PET/CT: Introduction
A PET/CT diagnostic study combines functional biochemical imaging (PET = Positron Emission Tomography) with morphologic imaging (CT) in a single examination. The examination makes it possible to simultaneously document metabolic information and the anatomy of healthy and pathologic tissue. Various radionuclides (known as tracers) are used depending on the specific clinical line of inquiry and the target organ.
Uptake Mechanism of Radioactive Tracers
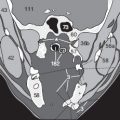
The most commonly used tracer is fluorine-18-FDG (fluorodeoxyglucose), in which one of the oxygen atoms in the glucose molecule has been replaced with a fluorine-18 isotope ( Fig. 202.1 ). During its half-life of about 110 minutes, the fluorine isotope emits measurable radiation that accumulates and can be measured at those locations at which the altered glucose molecule concentrates. This occurs not only in the brain, the working skeletal and cardiac musculature, the larynx and pharynx (after speech), the liver, the bowel, the kidney, and the urinary tract ( in Fig. 202.2 ); it also occurs in acutely inflamed tissues (such as in arthritis or gingivitis) with increased metabolism – or in metastases such as the right axillary one shown here ().



The glucose molecule is phosphorylated during glycolysis by the enzyme hexokinase in the mitochondria, particularly in the rapidly growing cells of malignant tumors or their metastases. The fluorine-18 isotope then impedes the further breakdown of glucose for some time, causing FDG molecules to accumulate more in malignant cells than in healthy tissues. This means that relatively increased FDG uptake can also indicate tumor metastases ( in Fig. 202.3b ) that would escape detection on conventional CT images ( Fig. 202.3a ).
Patient Preparation
After the indication has been verified and the physician has obtained the patient’s informed consent to the planned examination, the specific examination protocol for PET and CT is determined (i.e., IV, oral, rectal administration of contrast; arterial and portal venous phase). The patient is informed of possible risks and side effects that can occur within the scope of the examination (for example, contrast agent allergy). Then the blood glucose level is measured, which should be lower than 150 mg/dL so that the body’s cells take up a sufficient quantity of the injected FDG (for this reason patients should fast for about 4 to 6 hours before the examination begins).
The quantity of intravenous FDG is calculated from the respective body surface area and the patient’s body weight. The examination is performed following a waiting period of 60 minutes on average during which the FDG can circulate in the bloodstream, be taken up, and become phosphorylated. During the waiting period patients should rest (not walk around) and speak as little as possible (not talk on the phone or chew gum). This is to avoid increased FDG uptake in the neck and facial musculature that later might be difficult to distinguish from cervical metastases ( Fig. 202.2 ). Where orbital metastases of a neoplasm such as malignant melanoma on the head are to be excluded, patients should also not be allowed to read during the waiting period as otherwise the posterior ocular muscles could show increased uptake. The best solution is to have patients wear a blindfold and listen to music. It is important to ensure a sufficiently warm ambient temperature in the waiting room for all patients, but particularly for slender ones, and to provide warm blankets on the couches so that patients do not shiver. Shivering of the skeletal musculature can easily be overlooked but leads to increased uptake in the musculature and in brown fat. This increased uptake would later make it unnecessarily difficult to distinguish tumors in the local and regional lymph nodes or muscles. The quantity measured is the so-called SUVmax (maximum standardized uptake value), which is the correlate of the radionuclide taken up in the target tissue. While the measurements are being taken, it is important for the patient to lie as still as possible in order to facilitate subsequent fusion of the CT and PET images.
Exposure to Ionizing Radiation
For a full body scan about 200 to 400 mBq is applied intravenously depending on the patient’s body surface area and body weight. At about 0.02 mSv/mBq of radiation exposure, this corresponds to a total of about 7 to 10 mSv including the radiation dose of the CT scan. Note that the dose of radiation varies among the different organs. Accumulation of the tracer in urine means that at about 0.17 mSv/mBq the bladder receives a significantly higher dose than the other organs (see pp. 174–177).
Indications and Selection of Tracer
Aside from primary staging (extent of the primary tumor, detection of lymph node metastases and remote metastases), PET/CT can also be performed in the setting of restaging where there is cause to suspect recurrence and within the scope of follow-up (response evaluation). In these cases it is helpful in differentiating scar tissue from viable residual tumor tissue. In addition to tumor diagnostics, PET/CT is also used in specific neurologic and cardiologic settings. Most recently, PET/CT is increasingly being used in the diagnostic workup of specific cases of inflammatory disorders (vasculitis).
FDG (see p. 202) is not particularly well suited as a tracer with slowly progressive types of tumors, well-differentiated tumors, or mucinous tumor components (such as prostate tumors, low-grade brain tumors, well-differentiated hepatocellular carcinoma, mucinous gastric or ovarian carcinoma). In these cases, other radionuclides are preferred (see the following pages).
Brain Tumors
Brain tissue invariably exhibits a high level of glucose metabolism. As a result, it is often not possible to draw a clear distinction between moderately malignant grade I astrocytomas and healthy brain tissue (see high cerebral FDG uptake in Fig. 203.2 ), leading to false negative findings. For this reason radioactively labeled amino acids (carbon-11-methionine or fluorine-18-ethylene thyrosine (FET) are preferred when the line of inquiry does not involve highly malignant undifferentiated gliomas that can visualized with FDG.



Fig. 203.1 shows the comparison with an unremarkable low-dose CT of a patient with a suspected brain tumor: Because MRI (not shown here) had detected a left temporal edema, a PET/CT study was ordered which demonstrated focal 18F-FET uptake at that location and confirmed the suspected tumor.
Differential Diagnosis of Lymph Nodes
The CT morphologic criteria of enlarged lymph nodes do not always match up as they do in Fig. 203.2 : In the right axillary region () there is a benign lymph node with a hilum fat sign but without FDG uptake. However, in the left axillary region () there are two lymph node metastases with pathologic FDG uptake. Fig. 203.3 shows exactly the opposite: In this patient only a small 5-mm lymph node with a hilum fat sign ( Fig. 203.3a ) shows increased uptake. Surprisingly, it is this node which represents a metastasis (), whereas the larger 12-mm lymph node (with suspicious CT morphology) in another patient does not show increased uptake () and on PET/CT must be classified as benign ( Fig.203.3b ).



Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree