Sentinel Node Imaging in Head and Neck Tumors
Sandro J. Stoeckli
Christina M. Thuerl
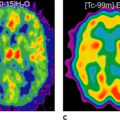
Sentinel node biopsy for head and neck squamous cell carcinoma seems to be able to accurately stage the cN0 neck and to select patients who benefit from elective neck dissection. The goal of sentinel node biopsy is to avoid unnecessary neck dissections in clinically N0 patients and thus decrease patient morbidity and health care costs. The average rate for detecting a sentinel node with lymphoscintigraphy and the intraoperative use of a handheld gamma probe is 95% to 100%. In the head and neck region, where lymphatic drainage patterns are of greater complexity and the primary sites close to the first-echelon node, integrated single-photon emission computed tomography (SPECT)–computed tomography (CT) imaging is thought to be of value in that it provides the surgeon with a more accurate roadmap by precisely defining the drainage basins and the sentinel node localization. SPECT-CT enhances topographic orientation and diagnostic sensitivity, with more sentinel nodes being detectable than by planar lymphoscintigraphy alone. We suggest that planar imaging should be accompanied by iterative reconstructed SPECT-CT to identify lymph nodes adjacent to the primary lesion. Such nodes are easily overlooked by planar lymphoscintigraphy and intraoperative gamma probes, as the high activity at the injection site can obscure their detection (see Fig. 35.1).
Introduction
Metastatic involvement of cervical lymph nodes is the most important prognostic factor for patients with head and neck squamous cell carcinoma. With the occurrence of neck metastases, the survival rate drops by 50%. Clinically apparent lymph node metastases have to be treated by surgery or radiation or a combination of both. The management of the cN0 neck is still controversial, although most centers advocate elective neck treatment, as the risk of occult metastases in head and neck squamous cell carcinoma is greater than 20% to 30% (1). Given these figures, as many as 70% of patients with a cN0 neck will undergo an unnecessary neck dissection. Sentinel node biopsy (SNB) has been introduced for the treatment of early oral and oropharyngeal squamous cell carcinoma and has shown promising results (2,3). Sentinel node biopsy seems to be able to accurately stage the cN0 neck and appropriately select patients who will benefit from elective neck dissection. The goal of sentinel node biopsy is to avoid unnecessary neck dissections in clinically N0 patients and thus decrease patient morbidity and health care costs.
Lymphatic mapping for the localization of the sentinel nodes includes preoperative lymphoscintigraphy. Lymphoscintigraphy assesses the individual lymphatic drainage pattern (4,5). In head and neck squamous cell carcinoma, the first successful sentinel node biopsy after lymphoscintigraphy was performed in 1996 (6). Since then, many other centers have adopted the technique and published promising results (7). The average rate for detecting a sentinel node with lymphoscintigraphy and the intraoperative use of a handheld gamma probe is 95% to 100%. Most authors stress that preoperative lymphoscintigraphy is pivotal in guiding the surgeon to the sentinel nodes and in visualizing unexpected drainage patterns (8). Different authors (9,10) share this opinion in the case of squamous cell carcinoma and melanoma of the head and neck, reporting on unpredictable sentinel lymph node sites that would not have been addressed by routine elective lymph node dissection.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree