Fig. 24.1
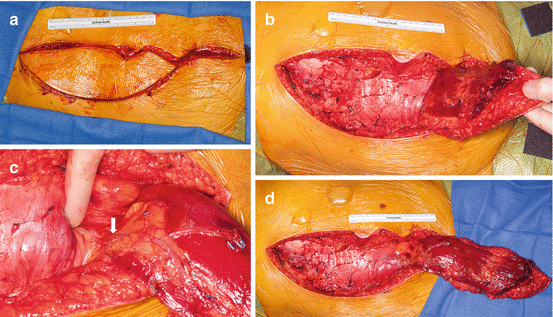
During an anterior exposure, the omentum is easily accessible and significant mobilization can be acheived through the anterior laporotomy incision (a). Following removal of a tumor, there is often a large potential space (b). The omentum can be mobilized and “tucked” into this space obliterating the dead space (c)
24.2.2 V–Y Advancement Gluteal Flaps
The V–Y advancement flaps are performed as a composite flap (fasciocutaneous and myocutaneous). Due to the loss of gluteal strength following the procedure, the flap is safer from a functional standpoint to perform in paraplegic patients but can also be used in ambulatory patients if the flap is modified to not include the muscle. The flap is based on the superior and inferior gluteal vessels. The use of this flap is contraindicated if there is concern about the patency of the gluteal vessels (and this may be the cases if there has been substantial preoperative gluteal radiation or preoperative embolization of the internal iliac vessels). In most cases, the donor site may be closed primarily, but in cases of very large flaps, the donor site can be skin grafted or left to heal by secondary intention. We prefer to use this flap (Fig. 24.2) only for patients undergoing an entirely prone procedure (caudal to S3). The tissue available with this flap is limited, and it is often not possible to obliterate larger deep pelvic spaces with this flap.
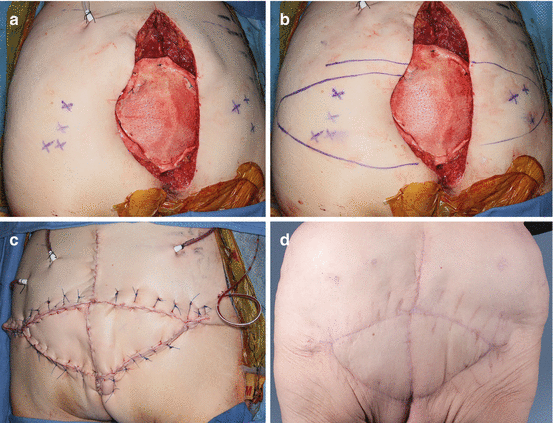

Fig. 24.2
For coverage of posterior-only sacrectomies, a V–Y advancement flap can be planned based on perforators from the gluteal vessels (a). Incisions are planned based on the location of the perforators (b), and the flaps can be elevated as either a fasciocutaneous or myocutaneous flap. The flaps are then mobilized to the midline (c). At 8-month postoperative, the flap has reliably healed (d)
24.2.3 Rectus Abdominis Musculocutaneous Flap
The rectus abdominis muscle can be elevated alone or as a composite flap with a skin paddle. The skin paddle can be elevated as a transverse rectus abdominis musculocutaneous (TRAM) or as a vertical rectus abdominis musculocutaneous (VRAM) flap, which can be either a distally based pedicle flap (inferior epigastric vessels) or microvascular free flap. We most commonly use a VRAM based on the deep inferior epigastric artery (DIEA). The DIEA arises above the inguinal ligament and lies superior to the peritoneum, but deep to the transversalis fascia. Once the pedicle enters the rectus sheath, it divides into the medial and lateral branches and located lateral to the muscle. The flap is elevated off the abdominal wall with both these perforators, with care taken to leave the flap attached the pubic ramus to prevent kinking of the pedicle.
The VRAM is the workhorse for reconstruction and can be used for a majority of soft tissue defects following sacrectomy. If there is a large skin defect, then we preferred to use a pedicled TRAM flap. Since these flaps are based on the inferior epigastric vessels, a detailed history of previous intra-abdominal surgery should be obtained in order to determine if the DIEA may have been previously divided (open appendectomy, inguinal hernia, colostomy, cesarean section, etc.). If there is a concern that the pedicle has been damaged, a duplex ultrasound or CTA should be performed to confirm patency.
The VRAM flap should be elevated prior to abdominal exploration. A large skin paddle should be planned in order to close the posterior soft tissue defect (Fig. 24.3). The rectus sheath is opened near the midline and elevated off the rectus abdominis muscle in the areas that are away from the skin island. Care should be taken to avoid the pedicle which lies on the undersurface of the muscle. The flap is left attached to the pubis and a stich is placed to mark superior orientation of the skin paddle. The flap is placed in a plastic bag or wrapped in a laparotomy pad and placed over the anterior portion of the lumbar spine and sacrum for easy identification during the posterior approach. The flap is then left buried in the abdomen until the posterior portion of the procedure is performed.