Clinical Presentation
The patient is a 73-year-old woman with a history of old fracture of the T12 vertebra secondary to prior motor vehicle accident. Patient was treated at the time of the fracture with thoracolumbar laminectomy and posterior fusion. The patient complains of progressive low back pain, lower extremity weakness, numbness, and pain. She has no bladder or bowel dysfunction. Upon examination, lower thoracic kyphosis is evident. She has mild to moderate motor weakness in both lower extremities proximally.
Imaging Presentation
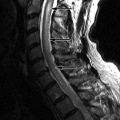
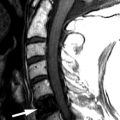
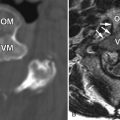
Magnetic resonance (MR) imaging obtained reveals kyphotic deformity of the spine at the T11-12 level and an old compression fracture of the T12 vertebral body with retropulsion of the T12 vertebral body impinging upon the ventral cord surface. Spinal cord syringomyelia extends from the T10 to the T12 level ( Figs. 76-1 and 76-2 ) .


Discussion
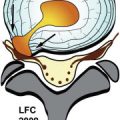
Hydromyelia (sometimes called primary cord syrinx ) refers to dilation of the ependymal-lined central canal of the spinal cord. Syringomyelia (or secondary cord syrinx ) is the term used to indicate a glial-lined cavity in the cord parenchyma without involvement of the central canal of the cord. The term syringohydromyelia encompasses both syringomyelia and hydromyelia and is used to include both cavitations occurring in the cord parenchyma and/or dilation of the central canal or an unspecified cavity in the cord. If the syrinx extends into the brainstem, this is referred to as syringobulbia .
Hydromyelia usually manifests in younger patients and is often associated with a developmental anomaly such as Chiari type 1 malformation, Chiari type 2 malformation (also called Arnold-Chiari malformation ), meningomyelocele, diastematomyelia, tethered cord, congenital scoliosis, basilar invagination, or hydrocephalus. In approximately 50% of patients with Chiari type 1 malformation, a hydromyelic cavity develops in the spinal cord. The hydromyelia may be of variable size, configuration, and length ( Figs. 76-3 and 76-4 ) . The hydromyelia may extend over a few vertebral levels or may extend the entire length of the spinal cord. Posterior fossa tumors can also cause dilation of the central canal of the spinal cord by obstruction of the obex or altered cerebrospinal fluid (CSF) flow dynamics near the foramen magnum region. Hydromyelia is believed to be due to interference in CSF flow in the spinal cord secondary to a mass, adhesions, or obstructing process in the posterior fossa interfering with CSF flow at the obex, foramen magnum, or C2-3 level. One theory suggests that when an obstructing or partially obstructing process exists at or near the foramen magnum level, caudal motion of the spinal cord, cerebellar tonsils, and brainstem, generates a piston-like effect that results in pulse-pressure abnormalities that drive the CSF downward into the central canal forming the hydromyelic cavity, assuming the central canal still communicates with the fourth ventricle. If the central canal does not communicate with the fourth ventricle, it is possible that exaggerated spinal pulse pressures may lead to increased transmedullary pressure gradients between the spinal subarachnoid space and the extracellular space within the cord, forcing CSF into the spinal cord via perivascular spaces and eventually leading to cord cavitation.


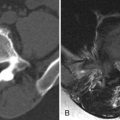
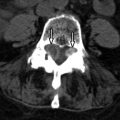
Syringomyelia is widely believed to be an acquired condition that is often idiopathic, but can be seen following trauma, spinal cord infarction, cord infection, noninfectious myelitis, arachnoiditis, or scoliosis, or can be associated with intramedullary tumors such as hemangioblastoma or ependymoma ( Figs. 76-5 and 76-6 ) . In these cases, the syrinx may form because of actual destruction of the cord parenchyma by the trauma, infection, or tumor. Alternatively, the syrinx cavity may form secondarily by underlying pathologic process interfering with the blood supply of the cord resulting in degeneration of spinal cord tissue and eventual cavitation. Uncommonly, a syrinx may develop adjacent to a large spondylitic ridge or large herniated disc compressing the spinal cord. However, in such cases, it is not known whether the cord compression is responsible for the syrinx formation or merely is a coexistent finding ( Figs. 76-7, 76-8, and 76-9 ) .




Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree