Chapter 20 Anatomy and physiology
 The respiratory system functions as a series of air passages through which air enters the lungs and travels to the alveoli where gaseous exchange occurs.
The respiratory system functions as a series of air passages through which air enters the lungs and travels to the alveoli where gaseous exchange occurs. The cardiovascular system is a closed network of blood vessels that carry oxygenated blood to all body tissues and transport deoxygenated blood away from body tissues to the lungs for excretion, with the exception of the pulmonary vessels.
The cardiovascular system is a closed network of blood vessels that carry oxygenated blood to all body tissues and transport deoxygenated blood away from body tissues to the lungs for excretion, with the exception of the pulmonary vessels. Blood is composed of a liquid plasma and formed elements consisting of red and white blood cells as well as platelets.
Blood is composed of a liquid plasma and formed elements consisting of red and white blood cells as well as platelets. Blood is the ‘life’ of body cells and tissues as it carries vital life-sustaining oxygen and nutrients.
Blood is the ‘life’ of body cells and tissues as it carries vital life-sustaining oxygen and nutrients. This skeleton provides a supportive and protective framework for the body, which together with muscles gives the body its ability to carry out a wide range of movements.
This skeleton provides a supportive and protective framework for the body, which together with muscles gives the body its ability to carry out a wide range of movements. A joint is where two or more bones meet. Muscles acting across joints provide the mechanism by which movement takes place.
A joint is where two or more bones meet. Muscles acting across joints provide the mechanism by which movement takes place. The nervous system is the body’s network of communication that receives, interprets and relays messages to and from the brain.
The nervous system is the body’s network of communication that receives, interprets and relays messages to and from the brain. Food taken into the mouth is swallowed (ingested); digested by mechanical movements and chemical enzymes; its nutrients are absorbed and the left over waste eliminated.
Food taken into the mouth is swallowed (ingested); digested by mechanical movements and chemical enzymes; its nutrients are absorbed and the left over waste eliminated. The nephron forms the functional unit of the kidney to filter waste material from the blood and eliminate this as urine.
The nephron forms the functional unit of the kidney to filter waste material from the blood and eliminate this as urine. The endocrine system plays a role in maintaining homeostasis by the action of chemical messengers called hormones.
The endocrine system plays a role in maintaining homeostasis by the action of chemical messengers called hormones.SKELETAL SYSTEM
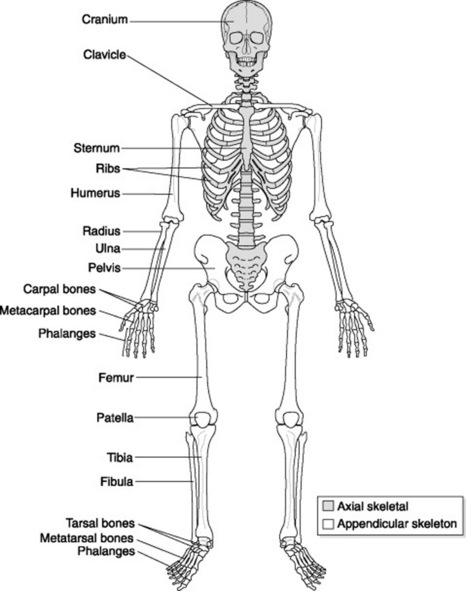
The skeletal system is made up of bones and joints that work together with muscles and ligaments to provide a framework for the body (Fig. 20.1).
BONES
General structure and appearance
Bone has an outer covering called the periosteum, which is a tough outer membrane made up of fibrous tissue and containing blood vessels. Thecortex is made up of compact tissue and lies directly below the periosteum. The inner layer of is made of spongy or cancellous bone, which is softer, compared to the tough outer cortex. Lastly, the innermost part of the bone is formed from ‘fatty’ yellow bone marrow, which contains a few white blood cells, and red marrow containing red blood cells.
Functions of bone
Bones are classified into the following types (Table 20.1):
Table 20.1 Classification of bone
| Shape | Description | Location in the body |
|---|---|---|
| Long bones | Length is greater than width | |
| Short bones | Equal in length, breadth and thickness | Wrist (carpal bones), ankle (tarsal bones) |
| Flat bones | Usually more curved and thin than flat; e.g. the curved bones of the skull protect the brain | Skull, chest (scapula, ribs, sternum), pelvis |
| Irregular bones | These do not have any of the above-mentioned shapes, hence ‘irregular’ | Axial skeleton, both shoulder and pelvic girdle and vertebrae |
| Sesamoid bones | Small bones that are found embedded in certain tendons connecting muscle to bone | Knee (the commonest sesamoid bone is the patella), but may also be seen on images of the hand, wrist and foot) |
JOINTS
A joint forms at a point where two bones and cartilages meet or where adjacent bones and cartilages are joined. Although bone gives the body protective structure and muscles provide the ability to move, it is actually the joints that provide the mechanism by which movement takes place. Radiographic contrast can sometimes be injected into a joint space (e.g. in the glenoid cavity of the shoulder) to visualise any underlying pathology. This procedure is known as an arthrogram.
Classification
A joint can be classified according to the range of movement it provides or by its articular surface structure. All joints in the body can be classified as shown in Table 20.2; however, certain areas of the body may have a combination of two joints; for example the temporomandibular joint (TMJ) comprises gliding and pivot joints.
Table 20.2 Classification of joints
CARDIOVASCULAR SYSTEM
This system forms the transport network for the body.
THE HEART
The heart is a muscle that acts as a pump and provides the energy and force to keep blood circulating throughout the body. Blood is circulated via a closed transport system; that is, oxygenated blood leaves the heart via arteries, passes through a tiny network of capillaries where transfer of oxygen and nutrients take place, and then deoxygenated blood returns to the heart via the veins.
Size, shape and location
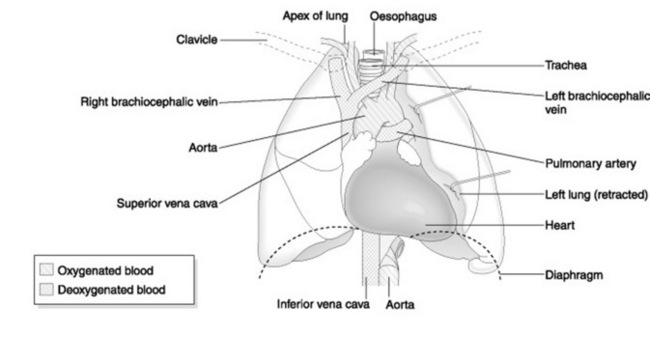
The heart is conical in shape and, under normal circumstances, about the size of its owner’s clenched fist. It is located anteriorly in the centre of the thorax, with about two-thirds of its bulk lying towards the left of the sternal margin. The tip of the ‘cone’ is called the apex and the flat portion is called the base. The base, normally found at the level of T5–T8, faces forwards and downwards to the left, ending in the apex. The apex lies at the level of the fifth intercostal space on the left midclavicular line (Fig. 20.2).
Occasionally patients may present with dextrocardia, a condition where the heart and great vessels originate with the same structure but opposite in direction (i.e. the apex lies towards the right side of the thorax rather than the left). This is a normal variant and is usually discovered as an incidental finding when the patient presents for a chest examination for an unrelated symptom.
Structure
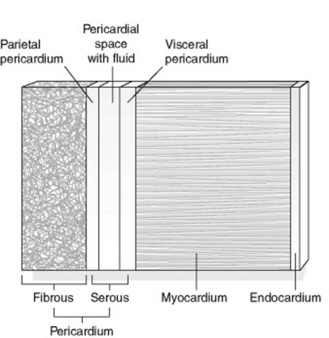
The heart wall is made up of three layers of tissue (Fig. 20.3):
The pericardium consists of two layers of tissue. The outer layer is a tough fibrous layer that serves to protect the heart wall and secure its position within the thorax. The inner layer is a serous layer. This serous pericardium is furtherdivided into an outer parietal layer, which forms the inner lining of the fibrous pericardium, and an inner visceral layer that forms the outer covering of the heart (also known as epicardium). Between these layers is a potential space, called the pericardial cavity. This contains serous fluid, which allows for flexibility in the movement of the heart during contraction and relaxation phases (heartbeats), thus reducing friction during these movements.
Chambers of the heart
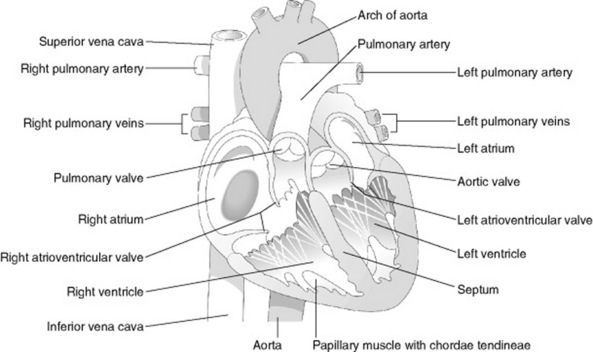
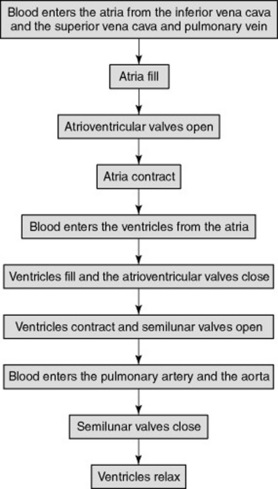
The heart is divided into left and right halves by a muscular septum. Each half has an upper atrium and a lower ventricle (Fig. 20.4). The atria are separated from each other by an interatrial septum and the ventricles are separated from each other by the interventricular septum. The atria are linked to the ventricles by atrioventricular valves. In a normal heart, blood flows from atria to ventricles and not the reverse. Figure 20.5 shows the sequence of events during the cardiac cycle.
Pumping action of the heart
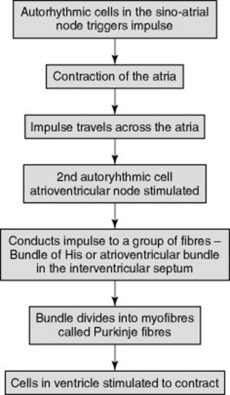
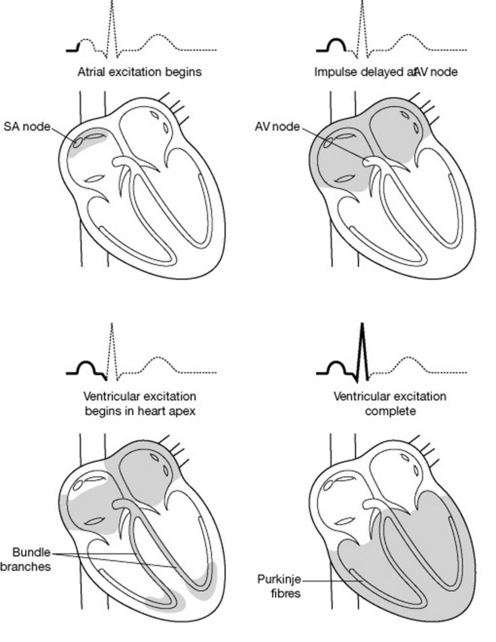
The heart’s own inherent autorhythmic cells act as a pacemaker to initiate and maintain the beating and pumping actions of the heart. These cells are also responsible for conducting these impulses throughout the cardiac muscle, thus creating an action in the path in which it travels (Fig. 20.6). Because the ventricles are responsible for sending blood out of the heart, the pressure in the ventricles is greater than the pressure inthe atria. The normal rhythm of a heart beat can be seen on an ECG (electrocardiograph) trace (see Fig. 20.7).
BLOOD VESSELS
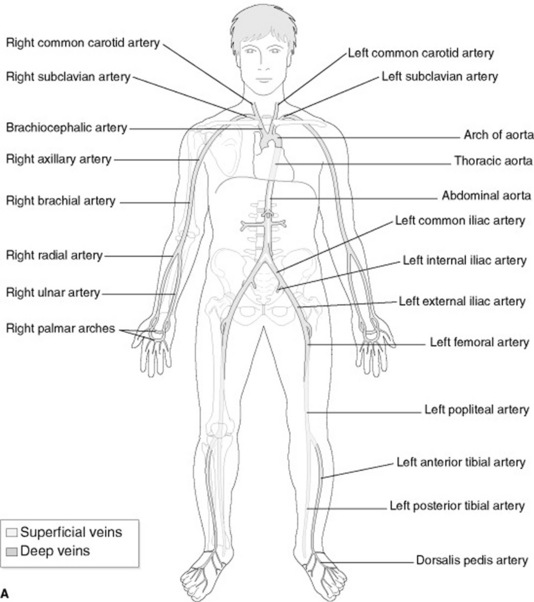
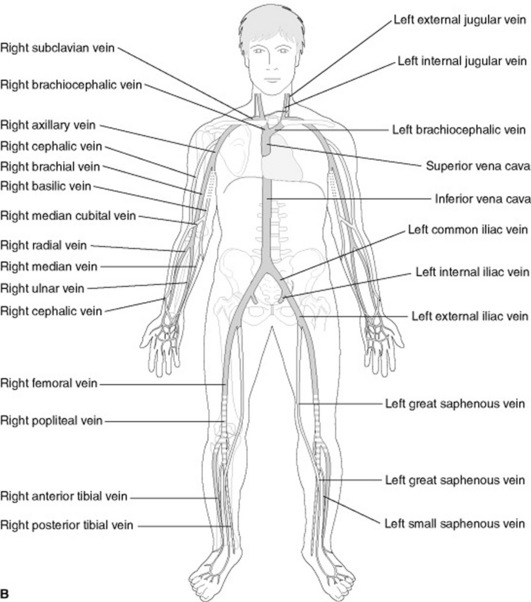
The aorta and other arteries carry oxygenated blood to the body (Fig. 20.8) and have thicker walls to withstand the high pressure at which blood is pumped into them. The closer the artery is to the heart, the thicker the walls of the artery. Arteries and veins can be demonstrated radiographically by using contrast media (e.g. in angiography and venography).
BLOOD
Blood is the ‘life’ of the body. It is a viscous tissue made up of liquid plasma and a combination of formed elements (blood cells). The plasma helpsthe body to maintain its normal state of hydration by responding to change in the internal environment via osmosis.
These blood cells have different functions (Table 20.3). Together they serve to:
Table 20.3 Blood cells and their function
| Blood cell | Function |
|---|---|
| Erythrocytes (red blood cells) | Contain haemoglobin (iron-containing pigment attached to a globular protein) for absorption and transport of oxygen from the lungs to cells and tissues |
| Leucocytes (white blood cells) | Provides immunity for the body by protecting against harmful invasion by disease-causing microorganisms – removes these, and debris from dead or damaged cells, from the blood. |
| Thrombocytes (blood platelets) | Responsible for clotting of the blood |
LYMPH AND LYMPH VESSELS
RESPIRATORY SYSTEM
The thorax is probably the most frequently imaged body part in radiology departments today because a single chest X-ray is sometimes sufficient to make a diagnosis and determine the overall health of a patient. The mechanism of breathing (inspiration and expiration) occurs within this system. It functions as a series of passages through which air travels from the outside (atmosphere) to the inside(lungs). In addition, this system contributes to wider ranging functions of voice production, coughing and sneezing.