Chapter Outline
Duplication of the Gallbladder
Anomalies of Gallbladder Shape
Abnormalities of Gallbladder Position
Abnormalities in Gallbladder Size
There are many congenital abnormalities of the gallbladder and bile ducts, which, excluding biliary atresia and choledochal cysts, are usually of no clinical or functional significance. These anomalies are usually found in the course of evaluating biliary disease in an adult patient and are of interest primarily to the surgeon, who must deal with the anatomic variation during the course of surgery.
Embryology
When the human embryo is 2.5 mm in size, a bifid bud forms along the anterior margin of the primitive foregut and proliferates laterally into the septum transversum. The more cephalad of these two diverticula is responsible for the formation of the liver and intrahepatic bile ducts, whereas the caudal diverticulum develops into the gallbladder and extrahepatic biliary tree. At the 5-mm stage of development, the originally hollow primordium of the gallbladder and common bile duct becomes occluded with endodermal cells but is soon revacuolated. If recanalization is incomplete, a compartmentalized multiseptate gallbladder results. A single, transversely oriented septum results in the phrygian cap deformity, whereas longitudinal septa produce a bifid or triple gallbladder. The lumen of the common bile duct is reestablished at the 7.5-mm stage and the gallbladder and duodenal lumen somewhat later. Bile is secreted by the 12th week.
At the 10- to 15-mm stage (6-7 weeks), the gallbladder has formed and is connected to the duodenum by a canalized choledochocystic duct. This duct originates from the lateral aspect of the primitive foregut and eventually terminates on the medial or posteromedial aspect of the descending portion of the duodenum after the foregut completes its 270-degree rotation.
The formation of the intrahepatic ducts is preceded by the development of the portal and hepatic veins and the formation of the hepatocytes and Kupffer cells. The intrahepatic ducts by the 18-mm stage consist only of a blindly ending solid core of cells that extends from the junction of the cystic and common ducts toward the liver hilum. At the point of contact between this blindly ending ductal anlage and the hepatocytes, the intrahepatic ducts develop along the framework of the previously formed portal vein branches similar to vines on a trellis. Significant variation in the configuration of the intrahepatic ducts can be accounted for by the unpredictable manner in which they wind around preexisting portal veins.
Agenesis of the Gallbladder
Agenesis of the gallbladder is caused by failure of development of the caudal division of the primitive hepatic diverticulum or failure of vacuolization after the solid phase of embryonic development. Atresia or hypoplasia of the gallbladder also represents aborted development of the organ. Other congenital anomalies are present in two thirds of these patients, including congenital heart lesions, polysplenia, imperforate anus, absence of one or more bones, and rectovaginal fistula. There appears to be a genetic input as well because several families with multiple individuals having agenesis have been identified. This malformation is reported in 0.013% to 0.155% of autopsy series, but many of these cases are in stillborn and young infants. The surgical incidence of gallbladder agenesis is approximately 0.02%. Nearly two thirds of adult patients with agenesis of the gallbladder have biliary tract symptoms, and extrahepatic biliary calculi are reported in 25% to 50% of these patients.
Preoperative diagnosis of gallbladder agenesis is difficult, and the absence of the gallbladder is often an intraoperative finding. Ultrasound or computed tomography (CT) may suggest the diagnosis, but this disorder is usually diagnosed at surgery when the gallbladder is not found at cholangiography. Intraoperative ultrasound may be helpful in establishing the diagnosis and excluding a completely intrahepatic gallbladder. Agenesis of the gallbladder is a rare cause of false-positive hepatobiliary scintiscans.
Duplication of the Gallbladder
Gallbladder duplication occurs in about 1 in 4000 people and 4.8% of domestic animals. This anomaly is caused by incomplete revacuolization of the primitive gallbladder, resulting in a persistent longitudinal septum that divides the gallbladder lengthwise. Another possible mechanism is the occurrence of separate cystic buds. To establish the diagnosis, two separate gallbladder cavities, each with its own cystic duct, must be present. These duplicated cystic ducts may enter the common duct separately or form a Y configuration before a common entrance.
Most reported cases of gallbladder duplication have a clinical picture of cholecystitis with cholelithiasis in at least one of the gallbladders. Sometimes one of the gallbladders appears normal on oral cholecystography, whereas the second, diseased, nonvisualized, and unsuspected gallbladder produces symptoms.
A number of entities can mimic the double gallbladder at sonography: folded gallbladder, bilobed gallbladder, choledochal cyst, pericholecystic fluid, gallbladder diverticulum, vascular band across the gallbladder, and focal adenomyomatosis. Complications associated with double gallbladder include torsion and the development of papilloma, carcinoma, common duct obstruction, and secondary biliary cirrhosis. Treatment of this disorder consists of removal of both gallbladders.
Triple and quadruple gallbladders have also been reported. Diverticular gallbladders without cystic ducts are classified as accessory gallbladders.
Anomalies of Gallbladder Shape
Phrygian Cap
Phrygian cap is the most common abnormality of gallbladder shape, occurring in 1% to 6% of the population. It is named after the headgear worn by ancient Greek slaves as a sign of liberation. This deformity is characterized by a fold or septum of the gallbladder between the body and fundus. Two variations of this anomaly have been described. In the retroserosal or concealed type, the gallbladder is smoothly invested by peritoneum, and the mucosal fold that projects into the lumen may not be visible externally. In the serosal or visible type, the peritoneum follows the bend in the fundus, then reflects on itself as the fundus overlies the body. This anomaly is of no clinical significance unless it is mistaken for a layer of stones or hyperplastic cholecystosis.
Multiseptate Gallbladder
The multiseptate gallbladder is a solitary gallbladder characterized by multiple septa of various sizes internally and a faintly bosselated surface externally. The gallbladder is usually normal in size and position, and the chambers communicate with one another by one or more orifices from fundus to cystic duct. These septations lead to stasis of bile and gallstone formation. On ultrasound studies, multiple communicating septations and locules are seen bridging the gallbladder lumen. Oral cholecystography reveals the “honeycomb” multicystic character of the gallbladder. The sonographic differential diagnoses are desquamated gallbladder mucosa and hyperplastic cholecystoses.
Diverticula
Gallbladder diverticula are rare and usually clinically silent. They can occur anywhere in the gallbladder and are usually single and vary greatly in size. Congenital diverticula are true diverticula and contain all the mural layers, as opposed to the pseudodiverticula of adenomyomatosis, which have little or no smooth muscle in their walls. Acquired traction diverticula from adjacent adhesions or duodenal disease must also be excluded.
Abnormalities of Gallbladder Position
Wandering Gallbladder
When the gallbladder has an unusually long mesentery, it can “wander” or “float.” The gallbladder may “disappear” into the pelvis on upright radiographs or wander in front of the spine or to the left of the abdomen. Rarely, the gallbladder can herniate through the foramen of Winslow into the lesser sac. In these cases, cholecystography reveals an unusual angulation of the gallbladder, which lies parallel and adjacent to the duodenal bulb with its fundus pointing to the left upper quadrant. The herniation can be intermittent and may be responsible for abdominal pain. It is best seen by a barium meal in conjunction with oral cholecystography. Cross-sectional imaging may not be specific, showing only a cystic structure in the lesser sac.
Gallbladder Torsion
Three unusual anatomic situations give rise to torsion of the gallbladder, and they all produce twisting of an unusually mobile gallbladder on a pedicle: (1) a gallbladder that is completely free of mesenteric or peritoneal investments except for its cystic duct and artery, (2) a long gallbladder mesentery sufficient to allow twisting, and (3) the presence of large stones in the gallbladder fundus that cause lengthening and torsion of the gallbladder mesentery. Kyphosis, vigorous gallbladder peristalsis, and atherosclerosis have also been implicated as other predisposing or contributing factors. The mesentery is sufficiently long to permit torsion in 4.5% of the population. Most cases of gallbladder torsion occur in women (female-to-male ratio of 3 : 1). The usual preoperative diagnosis is acute cholecystitis. The presence of fever is variable, leukocytosis is common, and one third of patients have a right upper quadrant mass. Gangrene develops in more than 50% of cases and is extremely common when the pain has been present for more than 48 hours. On cross-sectional imaging, the gallbladder is distended and may have an unusual location and show mural thickening. The diagnosis is seldom made preoperatively, however.
Ectopic Gallbladder
The gallbladder can be located in a variety of anomalous positions. In patients with an intrahepatic gallbladder, the gallbladder is completely surrounded by hepatic parenchyma. The intrahepatic gallbladder usually presents little difficulty in imaging, but it may complicate the clinical diagnosis of acute cholecystitis because of a paucity of peritoneal signs resulting from the long distance between the gallbladder and peritoneum. This anomaly also makes cholecystectomy more difficult. On sulfur colloid scans, the intrahepatic gallbladder presents as a cold hepatic defect.
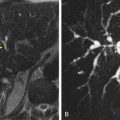
The gallbladder has also been reported in the following positions: suprahepatic, retrohepatic ( Fig. 76-1 ), supradiaphragmatic, and retroperitoneal. In patients with cirrhosis, small or absent right lobes, or chronic obstructive pulmonary disease, the gallbladder together with the colon is often interposed between the liver and the diaphragm. Left-sided gallbladders may occur in situs inversus or as an isolated finding. They can also lie in the falciform ligament, transverse mesocolon, and anterior abdominal wall.

Abnormalities in Gallbladder Size
Cholecystomegaly
Enlargement of the gallbladder has been reported in a number of disorders including diabetes (because of an autonomic neuropathy) and after truncal and selective vagotomy. The gallbladder also becomes larger than normal during pregnancy, in patients with sickle hemoglobinopathy, and in extremely obese people.
Microgallbladder
In patients with cystic fibrosis, the gallbladder is typically small, trabeculated, contracted, and poorly functioning. It often contains echogenic bile, sludge, and cholesterol gallstones. These changes are presumably due to the thick, tenacious bile that is characteristic of this disease.
Biliary Tract Anomalies
Anomalies of the biliary system are found in 2.4% of autopsies, 28% of surgical dissections, and 5% to 13% of operative cholangiograms. The most common anomaly is an aberrant intrahepatic duct draining a circumscribed portion of the liver, such as an anterior or posterior segment right lobe duct that drains into the left main rather than the right main hepatic duct. The aberrant duct can join the common hepatic duct, common bile duct, or cystic duct or insert into a low right hepatic duct. Rarely, it may run through the gallbladder fossa or into the gallbladder, predisposing it to injury at cholecystectomy.
The hepatic ducts may join either higher or lower than normal. Surgical difficulties may arise when the cystic duct enters into a low inserting right hepatic duct or when the right hepatic duct enters into the cystic duct before joining the left hepatic duct. Duplications of the cystic duct and common bile duct are rare. Anomalies of cystic duct insertion occur as well ( Fig. 76-2 ).

Congenital tracheobiliary fistula is a rare disorder that is manifested with respiratory distress and cough with bilious sputum. The fistula begins near the carina, traverses the diaphragm, and usually communicates with the left hepatic duct. Pneumobilia may be seen on plain radiography, and the diagnosis is confirmed with biliary scintigraphy.
Choledochal cysts, choledochoceles, and Caroli’s disease are a part of a spectrum of biliary anomalies that produce dilation of the biliary tree. They are discussed individually in the following section, and their relationship is illustrated in Figure 76-3 .