Abstract
Pierre Robin sequence is characterized by retro/micrognathia, glossoptosis, and cleft palate (U-shaped); however, cleft palate is absent in up to one-half of all cases. Polyhydramnios may also be observed on prenatal ultrasound. Proper precautions should be taken if this diagnosis is suspected prenatally because of the increased risk for airway obstruction. Pierre Robin sequence occurs as an isolated finding in up to 65% of cases. Velocardiofacial syndrome, Stickler syndrome, and Treacher Collins syndrome are the most common genetic conditions associated with Pierre Robin sequence. Intellectual disabilities are not associated with isolated Pierre Robin sequence.
Keywords
micrognathia, retrognathia, cleft palate, glossoptosis
Introduction
Pierre Robin sequence (PRS) is a result of hypoplasia of the mandible leading to retrognathia or micrognathia, cleft palate, and posterior displacement of the tongue (glossoptosis). The classic cleft palate in PRS is a U-shape. Retrognathia and glossoptosis lead to airway obstruction of varying severity, occasionally requiring intubation or tracheostomy for airway management. The PRS may occur in isolation or as part of a syndrome.
Disorder
Definition
PRS is typically defined as a clinical triad composed of retrognathia (or micrognathia), glossoptosis and cleft palate; however, cleft palate may be absent in up to 50% of cases. Although PRS may occur as part of a syndrome, it is isolated in about 40%–65% of cases. The syndromes most commonly associated with PRS are velocardiofacial syndrome and Stickler syndrome.
Prevalence and Epidemiology
The most cited estimated prevalence of PRS is 1 : 8500, although ranges from 1 : 2000 to 1 : 30,000 have been reported. In one case series, the diagnosis was suspected prenatally in only 7% of patients.
Etiology and Pathophysiology
Hypoplasia of the mandible allows the tongue to be posteriorly displaced, thereby interrupting closure of the palate. Hypoplasia of the mandible may be caused by mechanical forces such as oligohydramnios, uterine anomalies or, rarely, amniotic bands. Several genetic syndromes have been associated with PRS; the three most common (accounting for 65% of syndromic cases) are Stickler (the most frequent), velocardiofacial, and Treacher Collins.
PRS is more commonly isolated. Much work has been done in the area of identifying the genetic defect(s) associated with PRS. Several chromosomal aberrations have been found in patients with PRS, including 2q duplication, 2q deletion, 4q deletion, 11q deletion,17q deletion, and 18q deletion. Genes of interest include SOX9 , implicated in cartilage differentiation, and collagen XI genes. However, the precise roll of genetics in development of PRS is unknown currently, and therefore definitive molecular testing for PRS is not available. Teratogenic exposures such as alcohol, methotrexate, valproic acid, and tamoxifen have also been reported in association with PRS.
Manifestations of Disease
Clinical Presentation
The anomalies associated with PRS lead to airway obstruction and feeding difficulties caused by airway obstruction of varying severity. Abnormalities of the hyoid bone have been documented and may be associated with more severe feeding abnormalities, even in the absence of severe upper airway obstruction. In nonsyndromic PRS, major cognitive developmental delay has not been demonstrated, although minor developmental delays may be present.
Imaging Technique and Findings
Ultrasound
Micrognathia: has been reported in first trimester ; three-dimensional imaging may be useful ( Fig. 137.1 ).

Fig. 137.1
Micrognathia seen on a sagittal view of the fetal face.
Polyhydramnios: may be seen in as many as 65% of cases.
Cleft palate: although observed in 50% of patients with PRS, may only be diagnosed prenatally in 25% ( Figs. 137.2 and 137.3 ).

Fig. 137.2
Coronal view of fetal face demonstrating a cleft lip.

Fig. 137.3
Three-dimensional image demonstrating a cleft lip.
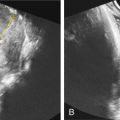
Glossoptosis: the tongue is an echogenic structure that should reach the anterior mandibular ridge. In a case report, the tongue could be demonstrated to reach only half way to the anterior mandibular alveolar ridge in the midtrimester ( Figs. 137.4 and 137.5 ).

Fig. 137.4
The normal appearance of the fetal tongue. The open arrow marks a normal fetal chin, and the closed arrow denotes a normal fetal tongue reaching the anterior mandibular alveolar ridge.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree