PET and PET-CT of Tumors of the Female Genital Tract
Lilie L. Lin
Farrokh Dehdashti
Barry A. Siegel
Perry W. Grigsby
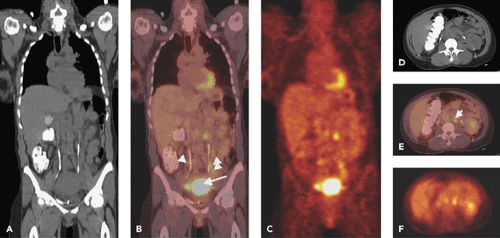
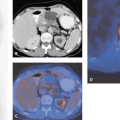
Gynecologic malignancies as a group represent a major worldwide health problem and result in significant mortality. Traditionally, imaging has not played a major role in diagnosis, staging, or monitoring response to therapy of these cancers. Conventional imaging, which relies on morphologic changes for detecting disease, has limited ability to detect small-volume tumor foci. Staging of these cancers has been based on clinical evaluation using Fédération Internationale de Gynécologie et d’Obstétrique (FIGO) staging system, which is not very accurate in determining the extent of disease or predicting prognosis. Positron emission tomography (PET), which relies on functional changes for detection of disease, offers a significant advantage over conventional imaging methods. PET has been successfully used for differentiation of benign from malignant lesions, staging of known cancer, detection of suspected recurrence, and monitoring response to therapy in various types of cancer (see Fig. 50.1). Although the use of PET has been only recently extended to include gynecologic cancers, the literature demonstrates an important role of PET in the management of patients with gynecologic cancers, especially cervical and ovarian carcinoma. This chapter discusses the current role of PET in the evaluation and management of patients with gynecologic neoplasms.
Introduction
The gynecologic malignancies include cancers of the vulva, vagina, cervix, uterus, fallopian tubes, and ovaries. Initial diagnosis and staging of most gynecologic malignancies are commonly achieved by history and physical examination and by use of selected imaging studies. Accurate staging of gynecologic cancers is important for both selecting appropriate therapy and predicting prognosis. Most gynecologic cancers initially spread regionally and then through lymphatic channels rather than through hematogenous dissemination to distant organs. With locally advanced disease, the status of pelvic and para-aortic lymph nodes is an important determinant of prognosis and guides treatment planning in patients undergoing radiation therapy. Computed tomography (CT) is the most widely used imaging method for assessment of nodal involvement and detection of distant metastatic disease. Despite its high resolution and excellent depiction of anatomy, CT is limited by its inability to detect small-volume metastatic involvement in normal-size lymph nodes and to determine whether enlarged nodes represent metastasis or reactive hyperplasia (which is particularly problematic in patients with large necrotic tumors with significant associated inflammation). Recognition of small peritoneal tumor deposits is also difficult on CT.
Over the last decade, fluorodeoxyglucose (FDG) positron emission tomography (PET) has become an
established oncologic imaging tool for many forms of cancers. The functional information about regional glucose metabolism provided by FDG-PET provides for greater sensitivity and specificity in most cancer imaging applications by comparison with CT and other anatomic imaging methods. The role of PET in gynecologic cancers is evolving, but the current literature suggests that PET is superior to conventional imaging modalities for evaluating patients with cervical and ovarian cancers. The role of PET in other gynecologic cancers is less well defined. The recent development and rapid dissemination of integrated PET-CT scanners that allow functional and anatomic information to be obtained in a single examination represents an important advance in PET imaging technology, resulting in a synergistic improvement in the accuracy of interpretation of both PET and CT images. Accordingly, the performance of PET based on published studies performed with conventional PET scanners is now being reevaluated in light of emerging PET-CT results. This chapter will discuss the role of PET and PET-CT in the management of gynecologic cancers.
established oncologic imaging tool for many forms of cancers. The functional information about regional glucose metabolism provided by FDG-PET provides for greater sensitivity and specificity in most cancer imaging applications by comparison with CT and other anatomic imaging methods. The role of PET in gynecologic cancers is evolving, but the current literature suggests that PET is superior to conventional imaging modalities for evaluating patients with cervical and ovarian cancers. The role of PET in other gynecologic cancers is less well defined. The recent development and rapid dissemination of integrated PET-CT scanners that allow functional and anatomic information to be obtained in a single examination represents an important advance in PET imaging technology, resulting in a synergistic improvement in the accuracy of interpretation of both PET and CT images. Accordingly, the performance of PET based on published studies performed with conventional PET scanners is now being reevaluated in light of emerging PET-CT results. This chapter will discuss the role of PET and PET-CT in the management of gynecologic cancers.
Patient Preparation and Imaging
Patient preparation for imaging of gynecologic tumors is similar to that for oncologic imaging generally. However, because of the potential for artifacts and interpretation errors related to intense FDG activity in urinary tract structures (e.g., streak artifacts, confusion of ureteral activity with lymph nodes), various interventions to minimize the amount of FDG in the urinary tract have been used in different clinical services. The current general use of iterative reconstruction algorithms instead of filtered back projection has eliminated most of the image artifacts related to intense urinary tract activity. Nevertheless, in some centers, urinary tract preparation is still performed for evaluation of gynecologic cancers. Most often this involves placement of a Foley catheter, intravenous administration of fluids (1,000 to 1,500 mL of 0.9% or 0.45% saline solution to be infused during the course of the study), and intravenous administration of 20 mg of furosemide before or after injection of FDG. The Foley catheter should be placed before injection of FDG to minimize radiation exposure to technical or nursing staff. Some investigators prefer the use of continuous bladder irrigation with a double-lumen catheter for the duration of the study.
The PET imaging methods used in patients with gynecologic tumors are also similar to those used for other cancers (see Chapter 19). For PET-CT, the administration of oral contrast agents is helpful for delineating bowel loops and makes image interpretation easier (1). There is no consensus regarding the need for administration of intravenous contrast agents (2). Several investigators have suggested that delayed PET imaging (>2 hours after injection of FDG) improves the sensitivity for detection of nodal metastasis in cervical cancer and peritoneal deposits in ovarian cancer (3,4,5).
Cervical Cancer
Worldwide, cervical cancer is the second most common cause of cancer-related deaths in women. Although less common in the United States, cervical cancer is still expected to account for approximately 10,370 new cancer diagnoses as well as 3,710 deaths in 2005 (6). Squamous cell carcinomas represent more than 90% of cervical cancers and originate in the surface epithelium of the cervix; adenocarcinomas represent approximately 5% to 9% of cervical cancers and originate in the cervical glandular tissue. Adenosquamous carcinoma is relatively infrequent and represents about 2% to 5% of all cervical carcinomas. Rare cervical sarcomas and small cell carcinomas account for the remainder.
Staging
Cervical cancer typically disseminates in a predictable fashion, with initial spread to local structures and regional lymphatics and later hematogenous spread to distant organs, such as bone and lung. The pattern of nodal metastasis is also predictable: tumor spreads from the primary lesion sequentially to pelvic lymph nodes, para-aortic lymph nodes, and supraclavicular lymph nodes. Cervical cancer is staged clinically based on the Fédération Internationale de Gynécologie et d’Obstétrique (FIGO) staging system. Involvement of a pelvic or para-aortic lymph node does not alter the FIGO clinical stage of disease, but indicates a worse prognosis and may have an important impact on therapy (7,8,9,10). Because of limitations of conventional radiologic techniques for evaluating lymph nodes, surgical assessment of para-aortic nodes is considered the gold standard. However, exploratory laparotomy and nodal dissection has not had a demonstrable impact on survival. Moreover, because of the morbidity associated with surgical staging, this procedure is not widely used; thus, the search for an accurate noninvasive staging method is an ongoing process.
FDG-PET appears to be well suited for imaging of cervical carcinoma. Most primary tumors, except for very small lesions, are readily seen on PET images and exhibit intense FDG uptake. In our experience, primary squamous cell carcinomas and adenocarcinomas have similar FDG avidity. In a review of 230 patients with cervical cancer (squamous cell carcinoma 200, adenocarcinoma 30), we found that the mean maximum standardized uptake value (SUVmax) of squamous cell carcinomas was slightly higher than that of adenocarcinoma, but the difference was not significant (11.7 versus 9.6) (unpublished data). However, because of its relatively poor spatial resolution and inability to assess parametrial invasion or involvement of adjacent organs reliably, FDG-PET is of limited value for staging of the primary tumor.
A number of studies have shown that FDG-PET is superior to conventional imaging methods for detecting metastatic disease, particularly lymph node metastasis (11,12,13,14,15,16,17).
Havrilesky et al. (17) recently reported a systematic review of the published literature up through 2003. They included only those studies involving 12 or more subjects who had PET performed with a dedicated scanner with specified resolution, and with clinical follow-up of 6 months or longer or histopathology as the reference standard. In patients with newly diagnosed cervical cancer, the pooled sensitivity of PET was 79% (95% confidence interval [CI], 65%–90%), and the pooled specificity was 99% (96%–99%) for detection of pelvic lymph nodes metastasis (17). Two studies were identified that each compared PET with magnetic resonance imaging (MRI) and CT (17). MRI had a pooled sensitivity of 72% (53%–87%) and pooled specificity of 96% (92%–98%), whereas CT had a pooled sensitivity of 47% (21%–73%) (there were insufficient data to calculate a pooled specificity). In four prospective studies in which histology after para-aortic lymphadenectomy was used as the reference standard, the pooled sensitivity of PET for the detection of para-aortic nodal metastasis was 84% (95% CI 68%–94%) and the pooled specificity was 95% (89%–98%) (17). In three of these studies, the inclusion criteria for study entry included a negative CT or MRI of the abdomen (17). Thus, the accuracy of conventional imaging could not be calculated. The fourth study did not require a negative abdominal imaging study prior to surgery (17). The sensitivity and specificity of MRI in the 12 patients who underwent aortic node sampling were 67% and 100%, respectively.
Havrilesky et al. (17) recently reported a systematic review of the published literature up through 2003. They included only those studies involving 12 or more subjects who had PET performed with a dedicated scanner with specified resolution, and with clinical follow-up of 6 months or longer or histopathology as the reference standard. In patients with newly diagnosed cervical cancer, the pooled sensitivity of PET was 79% (95% confidence interval [CI], 65%–90%), and the pooled specificity was 99% (96%–99%) for detection of pelvic lymph nodes metastasis (17). Two studies were identified that each compared PET with magnetic resonance imaging (MRI) and CT (17). MRI had a pooled sensitivity of 72% (53%–87%) and pooled specificity of 96% (92%–98%), whereas CT had a pooled sensitivity of 47% (21%–73%) (there were insufficient data to calculate a pooled specificity). In four prospective studies in which histology after para-aortic lymphadenectomy was used as the reference standard, the pooled sensitivity of PET for the detection of para-aortic nodal metastasis was 84% (95% CI 68%–94%) and the pooled specificity was 95% (89%–98%) (17). In three of these studies, the inclusion criteria for study entry included a negative CT or MRI of the abdomen (17). Thus, the accuracy of conventional imaging could not be calculated. The fourth study did not require a negative abdominal imaging study prior to surgery (17). The sensitivity and specificity of MRI in the 12 patients who underwent aortic node sampling were 67% and 100%, respectively.
False-negative results for detection of nodal metastasis are chiefly related to the limited resolution of PET and, thus, its inability to detect microscopic disease and small macroscopic tumor deposits. In a recent study that evaluated the sensitivity of FDG-PET by comparison with surgical lymphadenectomy in patients with early-stage cervical cancer, we found that the mean size of tumor deposits was larger in PET-positive pelvic nodes (15.2 mm; range 2 to 35 mm) than in PET-negative nodes (7.3 mm; range 0.3 to 20 mm) (18). False-positive results are most likely related to uptake of FDG in hyperplastic nodes or misinterpretation of physiologic activity in bowel or the urinary tract as nodal metastasis. The use of PET-CT has been shown to improve the accuracy of staging in various cancers, since the combined functional and anatomic information allows for a significant improvement in lesion localization and differentiation of physiologic FDG uptake from pathologic FDG uptake (19). This leads to a decrease in the frequencies of both false-positive and false-negative results.
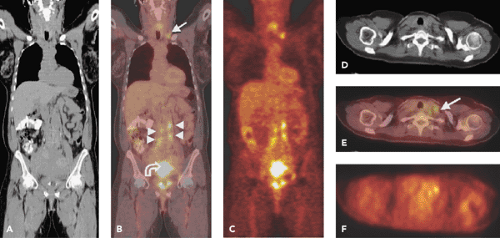
Our own studies have shown that FDG-PET is superior to CT and lymphangiography in showing unsuspected sites of metastasis in pelvic lymph nodes, extrapelvic lymph nodes, and visceral organs in patients with newly diagnosed advanced cervical cancer (20). FDG-PET showed abnormalities consistent with metastasis more often than did CT in pelvic lymph nodes (67% vs. 20%) and in para-aortic lymph nodes (21% vs. 7%) (Fig. 50.1). PET also showed disease in supraclavicular lymph nodes in 8% (21) (Fig. 50.2). These initial results have been sustained in subsequent evaluations (unpublished) of data from our prospective registry that now includes over 400 patients.
The role of PET-CT in staging of cervical cancer needs to be determined. The literature currently contains limited data on the use of PET-CT in cervical cancer; however, it is expected that PET-CT image fusion will allow for easier distinction of pathologic and physiologic tracer uptake and, thus, improve the accuracy of image interpretation (22). Based on the results in the literature to date, the United States Centers for Medicare and Medicaid Services in January 2005 approved coverage for use of FDG-PET in initial staging of patients with cervical cancer who have no evidence of extrapelvic metastatic disease on CT or MRI.
An evolving, competing imaging method for detection of metastatic disease in lymph nodes is MR lymphography with ultrasmall superparamagnetic iron oxide (USPIO) particles as the contrast agent. After intravenous injection, USPIO is taken up by macrophages in healthy lymph nodes and produces a loss of T1 signal, whereas the signal of metastatic tissue remains unchanged (23). Rockall et al. (24) recently have shown that USPIO-MRI is superior to standard size criteria for detection of metastatic lymph nodes in patients with endometrial and cervical cancer. In 44 patients, 768 pelvic or para-aortic lymph nodes were sampled histologically, of which 335 were correlated on MRI; 17 malignant lymph nodes were found in 11 of the 44 patients. MRI using USPIO criteria had significantly higher sensitivity than the size criteria for detecting lymph node metastasis on both a node-by-node basis (93% versus 29%) and a patient-by-patient basis (100% versus 27%). However, no significant differences were noted in the specificity or positive- and negative-predictive values between the two methods. The false-negative rate was relatively high with both methods, resulting in low positive-predictive values (61% versus 56%). The false-negative results were mainly due to failure in identifying involved lymph nodes in the parametrium and occurred only in patients with cervical cancer. Further studies in larger populations are needed to establish the use of this technique in clinical practice.
Directing Therapy
The use of FDG-PET in pretreatment clinical staging has had a significant impact on the therapeutic management of patients with cervix carcinoma. The standard treatment of advanced cervical carcinoma is radiotherapy with concurrent chemotherapy (25,26,27). Radiotherapy is directed at the pelvis to encompass primary disease as well as pelvic lymph nodes. The radiotherapy port is expanded to include the para-aortic lymph node region only in patients who have evidence of para-aortic nodal disease. Patients who have evidence of disease beyond the para-aortic lymph nodes at the time of initial diagnosis have little chance of a cure and receive palliative therapy. Based on the findings in the study of Grigsby et al. (21), we now routinely administer curative para-aortic irradiation to patients with CT-negative, FDG-positive para-aortic nodal disease, whereas no irradiation to this region would have been administered to such patients in the past before the use of PET to assess for para-aortic disease. Fourteen patients in that analysis had para-aortic disease detected by FDG-PET that was not detected by CT. These patients had
their radiation portals increased to include the para-aortic nodal region. Currently we are investigating the use of PET-CT-guided intensity-modulated radiotherapy (IMRT) to deliver higher doses to para-aortic nodes that have FDG-avid disease by PET-CT (28). Fused PET-CT images can be used to differentiate tumor from adjacent normal structures more reliably and thus allow for delivery of higher doses of radiation to the tumor while decreasing radiation dose to normal structures.
their radiation portals increased to include the para-aortic nodal region. Currently we are investigating the use of PET-CT-guided intensity-modulated radiotherapy (IMRT) to deliver higher doses to para-aortic nodes that have FDG-avid disease by PET-CT (28). Fused PET-CT images can be used to differentiate tumor from adjacent normal structures more reliably and thus allow for delivery of higher doses of radiation to the tumor while decreasing radiation dose to normal structures.
FDG-PET may also be useful in determining whether concurrent chemotherapy should be administered to patients with advanced-stage disease. A recent study from the Gynecologic Oncology Group (GOG 109) randomized patients with pathologically positive pelvic lymph nodes to either radiotherapy alone or to radiotherapy with concurrent and adjuvant cisplatin and 5-fluorouracil chemotherapy. The study demonstrated that there was both a superior disease-free and overall survival advantage when chemotherapy was added to radiation therapy (29). A subsequent report from this study demonstrated that there was no benefit to the use of concurrent chemotherapy in patients with only one positive lymph node (30). A similar finding was demonstrated by Grigsby et al. (31). In this retrospective analysis of 65 patients, there was no apparent clinical benefit to the use of concurrent chemotherapy with primary irradiation in patients who had no evidence of lymph node metastasis by FDG-PET. Thus, FDG-PET may be useful to select a subgroup of patients with locally advanced cervical cancer without evidence of lymph node metastases who may not benefit from the administration of concurrent chemotherapy. Larger prospective studies need to be done to confirm these results.
Prognosis
Several prognostic factors have been identified for patients with carcinoma of the cervix. These include patient age, tumor histology, tumor stage, tumor size, lymph node metastasis, and tumor hypoxia (32,33). In a study of 101 patients with newly diagnosed cervical cancer, Grigsby et al. (21) demonstrated that the lymph node status determined by FDG-PET is predictive of progression-free and overall survival in patients with cervical cancer. The 2-year disease-free survival was better predicted by PET evidence of lymph node involvement than by CT findings. Based on the imaging findings in the pelvic lymph nodes, the 2-year disease-free survival was 84% for CT-/PET- patients, 64% for CT-/PET+ patients, and 48% for CT+/PET+ patients (p = 0.05). Based on the imaging findings in the para-aortic nodes, the 2-year disease-free survival was 78% in CT-/PET- patients, 31% for CT-/PET+ patients, and 14% for CT+/PET+ patients (p ≤ 0.0001). None of the patients with PET+ supraclavicular lymph nodes survived 2 years. The PET-determined status of the para-aortic nodes was the strongest predictor of survival in a multivariate logistic regression analysis. These results suggest an opportunity to salvage some patients with para-aortic nodal metastasis defined by PET, as described above. In a recent review of data from 256 patients in our registry, we also found that the extent of lymph node involvement is inversely correlated with survival (34).
Recently, Miller and Grigsby (35) evaluated the usefulness of tumor volume measurement with FDG-PET in 57 patients with cervical cancer. Tumor volume and lymph node status determined by PET and FIGO stage determined by clinical examination were predictive of progression-free survival; tumor volume and lymph node involvement by PET predicted overall survival. The presence of lymph node involvement did not correlate with tumor volume. Most recently, we have demonstrated that the results of posttreatment surveillance FDG-PET studies in patients with cervical cancer are strongly predictive of patient survival (36). We have also found that FDG-PET demonstrated metastatic involvement in the left supraclavicular lymph nodes in 8% of our patient population; this finding has a positive-predictive value of 100% and indicates a dismal prognosis, despite aggressive therapy (37). Similarly, we found that the cause-specific survival for patients with FIGO stage IIIB carcinoma is highly dependent on the extent of lymph node metastasis demonstrated by whole-body FDG-PET at initial presentation (38). The 3-year estimates of cause-specific survival were 73% for those with no lymph node metastasis, 58% for those with only pelvic lymph node metastasis, 29% for those with pelvic and para-aortic lymph node metastasis, and 0% for those with pelvic, para-aortic, and supraclavicular lymph node metastasis (p = 0.0005). In a recent review of 96 patients with cervical cancer, we found that FDG uptake within the primary cervical tumor, as measured by the SUVmax, is predictive of disease-free survival in patients undergoing radiotherapy for cervical cancer (39). Thus, high FDG uptake may be useful in identifying patients who need more aggressive initial therapy.
In patients with cervical cancer, tumor hypoxia is an important prognostic factor indicating decreased overall and disease-free survival (33,40,41,42). Hypoxic tumors are resistant to radiotherapy and chemotherapy (43). Various therapeutic strategies directed toward tumor hypoxia have been unsuccessful, in part because a clinically relevant tool for determining and monitoring tumor oxygenation has not been available. The only established method for assessing the oxygenation status of tumors in vivo uses oxygen electrodes. However, this method is not clinically practical because it is invasive and subject to sampling errors, and can be used only in readily accessible tumors. We recently showed that a new tracer, 60Cu-labeled diacetyl-bis(N4-methylthiosemicarbazone) (60Cu-ATSM), accumulates avidly in hypoxic tissues but washes out rapidly from normoxic tissues (44). We studied 27 patients with advanced cervical cancer and demonstrated an inverse relationship between tumor uptake of 60Cu-ATSM and response to therapy (45) (and unpublished data). In addition, progression-free and overall survival were significantly worse in patients
with increased pretreatment primary tumor uptake of 60Cu-ATSM. In these patients, we found no significant difference in tumor FDG uptake in subjects with hypoxic (ATSM-avid) tumors versus those with normoxic tumors. Thus, 60Cu-ATSM-PET imaging of hypoxia provides prognostic information that cannot be derived from FDG-PET, and this examination has the potential to be used to monitor hypoxic-directed therapy in patients with hypoxic cervical cancer.
with increased pretreatment primary tumor uptake of 60Cu-ATSM. In these patients, we found no significant difference in tumor FDG uptake in subjects with hypoxic (ATSM-avid) tumors versus those with normoxic tumors. Thus, 60Cu-ATSM-PET imaging of hypoxia provides prognostic information that cannot be derived from FDG-PET, and this examination has the potential to be used to monitor hypoxic-directed therapy in patients with hypoxic cervical cancer.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree