8 Transcatheter Management of Nonvariceal Lower Gastrointestinal Hemorrhage
Richard A. Baum and Stanley Baum
8.1 Introduction
Bleeding from the lower gastrointestinal (GI) tract has always presented a major challenge to clinicians as they attempt to identify the site of hemorrhage and treat the condition. If the bleeding is massive, colonoscopy is usually unsuccessful in identifying the source. If the site can be identified, surgery on an unprepared bowel presents another major obstacle. This chapter will discuss various causes of arterial acute and chronic lower GI bleeding such as diverticulosis, angiodysplasia, neoplasm, postoperative anastomoses, and inflammation.
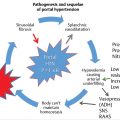
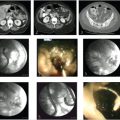
The transcatheter management of lower GI bleeding is a procedure that has stood the test of time. This life-saving procedure has been performed successfully for more than 50 years by two generations of interventional radiologists. What began with a rogue group of radiologists in the 1960s trying to control lower GI bleeding with direct intra-arterial injection of vasoactive drugs 1 , 2 , 3 , 4 has blossomed into a medical specialty with thousands of practitioners worldwide. Indeed, the beginning of angiography and interventional radiology as a subspecialty can be traced back to the need to develop techniques for the diagnosis and subsequent treatment of GI bleeding. Although the tools of the trade have changed over the past 50 years, 5 the basic approach and techniques remain the same (▶ Fig. 8.1).

The goals of transcatheter treatment of lower GI bleeding can be characterized by the type of bleeding and the durability of treatment. The ultimate goal of treatment is the permanent cessation of bleeding. Even for patients in whom durability of treatment cannot be achieved, a temporary result is acceptable, as this will allow patients to undergo elective surgery rather than an emergent procedure without proper bowel preparation.
8.2 History of Transcatheter Treatment of Lower GI Bleeding
In 1963, Nusbaum and Baum 6 demonstrated the feasibility of identifying experimentally created bleeding sites in the GI tract of dogs. Bleeding sites were created at various points of the GI tract by means of a catheter placed in a small segmental artery and passed through an enterotomy directly into the lumen of the intestine. After selective arteriography of the superior mesenteric artery was performed, the bleeding site was identified. By varying the diameter of the catheter used, different bleeding rates could be obtained. This technique was successful in demonstrating bleeding rates as low as 0.5 mL/min (▶ Fig. 8.2). 7

When selective mesenteric angiography was initially introduced for clinical use, it was used exclusively to establish a diagnosis of GI bleeding (▶ Fig. 8.3). The selective infusion of vasoconstricting drugs through the same catheter used for the diagnostic angiogram evolved as a natural outgrowth of diagnostic arteriography. The progression from diagnosis to a therapeutic application of the procedure heralded the beginnings of interventional radiology (▶ Fig. 8.4, ▶ Fig. 8.5).



Advances in catheters and wires over the years have also allowed for more expeditious catheterization of the mesenteric vessels, with catheters specifically designed to atraumatically cannulate the superior and inferior mesenteric arteries. The imaging chain has also seen dramatic improvement over the past half century. Static cut film imaging was replaced with rapid film changers in the 1970s. Digital subtraction angiography revolutionized the way vascular images were obtained in the mid-1980s and 1990s. 8 Image intensifiers were ultimately replaced with flat-panel digital detectors in the 2000s, greatly reducing ionizing radiation exposure to both patients and operators. Iodinated contrast agents have also seen great improvements over the years, greatly reducing their toxic effects.
The development of microcatheters has been particularly beneficial for the transcatheter treatment of lower GI bleeding. Before this development, pharmacologic treatment was useful if direct access to the bleeding site could not be obtained. Vasoconstrictors were applied to the upstream vasculature, and the resulting splanchnic vasoconstriction resulted in cessation of GI hemorrhage. With coaxial microcatheters, direct access to the injured artery is possible, allowing for a more varied and customizable treatment (▶ Fig. 8.6). 9

Unlike the stomach and duodenum, which have a redundant vascular supply, the large bowel mucosa is supplied by end arteries from the superior and inferior mesenteric arteries. Although there is collateral flow between medium-sized mesenteric and rectal vasculature, the colonic mucosa is fed by a delicate network of small arteries. This is why particulate embolization is not typically appropriate for managing hemorrhage in the lower GI tract. 10 Direct coil embolization of the injured vessel has become the standard treatment for most colonic bleeding. 10 , 11 , 12 , 13 , 14 , 15
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree