Cornelia Wenokor, MD
The axial skeleton consists of the bones that form the central axis of the body and includes the skull, sternum, ribs, and vertebra.
SKULL
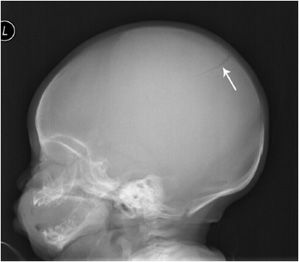
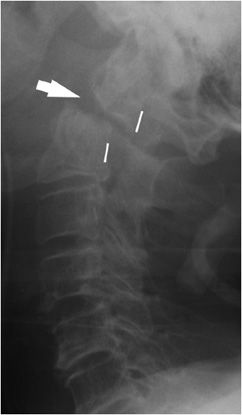
As most trauma patients with suspected head injuries are imaged with computed tomography (CT), skull radiographs are now rarely used to diagnose fractures. Fracture types include simple linear (Figure 4-1) and depressed (Figure 4-2A,B). Patients with skull fractures demonstrate an increased risk for intracranial hemorrhage,1,2 and dural laceration can be seen with the depressed type.3
Figure 4-1. Linear skull fracture. Lateral radiograph of skull shows linear skull fracture in pediatric patient (arrow).
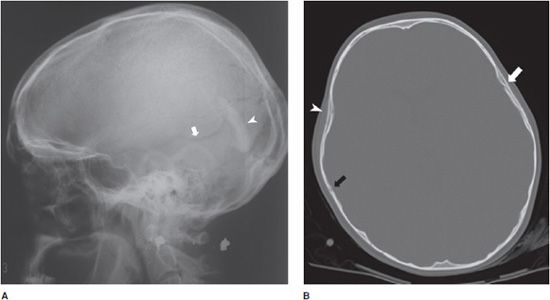
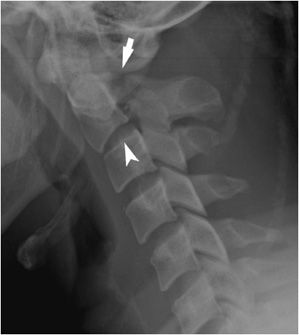
Figure 4-2. Depressed skull fracture. (A) Lateral radiograph of the skull shows sclerotic double line seen with depressed skull fracture (arrowhead). This finding is often mistaken for artifact. Linear skull fracture is also seen (arrow). (B) Axial CT image of the head showing depression in skull (arrowhead) compared to normal side (white arrow). Linear fracture (black arrow).
TORSO
Injury to the sternoclavicular and sternomanubrial joints usually occurs after forceful impact and compression. Sternoclavicular dislocation should be suspected on radiographs where the clavicular heads are seen at different craniocaudal positions (Figure 4-3A). Posterior dislocation of the medial clavicle can compromise structures of the thoracic outlet including the great vessels, brachial plexus, and trachea (Figure 4-3B,C).4 Type I sternomanubrial dislocation, where the sternum is displaced posterior to the manubrium, is often identified on physical examination (Figure 4-4). CT can demonstrate any associated mediastinal injuries.5
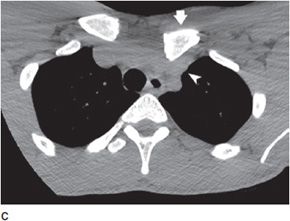
Figure 4-3. Disruption of sternoclavicular joint. (A) Frontal chest radiograph shows normally positioned head of right clavicle (arrowheads) compared to superiorly and posteriorly dislocated left clavicular head (arrows). (B) Axial CT image of the clavicles shows normally positioned right clavicular head (arrowhead) and superiorly and posteriorly dislocated left clavicular head (arrow). (C) Axial CT image of the clavicles done in soft tissue algorithm shows superiorly and posteriorly dislocated left clavicular head (arrow) and compression of left subclavian vessels (arrowhead).
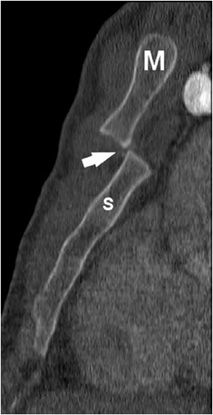
Figure 4-4. Sternomanubrial dislocation. Sagittal CT reformat of the sternum shows type I sternomanubrial dislocation occurring at the sternomanubrial joint (arrow). S, sternum; M, manubrium.
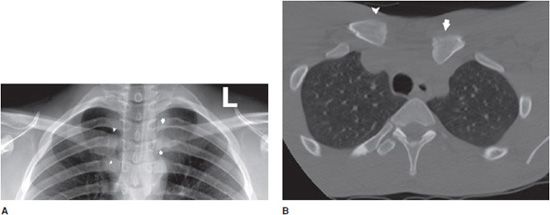
Rib fractures are a frequent finding on chest radiographs obtained on admission to the trauma emergency department or on the CT scan done to evaluate chest, abdomen, and pelvis injuries (Figure 4-5). An associated pneumothorax can be seen on one or both of these studies, but CT often identifies small pneumothoraces missed on portable radiographs.
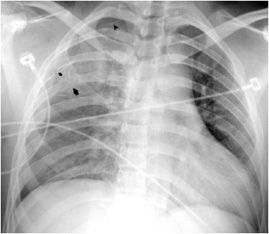
Figure 4-5. Rib fractures with small pneumothorax. Frontal chest radiograph shows comminuted fractures of the right posterior 4 and 5 ribs (arrows). Small apical pneumothorax is present (arrowhead).
CERVICAL SPINE
In cervical spine injury, CT with coronal and sagittal reformatting is the preferred study. If a radiographic evaluation is performed, begin with a lateral view of the spine and the radiograph must include the C7 (seventh cervical vertebral body) and, ideally, the T1 (first thoracic) vertebral body. Interpretation of the radiograph should be done in a systematic fashion. The posterior vertebral body line (Figure 4-6) should form a smooth curve from C1 to the C7 level and it outlines the anterior wall of the spinal canal. It is important to examine this line and identify any offset that may cause cord compression. Anterior subluxation of the more proximal vertebral body on the subjacent body is called a spondylolisthesis. Posterior subluxation of the proximal vertebral body on the subjacent vertebral body is called a retrolisthesis. Facet joints are stacked one on another like shingles on a roof, and the width of these articulations should all be similar. The articulation between the tip of the dens (odontoid process) and the anterior arch of C1 is the atlantodental interval (ADI), and this normally measures up to 3 mm in adults and up to 5 mm in children. Evaluation of vertebral body integrity and width of the disc spaces must also be done. A satisfactory lateral radiograph should be obtained to avoid mistaking normal overlying bony structures for vertebral fractures. Abrupt widening of the disc space may be the only radiographic indication of a hyperextension injury. A narrowed disc space often occurs secondary to degenerative disc disease, but may also, on occasion, indicate a flexion injury.
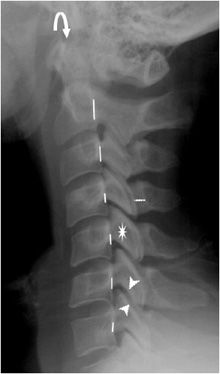
Figure 4-6. Normal lateral radiograph of cervical spine. Normal lateral radiograph of the cervical spine showing posterior vertebral body line (solid lines) and normal atlantodental (atlantoaxial) interval (curved arrow). Facet joints outlined by arrowheads, and lamina denoted by dotted line. Asterisk denotes articular mass.
Signs of spinal instability include widened facet joints or interspinous distances, widening or elongation of the spinal canal in the transverse or vertical plane, and significant vertebral subluxation, causing offset of the posterior vertebral body line. Focal angulation of the spine and asymmetrically widened or narrowed disc spaces may also be clues to instability.
Widening of the ADI is called atlantodental (atlantoaxial) subluxation. The injury can be caused by hyperflexion and is often associated with fractures of the dens. Cord compression can occur and this is considered an unstable injury (Figure 4-7). The Jefferson fracture is caused by axial loading and is characterized by four breaks in the C1 ring: two anteriorly and two posteriorly. It is considered a relatively minor injury with little neurologic sequelae. An offset of the lateral masses greater than 3 mm on either side of C1 with respect to C2 is diagnostic of this injury (Figure 4-8A–C).6
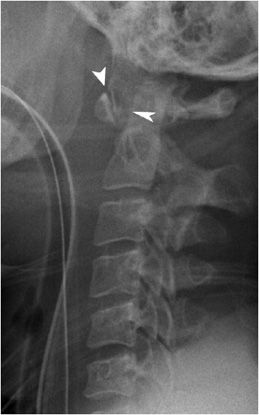
Figure 4-7. Atlantodental dislocation. Lateral cervical radiograph shows abnormal widening of the atlantodental (atlantoaxial) interval (arrowheads).
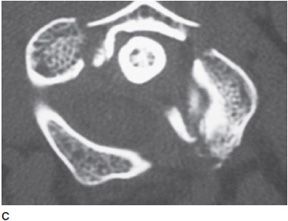
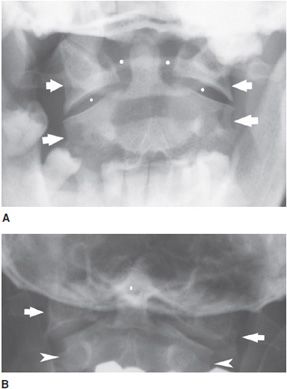
Figure 4-8. Open mouth view of normal odontoid. (A) Normal odontoid radiograph shows that the lateral margins of the C1 and C2 vertebral bodies align closely with little overlap (arrows). Clear spaces between the vertebrae are symmetric (dots). (B) Jefferson fracture: Odontoid radiograph shows Jefferson fracture. Lateral margins of C1 (arrows) exceed the lateral margins of C2 by <3 mm (arrowheads). (C) Axial CT image shows comminuted fracture of the arch of C1 (atlas) vertebra. Dot denotes tip of dens.
Fractures of the dens comprise 10–13% of all cervical injuries.7 The mechanism of injury is not clearly delineated with flexion, extension, and lateral shearing all thought to play a role. The classification of dens fractures as described by Anderson and D’Alonzo is based on location of the fracture.8 Type I dens fractures occur at the tip of the dens. Type II dens fractures occur at the junction of the odontoid process and the body of C2. This fracture type is the most common type of odontoid fracture. Without surgical intervention, this type of fracture also has the highest nonunion rate (Figure 4-9). Type III fractures involve the body of C2.
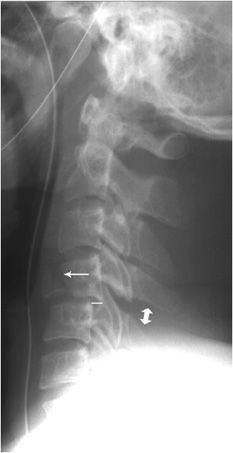
Figure 4-9. Type II odontoid fracture. Lateral cervical spine radiograph shows type II odontoid fracture (arrow). Offset of posterior vertebral body line caused by anterior displacement of the base of C2 relative to the tip of the odontoid (broken lines).
Hangman fracture occurs through the posterior neural arch of C2. Levine has developed a classification system for this fracture. Type I shows no subluxation of C2 on C3, while type II injury shows angulation or subluxation across the C2-3 disc space. Type III may include unilateral or bilateral facet dislocations at the C2-3 level. The mechanism of injury is hyperextension for type I, and hyperflexion and compression with the type III injury. Additional cervical fractures are seen in 26–31% of the cases, and this is one reason to do CT imaging when a Hangman fracture is identified (Figure 4-10). The majority of major neurologic injuries occur with type II and III injuries, as disruption of the posterior ligamentous complex is likely to be present causing instability.9
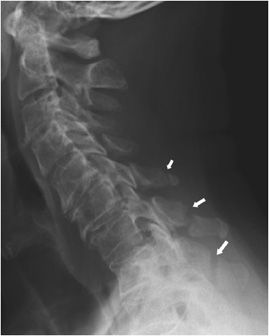
Figure 4-10. Hangman fracture. Lateral cervical spine radiograph shows a C2 Hangman fracture. Fracture through the posterior arch of C2 is nondisplaced (arrow) and there is asymmetric narrowing and angulation at the anterior margin of the C2-3 disc space (arrowhead).
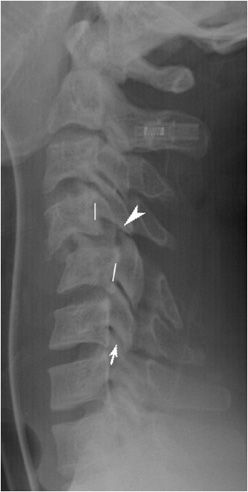
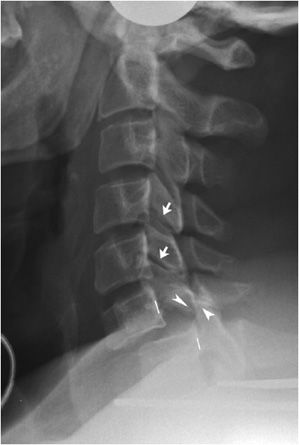
Injuries to the middle and lower cervical spine are usually secondary to flexion mechanisms. Pure flexion is the mechanism behind bilateral dislocated or locked facets, while flexion and rotation is the cause of a unilateral locked facet. Radiographs of unilateral locked facets will demonstrate sudden obliquity with two facet outlines at and above the locked level. The subjacent superior articular mass is dislocated posterior to the inferior articular process of the vertebral body above, locking the facet in place. Anterior subluxation of less than 50% vertebral body width can be seen (Figure 4-11).10 Bilateral locked facets show the subjacent superior articular processes locked behind the articular masses of the anteriorly subluxated vertebral body. Vertebral subluxation with this injury is often greater than 50% of vertebral body width (Figure 4-12). Both injuries are associated with a high frequency of spinal cord damage. The extent of cord damage may be secondary to the width of the cervical spinal canal at the level of injury and the severity of cord compression. Patients often need to be placed in skeletal traction to stretch the cervical spine longitudinally and unlock these dislocations.
Figure 4-11. Unilateral locked facet. Lateral cervical spine radiograph shows unilateral locked facet, normal facet joints (arrow) and normal alignment of lower cervical spine, and abrupt obliquity of upper cervical spine and subluxation of C4 on C5 (broken lines). Arrowhead shows the inferior articular process of C4 “locked” in front of the superior articular process of C5.
Figure 4-12. Bilateral locked facet. Lateral cervical radiograph shows bilateral locked facets at the C6-7 level and significant anterior subluxation at the C6-7 level (broken lines). Articular mass at C6 level is dislocated anterior to articular mass at C7 level, “locking” this vertebra in position (arrowheads). Normal facet joints are seen proximally (arrows).
The “Flexion teardrop” injury is caused by flexion and compression, where the neck is flexed and the head strikes an object. A high percentage of patients demonstrate a kyphosis at the level of injury, and disc space narrowing at the level of the fracture is also common. Disruption of the posterior vertebral body line and widened interspinous distance should be searched for. There is a broad range of neurologic injury from normal to quadriplegia (Figures 4-13 and 4-14).11 Hyperextension injuries of the cervical spine may result in an “Extension teardrop” fracture that is an avulsion fracture of the anterior inferior corner of the C2 vertebra (Figure 4-15A–C).
Figure 4-13. Flexion teardrop fracture. Lateral cervical spine radiograph shows flexion teardrop fracture (arrow) with fragment originating from anterior inferior corner of C4, narrowed C4-5 disc space and offset of posterior vertebral body line (line), and widened interspinous distance (double arrow).
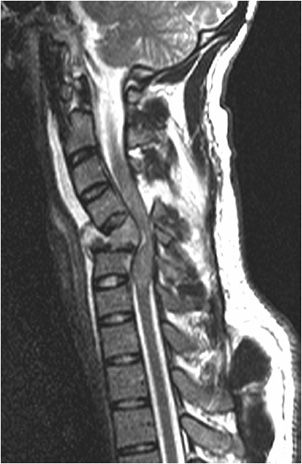
Figure 4-14. Flexion teardrop fracture (MR). Sagittal T2-weighted image shows flexion teardrop fracture of C5 vertebra with cord compression.
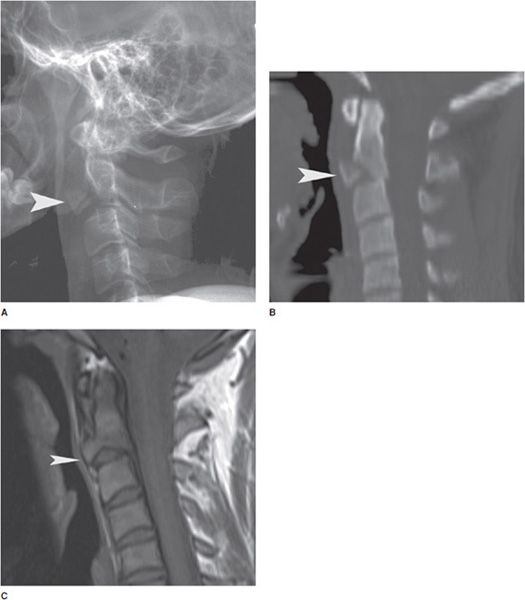
Figure 4-15. Extension teardrop fracture (A–C). Lateral radiograph, CT sagittal reformat, and MRI sagittal T1-weighted image of the cervical spine shows a triangular piece of bone (arrowhead) being avulsed from the anterior inferior corner of C2 vertebra as a result of hyperextension injury.
Clay shoveler fracture is an avulsion of the spinous process caused by flexion and rotation, occurring in the lower cervical or upper thoracic levels (Figure 4-16).12 This is a stable injury.
Figure 4-16. Clay shoveler fracture. Lateral cervical spine radiograph shows clay shoveler fractures of the spinous processes of C5 through C7 (arrows).
THOEACIC AND LUMBER SPINE
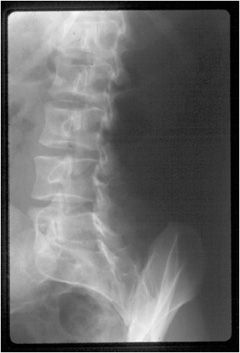
Burst fractures are caused by flexion and axial loading, and can cause devastating neurologic damage. This is an unstable injury characterized by retropulsed fracture fragments in the spinal canal and damage to the posterior longitudinal ligament (Figure 4-17A–D). The vertebral body is compressed and expands in both anterior–posterior and transverse diameter. In contrast, compression fractures only demonstrate diminished vertebral height anteriorly and normal height posteriorly. There is no retropulsed bone in the canal (Figure 4-18).
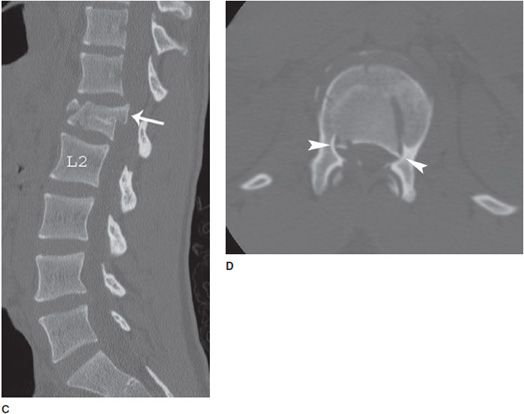
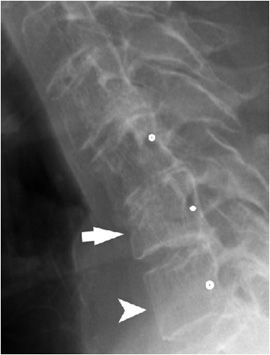
Figure 4-17. Burst fracture. (A) Lateral lumbar radiograph shows anterior loss of height and the L1 level with retropulsion off bony fragment into the spinal canal (arrow). There is a mild kyphosis at this level. (B) Frontal radiograph of lumbar spine shows asymmetric narrowing of the right side of the vertebra (arrow) with mild expansion of the transverse diameter of this vertebra relative to other lumbar levels (arrowhead). Note widening of interpediculate distance at this level (double arrow). (C) Sagittal CT reformat of the lumbar spine reveals comminuted fracture in L1 vertebra as well as retropulsion of bone fragment into the spinal canal (arrow). (D) Axial CT image of L1 vertebral body shows retropulsed bone fragment compromising width of the spinal canal by approximately 50% (arrowheads). Note widening of the interpediculate distance (arrowheads).
Figure 4-18. Partial compression fracture. Lateral cervical radiograph shows compression fracture with anterior loss of vertebral height (arrow) and normal vertebral height at subjacent level (arrowhead). Note straight or concave posterior vertebral bodies (dots) with no evidence of retropulsed bone.
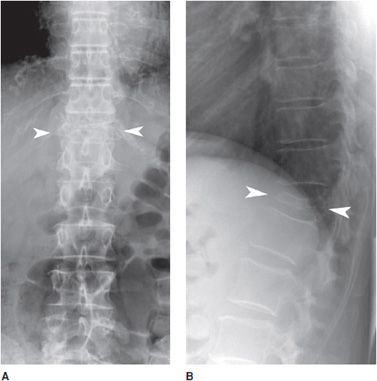
Chance fracture or “seatbelt” fracture is caused by acute hyperflexion with distraction, and fractures usually occur close to the thoracolumbar junction. This will cause a horizontal fracture through all aspects of the vertebral body, splitting the vertebral body. Flexion will cause some anterior compression. There may be posterior ligamentous injury as well as retropulsion of bone fragments into the spinal canal, and this fracture is considered unstable. When a burst component is seen, spinal cord injury is usually noted. Up to 40% of patients with this fracture demonstrate intra-abdominal injury (Figure 4-19A,B).13 Spinal dislocation is caused by falling from a great height or a motor vehicle accident, and will also result in paralysis (Figures 4-20 and 4-21).
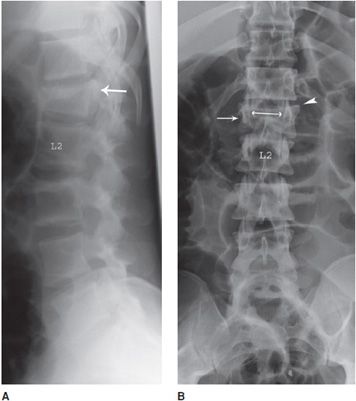
Figure 4-19. Chance fracture. (A) Frontal radiograph of lumbar spine shows transverse fracture at the L2 level overlying the pedicles (arrow). (B) Lateral lumbar radiograph shows anterior loss of height at the L1 level when compared to the L2 level (broken lines). Lucent fracture line noted transversely through posterior elements (arrow).
Figure 4-20. Thoracolumbar spine dislocation. Frontal radiograph shows thoracolumbar spine dislocation, transverse fracture through proximal margin of T12 vertebral body with leftward displacement of the remainder of the T12 vertebra and lumbar-sacral spine (arrows), proximal migration of lower spine with overriding bone at the T12 level, dislocation of right T12 rib (arrowhead), and right transverse process fracture at L5.
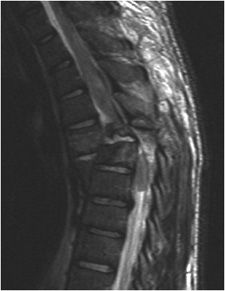
Figure 4-21. Thoracic spine fracture dislocation. Fat-saturated T2-weighted image of thoracic spine shows fracture dislocation of the thoracic spine with spinal cord transsection.
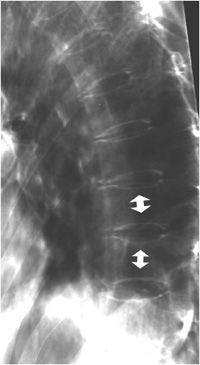
Biconcave vertebral endplates or “fish” vertebra are seen in patients who have osteoporosis. Weakened bone results in central depression of the vertebral endplates (Figure 4-22). The term vertebra plana is reserved for a fractured vertebral body that has significant loss of height and appears almost flat in shape. This is usually the result of neoplastic infiltration (Figure 4-23A,B).
Figure 4-22. Biconcave osteoporotic compression fracture. Central depression of biconcave endplates (double arrows) in osteoporotic vertebrae.
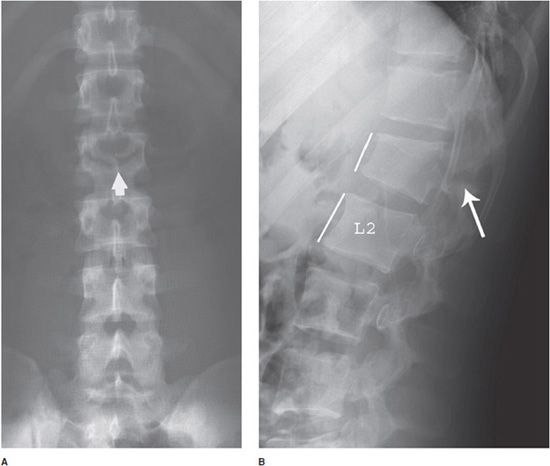
Figure 4-23. Vertebra collapse in multiple myeloma. (A) Frontal radiograph shows marked flattening of the T12 vertebral body (arrowheads). (B) Lateral lumbar spine radiograph again shows marked loss of height after pathologic fracture at this level (arrowheads).
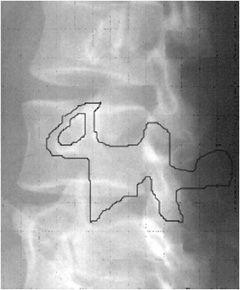
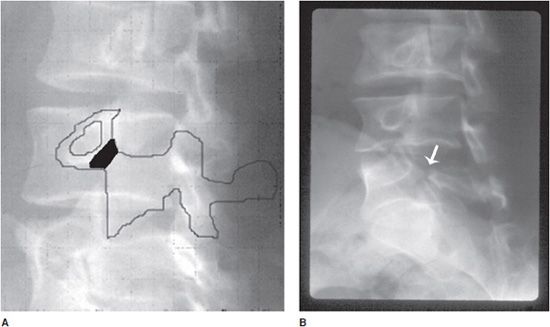
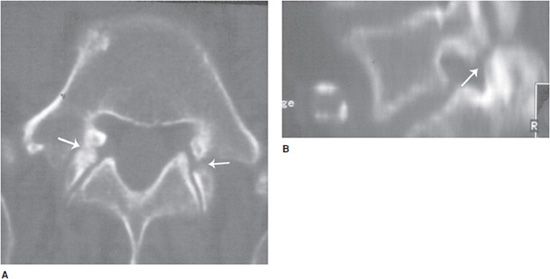
Pars interarticularis (isthmus) is a segment of bone connecting the superior to the inferior articular processes of the vertebrae (Figures 4-24 and 4-25). Fractures of the pars interarticularis of the vertebra will lead to a defect in this segment of bone between the superior and inferior articular processes of the facet joints called spondylolysis; this fracture is referred to as the “Scotty dog lost its collar” sign (Figures 4-26A,B and 4-27A,B). Subluxation resulting from this pars interarticularis fracture is called spondylolisthesis.
Figure 4-24. Normal oblique lumbar spine. Normal oblique radiograph of the lumbar spine.
Figure 4-25. Normal oblique lumbar spine. Coned-down normal oblique radiograph of lumbar spine shows “Scotty dog.” The ear of the dog is the superior articular process. The eye of the dog is the pedicle. The anterior and posterior legs of the dog are inferior articular processes. The tail of the dog is the spinous process of vertebra.
Figure 4-26. Spondylolysis (A,B). Coned-down view of oblique lumbar spine radiograph with spondylolysis shows “Scotty dog has lost its collar.” Note defect in the pars interarticularis (arrow) or neck of the dog.
Figure 4-27. Pars interarticularis defect (spondylolysis) (A,B). Axial CT and sagittal reformatted CT of pars interarticularis defects (arrows).
SACRUM
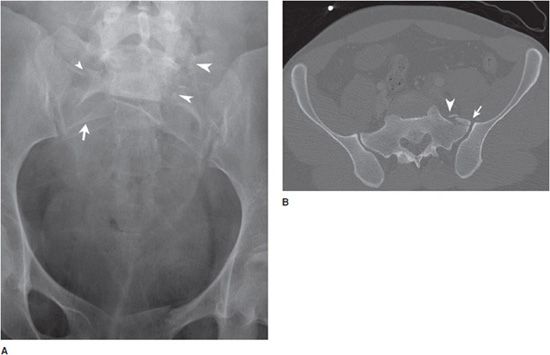
Sacral fractures are often difficult to visualize on radiographs because of overlying bowel gas or contrast material remaining in the bladder that obscures this region (Figure 4-28A,B). Such fractures should always be suspected in patients who have sustained fractures to the anterior pelvic ring or who have diastasis of the pubic symphysis. With the prevalence of CT imaging, sacral fractures are more often identified on CT reformatting of the pelvis. Denis et al. describe three locations for sacral fractures. Zone 1 fractures occur vertically through the ala and lateral to the sacral neural foramen. This type of fracture is the most frequent and has the lowest rate of nerve injury, usually limited to the L5 nerve root. Zone 2 fractures are propagated through the sacral neural foramina, are less frequent than zone 1 injuries, and have a 28% incidence of nerve root injury. Zone 3 injuries affect the spinal canal and have the highest rate of nerve injury with bladder and sphincter dysfunction.14
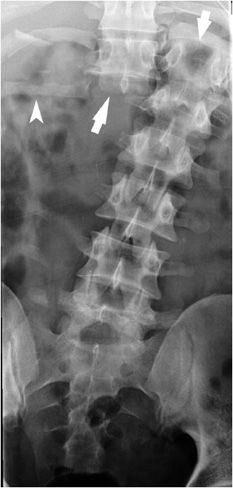
Figure 4-28. Sacral fractures. (A) Frontal view of the pelvis shows bilateral sacral fractures (arrowheads). Right fracture more easily recognized by interruption of the arcuate line. Note normal arcuate line (arrow). (B) Axial CT image shows zone 1 left sacral ala fracture (arrowhead) and mild diastasis of left sacroiliac joint (arrow).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree