After completing this chapter, the reader will be able to perform the following: • Describe the relationship between autonomy, the respect for autonomy, and informed consent. • Identify the stresses involved in granting informed consent and autonomy. • List methods of verifying informed consent. • Compare and contrast competence and incompetence. • Correlate coercion, paternalism, and therapeutic privilege. • Explain why emergency situations and certain facilities may alter informed consent processes. • Identify ethical theories that may be implemented to facilitate problem solving. • Give examples of the difference between intentional and unintentional torts and ways the perception of intent rather than the actual intent may be the basis for allegations. • Provide examples of simple consent as it relates to assault, battery, and false imprisonment. • Differentiate standards of care with regard to the duty of informed consent. • Define and contrast the roles of the physician and the imaging professional in informed consent. • Identify the important but limited role of the consent form. During the early stages of development within the medical community, the patient’s autonomy was not a serious consideration. Physicians were expected to be omniscient and were rarely questioned. They acted as the “fathers” of their clientele. This paternalism and the invocation of therapeutic privilege were standard professional philosophies. As years passed and patients became more aware of their rights and privileges, however, the medical community developed new methods of informing patients. The emphasis on patient autonomy and informed consent has come from many areas (Box 4-1). Autonomy means that “one human person, precisely as a human person, dares not have the authority and should not have power over another human person. In a medical sense, a patient will not be treated without informed consent of his or her lawful surrogates, except in narrowly defined emergencies.”1 The patient’s right to information is important in considerations of autonomy. The American Hospital Association has established a patient care partnership document (see p. 255),2 which is to be given to hospitalized patients to help them understand the expectations, rights, and responsibilities regarding their health care. The way in which information is given depends on the criteria used to inform the patient. The following four potentially conflicting rules may guide the physician or other health care provider in explaining information to patients1: Institutional rules must also be taken into account. The prudent person rule, or reasonable patient standard, measures the physician’s disclosure to the patient based on the patient’s need for information to make decisions regarding treatment.1 The imaging professional must consider the information the patient needs to make informed decisions concerning a procedure. In the previous examples, the imaging professional or physician would have to decide how much the patient needs to know before he or she can make an adequate informed consent decision. The prudent person rule addresses many of the important elements of informed consent. A combination of the prudent person rule and the subjective disclosure rule, which requires the physician to communicate meaningfully with the patient, provides the information the patient needs to make an informed decision. Such a combination ensures that the physician has adequate knowledge about the patient and the patient has adequate knowledge about the procedure (Box 4-2). The Patient Self-Determination Act of 1991 helps ensure patient autonomy3: Heeding the principle of autonomy … means that imaging professionals should respect a patient’s choice to refuse treatments. The basic human right of all patients to refuse treatment was formally legislated by the Omnibus Budget Reconciliation Act (1990). The Patient Self-Determination Act became effective December 1, 1991, and requires all health care institutions receiving Medicare or Medicaid funds to inform patients that they have the right to refuse medical and surgical care and the right to initiate a written advance directive (i.e., a written or oral statement by which a competent person makes known his or her treatment preferences and/or designates a surrogate decision maker in the event he or she should become unable to make medical decisions on his or her own behalf [Box 4-3]). Hospitals, home health care agencies, and managed care organizations are required to make this information available, in writing, at the time the patient comes under an agency’s care. An imaging professional may overhear a co-worker speaking disrespectfully about an unconscious or deaf patient. Because respect for freedom and privacy is ultimately rooted in the dignity of each person, the maintenance of autonomy requires health care providers to respect all individuals, even those who are not currently capable of free choice.1 In short, people do not lose their dignity because they are unconscious, in a coma, or out of contact with reality. Such patients present special difficulties, but they must nevertheless be respected. Dignity and autonomy do not stem from a person’s ability to function in an imaging suite; instead, the clinical area should accommodate itself to the individual’s limitations.
Patient Autonomy and Informed Consent
ETHICAL ISSUES
DEFINITION OF AUTONOMY
PATIENT CARE PARTNERSHIP
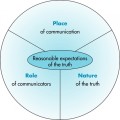
INFORMATION DELIVERY
Prudent Person Rule
Subjective Substantial Disclosure Rule
COMPLICATIONS OF AUTONOMY, INFORMED CONSENT, AND RIGHT OF REFUSAL
VERIFICATION OF INFORMED CONSENT
Patient Autonomy and Informed Consent