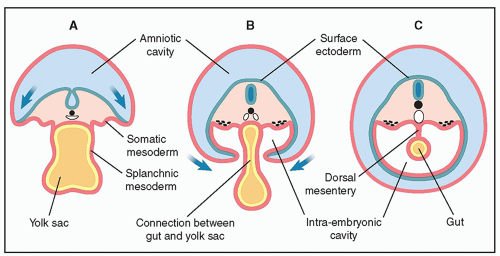
ileum, cecum, ascending colon, and proximal two-thirds of transverse colon. The hindgut, supplied by the inferior mesenteric artery, gives rise to the distal one-third of transverse colon, descending colon, sigmoid, rectum, and urogenital sinus. Because of lengthening of the gut and enlargement of upper abdominal organs, an intestinal loop from the midgut protrudes through the umbilical cord insertion into the abdomen at about the sixth week of embryogenesis (from fertilization). This intestinal loop returns to the intraabdominal cavity by about the 10th week of embryogenesis (from fertilization). Through the embryologic process, the midgut loop undergoes a series of three 90-degree counterclockwise rotations around the superior mesenteric artery.
multiplanar display, with reconstruction of planes for the specific evaluation of target anatomic regions displayed in tomographic view of axial (Fig. 12.10) or coronal (Fig. 12.11) planes. For more details on the use of 3D ultrasound in the first trimester, refer to Chapter 3 in this book and a recent book on the clinical use of 3D in prenatal medicine.4 Figures 12.5C and 12.9 show surface mode of the fetal anterior abdominal wall and Figures 12.10 and 12.11 show the use of multiplanar mode with plane reconstruction of axial and coronal views. In our experience, multiplanar mode can be of help especially in the transvaginal approach where transducer manipulation is limited (Figs. 12.10 and 12.11).
Table 12.1 • First Trimester Ultrasound and Ventral Wall Defects | ||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
additional anomalies of the heart, brain, kidneys, and spine. On occasion, the omphalocele can be as large or even larger than the abdominal circumference (Fig. 12.15). Follow-up of a first trimester isolated small omphalocele with a normal karyotype and nuchal translucency into the late second trimester is important because resolution of such cases has been documented in about 58% of fetuses.7 The presence of the liver in the omphalocele precludes resolution.
 Figure 12.14: Parasagittal (A) and axial (B) view of a fetus at 12 weeks of gestation with a large omphalocele (arrows). Note the presence of liver and bowel within the omphalocele. |
 Figure 12.17: Sagittal (A) and axial (B) planes of the mid-abdomen in color Doppler in a fetus at 12 weeks of gestation with trisomy 18. Note the presence of a small omphalocele (asterisk) in A and B and a thickened nuchal translucency (double headed arrow) in A. The use of color Doppler is helpful because it shows the umbilical cord arising from the top of the omphalocele in A (arrow) (compare with Fig. 12.12A) and a single umbilical artery in B (arrow). |
gastroschisis is rarely associated with chromosomal or structural abnormalities. There has been an increase in the prevalence of gastroschisis worldwide.13
 Figure 12.19: Schematic drawing (A) and corresponding 3D ultrasound image in surface mode of a fetus at 13 weeks of gestation with gastroschisis. Note in A and B the presence of bowel loops anterior to the abdominal wall (arrows). There is no covering sac around the bowel and the surface of herniated bowel appears irregular.
Stay updated, free articles. Join our Telegram channel
Full access? Get Clinical Tree
 Get Clinical Tree app for offline access
Get Clinical Tree app for offline access

|