Bunionette
Anatomic Considerations
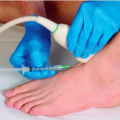
The metatarsophalangeal joints are condyloid joints characterized by the articulation of the rounded articular surfaces of the metatarsal heads into the shallow concavities of the articular surfaces of the proximal end of the first phalanges (Fig. 20.1). Each joint is lined with synovium and the ample synovial space allows for intra-articular placement of needles for injection and aspiration. The metatarsophalangeal joints have a dense joint capsule and strong plantar and collateral ligaments, although fracture and subluxation may still occur (Figs. 20.2 to 20.4). The metatarsophalangeal joints are also susceptible to overuse and misuse injuries with resultant inflammation and arthritis.
Clinical Correlates
Bunionette, which is also known as the tailor’s bunion, refers to a constellation of symptoms including soft tissue swelling over the fifth metatarsophalangeal joint associated with abnormal angulations of the joint that results in a prominent fifth metatarsal head (Fig. 20.5). Ultimately, the fifth metatarsophalangeal joint may sublux, and a corn overlying the metatarsal head will develop along with an inflamed adventitious bursa may coexist with the bunionette, further exacerbating the pain and cosmetic deformity (Figs. 20.6 and 20.7). Occurring more commonly in women, bunionette is most commonly the result of wearing shoes with a too-tight toe box, with the wearing of high-heeled shoes exacerbating the problem.
Most patients who present with bunionette also present with the complaint of pain that is localized to the affected fifth metatarsophalangeal joint and the inability to get shoes to fit. Walking makes the pain worse, with rest and heat providing some relief. The pain is constant and is characterized as aching and may interfere with sleep. Some patients complain of a grating or popping sensation with use of the joint and crepitus may be present on physical examination. In addition to the just-mentioned pain, patients who suffer with bunionette develop the characteristic bunionette deformity, which consists of a prominent fifth metatarsal head and improper angulation of the fifth metatarsal (Fig. 20.8).
Functional disability often accompanies the pain of the bunionette joint. Patients will often notice increasing difficulty in performing their activities of daily living and tasks that require standing, walking, or weight bearing. If the pathologic process responsible for pain of bunionette is not adequately treated, the patient’s functional disability may worsen and muscle wasting and ultimately a frozen fifth metatarsophalangeal joint may occur.
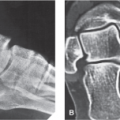
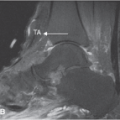
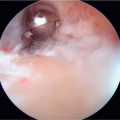
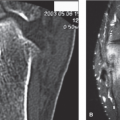
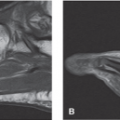
Plain radiographs are indicated in all patients who present with pain of the bunionette (Figs. 20.9 and 20.10). Based on the patient’s clinical presentation, additional testing may be indicated, including complete blood cell count, sedimentation rate, and antinuclear antibody testing. MRI or ultrasound of the bunionette joint is indicated if fracture, effusion, tendinopathy, crystal arthropathy, joint mice, synovitis, foreign body, bursitis, or ligamentous injury is suspected (Fig. 20.11).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree