CHAPTER 39 Acute Labyrinthitis
Epidemiology
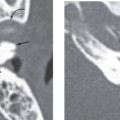
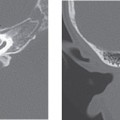
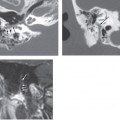
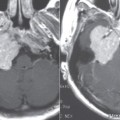
Acute labyrinthitis is an inflammatory process of the membranous labyrinth. The inflammatory response may be secondary to infections—bacterial, viral, or leutic—or may be secondary to trauma or autoimmune processes. There can be different routes for infection to reach the cochlea. It may be a complication of bacterial meningitis (meningogenic), in which infection can spread into the inner ear from the cochlear aqueduct. Infection can spread into the labyrinth also through a hematogenous route (hematogenic) via the cochlear vasculature. The most common cause is due to viral infections, though measles, mumps, tuberculosis, syphilis, and other bacterial infections can also spread via the hematogenous route. Posttraumatic labyrinthitis occurs either due to prior iatrogenic injury, from middle ear surgery, or due to prior injury. Labyrinthitis may be a complication of acute otomastoiditis (tympanogenic) with infection spreading from the middle ear cavity via the oval or round windows or through direct invasion of the bony labyrinth through a fistula in the lateral semicircular canal.
Clinical Features
Sudden sensorineural hearing loss and vertigo are common. Vertigo may be severe enough to cause nausea and vomiting. There are no associated auditory or central nervous system symptoms. This helps to differentiate labyrinthitis from cerebellar infarction, vestibular schwannoma, and Meniere disease, which can also present with sensorineural hearing loss. The disease may manifest as a single attack, or a patient may have multiple attacks. The acute phase may last for days to weeks, with generally complete recovery occurring around 6 months. There may be associated otitis media. Milder attacks of shorter duration of vertigo may occur in patients with multiple attacks.
Pathology
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree