Cervical CT
Whenever there is no contraindication, CT examinations of the neck are carried out after i.v. administration of CM. Malignant and inflammatory processes can be depicted more accurately with the aid of CM. Adequate enhancement of cervical vessels requires higher doses of CM than, for example, in CTs of the head. In spiral CT, the injection of CM must be precisely timed to the acquisition of data. There are specific recommendations and suggested schemes for CM injection at the end of the manual.
Selection of the Image Plane
In an analogous manner to head CT, a sagittal planning topogram (scanogram) at lower resolution is obtained first. The transverse (axial) levels and gantry angulation are determined from this topogram ( Fig. 64.1 ). Usually sections of the neck are obtained using a 4–5 mm thickness. The axial images are obtained and printed as viewed from caudally so the right lobe of the thyroid is imaged to the left of the trachea, the left lobe to the right.
Images should be obtained with a small-scan field-of-view to optimize detail in smaller structures in the neck. As the thoracic inlet is approached during the scanning, the scan field-of-view is increased to include possible abnormalities in the clavicular fossa and the axilla.
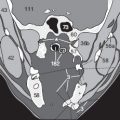
Artifacts caused by dental prostheses (3) usually obscure surrounding structures (*) in only one or two levels ( Fig. 64.2a ). It may be necessary to carry out a second acquisition at another angle ( Fig. 64.2b ) to reveal areas hidden by artifact (*).



Systematic Sequence for Readings
We have already recommended a systematic approach with which to read CT scans of the head (see p. 26). For cervical CTs there is also no ‘one and only’ approach. The checklist presented here was developed through experience and is just one of many options for the beginner. Each examiner is free to set up his or her own checklist and strategy.
During neck imaging, separate hard copies at bone windows are rarely printed owing to cost. The radiologist must remember to check images at bone windows on the screen for fractures or lytic lesions.
Checklist for Reading Cervical CT Images
Symmetry of neck musculature? |
Condition and clarity of fat? |
Normal perfusion of vessels? |
Thromboses or atherosclerotic stenoses? |
Symmetry and definition of salivary glands? |
Thyroid parenchyma homogeneous and without nodules? |
Any focal pathologic enhancement with CM? |
Narrowing of the tracheal lumen? |
Assessment of lymph nodes? Number and size? |
Cervical vertebrae examined in bone window? |
Vertebral canal patent or narrowed? |
The radiologist quickly reaches the limits of CT resolution (perhaps also of his/her anatomic knowledge) when trying to identify all of the different neck muscles. We have therefore reduced the amount of detail in the accompanying drawings so that smaller muscles are grouped. Single muscles have little clinical relevance and thus the legends to these images refer to combined muscle groups, e.g. the scalene muscles, the erector spinae muscles. Readers who want more anatomic detail should consult the relevant literature [5, 31].
Cervical images usually begin at the base of the skull and continue caudally to the thoracic inlet. The cranial sections ( Figs. 65.1–65.3 ) therefore include the maxillary sinus (75), the nasal cavity (77), and the pharynx (176). Dorsal to the pharynx lie the longus capitis and longus cervicis muscles (26), which extend caudally. Lateral to the mandible (58), beginning in Figure 65.2a , the parotid gland (153) is situated next to the large cervical vessels and vagus nerve (also p. 66). In front of the pons/medulla oblongata (107), the vertebral arteries (88) join to form the basilar artery (90).
The spread of inflammatory processes within the cervical connective tissue spaces is restricted within compartments defined by the cervical fascia [30]. The different layers of the cervical fascia are explained on the following page ( Fig. 66.4 ).






Further caudally the following cervical muscles become visible beneath the trapezius muscle (23): medial lie the semispinalis capitis (28) and longissimus capitis muscles (27), and more laterally the splenius capitis muscle (25). The parotid gland (153) is situated cranial and posterior to the submandibular gland (154) next to the mandible (58). The pharynx (176) is surrounded by Waldeyer’s ring of tonsillar tissue (157, 156). Note that the carotid bulb is situated between Figures 67.4a and 68.2a ; it is the point at which the common carotid artery (85) bifurcates into internal (85a) and external (85b) carotid branches. Under the tongue (155) the floor of the mouth is organized in layers. From cranial to caudal are: the genioglossus muscle (33), further laterally the geniohyoid muscle (34), and the anterior belly of the digastric muscle (31). The thin superficial muscle is the platysma (48).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree