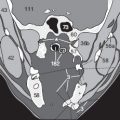
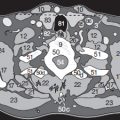
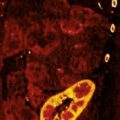
ABC-Primer of CT Evaluation
Occasionally, the beginner faces the question to decide whether a finding represents a true lesion or just an artifact. A contralateral comparison or a comparison with adjacent cranial or cauda sections can often be helpful. Furthermore, uncertainty arises when describing a lesion without familiarity with the appropriate vocabulary. This primer aims to remedy these problems.
A
General Approach to an Abnormality of the CT Morphology: | |
Where ? | Location, lateralization, relative position to other organs/vessels |
Size ? | Size (diameter in [mm, cm]; important, e.g., monitoring of therapy) |
Density ? | Relative to its surrounding: isodense (equal density); hyperdense (denser); or hypodense (less dense) |
Structure ? | Homogenous (e.g., fluids) or heterogenous / septate / geographic |
Shape ? | Tubular (vessels, muscles, …) or nodular (tumor, lymph nodes)? Reticular (resembling a net), striate or diffuse? |
Demarcation ? | Sharply marginated (more likely benign) or indistinctly marginated (infiltration into the surrounding, e.g., inflammation, malignancy) Caution: Partial volume effect can mimic an indistinct margin! |
Perfusion ? | No, peripheral, homogenous or heterogenous contrast enhancement |
Expansion ? | Space-occupying effect not invariably a sign of malignancy: e.g., large benign cysts can displace adjacent vessels |
B
Useful Terms, in Alphabetic Order | ( Application, Possible Significance) |
Air inclusions | Infection with gas-forming bacteria |
Ampullary | Dilatation of the renal pelvis |
Articular involvement | Evaluation of fractures ( risk of degenerative osteoarthritis) |
Bolus CT | Dynamic examination, often without table movement to assess the contrast enhancement pattern |
Bullae | Lung ( pulmonary emphysema) |
Capping | Periventricular abnormality in the white matter ( transependymal diffusion of CNS; sign of SAE) |
Cavity | Intrapulmonary hollow space ( tuberculosis) |
Central | In the center of a lesion or close to the hilum of parenchymatous organs |
Clubbing | e.g., of a limb of the adrenal gland ( adenoma, metastases) |
CM | Contrast medium, given orally, rectally or intravenously |
Concentric | Location of intravascular thrombi ( aortic aneurysm) |
Course of fracture lines | Evaluation with additional MPR ( surgical planning) |
Crescentic | Typical configuration, e.g., subdural hematoma or perihepatic effusion / ascites |
Defect | Pathologic phenomenon in opacified vessels / urinary collecting system |
Defect | In opacified vessels ( thrombus), in urinary bladder ( tumor, blood clot) |
Demarcation | Depending on the vascularization, lesions become visible only after administration of contrast medium |
Dense band | Band-like density ( lung, connective tissue: post-inflammatory, scar) |
Densitometry | Measuring of density ( differential diagnosis) |
Diffuse | Uniform, neither focal nor nodular; e.g., liver: hypodense hepatic steatosis (fatty liver) hyperdense hemochromatosis |
Dumbbell-like | Typical calcification pattern of benign hamartomas ( lung) |
Eggshell-shaped | Calcification pattern of perihilar lymph nodes (lung silicosis; porcelain gallbladder) |
Enhancement | Increased density due to accumulation of contrast medium |
Enhancement pattern | Perfusion pattern (homogenous, timely or delayed) |
Excentric | Intravascular location of thrombi ( aortic aneurysm) |
Fluid Levels | Phenomenon ( sedimented hematoma) or air-fluid levels ( paralytic ileus or intestinal obstruction) |
Fractures | Cortical step deformity, displacement, number of fragments, stability, articular surface? |
Ground glass density | Diffuse, slight increase density seen in perifocal edema ( fat, lung) |
Halo | Confined perifocal edema ( around inflammatory foci and metastases) |
Hemorrhagic | Blood-containing ( large infarcts, e.g., cerebral) |
Hilar fat | Benign criterion for lymph nodes ( nodal index) |
Honeycombing | Typical for vascular rarefaction in the lung ( emphysema) |
HRCT | High resolution computed tomography (thin sections) ( lung; also for MPR and 3D) |
Hyperdense | Denser than the surrounding tissue |
Hyperperfusion | Enhancement ( inflammation, hypervascular tumor) |
Hypodense | Less dense than the surrounding (dark fluid, fat, air) |
Imbibition | Striate to diffuse enhancement ( fatty tissue: scar, inflammation) |
Indentation | Blunt convex bulging / displacement of adjacent structures ( tumors) |
Indistinct | Outline of a lesion (see marginal indistinctness) |
Indistinct margin | Caused by inflammatory and tumorous infiltration of the surrounding tissue (caution: DD partial volume effect) |
Induration | Thickened fibrous tissue ( scar, pulmonary fibrosis) |
Infiltration | Perifocal extension of an inflammatory or malignant process |
Inflow effect | Incomplete mixing of contrast medium, can mimic intravascular thrombi |
Intramural | Located in the wall of a hollow viscus ( gas, tumor) |
Iris effect | Centripetal enhancement ( hepatic hemangiomas) |
Isodense | As dense as … (= isointense) |
Jet effect | Inflow of opacified urine from the ureter into the urinary bladder |
Lacuna | Lacunar defect ( late stage after cerebral infarct, isointense with CSF) |
LN | Lymph node (for size see checklists, hilar fat) |
Lymphangiomatosis | Ground glass-density ( pulmonary parenchyma, breast carcinoma) |
MPR | Multiplanar reconstruction of various image planes (sagittal, coronal diagnostic evaluation of e.g. fractures) |
Multiphase technique | Data acquisition during early arterial, portovenous or late venous passage of the contrast medium bolus ( spiral CT of the liver) |
Multislice | New multislice technique consisting of simultaneous acquisitions of several sections in spiral mode |
Mural thickness | Single or multiple layers (wall of a hollow viscus: ischemia, inflammation) |
Narrowed parenchymal rim | Renal atrophy (degenerative, hydronephrosis) |
Necrosis | Central, hypodense or homogenous liquefaction |
Nodal index | Longitudinal-transverse diameter ratio (characterization of lymph nodes) |
Nodular | Nodular configuration ( lymph nodes, tumors, adenomas), miliary < granular < fine-nodular < large-nodular < confluent ( pulmonary interstitium) |
Obliterated | Surface of cerebral gyri ( cerebral edema, DD: child) or pancreas outline ( acute pancreatitis) |
Osteolytic | Destruction of bony matrix ( metastases, multiple myeloma) |
Osteoproliferative | Osseous apposition ( degenerative), less frequent due to sclerotic metastases |
Partial volume effect | Effect of partial volume (causes apparent indistinctness) |
Patchy | Parenchymal perfusion pattern in the spleen during the early arterial phase |
Perifocal | Circular around a lesion (edematous zone) |
Perihilar | Topographic description of an intrapulmonary lesion |
Peripheral | Along the periphery, in contrast to central |
Pitch | Ratio of table feed per rotation and section thickness ( spiral technique, see p. 8 / 9) |
Pixel | Picture element (image formation, see p. 14) |
Plaque | Intravascular ( arteriosclerosis), pleura-based ( asbestosis) |
Polycyclic | = scalloped, cauliflower-like ( hilar lymph nodes of the lung, e.g., Boeck’s disease) |
Popcorn | Typical pattern of benign calcifications ( lung) |
Process | Favored term for “I don’t know what is means” |
Pseudocysts | chronic pancreatitis |
Pulsation | Can induce artifacts along vessels ( aortic aneurysm) |
Rarefaction | Less vessels per pulmonary volume ( emphysema, S/P lobectomy) |
Respecting soft-tissue planes | Lacking in malignant tumors or advanced inflammations (no longer respecting natural borders => infiltration) |
Retention cyst | Convex projection into the paranasal sinus, homogenous |
Reticular | Net-like pattern ( fibrosis of the pulmonary interstitium) |
Retrocrural | Preferred posterior paravertebral lymph node station |
Risk of herniation | Internal herniation of brain stem due to increased intracranial pressure |
ROI | Region of interest ( densitometry) |
Round lesion | Focal space-occupying lesion (only intrapulmonic) |
Scalloped enhancement | Peripheral contrast enhancement ( glioblastoma) |
Site of predilection | Preferred site for certain changes ( lymph nodes, metastases) |
Sludge | Thickened bile ( cholestasis, cholecystitis) |
Space-occupying process | Tumor of unknown nature (ubiquitously applicable) |
Spindle-shaped | Biconvex configuration ( aortic aneurysm; epidural hematoma) |
Spiral CT | Acquisition of a 3D data set with continuous table feed and any section reconstruction, see p. 7 |
Stellar | Hypodense star-like figure ( FNH of the liver) |
Stellate | Septation ( echinococcal cyst) |
Stent | Short tube of various materials to stent vessels, ureter or common bile duct |
Step deformity | bony cortex ( fracture diagnosis) |
Structure | Non-descriptive term of a lesion, try to use more precise term |
Subcarinal | Preferred lymph node station |
Timely | Symmetric and timely renal enhancement and excretion of contrast medium = normal |
Triangular | Wedge-shaped ( typical infarct pattern, scar residue) |
Tumor extension | Renal vein or vena cava ( renal tumor) |
Vascular configuration | Normal configuration of the pulmonary hila |
Voxel | Volume element (image formation, see page 14) |
Wedge-shaped | Triangular configuration ( typical infarct pattern, scar residue) |
Related posts:
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree