Introduction
Noninvasive imaging during and following carotid artery and peripheral arterial interventions can improve procedural and patient outcomes. Duplex ultrasound imaging alone or in conjunction with extremity systolic blood pressure measurements provides accurate diagnostic information sufficient to identify technical problems and occlusive lesions that can occur following open surgical procedures and endovascular therapy. Color and pulsed Doppler imaging can be performed during interventions with the goal of improving the technical precision of carotid and extremity arterial procedures. Abnormalities at the repair site (stenosis, kinks, dissection, thrombus, low-volume flow) interfere with normal functional patency and contribute to early failure. Routine duplex testing has shown that residual stenosis is a common finding following percutaneous transluminal angioplasty (PTA; 5% to 25%) as well as infrainguinal vein bypass (10% to 15%). The incidence of arterial repair failure is low, 2% to 7% at 1 and 3 years, respectively, when duplex-detected lesions are corrected.
In outpatients, duplex testing is the cornerstone of a vascular laboratory-based surveillance program. Serial testing is performed initially to confirm that the repair simulates normal arterial blood flow and thereafter to detect developing stenosis caused by fibrointimal (myointimal) hyperplasia, a common mode of arterial repair failure, and to identify atherosclerotic disease progression. Repeat intervention based on duplex velocity criteria has been shown to increase long-term patency compared with a clinical follow-up regimen that relies on a recurrence of symptoms or signs of peripheral arterial occlusive disease.
Intraprocedural Duplex Ultrasound Assessment
Assessment of an arterial intervention by inspection, pulse palpation, and continuous-wave handheld Doppler signal analysis is safe and easy to perform but lacks diagnostic sensitivity for moderate to severe stenosis or intraluminal defects (dissection, intimal flaps and thrombus). Although fluoroscopic digital subtraction angiography (DSA) is considered a “gold standard” for arterial repair assessment, the technique is invasive, requires arterial puncture, entails radiation exposure, and has the risk of contrast-induced nephrotoxicity. Interpretation of DSA studies, even with multiple imaging runs, is prone to false-negative errors. Duplex testing has emerged as a preferred intraprocedural diagnostic technique because it provides real-time high-resolution imaging coupled with the physiologic information of Doppler waveform analysis. Essentially all open and endovascular vascular procedures can be evaluated with an appropriately selected transducer (either placed directly over the repair or transcutaneous) using a set of interpretative criteria ( Table 16.1 ). Endovascular interventions of the extracranial carotid, subclavian, renal, or mesenteric arteries should be assessed using either DSA alone, with catheter pullback systolic pressure measurement confirming a gradient of less than 10 mm Hg across the repair, or with intravascular ultrasound in selected cases. For open arterial surgical repairs, (carotid endarterectomy [CEA], renal/visceral artery bypass or endarterectomy, extremity arterial bypass), intraoperative duplex ultrasound imaging and the application of Doppler velocity criteria selected to have high diagnostic accuracy (sensitivity and negative predictive value rates of >90%) should be considered. Procedural duplex imaging can be completed within 5 to 10 minutes and is more convenient than completion arteriography.
| Procedure | Angiogram a to Measure Degree of Stenosis | Measurement of Systolic Arterial Pressure Gradient b | Duplex Ultrasound c |
|---|---|---|---|
| Open surgical repair | |||
| Carotid endarterectomy | Yes, <20% | Not used | Yes, PSV <150 cm/s |
| Renal bypass | Not used | Not used | Yes, PSV <180 cm/s |
| Mesenteric bypass | Not used | Not used | Yes, PSV <180 cm/s |
| Infrainguinal bypass | Yes, <30% | Not used | Yes, PSV <180 cm/s |
| Endovascular intervention-percutaneous transluminal angioplasty | |||
| Carotid stent-angioplasty | Yes, <20% | Not used | Yes, PSV <150 cm/s |
| Renal PTA | Yes, <30% | Yes, <10 mm Hg | Not used |
| Mesenteric PTA | Yes, <30% | Yes, <10 mm Hg | Not used |
| Iliac PTA | Yes, <30% | Yes, <10 mm Hg | Yes, PSV <180 cm/s |
| Infrainguinal PTA | Yes, <30% | Not used | Yes, PSV <180 cm/s |
| Vein bypass balloon PTA | Yes, <30% | Not used | Yes, PSV <180 cm/s |
a Criteria for acceptable residual stenosis, expressed as diameter reduction.
b Catheter measurement of pressure gradient during systole across angioplasty site.
c Peak systolic velocity threshold for revision of residual stenosis, used in conjunction with B-mode imaging criteria of stenosis and peak systolic velocity ratio of >2.0 at site of abnormality.
The type of abnormality seen during imaging varies with the procedure type, but a stenosis caused by residual disease, plaque dissection, or improper suturing is the most common abnormality seen with either duplex scanning or DSA. When color flow imaging and the Doppler waveform indicate the presence of a severe stenosis, the stenosis probably reduces volume blood flow and downstream pressure. In severe cases, this causes stasis proximal (upstream) to the stenosis and can promote platelet-thrombus formation and thrombosis. Failure to identify the abnormal repair increases the likelihood of procedure failure, an outcome that requires a secondary salvage procedure and is associated with increased morbidity and health care costs.
It is recommended that a vascular technologist participate in duplex ultrasound evaluations performed in the operating room or angiography suite. The technologist assists in instrument setup to optimize image resolution and color Doppler settings that are essential for high-quality imaging. For intraoperative assessment, a 10- to 15-MHz linear array transducer with a small footprint affords high-resolution imaging and can be placed within the surgical wound, directly on the repair site. For transcutaneous imaging of bypass grafts or extremity angioplasty/atherectomy procedures, 5 MHz or higher frequency linear array transducers are necessary to image the deeper-positioned vessels. Acoustic coupling necessary for duplex imaging is achieved by placing the transducer within a sterile plastic sleeve containing acoustic gel. Acoustic coupling to the patient is achieved with sterile gel on the prepped operative field or with saline in the wound.
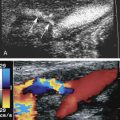
Reluctance to adopt routine intraprocedural duplex assessment is based on the false belief that testing is difficult to perform and to interpret, whereas clinical assessment and arteriography provide equivalent diagnostic accuracy. Intraoperative duplex assessment of infrainguinal vein bypass doubles the immediate revision rate compared with completion DSA, and early (30-day) thrombosis/revision rate is halved. The recommended velocity criteria thresholds for repair of a duplex-detected stenosis in a vein bypass graft vary. However, a peak systolic velocity (PSV) greater than 150 to 180 cm/s associated with a velocity ratio (Vr) greater than 2 across the imaged stenosis ( Fig. 16.1 ) has been shown to predict both lower extremity bypass and angioplasty site failure. In a blinded prospective trial, a Vr of 3 or above achieved a high predictive value for occlusion or future graft revision with a sensitivity of 71%, a value lower than that for a Vr of 2 or more. Revision rates based on duplex testing are higher with infrainguinal bypass to below the popliteal artery (17%), when arm (27%) versus saphenous (15%) vein conduit is used, and when percutaneous atherectomy is performed (20%) versus balloon (15%) or stent angioplasty (5%).
- •
Intraprocedural imaging can be performed after placement of the transducer in a gel containing sterile bag and ensuring acoustic coupling with:
- •
sterile gel if on top of the sterile field
- •
sterile saline in the operative wound
- •
- •
A small footprint transducer with high-frequency (10 to 15 MHz) range can be placed in a wound.
- •
A high-frequency transducer (5 MHz or more) can be used via a transcutaneous approach or placed on a graft conduit.
- •
A peak systolic velocity ratio of 2 or more and a peak systolic velocity above 150 to 180 cm/s are very sensitive indices of a residual stenosis.

Surveillance After Carotid Intervention
On the basis of prospective randomized clinical trials such as the Asymptomatic Carotid Atherosclerosis Study (ACAS) and North American Symptomatic Carotid Endarterectomy Trial (NASCET), carotid artery endarterectomy has been shown to be more effective than medical therapy in the prevention of stroke. Carotid artery stent placement has also been shown to be equivalent to CEA in the Carotid Revascularization Endarterectomy vs. Stenting Trial (CREST). The efficacy of CEA and carotid artery stenting (CAS) is highly dependent on completing the procedure with a low perioperative morbidity rate (<5%) and producing a durable repair with a low incidence of recurrent disease or occlusion.
Studies have documented that the rate of recurrent carotid artery stenosis following CEA is relatively low especially if an early imaging study does not indicate significant abnormality. However, monitoring the progression of internal carotid artery (ICA) stenosis with ultrasound on the nonoperated side may justify its use. When intraoperative or early duplex imaging of a CEA procedure shows the absence of a significant blood flow abnormality, the rate of restenosis is very low. However, the presence of a peak systolic velocity elevation of more than 150 cm/s or the presence of a luminal lesion of 2 mm or more should be considered indications for surgical revision.
B-mode ultrasound images following CEA will often show characteristic features. After endarterectomy, the normal intima-media stripe is absent at the beginning of the endarterectomy and often causes a step or shelf at the beginning of the repair site ( Fig. 16.2 ). The arteriotomy closure sutures can appear as bright reflectors in the anterior wall typically starting in the distal common carotid artery (see Fig. 16.2 ), but this finding may not be seen in all patients. As wall remodeling occurs over the subsequent weeks to months, wall thickening develops due to fibrointimal hyperplasia and a neointima develops ( Fig. 16.3 ). The clinical importance of the neointima is normally minor unless it causes severe lumen reduction and an increase in PSV ( Fig. 16.4 ). The development of a neointima is easily seen following a patch closure of the arteriotomy site (see Figs. 16.3 and 16.4 ). However, primary patch placement will prevent recurrent stenosis in many cases.



After CAS, the stent is often seen by using ultrasound ( Fig. 16.5 ) but this depends on the stent type and the extent of carotid artery wall calcification. Slight lumen narrowing may persist at the ends of the stent, but these anatomic changes should not result in significant velocity elevation. Typically, blood flow is laminar or only slightly disturbed at the site of the CEA and CAS. However, increased PSVs are very common at the site of stent placement despite the absence of any measurable lesion on arteriography. This is believed to be due to the loss of wall compliance at the stent site, a likely hypothesis based on the results of an in vitro study, and with a higher likelihood of increasing peak systolic velocities over time in CAS patients. Elevation of the external carotid artery PSV can occur at the origin of the external carotid artery and may be a normal finding or a harbinger of external carotid artery occlusion. This might also in part be due to plaque remodeling following stent placement ( Fig. 16.6 ).


Abnormal findings following CEA include blood flow disturbances (usually caused by an intimal flap or retained plaque), stenosis, and occlusion. Intimal flaps and retained plaque are immediately apparent postoperatively and should not be encountered on a follow-up basis if intraoperative sonography is performed. Typically, intimal flaps occur at the distal end of the endarterectomy, where the cut edge of the intima is subject to dislodgement by the flow stream moving toward the head (cephalad). This elevated intima can cause a tremendous blood flow disturbance and may ultimately lead to restenosis or thrombosis.
Fibrointimal (myointimal) hyperplasia (see Figs. 16.3 and 16.4 ) is a delayed complication that develops over a period of months after CEA or CAS (usually within the first 2 years). This process can result in either focal or diffuse narrowing at the endarterectomy/angioplasty site as well as within the stent and at the edges. Ultimately, this can lead to blood flow velocity elevation and poststenotic flow disturbances. The natural history of recurrent internal carotid stenosis caused by fibrointimal hyperplasia (smooth muscle and fibrous overgrowth of the tissue layer that replaces the intima following carotid intervention) is thought to be self-limited and associated with a lower risk of stroke or occlusion compared with atherosclerosis. Occasionally, some of the early postoperative lesions (10%) can show regression on serial duplex scans. Fibrointimal lesions tend to be smooth and occur within the first 2 years following the intervention. Lesions that develop after this time are likely to be new atherosclerotic plaques, with abundant collagen, foam cells, and calcium deposits.
Postintervention imaging focuses on detecting recurrent stenosis and determining whether an additional intervention or revision might be needed. The baseline PSVs can be falsely elevated following stent placement simply due to geometric factors ( Fig. 16.7 ). Modest increases in PSVs are common and need not indicate the presence of a 50% or more diameter narrowing. The Doppler velocity thresholds for confirming the presence of a high-grade ICA restenosis vary with the investigator ( Table 16.2 ). As shown in this table, the number of diseased vessels studied is low and the thresholds vary by the investigator. However, a PSV of 300 cm/s has been used as a marker of significant recurrent stenosis of greater than 70% diameter narrowing. Other plausible markers are a Vr of 4 or more, or an end-diastolic velocity (EDV) above 125 to 140 cm/s. Whether from fibrointimal hyperplasia or the development of new atherosclerotic plaque, high degrees of stenosis ( Fig. 16.8 ). are associated with an increased risk of ICA thrombosis and late stroke. Considering the potential for recurrence of carotid stenosis, duplex surveillance after CEA or CAS is considered a viable strategy ( Fig. 16.9 ). Testing intervals of 1 year for less than 50% stenosis and every 6 months for greater than 50% stenosis appear to be sufficient to detect the development of restenosis and to follow its progression. In the majority of patients, however, the main reason for duplex surveillance is to identify progression of contralateral ICA stenosis of more than 50% rather than to detect restenosis of the CEA or CAS site.

| Study | Comments | <20% Stenosis | ≥50% | ≥70% | ≥80% |
|---|---|---|---|---|---|
| Lal et al. | 90 bifurcations 6 with ≥20% | PSV <150 cm/s and ICA/CCA of ≤2.16 | |||
| Zhou et al. | 18 cases, 16 with ≥70% a | PSV 300 cm/s | |||
| Stanziale et al. | 118 cases; 20 with ≥50%; 13 with ≥70% | PSV 225 cm/s; ICA/CCA: 2.5 | PSV: 350 cm/s; ICA/CCA: 4.75 | ||
| Setacci et al. | 73 with ≥50% 22 with ≥70%; | PSV 175 cm/s | PSV: 300 cm/s; ICA/CCA: 3.8; EDV: 140 cm/s | ||
| Chi et al. | 13 patients 12 with ≥50% | PSV 240 cm/s; ICA/CCA: 2.75 | PSV: 450 cm/s; ICA/CCA: 4.3 | ||
| Lal et al. | 310 bifurcations 25 with 50%–79% 19 with ≥80% | PSV: 220 cm/s; ICA/CCA: 2.7 | PSV: 340 cm/s; ICA/CCA: 4.16 | ||
| Aburahma et al. | 144 cases 19 ≥50% | PSV: 224 cm/s; EDV: 88 cm/s; ICA/CCA: 3.43 | PSV: 325 cm/s EDV:119 cm/s; ICA/CCA: 4.5 |
a Sensitivity and specificity values very similar for different cut-points because of small sample size.


An early normal duplex scan of the CEA or CAS site (other than intraoperative) at 1 to 3 months is useful to exclude residual stenosis. The majority of patients demonstrate no stenosis after CEA/CAS, and if there is less than 50% contralateral ICA stenosis, duplex surveillance every 1 to 2 years should be adequate (see Fig. 16.9 ). A recent meta-analysis confirms that a normal baseline scan following CEA indicates that the likelihood of a significant stenosis developing in the next 2 years is very low. This finding was supported by a single center study of patients followed after CEA. Surveillance every 6 months is indicated in patients with residual or recurrent same side stenosis and contralateral ICA occlusion. The yield (i.e., intervention rate for severe stenosis) of duplex surveillance after CEA (5% to 7%) is less than after CAS (10%). Progression of contralateral disease, however, is five times more common. A policy of duplex ultrasound surveillance and reintervention for high-grade stenosis is associated with a low (<1%/year) incidence of ipsilateral hemispheric, disabling stroke. The development of hemispheric symptoms in the presence of ICA stenosis with a greater than 50% stenosis or the presence of asymptomatic disease progression to a high-grade stenosis (>70% to 80% stenosis; PSV >300 cm/s; EDV >125 to 140 cm/s; ICA/common carotid artery ratio >4) should prompt a recommendation for intervention in appropriately selected patients. Once detected by Doppler ultrasound, high-grade ICA stenosis should prompt consideration for reintervention, especially if the stenosis is rapidly progressing, is longer than 1 cm, or occurs following CAS.
- •
Intraoperative and early postprocedure evaluation after CEA have shown that the absence of the following findings is associated with a low risk of recurrent stenosis:
- •
2 mm or larger lesion on grayscale imaging
- •
a PSV above 150 cm/s
- •
- •
If present after endarterectomy and stent placement, progression of a contralateral lesion is a strong indication for carotid artery Doppler surveillance.
- •
Carotid artery stents tend to have increased PSVs. This is thought to be because of:
- •
geometric factors
- •
loss of compliance at the site of the stent
- •
- •
Doppler derived criteria for possible reintervention on a high-grade recurrent stenosis include:
- •
a PSV ≥300 cm/s
- •
an EDV >125 to 140 cm/s
- •
an internal to common carotid artery PSV ratio ≥4
- •
Surveillance After Peripheral Intervention
The major causes of lesion recurrence or procedural failure after peripheral arterial interventions are normally separated into three major categories: (1) technical failure if occurring in the first 30 days; (2) fibrointimal hyperplasia over the first month to 2 years following the intervention; and (3) progression of native atherosclerotic disease if occurring later. Fibrointimal (myointimal) hyperplasia is the same process as that seen in the carotid artery following interventions. It consists of smooth muscle cell proliferation and collagen matrix formation, producing occlusive lesions at anastomotic, vein valve, angioplasty, or endarterectomy sites. These lesions can progress to reduce blood flow and distal perfusion pressure. The development and progression of fibrointimal and atherosclerotic stenotic lesions can be monitored using serial duplex testing. Identification of a progressive stenosis permits elective intervention, usually with endovascular therapy because the lesion is focal (i.e., involving a short vessel segment). Duplex ultrasound surveillance has been shown to yield superior patency rates after infrainguinal vein bypass, peripheral angioplasty, and stent placement compared with clinical assessment alone. Surveillance is associated with a greater number of secondary procedures to repair typically asymptomatic high-grade (>70% to 80%) stenoses identified with Doppler ultrasound. The efficacy of surveillance has been best demonstrated following infrainguinal vein bypass (78% versus 53% assisted primary patency) with lesser levels of benefit shown after prosthetic lower limb bypass grafting, dialysis access placement, or carotid intervention. Infrainguinal prosthetic bypass graft surveillance is also recommended based on the higher diagnostic accuracy of duplex scanning (81%) when compared with a clinical evaluation with ankle-brachial systolic pressure index (ABI) measurement (24%) for identifying a graft stenosis that warrants repair. The accuracy of predicting graft failure or the need for revision was higher for femorotibial than for femoropopliteal grafts.
Timing of the initial vascular laboratory surveillance study varies with procedure type and whether or not an intraprocedural ultrasound study was performed and how it was interpreted. If the intraprocedural or predischarge ultrasound assessment was normal, surveillance may be initiated within 6 months after infrainguinal bypass. Procedures with residual stenosis by arteriography or ultrasound assessment should be evaluated earlier, especially if the predischarge duplex scan identified a moderate stenosis. In general, duplex surveillance at 6-month intervals is sufficient to detect developing stenosis. After 1 year, the incidence of failure due to fibrointimal hyperplasia decreases and surveillance intervals can be extended to 9 to 12 months for the detection of atherosclerotic disease progression or aneurysm formation.
- •
Saphenous vein bypass failure can be divided into three categories based on the time interval since the surgery:
- •
30 days or less: due to technical factors
- •
1 month to 2 years: due to fibrointimal hyperplasia
- •
after 2 years: due to progression of atherosclerosis
- •
- •
Follow-up intervals vary and should occur earlier if the predischarge ultrasound examination showed a residual blood flow abnormality.
Infrainguinal Bypass Assessment
Intraoperative assessment
The intraoperative scanning algorithm relies on real-time color Doppler imaging to identify lumen stenosis and sites of disturbed, turbulent flow. There are two approaches: following the administration of a vasodilator such as papaverine or “as is”.
Augmented assessment (vasodilation)
The entire bypass should be imaged as far as possible beginning at the distal anastomotic region and proceeding proximally ( Fig. 16.10 ). Before duplex scanning, papaverine hydrochloride (30 to 60 mg) can be administered into the conduit (with a 27-gauge needle) to vasodilate the runoff arterial bed and to augment graft blood flow. This technique, termed papaverine-augmented duplex scanning, improves diagnostic sensitivity for the detection and grading of residual stenosis severity. Use of a vasodilator drug is also useful to confirm the presence of low-resistance blood flow pattern in distal bypass graft and runoff arteries ( Fig. 16.11 ), which is a hemodynamic characteristic associated with successful placement of a lower limb bypass graft. Doppler velocity spectra are recorded using a Doppler angle of 60 degrees or less relative to the vessel wall and the sample volume placed in the center of the bypass conduit.



Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree