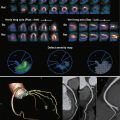
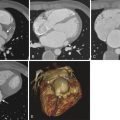
The bronchial arteries represent approximately 1% of the blood supply to the lungs and do not participate in gas exchange. They provide systemic blood supply to the airways, esophagus, posterior mediastinum, portions of the visceral pleura, and mediastinal lymph nodes, as well as to the pulmonary arteries themselves through their vasa vasorum. When normal, the bronchial arteries are not typically well visualized on thoracic aortography. In patients with various cardiopulmonary disorders, including chronic lung infections, lung tumors, inflammatory lung disease, pulmonary vasculitis, congenital heart disease, and chronic pulmonary vascular obstruction, the bronchial arteries can become enlarged as a major source of collateral circulation. In these settings, the risk of hemoptysis from a bronchial artery source exists. Imaging of the bronchial arteries is therefore an important step in the management of these patients. Although evaluation of the bronchial arteries has relied on thoracic aortography and selective bronchial artery angiography, computed tomography (CT) imaging of the bronchial arteries has become more technically feasible and can yield valuable information in the diagnostic workup of a patient with hemoptysis.
Key Issues for Problem Solving in Bronchial Artery Imaging
- ▪
Anatomy of the bronchial arteries
- ▪
Technique for CT imaging in hemoptysis: how to optimize visualization of the bronchial arteries
- ▪
CT findings in bronchial artery imaging
- ▪
CT evaluation of nonbronchial systemic collateral vessels
- ▪
CT evaluation of bronchial-to-systemic artery communications
- ▪
Bronchial artery embolization: technique and considerations
Anatomy
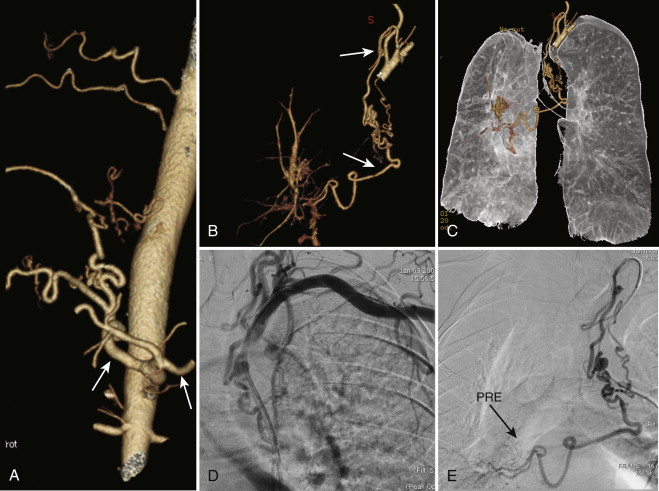
The bronchial arteries are variable in number and origin ( Box 45-1 ). Certain typical features may be seen, however. The bronchial arteries arise from the descending thoracic aorta in approximately 70% of individuals, usually at the T5 to T6 thoracic vertebral body level. This configuration is considered the orthotopic origin of the bronchial arteries. Based on cadaveric studies, the most common orthotopic pattern is of a right intercostobronchial trunk and two separate left bronchial arteries. The right intercostobronchial trunk has branches supplying the bronchi and the chest wall, and it typically originates from the posteromedial wall of the aorta. The left bronchial arteries typically arise along the anterior wall of the aorta, although an origin from the right posteromedial aorta or even the right intercostobronchial trunk has been observed. Occasionally, a right and left bronchial artery will arise from a common trunk along the anterior thoracic aorta ( Fig. 45-1 ). Less common or aberrant sites of origin of the bronchial arteries include the thoracic aortic arch (typically from the concavity, but also from the convexity), the subclavian artery and its branches, the internal thoracic artery, the brachiocephalic trunk, and the abdominal aorta (see Fig. 45-1 ). Important anastomoses of the bronchial arteries include contributions to the anterior spinal artery, branches to the esophagus, anastomoses to the coronary arteries, and anastomoses to the pulmonary arteries, particularly in the setting of chronic lung disease. Of these anastomoses, contributions to the anterior spinal artery are the most feared aspect of bronchial artery intervention because inadvertent embolization results in potential paralysis. Evaluation of the bronchial arteries has traditionally required catheter angiography. The improved quality of high-resolution multidetector row CT (MDCT) has enabled visualization of the origin and course of the bronchial arteries before intervention and can be a helpful aid in the evaluation of hemoptysis.
Orthotopic Bronchial Artery Origin
Right intercostobronchial trunk; two left bronchial arteries
Right intercostobronchial trunk; one left bronchial artery
Right intercostobronchial trunk and one additional right bronchial artery; two left bronchial arteries
Right intercostobronchial trunk and one additional right bronchial artery; one left bronchial artery
Common trunk supplying a right and left bronchial artery
Aberrant Bronchial Artery Origin
Aortic arch (mostly from concavity)
Subclavian artery (ipsilateral or contralateral)
Descending aorta; abdominal aorta
Brachiocephalic trunk
Internal thoracic artery
Thyrocervical trunk
Pearls and Pitfalls
- ▪
Bronchial artery anatomy is variable; 70% of bronchial arteries arise from the descending aorta at the T5 to T6 vertebral body level.
- ▪
Aberrant origins of the bronchial arteries are commonly seen from the concavity of the thoracic aortic arch, but they can also be found from the convexity of the arch, the subclavian artery and its branches, the internal thoracic artery, and the abdominal aorta.
- ▪
A potential communication of the bronchial arteries with the anterior spinal artery should always be scrutinized before intervention.
Computed Tomography Technique for Imaging the Bronchial Arteries
If CT is being performed for a case of hemoptysis, the examiner must obtain high-resolution images with thin-slice collimation and considerable overlap. MDCT angiographic protocols are preferable, particularly because evaluation of lung parenchyma, with its intrinsic high contrast, is less dependent on the phase of vessel opacification. Slice thickness of 1.25 mm with 0.625-mm overlapping increments allows for high-resolution reformations, to visualize the origin and course of the bronchial arteries most clearly. Imaging parameters with most 16- and 64-row MDCT scanners include 80- to 140 kilovolt peak (kVp) range, 90 to 140 mA, a 10-mm beam width, and a beam pitch of 1.2 to 1.5. A contrast injection rate of at least 3.5 mL/second with a power injector through an 18-gauge cannula is suggested. Typically, 80 to 120 mL high-density nonionic contrast agent (300 to 350 mg/dL) is used with either bolus tracking or an 18-second delay to begin scanning at peak arterial enhancement. These parameters usually provide adequate opacification of both systemic and pulmonary arterial vasculature in the regions of interest.
The scan should ideally span the base of the neck to the level of the renal arteries, to capture potential aberrant origins of the bronchial arteries, as well as major sources of potential nonbronchial systemic collateral vessels. With 16- or 64-detector row scanners, the entire scan may be performed in a single breath hold. Sagittal and coronal reformations are routinely performed using the raw data in the axial thin-section images, with additional two-dimensional and three-dimensional reformations and volume rendered images as necessary on a case by case basis. Imaging the origin and course of the bronchial arteries in this way provides information valuable to the interventionalist in planning potential embolization, and it may also assist a surgeon for planning potential vessel ligation.
Pearls and Pitfalls
- ▪
Thin-collimation MDCT technique provides the best current resolution for identifying the origin and course of the bronchial arteries.
- ▪
Sagittal, coronal, two-dimensional, and three-dimensional reformation techniques may all be used to improve visualization of the origin and course of the bronchial arteries.
- ▪
Scan should extend from the base of the neck to the level of the renal artery origins, to identify any aberrant origins of the bronchial arteries and common sources of potential nonbronchial systemic collateral vessels.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree