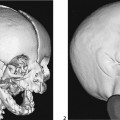
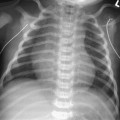
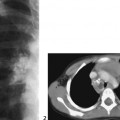
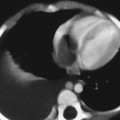
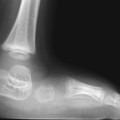
CASE 107 A newborn presents with respiratory distress and fluid return from the nose and mouth following the first few attempts at swallowing. The abdomen is noted to appear small. Attempts at placing a nasogastric tube failed, and the patient is sent for chest and abdominal radiographs. What should be done for this neonate? Figure 107A Figure 107B Chest radiograph shows the nasogastric tube coiled in the upper esophagus (Fig. 107A). Abdominal radiograph demonstrates a gasless abdomen (Fig. 107B). Esophageal atresia without evidence of a tracheoesophageal fistula (TEF), requiring definitive repair or gastrostomy tube prior to definitive repair Neonates with esophageal atresia may require a gastrostomy tube prior to definitive repair. Traditionally, the tube has been inserted via an open surgical approach. Recently, less invasive techniques for gastrostomy tube insertion, including the percutaneous image-guided gastrostomy, has been used in the pediatric population. The main advantage of this technique is the avoidance of a laparotomy. In patients with esophageal atresia without TEF, percutaneous gastrostomy tube insertion is problematic. The stomach is small and gasless, and it cannot be inflated as is usually done with a nasogastric tube. Access to the abdomen under radiologic guidance is therefore risky. A novel transhepatic approach is used to instill air into the stomach, which can then permit percutaneous gastrostomy tube insertion under fluoroscopic guidance.
Clinical Presentation
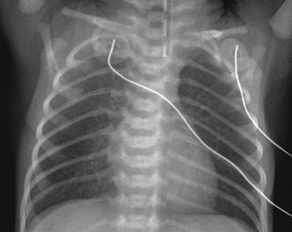
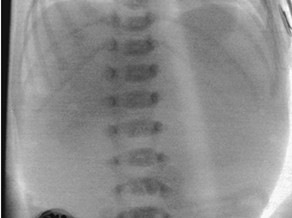
Radiologic Findings
Diagnosis
Differential Diagnosis
Discussion
Background
Indications
Imaging Findings
Technique
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree