3 Head and Neck
Approach
Head and neck conditions evaluated in the emergency department include facial trauma, blunt neck injury, orbital and peri-orbital inflammatory disease, neck masses, pharyngitis, and dental or neck abscesses. Most imaging involves face or neck CT, usually without contrast in the setting of trauma or with contrast for suspected inflammatory or neoplastic disease.
Facial trauma is common, and in this setting the radiologist′s goals are to describe fractures and their displacements, identify specific fracture patterns, anticipate injuries to adjacent soft tissue structures, and communicate findings effectively to the surgeon. In the face, the most important fracture patterns include nasal and naso-orbito-ethmoid (NOE), zygomaticomaxillary (ZMC) complex fractures, Le Fort fractures, orbital wall fractures, and mandibular fractures.
Noncontrast CT is the primary imaging study for facial trauma, and multiplanar reformations are essential for accurate interpretation. Three-dimensional reconstructions aid in surgical visualization and should be included if available. All facial fractures should be individually listed in the report and assigned to whichever fracture pattern they most closely correspond. It is unusual for an acute fracture to involve a sinus wall without intrasinus hemorrhage. Intraorbital air indicates an orbital wall fracture and potential for complicating orbital infection. If the pterygoid plates are intact, all of the Le Fort fractures are excluded.
Facial Trauma Checklist
First Look
Blood in sinuses?
Blood in mastoid air cells?
Pterygoid fracture?
Orbital emphysema?
Orbital hematoma or fat stranding?
Bone Survey
Frontal sinus
Nasal bones
Ethmoid air cells
Medial orbital walls (with attention to the nasolacrimal duct and attachment of the medial canthal ligament)
Orbital rim
Zygomatic arch
Zygomaticofrontal suture
Lateral orbital wall
Orbital floor
Orbital roof
Pterygoid plates (involvement of the pterygoid plates defines the Le Fort fractures)
Maxillary alveolus
Maxillary sinus walls
Mandible and temporomandibular joints
Teeth
Sphenoid sinus
Carotid canals
Mastoid air cells
Petrous temporal bone (cochleae, vestibule and semicircular canals, ossicles)
Soft Tissue Survey
Superficial soft tissues
Nasal septum
Sinus contents
Orbital fat (with attention to any orbital stranding, emphysema, or subperiosteal hematoma)
Globes
Optic nerves
Extra-ocular muscles
Brain (pneumocephalus, hemorrhage)
Indications for Neck CT Angiogram in Trauma
Blunt neck trauma is associated with clinically occult vascular injury in up to 3% of hospitalized patients. Early detection of vascular injury and therapeutic anticoagulation or endovascular occlusion can significantly reduce the incidence of stroke in this group. The Denver Modified Blunt Cerebrovascular Screening Criteria define a high-risk group of trauma patients for whom urgent CT angiographic imaging is indicated:
Direct signs of vascular injury (hemorrhage, bruit, hematoma)
Focal neurologic deficit or CT demonstrating acute cerebral infarct.
Le Fort II or III fracture
Cervical spine fracture
Basilar skull fracture involving carotid canal
Severe brain injury (diffuse axonal injury, GCS < 6)
Hanging injury
Neck contusion
Patients with penetrating injuries who do not undergo immediate surgical exploration should be imaged by CTA or conventional angiography. Typical vascular injuries in both blunt and penetrating trauma include dissection, occlusion, pseudoaneurysm, and arteriovenous fistula. Urgent CTA should also be considered in patients who present with focal neurologic findings, as vascular dissection with minimal or no trauma is an important cause of stroke, particularly in younger adults.
Approach to Inflammatory or Neoplastic Conditions
Suspected inflammatory or neoplastic conditions of the face and neck should be evaluated using postcontrast CT. Because of its anatomic complexity, neck CT interpretation is aided by grouping related structures.
Nontraumatic Face/Neck Checklist
Airway and Related Structures
Nasal cavity
Nasopharynx
Oropharynx
Hypopharynx
Larynx
Trachea
Lung apices
Esophagus
Thyroid gland
Soft Tissues and Bones
Muscles
Blood vessels
Lymph nodes
Cervical spine and skull base
Oral Cavity and Salivary Glands
Tongue
Tongue base
Mandible, maxilla, and dentition
Floor of mouth
Submandibular glands
Parotid glands
Orbits
Globes
Muscles
Optic nerve
Orbital fat
Orbital walls
Everything else
Skull base
Brain
Temporal bones
Temporal Bone Approach
Like the face and neck, the temporal bone is a complex structure, and a repeatable anatomic method is useful in order to avoid errors. One practical approach is to:
Address structures from outside to inside, beginning with the auricle and ending with the ossicles.
Evaluate the mastoid bone.
Address structures from inside to outside, beginning at the cerebellopontine angle, evaluating the internal auditory canal, cochlea, vestibule, and semicircular canals and ending with the facial nerve. The facial nerve, carotid canal, and jugular bulb canals can be dehiscent, and they should be described if so, as these anatomic variants can complicate surgery if not detected preoperatively.
Outside to Inside
Auricle
External auditory canal
Tympanic membrane
Tympanic cavity (hypo-tympanum and epitympanum)
Sinus tympani and pyramidal eminence
Ossicles and scutum
Mastoid Bone
Mastoid air cells
Mastoid antrum
Tegmen tympani
Tegmen mastoideum
Inside to Outside
Cerebellopontine angle and brainstem
Internal auditory canal
Cochlea, vestibule
Semicircular canals
Vestibular aqueduct
Petrous bone mineralization
Facial nerve
Carotid canal
Jugular bulb
Imaging and Anatomy
Imaging
Face CT (Noncontrast Helical)
Indications: Facial, orbital, or mandibular trauma.
Technique: 0.6-mm dataset with 1–2-mm axial, 2-mm sagittal, and 2-mm coronal reformations of head, face, and cervical spine. Oblique sagittal images, 1 mm, along the course of the optic nerve may be obtained for evaluation of orbital pathology. Images obtained from orbital roof to hyoid (unless obtained in conjunction with head and cervical spine CT).
Face CT (Helical + Contrast)
Indications: Orbital cellulitis, suspected facial abscess, mass.
Technique: 0.6-mm dataset with 1–2-mm axial, 2-mm sagittal, and 2-mm coronal reformations of head, face, and cervical spine. Oblique sagittal images, 1 mm, along the course of the optic nerve may be obtained for evaluation of orbital pathology. Images obtained from orbital roof to hyoid (unless obtained in conjunction with head and cervical spine CT).
Contrast: 60–100 mL at 1–2 mL/sec with 100-second delay.
Neck CT (Helical + Contrast)
Indications: Neck mass, abscess, adenopathy.
Technique: 0.6-mm dataset with 2–3-mm axial, 2-mm sagittal, and 2-mm coronal reformations of head, face, and cervical spine. Images obtained from orbital roof to thoracic inlet.
Contrast: 60–100 mL at 1–2 mL/sec with 100-second delay.
Neck CT Arteriogram
Indications: High-energy blunt trauma, suspected arterial dissection, penetrating injury.
Technique: 0.6-mm dataset with 2-mm axial, 2-mm sagittal, and 2-mm coronal reformations of head, face, and cervical spine. Images obtained from orbital roof to thoracic inlet.
Contrast: 60–100 mL at 3–4 mL/sec in arterial phase.
Temporal Bone CT
Indications: Skull base fracture, auditory or vestibular dysfunction, hemotympanum in trauma, mastoiditis, otitis media or externa.
Technique: 0.6-mm dataset with 0.6-mm axial, 1-mm sagittal, and 1-mm coronal reformations of the temporal bone in bone algorithm. Images obtained from petrous apex to C1.
Contrast (optional depending on indication): 60–100 mL at 3–4 mL/sec in venous phase (30–45-second delay).
Anatomy
Interpreting neck CT is aided by an understanding of the various deep compartments that are separated by investing fascia. Because the differential diagnosis of a neck mass depends primarily on its location, this approach is useful for establishing the likely nature of an inflammatory or neoplastic processes. These compartments include
Pharyngeal mucosal space
Parapharyngeal space
Retropharyngeal space
Pre- (or peri-) vertebral space
Carotid space
Parotid space
Masticator space
Submandibular space
Sublingual space
Because the fascia investing each of these spaces acts as a barrier to the spread of infection and because each contains specific tissues, locating a process to one space or another goes a long way toward making a diagnosis of head and neck disease.
The pharyngeal mucosal space (PMS) consists of the mucosa lining the upper aerodigestive tract and associate lymphatic tissues. Pharyngitis, tonsillitis, and most squamous cell carcinomas of the head and neck will be located in the PMS.
The parapharyngeal space (PPS) is important not for what it contains, which is mainly fat and small blood vessels, but because it is easily identified by its low density and displaced by masses in the adjacent pharyngeal mucosal space, carotid space, masticator space, and retropharyngeal space.
The retropharyngeal space (RPS) is a potential space containing lymph nodes located behind the dorsal PMS. It is an important route of spread for infections of the PMS, including tonsillitis and peritonsillar abscess. Infections involving the RPS can arise by contiguous spread from adjacent spaces and by suppuration of draining lymph nodes in the RPS. RPS infections can also extend inferiorly to the chest, leading to mediastinitis, a severe and potentially fatal condition.
The prevertebral space (PVS) is defined by the fascia that invests the vertebrae and prevertebral muscles. Infections and tumors located in the PVS usually arise from the disk or vertebral body. Because the PVS is contiguous with the epidural space, infection of the PVS can potentially lead to an epidural abscess.
The carotid space (CS) contains the carotid artery, jugular vein, lymph nodes, the carotid body, and the ninth and tenth cranial nerves. Pathologies specific to this space include carotid body tumors, CN9 and CN10 schwannomas, vascular disease (arteritis and thrombophlebitis), and arterial injuries and anomalies including pseudoaneurysms and arteriovenous fistula.
The parotid space (PS) surrounds the parotid gland, a number of lymph nodes, the proximal parotid duct, and the seventh cranial nerves. Parotitis, parotid sialadenitis, benign and malignant salivary gland tumors, lymphoepithelial cysts (seen in HIV-positive patients), and lymphadenitis occur here.
The masticator space (MS) contains portions of the mandible and the masseter, temporalis, and pterygoid muscles, as well as blood vessels and nerves. Most infections in this space are of dental origin. Neoplasms arising from muscle and bone can also occur in the MS.
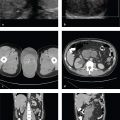
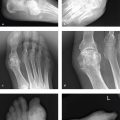
The submandibular space (SMS) is located inferior and lateral to the mylohyoid muscle. It contains the submandibular glands, second branchial cleft cysts, and lymph nodes. The sublingual space (SLS) is superior and medial to the mylohyoid and contains minor salivary glands as well as portions of the submandibular gland and duct. Infections in these spaces are usually odontogenic or submandibular in origin. Neoplasms tend to arise from minor salivary glands or the mandible ( Fig. 3.1 and Fig. 3.2 ).


Clinical Presentations and Differential Diagnosis
Clinical Presentations and Appropriate Initial Studies
Trauma
CT Face or Neck without Intravenous Contrast
– Frontal sinus/orbital roof fracture
– Nasal or nasal septal fracture
– Naso-orbito-ethmoid fracture
– Zygomaticomaxillary complex fracture
– Le Fort fracture
– Orbital wall (blowout) fracture
– Globe rupture
– Orbital hematoma
– Temporal bone fracture
– Skull base fracture
– Carotid or vertebral vascular injury
– Larynx fracture
Infection/Inflammation
CT Face or Neck with Intravenous Contrast
– Tonsillitis/pharyngitis
– Parapharyngeal or retropharyngeal abscess
– Dental or periodontal disease with abscess
– Sialadenitis
– Orbital cellulitis
– Infectious or reactive adenopathy (suppurative adenitis, mycobacterial disease, mononucleosis)
Mass
CT Face or Neck with Intravenous Contrast
MRI with Gadolinium
– Lymphoma
– Metastatic head and neck carcinoma
– Parotid or submandibular neoplasm
– Developmental cysts (thyroglossal duct cyst, branchial cleft cyst)
Differential Diagnosis
Clival/Skull Base Mass
Metastasis
Chordoma
Chondrosarcoma
Nasopharyngeal Mass
Prominent lymphatic tissue (normal in patients < 30, consider HIV in patients > 40)
Prevertebral space infection (osteomyelitis/diskitis)
Nasopharyngeal carcinoma
Juvenile nasopharyngeal angiofibroma (adolescent males)
Lymphoma
Tornwaldt cyst
Pharyngeal Mucosal Space Mass
Tonsillitis/abscess
Squamous cell carcinoma
Lymphoma
Retropharyngeal Mass
Abscess/phlegmon
Adenopathy/nodal metastasis
Lymphoma
Prevertebral Space Mass
Osteomyelitis/diskitis
Abscess
Chordoma/skull base chondrosarcoma/vertebral metastasis
Parotid Space Mass
Parotitis (diffuse enlargement)
Benign salivary gland neoplasm, 80% (pleomorphic adenoma, Warthin tumor)
Malignant neoplasm, 20% (mucoepidermoid, adenoid cystic carcinoma)
Intraparotid lymph node
Lymphoepithelial cyst (HIV)
Carotid Space Mass
Paraganglioma
Schwannoma
Carotid pseudoaneurysm/dissection
Jugular Foramen Mass
Schwannoma
Meningioma
Paraganglioma
Masticator Space Mass
Odontogenic abscess
Primary bone or muscle neoplasm (sarcoma)
Osteomyelitis
Submandibular Space Mass
Odontogenic abscess
Submandibular sialadenitis/abscess
Salivary gland neoplasm
Obstructed minor salivary gland (ranula)
Lymphadenopathy
Mandibular Cystic Lesion
Periradicular cyst (in carious teeth)
Dentigerous cyst (around crown of unerupted tooth)
Aneurysmal bone cyst
Ameloblastoma
Giant cell tumor
Sinus Disease with Bone Destruction
Invasive fungal sinusitis (mucormycosis, actinomycosis)
Carcinoma
Lymphoma
Wegener granulomatosis
Thyroid Mass
Benign nodule
Carcinoma
Parathyroid adenoma
Distal thyroglossal duct cyst
Multiple Enlarged Cervical Lymph Nodes
Lymphoma
Mycobacterial disease
Metastatic head and neck carcinoma
Lymph node hyperplasia
Low Attenuation Lymph Nodes
Mycobacterial disease
Metastatic head and neck carcinoma
Ocular Mass
Retinoblastoma
Melanoma
Retinal detachment
Intraconal Orbital Mass
Cavernous malformation
Optic nerve meningioma
Optic glioma
Inflammatory pseudotumor
Metastasis
Lymphoma
Hematoma
Extraconal Orbital Mass
Orbital abscess
Lacrimal gland tumor or inflammation
Dermoid
Lymphoma
Metastasis
Hematoma
Orbital Muscle Enlargement
Thyroid orbitopathy
Idiopathic orbital inflammation (pseudotumor)
Nasal and Naso-Orbito-Ethmoid Fracture
Nasal fractures result from direct impact, and deformity, laceration, or ecchymosis are often evident on examination. Epistaxis and CSF rhinorrhea indicate potentially severe injuries to the ethmoid bones or nasal septum.
Plain radiographs are rarely helpful. At best, they serve to document the presence of a fracture. If there is clinical concern for septal fracture or adjacent facial bone injury, or if operative reduction is planned, CT scanning is preferred and provides more comprehensive evaluation. Nasal fractures are often detected when CT is obtained for more severe injuries, and they often make up a part of a larger facial fracture complex. Most are oriented perpendicular to the nasal bridge, cross the nasomaxillary suture, and traverse the groove for the nasociliary nerve.
Because most simple nasal bone fractures are managed conservatively, clinical examination should include a search for septal deformity or hematoma. Although not specific for fracture, nasal septal hematomas are associated with significant morbidity and may lead to septal perforation or necrosis if untreated. Other consequences of failing to recognize a septal fracture are delayed nasal obstruction and cosmetic deformity. CT findings include fracture through the vomer or perpendicular ethmoid plate, and swollen paraseptal soft tissues. Treatment for significantly displaced septal fractures is surgical.
Naso-orbito-ethmoid (NOE) fractures are complex fractures of the nasal bones and the upper central mid-face due to direct impact to the nasal bridge. Fragments of the nasal bones, ethmoid air cells, and medial orbital walls are compressed and displaced posteriorly toward the sphenoid sinus. Cribriform plate and ethmoid roof fractures, when present, can be associated with anosmia, pneumocephalus, or CSF leak. Comminution and lateral displacement of the lacrimal bone can result in ocular, nasolacrimal duct, or nasofrontal duct injury. The medial canthal ligament, which anchors the globe, can be disrupted, with consequent enophthalmos, telecanthus, or ptosis. Traumatic nasolacrimal duct obstruction may require surgical repair.
CT scans should include reformations in three planes, with particular attention to the nasolacrimal ducts, attachment of the medial canthal ligament, and integrity of the anterior skull base. Three-dimensional reformations are valuable for surgical planning ( Fig. 3.3 ).

Zygomaticomaxillary Complex Fracture
The zygomaticomaxillary complex (ZMC) fracture results from a direct blow to the cheek and comprises the following fractures: (1) zygomatic arch, (2) lateral orbital wall (or diastasis of the zygomaticofacial suture), (3) inferior orbital rim and floor, and (4) anterolateral maxillary sinus wall. As they involve all four zygomatic articulations, the ZMC fractures effectively separate a malar fragment from the lateral facial skeleton. ZMC fractures can be variably rotated or depressed. Clinical findings include a palpable step-off at the inferior orbital rim or zygoma, subcutaneous emphysema, and hyperesthesia or anesthesia over the cheek (CN V2 distribution). Diplopia on upward gaze may be due to orbital edema or impingement of the inferior rectus muscle by an orbital floor bone fragment. Other clinical findings include pain with mastication from associated mandibular coracoid process and temporalis muscle impingement.
CT with multiplanar reformations locates the fracture components, the degree of malar fragment displacement and rotation, and any associated soft tissue or ocular injuries. The infraorbital canal (containing the maxillary nerve), orbital contents, nasolacrimal duct, and medial canthal ligament attachment should be specifically examined ( Fig. 3.4 ).

Le Fort Fractures
The sine qua non of a Le Fort fracture is involvement of the pterygoid plates, and all Le Fort fractures effectively separate a portion of the midface from the cranium. Le Fort I, II, and III patterns often occur in combination and can overlap with other complex fracture patterns such as mid-face smash, naso-orbito-ethmoid, and ZMC ( Fig. 3.5 ).

The Le Fort I fracture is a horizontal maxillary fracture that traverses the pterygoid plates, inferior maxillary sinus, and nasal septum, separating the teeth and maxillary alveolus from the upper face. This injury can often be diagnosed on physical exam based on isolated mobility of the hard palate. Le Fort I fractures always involve the inferior maxillary sinus walls and do not extend to the orbits or upper nasal bones.
Le Fort II is a pyramidal midface fracture that involves the maxillary antra and inferior orbital rims, intersecting at the glabella. The fracture follows an oblique course from the bridge of the nose to the pterygoid plates and separates the maxilla, anterior nasal bones, and anterior orbital floor and rim from the remainder of the skull. Le Fort II fractures do not involve the lateral orbital walls or zygomatic arches. The absence of an infraorbital rim fracture excludes a Le Fort II injury.
Le Fort III fractures separate the entire midface from the cranium and involve the pterygoid plates, the orbital walls, and the zygomatic arches. The fracture passes horizontally and posteriorly through the nasofrontal suture, frontomaxillary suture, lateral orbital wall, zygomatic arches, and pterygoid plates. Zygomatic arch fracture, best visualized on axial CT images, is unique to a Le Fort III fracture, and its absence excludes the diagnosis ( Fig. 3.6 ).

Midface Smash Injury
Midface smash injury is a general term applied to severely comminuted, high-energy impact, facial fractures that are not easily categorized as Le Fort, SMC, or NOE fractures. They can be loosely classified based on the their location as frontal, nasofrontal, or central, but these categories typically overlap. Frontal midface smash injuries are characterized by disruption of the frontal sinus; nasofrontal injuries involve the orbits, orbital apices, and ethmoidal roof; and central smash injuries involve the orbits, maxilla, and mandible. CT shows extensive facial bone comminution, often with posterior fragment displacement. Nonosseous structures that can be injured include upper cranial nerves, globes, extraocular muscles, nasolacrimal ducts, and sinuses ( Fig. 3.7 ).

Orbital Wall Fractures
Orbital wall fractures may be due to extension from a calvarial or skull base fracture, or they can follow direct impact from a fist or a ball to the eye socket. In this case an abrupt increase in intraorbital pressure leads most commonly to orbital floor failure with variable orbital fat herniation, inferior rectus or oblique muscle entrapment, orbital emphysema, and intrasinus hemorrhage. These are often referred to as orbital blowout fractures. Clinical findings, when present, include restricted upward and lateral gaze, subcutaneous emphysema, and diminished sensation in the distribution of the infraorbital nerve (V2). Enophthalmos is usually not evident acutely, but it can be seen in unrepaired fractures after initial swelling resolves. Rarely symptomatic bradycardia can result from stretching of the infraorbital nerve (oculocardiac reflex).
Medial orbital wall, or lamina papyracea, fractures often occur in conjunction with floor fractures, but isolated medial wall fractures are much less common than floor fractures or combinations. Most medial orbital wall fractures are small, of little consequence, and discovered on CT obtained for other indications long after an injury. When symptomatic, medial wall fractures are associated with orbital emphysema and potential medial rectus muscle entrapment, which can lead to diplopia on lateral gaze.
Orbital roof fractures are uncommon, and most are due to extension from frontal and calvarial fractures in major head injury.
CT defines the area and location of the fracture as well as any fragment displacement. Orbital fat herniation, extraocular muscle entrapment, and infraorbital canal involvement are easily identified. Muscle entrapment is evident clinically by diplopia on horizontal or vertical gaze, and corresponding CT findings include an acute change in the angle of the muscle as it passes through the orbit or impalement of one of the muscles on a bone spicule. Intra-orbital emphysema and retroseptal intra-orbital or subperiosteal hematoma should be sought, as the former indicates risk of orbital infection and the latter may lead to increased intraorbital pressures, with secondary globe ischemia or optic nerve damage.
Surgical intervention is usually indicated for severe fractures to prevent late enophthalmos and diplopia. Emergent surgical indications include symptomatic bradycardia and large orbital hematoma ( Fig. 3.8 ).

Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree