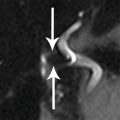
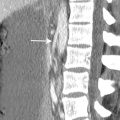
A. Chemotherapy toxicity
B. Gastric ulcer
C. Linitis plastica
D. Gastric volvulus
2 A 67-year-old patient presents with hematemesis. Endoscopic evaluation demonstrates marked fold thickening with ulcerations, and biopsy is consistent with lymphoma. The CT and PET scan obtained for staging is shown below. Regarding primary gastric lymphoma, which of the following statements is TRUE?


A. Most primary gastric lymphomas are Hodgkin lymphoma.
B. Lymphoma is the most common type of gastric malignancy.
C. Transpyloric spread of a gastric mass favors the diagnosis of lymphoma over adenocarcinoma.
D. Eradication of H. pylori infection may cause regression of low-grade MALT lymphoma.
3 A 38-year-old male presents with epigastric pain and has an upper GI barium examination. What is the next best step?


A. The findings are likely malignant, and endoscopy with polypectomy is recommended.
B. The findings are likely benign, and no further workup is necessary.
C. The findings are likely benign, but the patient should undergo endoscopy with biopsy, and colonoscopy should be considered.
D. The findings are likely benign, but endoscopy with polypectomy is still warranted.
4 A 34-year-old patient with a history of dyspepsia undergoes an upper GI barium study. Based upon the findings, what is the next best step?


A. The findings are likely benign, and no further workup is warranted in this young patient.
B. The findings are likely benign, and a repeat upper GI barium study is recommended after a trial of PPIs.
C. The findings are possibly malignant and endoscopy with polypectomy warranted.
D. The findings are possibly malignant and endoscopy with polypectomy recommended, and screening colonoscopy should be considered.
5a A 45-year-old male presents with left upper quadrant pain, melena, and a hematocrit of 30. An endoscopy reveals an ulcerated gastric mass. Immunohistochemistry of the biopsy is strongly positive for CD117. A CT scan is performed for staging purposes. What type of tumor is this most likely?


A. Leiomyosarcoma
B. Adenocarcinoma
C. Lymphoma
D. Gastrointestinal stromal tumor
5b A factor which determines for malignant potential of gastric GIST is
A. Size
B. Ulceration
C. Degree of enhancement
D. Adjacent mesenteric fat stranding
6 A 45-year-old female presents with epigastric pain. She undergoes a single-contrast barium UGI examination. Based upon the finding, which of the following statements is most accurate?


A. The ulcer appears benign because it extends beyond the expected lumen of the stomach.
B. The ulcer appears malignant because it is associated with a mass.
C. The ulcer appears malignant because it is located in the body of the stomach.
D. The ulcer is indeterminate and has no features suggestive of a benign or malignant nature.
7 A radiologist is performing an UGI study and sees a possible small ulceration in the stomach. The finding is subtle, and she chooses a smaller field of view (FOV) to better visualize the finding. As a consequence of this magnification, which of the following statements is TRUE?
A. The spatial resolution is decreased.
B. The dose to the patient is increased.
C. The minification gain is higher.
D. There is a decrease in the kVp.
A. Gastric erosions are best visualized on single-contrast UGI.
B. Gastric erosions are the most common radiographic manifestation of gastritis due to H. pylori infection.
C. Gastric erosions are most commonly located in the stomach fundus.
D. Gastric erosions are nonspecific and may be seen with a number of different etiologies.
9a A 56-year-old male with a history of smoking and peripheral vascular disease undergoes a CT angiogram for preoperative workup of leg claudication, during which an abnormal appearance of the stomach is incidentally noted. A urea breath test is reported as abnormal. What is the most likely diagnosis?


A. Helicobacter pylori gastritis
B. Ménétrier disease
C. Gastric lymphoma
D. Zollinger-Ellison syndrome
9b Regarding H. pylori infection in the United States, which of the following statements is TRUE?
A. H. pylori is an uncommon gram-positive rod that typically affects young patients.
B. H. pylori infection is frequently encountered in patients with gastric and duodenal ulcers.
C. H. pylori gastritis is readily distinguished from Ménétrier disease on upper GI studies.
D. H. pylori gastritis is an indolent process with little long-term significance.
10a A 41-year-old female presents with a history of chronic abdominal pain. A contrast-enhanced CT scan was obtained, followed by an In-111 octreotide SPECT study. What is the best diagnosis?




A. H. pylori gastritis
B. Ménétrier disease
C. Gastric lymphoma
D. Zollinger-Ellison syndrome
10b The mass identified in this patient is located in the gastrinoma triangle, which is bounded medially by the junction of the pancreatic neck–body and inferiorly by the junction of the second–third portions of the duodenum. What comprises the superior margin of the gastrinoma triangle?
A. Falciform ligament
B. Junction of common hepatic artery and gastroduodenal artery
C. Junction of cystic duct and common bile duct
D. Right portal vein
11 In these cases of gastric outlet obstruction, match the following images with the best diagnosis. Each answer may be used once only.
1. A 39-year-old male with a history of vomiting after an ERCP.


2. A 31-year-old male recently begun on a proton pump inhibitor with postprandial bloating.


3. A 78-year-old female with early satiety.


4. A 40-year-old male with severe acute abdominal pain.


A. Gastric carcinoma involving the antrum and duodenal bulb
B. Adult hypertrophic pyloric stenosis
C. Perforated duodenal ulcer
D. Duodenal hematoma
12 A 53-year-old female with a history of laparoscopic gastric band placement for morbid obesity presents with increased vomiting and poor oral intake. An upper GI study was performed. What is the most likely diagnosis?


A. Gastric band slippage
B. Gastric perforation
C. Intraluminal band erosion
D. Normal appearance
13 A 60-year-old female who had a sleeve gastrectomy performed 5 days ago undergoes a routine postoperative upper GI study. What is the best diagnosis?


A. Normal postoperative appearance
B. Staple line leak
C. Gastrocolic fistula
D. Gastric obstruction
14 A 50-year-old female with a history of laparoscopic Roux-en-Y gastric bypass presents with a history of persistent abdominal pain and poor weight loss. An upper GI study was performed. What finding is demonstrated?


A. Esophageal reflux
B. Gastrocolic fistula
C. Gastrogastric fistula
D. Efferent limb obstruction
15 An 86-year-old female with symptoms of mild early satiety has an upper GI barium examination. What is the name for the gastric abnormality seen?

A. Organoaxial rotation
B. Mesenteroaxial rotation
C. Borchardt hernia
D. Bochdalek hernia
16 A 26-year-old female presents with cramping epigastric pain. An upper GI and small bowel follow-through examination is performed. What is the most likely diagnosis?



A. H. pylori gastroduodenitis
B. Crohn disease
C. Eosinophilic gastroenteritis
D. Pancreatitis
17 A 74-year-old female with a history of hiatal hernia presents to the emergency department with acute onset of nausea and vomiting. An upper GI study was performed. Based on these results, the most appropriate treatment strategy is


A. Discharge to home with prescription for proton pump inhibitor
B. Obtain a CT scan of the chest and abdomen
C. Admit to medicine service for observation
D. Obtain surgical consultation for urgent operation
18 A 77-year-old male underwent endoscopic retrograde cholangiopancreatography (ERCP) for the evaluation of suspected choledocholithiasis and cholangitis. Multiple attempts to cannulate the papilla were unsuccessful due to angulation of the distal common bile duct. He had a percutaneous transhepatic biliary drainage catheter placed and improved clinically by the time of the CT scan below. What is the most likely cause of the finding below?


A. Clostridium infection
B. Ischemia
C. Iatrogenic from the ERCP
D. Benign pneumatosis related to underlying COPD
19 An 81-year-old male presents to the emergency department with a history of acute abdominal pain after several hours of severe intermittently productive retching. He becomes hypotensive, and a CT without contrast is obtained, due to renal impairment. What is the diagnosis?




A. Large sliding hiatal hernia with pneumobilia
B. Nasogastric tube perforation of the esophagus with mediastinal abscess
C. Large paraesophageal hernia with gastric ischemia and perforation
D. Achalasia with perforation
20 An image from an abdominal CT is shown. Which of the following statements is TRUE about the artifact in the stomach?

A. The artifact is a result of both image acquisition and reconstruction processes.
B. The artifact may be eliminated by slower scanning.
C. The artifact is caused by the presence of stationary gas bubbles.
D. The artifact is increased with solid food ingestion.
21 A 38-year-old female with epigastric pain undergoes an upper GI study. What is the most likely diagnosis?

A. Epiphrenic diverticulum
B. Gastric diverticulum
C. Slipped fundoplication
D. Gastric fundal ulcer
22 A 22-year-old male who presents with vague upper abdominal pain undergoes an upper GI barium examination. No additional lesions in the esophagus, stomach, or duodenum were identified on the examination. What is the most likely diagnosis?


A. Metastatic melanoma
B. Gastrointestinal stromal tumor
C. Lymphoma
D. Ectopic pancreatic rest
23 A 20-year-old female presents with a 2-week history of abdominal pain and nausea. On examination, she has a palpable periumbilical mass. She has a CT scan performed. What should be recommended as the next step in the evaluation?


A. Endoscopic evaluation
B. Surgical consultation
C. PET scan
D. Gastric emptying study
ANSWERS AND EXPLANATIONS
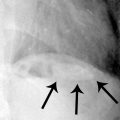
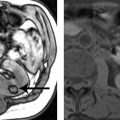
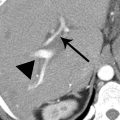
1 Answer C.Fluoroscopic spot image from a double-contrast upper GI demonstrates dilatation of the gastric body with nodular narrowing of the gastric antrum. Axial contrast-enhanced CT image demonstrates soft tissue thickening and narrowing along the antrum and pylorus. No ulceration is demonstrated, and the position of the stomach is normal. Gastritis from chemotherapy would not be confined to the antrum, and the more proximal wall does not appear to be involved. The imaging features are most compatible with linitis plastica, in this case from metastatic breast carcinoma.
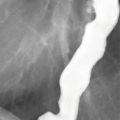
Linitis plastica is characterized by loss of normal gastric distensibility as a result of infiltrative tumor, leading to a “leather bottle” appearance of the stomach. The degree of gastric distensibility is variable, ranging from a quite subtle limitation to severe rigidity. Typically, this occurs in the setting of advanced scirrhous gastric carcinoma as in this case below from a different patient. Note the invariant gastric contours on the AP (left) and RAO (right) images.


A linitis plastica appearance can also be seen with lymphoma or metastatic disease (most commonly of breast and lung origin). Imaging plays an important role in diagnosis, as up to 30% of cases may have a false-negative endoscopic biopsy due to the tumor’s deep and infiltrative behavior.
References: Levine MS. Stomach. In: Levine MS, Ramchandani P, Rubesin SE (eds). Practical fluoroscopy of the GI and GU tracts. New York: Cambridge University Press, 2012:73–104.
Taal BG, Peterse H, Boot H. Clinical presentation, endoscopic features, and treatment of gastric metastases from breast carcinoma. Cancer 2000;89(11):2214–2221.
2 Answer D.Primary gastric lymphoma is the most common type of extranodal lymphoma, accounting for 50% to 70% of all primary gastrointestinal lymphomas. Gastrointestinal lymphoma is nearly always of the non-Hodgkin type. Lymphoma is much less common than adenocarcinoma in the stomach, accounting for only 1% to 5% of all gastric malignancies. Adenocarcinoma and lymphoma may have overlapping appearances on radiographic studies, with multiple manifestations including fold thickening, polypoid masses, and ulceration. Severe infiltration with lymphoma may even produce a linitis plastica appearance, although it is distinguished from that caused by adenocarcinoma by relative preservation of gastric distensibility. Note that while transpyloric spread is more common in lymphoma than adenocarcinoma, a tumor showing such transpyloric spread is still more likely to be adenocarcinoma, given its much higher prevalence.
Of the primary gastric lymphomas, a large proportion (50% to 72%) are mucosa-associated lymphoid tissue (MALT)–type lymphomas. MALT-type lymphomas are associated with chronic H. pylori infection and are classified into low-grade and high-grade histologic categories. Eradication of H. pylori infection with dual or triple therapy, which includes antibiotics and proton pump inhibitors, is the first line of therapy for low-grade tumors and may cause complete tumor regression. High-grade tumors likely originate from low-grade tumors that were not treated or represented treatment failures.
Radiographically, most low-grade MALT lymphomas may show superficial spreading lesions with mucosal nodularity, shallow ulcerations, and mild fold thickening on barium studies. High-grade tumors are associated with formation of masses or marked wall thickening.
References: Choi D, Lim HK, Lee SJ, et al. Gastric mucosa-associated lymphoid tissue lymphoma: helical CT findings and pathologic correlation. AJR Am J Roentgenol 2002;178(5):1117–1122.
Ghai S, Pattison J, Ghai S, et al. Primary gastrointestinal lymphoma: spectrum of imaging findings with pathologic correlation. Radiographics 2007;27(5):1371–1388.
Park MS, Kim KW, Yu JS, et al. Radiographic findings of primary B-cell lymphoma of the stomach: low-grade versus high-grade malignancy in relation to the mucosa-associated lymphoid tissue concept. AJR Am J Roentgenol 2002;179(5):1297–1304.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree