13 Acute Cholecystitis, Cholelithiasis, and Choledocholithiasis
Daniel B. Gans, Jon C. Davidson, and Indravadan J. Patel
13.1 Introduction
Cholelithiasis, a common condition seen in approximately 10% of the Western population, is symptomatic in only approximately 20% of afflicted patients. 1 When gallstones do become pathologic, the associated conditions are potentially fatal, including acute cholecystitis, ascending cholangitis, pancreatitis, Mirizzi′s syndrome, and gallstone ileus. The advent of minimally invasive image-guided procedures has allowed for safer and, at times, more effective treatment for acute cholecystitis, cholelithiasis, and choledocholithiasis. Often, patients present to interventional radiology for treatment when their condition is too unstable for surgery or when their anatomy is too complex for endoscopic therapy. In such cases, radiologists have a unique opportunity to independently treat the patient or work in concert with the gastroenterology and/or surgical teams. This chapter aims to discuss the different treatment options for acute cholecystitis, cholelithiasis, and choledocholithiasis, including a historical perspective and the indications, contraindications, and techniques involved in treating such pathology.
13.2 Acute Cholecystitis
Acute calculous cholecystitis carries a low risk of mortality in patients younger than 80 years, approximately 0.5%; however, the mortality risk can be as high as 11.6% in patients older than 80 years. 2 The pathogenesis involves a gallstone or biliary sludge obstructing the cystic duct, resulting in increased intraluminal pressure. This pressure, in combination with cholesterol supersaturated bile, triggers an inflammatory response. Superimposed infection occurs in approximately 20% of cases, usually from enteric organisms such as Escherichia coli, Klebsiella species, and Streptococcus faecalis. If left untreated, potential sequelae include gangrenous cholecystitis, gallbladder perforation, cholecystoenteric fistulas, and/or gallstone ileus. 1
In comparison, acute acalculous cholecystitis, which accounts for 10% of all cases, is a much more fatal condition, with a mortality rate of 41% irrespective of age. The majority of these cases occur in critically ill patients or in patients recovering from trauma or nonbiliary tract operations. 3 Acalculous cholecystitis is thought to be the result of biliary stasis and gallbladder ischemia, commonly seen with fasting states or in patients receiving total parenteral nutrition. 4
13.2.1 Treatment
The first documented surgical percutaneous cholecystostomy (PC) was performed in 1867 by Bobbs, 5 , 6 and Langebuch performed the first open cholecystectomy (OC) in 1882. 7 For a century, these were the only treatment options for acute cholecystitis until Radder performed the first image-guided PC in 1980. In this case, Radder described an ultrasound (US) guided catheter drainage of a gallbladder empyema. 8 The first laparoscopic cholecystectomy (LC) was performed a few years later in 1985 by Mühe. 7
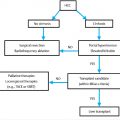
The treatment of choice for acute cholecystitis differs based on the severity of the cholecystitis and the presence of comorbidities. The Tokyo Guidelines offer a severity grading system that can be used to determine the optimal treatment strategy (▶ Table 13.1). 9 Using this grading system, Miura et al 10 created a flowchart for the treatment of acute cholecystitis (▶ Fig. 13.1).

In most cases, the treatment of choice for acute cholecystitis is LC. The choice between whether to perform an “early” cholecystectomy (during first presenting admission) or a “delayed” cholecystectomy (6–12 weeks after initial nonoperative management) remains under debate. Although multiple studies have demonstrated that early cholecystectomy is associated with less morbidity, 11 , 12 studies in which patients underwent PC followed by delayed cholecystectomy found that these patients had shorter mean postoperative hospital stays, a lower frequency of surgical complications, and a lower frequency of conversion to open surgery. 13
Although LC and PC are currently the most common treatment options, newer techniques are also being used. These include natural orifice transluminal endoscopic surgery (NOTES) and peroral endoscopic transpapillary/transmural drainage. NOTES cholecystectomy involves removal of the gallbladder through a natural orifice, via a transgastric, transrectal, or transvaginal approach. Peroral endoscopic transpapillary drainage entails placement of a double pigtail stent extending from the duodenum through the papilla and cystic duct into the gallbladder. 14 Transmural drainage is performed under endoscopic ultrasound (EUS), in which there is a direct puncture into the gallbladder through the small bowel wall. 15
Percutaneous Cholecystostomy
Indications and Contraindications
Although cholecystectomy is considered a safe procedure with a mortality risk of 0.8%, the mortality risk increases significantly in the presence of comorbidities, reaching upward of 30%. 16 In such cases, medical management is typically initiated first. If there is no clinical improvement after 72 hours of medical management, PC is considered to be a reasonable alternative to surgery. In a study of 82 critically ill patients with unexplained sepsis who underwent PC, Boland et al 17 observed substantial clinical improvement within 48 hours in 48 (59%) of these patients. Similarly, Boggi et al 18 found that 10 of 11 critically ill patients (91%) with acute cholecystitis who underwent PC had subsequent resolution of their sepsis. In a retrospective study of 57 patients with acute acalculous cholecystitis, a condition most commonly seen in the intensive care unit, Chung et al 19 observed resolution of symptoms in 53 (93%) patients after 4 days of PC tube placement.
Other conditions associated with acute cholecystitis that expose patients to higher perioperative risk include pregnancy 20 and diabetes mellitus. Cholelithiasis has long been associated with pregnancy, with acute cholecystitis occurring in approximately 1/1,000 pregnancies. 21 PC may be performed as a definitive treatment or a temporizing measure in such cases. Diabetes mellitus is a risk factor for acute acalculous cholecystitis, 22 a poor prognostic factor for acute cholecystitis, and is associated with complications of cholecystectomy such as biliary sepsis, gangrenous changes, and gallbladder wall perforation. 23 Therefore, PC should be considered in such cases.
Contraindications to PC are shown in ▶ Table 13.2. 20 , 24 , 25
Bleeding diathesis Interposing bowel Bile peritonitis Ascites Decompressed gallbladder due to decompression Gallbladder completely packed with calculi Gallbladder cancer (risk of seeding the track) |
Preprocedural Considerations
All cross-sectional imaging results should be reviewed before the procedure. Laboratory studies, including prothrombin time/international normalized ratio and a complete blood count, should be obtained. According to the Society of Interventional Radiology consensus guidelines, PC is considered a category II procedure (moderate risk of bleeding); therefore, an international normalized ratio ≤ 1.5 and a platelet count ≥ 50,000/μL are recommended. 26 Fresh frozen plasma, vitamin K, and/or platelets should be administered to meet these thresholds. The patient′s medication list should be reviewed, and pertinent anticoagulants should be withheld. The patient take nothing by mouth the night before the procedure to maximally distend the gallbladder and decompress the bowel. 27 If the patient has not received antibiotics before the procedure, a prophylactic antibiotic should be administered. Although there is no consensus on which medication to use, commonly used antibiotics include ceftriaxone, ampicillin/sulbactam, or vancomycin if the patient is allergic to penicillin. 28
Technique
Two approaches have been described: transhepatic and trans-peritoneal. With a transhepatic approach, a catheter is passed through the hepatic parenchyma into the gallbladder via the bare area of the liver (▶ Fig. 13.2a,b). In contradistinction, a transperitoneal approach involves cannulating the gallbladder directly through the fundus without traversing the hepatic parenchyma (▶ Fig. 13.2c,d).

Although the transhepatic route is generally the preferred method, several factors must be considered. The transhepatic route is associated with earlier tract maturation 29 but is considered riskier in the setting of bleeding diathesis. Additional potential risks include pneumothorax, hemobiliary fistula formation, and an increased theoretical risk of bile leak, although this remains controversial. 20 , 27 The transperitoneal approach is advantageous if this access will be used as a portal for future intervention, such as stone extraction or cystic duct cannulation. 27 Loberant et al 30 compared 59 patients who underwent transhepatic PC with 73 patients who underwent transperitoneal PC. There were no significant differences in short-term complications between the two groups, although a tendency toward the transhepatic approach was noted with CT guidance, while a transperitoneal approach was performed more commonly under US guidance.
For this procedure, the patient is typically placed in a supine position, with the right side elevated slightly (if possible). The cutaneous tissues should be prepared and draped before subcutaneous local anesthesia is administered. Two general techniques for PC have been described in the literature: the modified Seldinger technique and the trocar technique. 4 , 15 , 16 , 20 , 31 , 32 , 33 , 34 , 35 , 36 , 37 In the modified Seldinger technique, a small-diameter needle such as an 18- to 22-gauge Chiba needle is used to perform a micropuncture through the gallbladder wall under US or CT guidance. Confirmation of the needle′s location is achieved through aspiration of bile. A 0.018-inch guidewire is then advanced through the needle, and the needle is exchanged over the wire for a coaxial dilator. The coaxial dilator is then used to maintain access within the gallbladder for exchange of the 0.018-inch guidewire for a 0.035-inch guidewire. The coaxial dilator can then be exchanged over the wire for serial dilators and eventually a 6- to 12-Fr Cope Loop drain. 16 , 38 The trocar technique involves a combination drainage catheter, inner metal stiffener, and a sharp stylet. Under US or CT guidance, a single stick puncture is made into the gallbladder. The drain is advanced over the metal stiffener and sharp stylet into the gallbladder. 25 , 39 With both techniques, a Cope Loop catheter is preferred to prevent dislodgement from the gallbladder.
Each technique has advantages and disadvantages. The modified Seldinger technique allows for confirmation of access into the gallbladder before the formation of a large-bore cholecystostomy. Additionally, there are less severe consequences if nontarget puncture occurs. However, the multiple steps involved in the modified Seldinger technique make this technique less appealing when urgent drainage is required, when only one operator is present, or when the procedure is being performed at the bedside. Another disadvantage of the Seldinger technique is the risk of fluid leak while exchanging dilators. Therefore, the trocar technique can be advantageous under time constraints and when attempting to limit bile leak. However, when using this technique, nontarget puncture can result in more severe consequences due to the large size of the trocar. 38
There is very limited research comparing the outcomes of these two techniques for PC, although one study comparing the techniques for peritoneal dialysis catheter placement demonstrated a significantly lower risk of leak and longer catheter survival when placed via the modified Seldinger technique. 40
The final step of the procedure with either technique is to secure the catheter to the skin with sutures and sterile dressing and connect the catheter to a drainage container. Vital signs should be monitored for 4 to 6 hours after the procedure. A sample of bile may be sent for Gram stain and culture.
Outcomes
With technical success rates ranging from 90 to 100%, PC is an efficient and safe procedure. 29 , 35 , 41 , 42 , 43 Causes for unsuccessful PC drain placement include loss of wire access, 41 gallbladder full of calculi, 44 bile too thick for aspiration, 44 suboptimal patient cooperation, 29 lack of operator experience, 29 and porcelain gallbladder/thickened gallbladder wall. 45 Clinical response rates in studies have ranged from 59 to 94%, likely in part because of variations in patient populations and clinical response definitions. 17 , 18 , 19 , 33 , 34 , 35 , 41 , 42 , 44 , 46 , 47 , 48 The most common indicators of a clinical response included reduction in white blood cell count, defervescence, and reduction of abdominal pain. Most clinical responses were noted in the first 48 hours.
Although PC is considered a safe procedure, complications can occur either immediately after the procedure or slightly later. Potential complications are shown in ▶ Table 13.3. 31 , 34 , 35 , 44 In a study of 127 patients who underwent PC, the total complication rate was 13%, with vagal hypotension and bradycardia most commonly reported (combination occurring in total of 5 patients [4%]). 49 Vagal reactions can be treated with intravenous fluids and atropine. The most lethal complication observed was biliary peritonitis requiring surgical intervention, seen in 3 patients (2%). The 30-day mortality rate was 3.1%, although in each case the cause of death was sepsis and was not directly related to the procedure itself. More recent studies have reported 30-day mortality rates as high as 25%, although only 4% of deaths were attributed to gallbladder-related disease; most were due to preexisting comorbidities. 50
Immediate complications | Delayed complications |
Biliary leak and peritonitis Hematoma Vagal reaction Hypotension Pneumothorax Respiratory distress Severe pain Intestinal perforation | Tube dislodgement Tube obstruction Abscess formation Biliary fistula |
Follow-Up
While the drain is in place, flushing once or twice daily with 10 mL of saline is recommended to prevent obstruction. Based on the results of the bacterial culture, proper antibiotic therapy should be continued. If an obstructing calculus was present, percutaneous cholecystolithotomy can be considered (discussed later in this chapter).
“Delayed” or “interval” cholecystectomy can be performed 6 to 12 weeks after PC, particularly if the patient is too unstable for surgery at presentation. There is debate about whether this procedure is necessary; the percentage of patients undergoing delayed LC ranges from 3 to 87%. 51 In a retrospective study of 55 patients who had PC for acute cholecystitis, 28 patients (51%) underwent delayed LC. Conversion to OC occurred in only 4 (14%) of these patients, significantly fewer than in the emergent setting. Additionally, no bile duct injuries or major surgical complications occurred. 36 In another study, 11 patients with acute cholecystitis who underwent PC with delayed LC were followed, and conversion to OC was needed in only 1 patient (9%). 52 Although PC with delayed LC is associated with less risk and a lower rate of conversion to OC, one study demonstrated a significantly higher risk of conversion to OC and complications when delayed LC was compared with elective cholecystectomy. 51 One disadvantage of not performing delayed LC is the risk for recurrence. In one study of patients who received a PC drain but did not have delayed cholecystectomy, recurrence of gallbladder-related disease was found to be as high as 41%. 42 However, Chung et al 19 reported a lower risk of recurrence (7%) when a PC drain was placed for acute acalculous cholecystitis. Therefore, PC and eventual drain removal can be considered as definitive treatment in cases of acute acalculous cholecystitis, although interval LC may be necessary in cases of calculous cholecystitis due to the high risk of recurrence.
Cholecystostomy tube removal can only be performed when the tract has matured, which typically occurs approximately 3 to 6 weeks after initial placement. Tract maturity can be assessed beginning at 14 days after tube placement via “tractography.” The process involves placing a guidewire through the existing catheter and exchanging the catheter for a 6- to 8-Fr sheath with its tip at the skin site. Undiluted contrast is then injected through the sheath. The tract is considered mature if there is no leakage of contrast into the peritoneal cavity, subhepatic, subcapsular, or subdiaphragmatic spaces. In the presence of leakage, a new catheter of equal or greater size should be placed over the wire back into the gallbladder. 16 One study comparing time to maturation based on approach demonstrated that 93% of transhepatic PC tracts were mature at 14 days, with the remaining mature at 3 weeks. In comparison, only 13% of transperitoneal PC tracts were mature at 14 days, with maturation rates of 87% at 3 weeks and 100% at 4 weeks. 29
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree