Options
Prenatal
Prenatal intervention is only indicated in massive cysts producing mediastinal shift. In utero pulmonary drainage may be associated with improvement in perinatal survival, but there is scarce experience and fluid may reaccumulate. There is no experience with thoracoamniotic shunts. Ex utero intrapartum treatment (EXIT) with cyst resection by thoracotomy has been recently described to avoid acute respiratory decompensation at birth.
Postnatal
Bronchogenic cysts may continue to grow slowly in the first months of life, but even in the absence of complications, size tends to increase constantly at an exponential rate, so resection is often recommended before 2 years of age, to avoid recurrent respiratory infection. In cases where intraparenchymal cysts wedge resection, segmental resection, or lobectomy may be required, prognosis will depend on location and size of the mass. Prenatally diagnosed cases may require urgent surgery at birth more often because of larger size.
- •
A very rare lesion appearing as a single cyst in the mediastinum or the lung.
- •
Prognosis depends on precise location and size, but is usually good.
- •
Large masses require planned delivery in a tertiary center.
- •
A benign tumor of the bronchial tree.
- •
With the rare exception of very large cysts, prognosis is generally good.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree