1 Introduction to Emergency Imaging
Observing and Interpreting
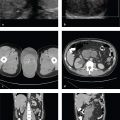
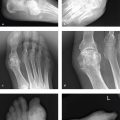
Some examinations, such as a radiograph of a simple fracture in a long bone, can be appreciated immediately and accurately. Others, especially those involving complex anatomic structures such as the hand, wrist, or foot and most cross-sectional examinations, require a structured approach to ensure that all elements of the study have been reviewed. In reality, most radiologists and other observers use a combination of immediate recognition, or “gestalt,” and a mental checklist, and the mix changes with experience. It is much easier to recognize an important finding if one has seen it before, preferably many times before.
Appreciating the significance of an imaging finding is as important as its recognition, and “normality” on a radiograph is a function of many factors, including age, body habitus and composition, radiograph or computed tomography (CT) image quality, and position. Experience and practice leads to both sensitivity in detecting subtle abnormalities and an understanding of whether a finding is truly pathologic.
Reporting
The imaging report is the radiologist′s work product. It consists of two major elements: a written description of all observations that support the diagnostic impression and a summary that contains one or several diagnoses and any necessary discussion or recommendations. The format of the report may vary depending on the type of study and the preferences of the radiologist or their institution, but it should always include the following:
Body part imaged
Technique
Indication and relevant history
Comparison studies (if any)
Findings
Impression
It is important to present one′s findings and conclusions in a clear, organized, and succinct manner. Unfortunately, many reports are hobbled by wordiness, jargon, and redundancy.
Reports should be complete, but the ratio of “signal to noise” should be as high as possible, especially in the emergency setting. No one has time to wade through excessive, meandering, or unnecessary description of findings not pertinent to the primary goals of the treating emergency physician: acute management, patient disposition, or safe discharge from the emergency department. Although every radiologist will develop a personal style, usually by emulating teachers and colleagues, application of some basic principles will result in reports distinguished by clarity, brevity, and meaning.
Describe findings anatomically, especially when reporting studies of anatomically complex regions, such as the neck and abdomen. Within this context, try to address the findings relevant to the clinical question early in the report, and note incidental findings later.
If many findings—such as multiple facial fractures, intracranial metastases, or enlarged lymph nodes—need to be accounted for on a single report, list each one on a separate line rather than in a densely packed paragraph. Summarize the pattern or condition in the report′s impression.
Avoid using “there is” before each finding. “No pneumothorax,” for example, delivers the same information as “There is no pneumothorax.”
Avoid “is seen,” “is noted,” “is demonstrated,” and the like. These are the equivalent of putting “there is” in front of each finding. Simply state the finding.
Avoid “of the.” It is usually possible (and preferred) to put an adjective in front of the noun it modifies. “The neck of the femur” is better described as “the femoral neck.”
Avoid abbreviations and jargon. You do not know who will be reading your report. MR can mean mitral regurgitation to one physician and mental retardation to another. It is best to spell out most words and use conventional anatomic terminology: “The first carpometacarpal joint,” for example, is understood by anyone who knows basic anatomy. Its synonym, “the basal joint,” is known to hand surgeons but not necessarily to psychiatrists or internists, who may be caring for the patient.
While eponyms make for useful shorthand, they should be used in addition to, rather than in place of, a clear anatomic description: “A transverse, extra-articular, fifth metatarsal fracture, one centimeter from the base (Jones fracture)” is preferable to “fifth metatarsal Jones fracture.”
Finally, if a word or phrase doesn′t add to the meaning of the report, delete it. Radiologists are not meant to create a mood, develop a complex story line, or vividly paint a character. Our aim is to efficiently and effectively interpret the visual evidence presented in order to support an accurate clinical diagnosis and help direct treatment.
Grading and Measuring
When a measurement is necessary to establish a diagnosis, or to provide the approximate size of a mass, it should be recorded in either one dimension (round masses/cysts) or three dimensions (oblong or complex masses). Specific measurements and grading assignments necessary for surgical planning are usually best left to the treating physician, who usually has direct access to images and considerably more detailed clinical information than the radiologist does.
Incidental Findings
“Incidentalomas”—cysts, nodules, osseous lesions, and visceral or other soft tissue masses—are frequently detected on imaging studies. Most are obviously benign, such as simple renal cysts or small ovarian cysts in reproductive-age women, and need not even be described. The radiologist should report any unexpected finding that could potentially endanger the patient in the future or that needs further imaging evaluation. At minimum, any patient with such a finding should be directed to appropriate primary or specialist physician referral. The radiologist should document that this has been communicated to the emergency physician in the report. Common incidental findings will be addressed by anatomic region in each section of this book. The most commonly encountered incidental findings include lung nodules and abdominal visceral cysts or masses.
Learning Radiology
Diagnostic radiology is a broad discipline, and the scope of essential knowledge can be daunting to the student or resident. It is helpful to define learning goals at different stages of training and to remember that learning radiology, like learning anything, is a cyclical process of returning to the beginning again and again. Because one aim of this book is to support the novice radiologist and the learning that takes place in the first year of residency, the following suggestions are presented for consideration.
As a first-year resident, one′s focus should be on learning the relevant anatomy for each rotation, learning to communicate results clearly both in reports and verbally, and acquainting oneself with the several hundred conditions likely to be encountered in the emergency setting. These also happen to be the most common diseases one will encounter in any but the most specialized practices. Since the first major step toward independence as a radiologist is beginning overnight call, it makes sense that one′s work for the first 6 to 12 months of residency should be directed at preparation for that experience.
Some suggestions for learning in the first year:
Interpret (and report) as many studies as you can by yourself. Watching other radiologists report studies is a poor substitute for coming to your own conclusions before reviewing them with a more experienced radiologist.
Read about the diseases you encounter during the workday. Keep a list.
Follow up uncertain findings (and some of the ones you feel certain about). Speak with clinicians when you can; check pathology and laboratory reports on patients whose studies you have interpreted to be sure of your impression.
Learn radiographic, CT, ultrasound, and magnetic resonance (MR) anatomy as it applies to image interpretation.
Practice “taking cases” with a colleague on a regular basis and from the beginning of training. You will learn the most from your fellow residents.
Read other radiologists’ reports, and pay attention to how clearly they express themselves. In your own reports, strive to develop concise written descriptions and terse, clear analysis of your findings.
Learn the basic physical principles of radiography, CT, ultrasound, MR imaging (MRI), and nuclear medicine.
Become acquainted with all common and many not-so-common emergent conditions.
Know the imaging indications and the most appropriate studies for evaluating common conditions.
Learn the various protocols for CT and MRI examinations and how to modify them to optimize a particular study.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree