Key Points
- ▪
The conventional test of choice to identify coronary artery dissections is standard coronary angiography.
- ▪
Cardiac CT angiography shows some early ability to depict coronary artery dissection; validation is limited.
Although coronary artery dissections are rare overall (0.1–0.3% incidence in angiographic series), when they do occur it is usually within the settings of the pregnant or peripartum state, blunt chest trauma, iatrogenesis, or severe exertion or stress, or associated with one of several medical conditions (see Etiologies and Associations).
Coronary artery dissections may be single or multiple and may involve all three coronary arteries and the left main stem coronary artery.
Repeated angiography may reveal regression or healing, although progression has been described, as has recurrence, and conventional catheter-based angiography may initiate coronary artery dissection.
Some coronary artery dissections, usually iatrogenic ones, may propagate retrograde back into the aortic root. Most spontaneous coronary artery dissections remain within the coronary tree.
Etiologies and Associations
- □
Hormone-associated
- •
Oral contraception–related
- •
Pregnancy-associated
- •
Mid-term
- •
Third trimester
- •
Twin pregnancy
- •
- •
Peri-/postpartum–associated
- •
Post-abortion
- •
Menstruation-associated
- •
Postmenopausal
- •
- □
Nonhormone-associated
- •
Iatrogenic
- •
Coronary angiography
- •
Percutaneous coronary intervention
- •
Plain old balloon angioplasty (POBA)
- •
Coronary artery stenting (bare metal; drug-eluting)
- •
Cutting balloon
- •
Intracoronary radiation
- •
Intravascular ultrasound (IVUS)
- •
- •
Cryoablation for atrial fibrillation
- •
Coronary artery bypass grafting
- •
- •
Drug abuse–associated
- •
Cocaine abuse
- •
Ergotamine abuse
- •
- •
Drug-associated
- •
Fenfluramine
- •
5-FU
- •
- •
Hypertension-associated
- •
Retching-associated
- •
Weight-lifting–associated
- •
- •
Acute aortic dissection (type A)
- •
Acute aortic dissection, despite repair of the dissected aorta
- •
Supravalvular aortic stenosis
- •
Disease-associated
- •
Active inflammatory bowel disease
- •
Systemic lupus erythematosus
- •
Polycystic kidney disease
- •
Renal transplantation–associated
- •
Anti-phospholipid antibody
- •
Alpha-1 antitrypsin–associated
- •
Pulmonary embolism
- •
- •
Vascular disease–associated
- •
Eosinophilic monoarteritis
- •
Fibromuscular dysplasia
- •
Coronary ectasia
- •
- •
Inheritable connective tissue disorder
- •
Marfan syndrome
- •
Cystic medial necrosis
- •
- •
Exertion
- •
Skiing at altitude
- •
Wrestling
- •
Exercise/athleticism/strenuous workouts
- •
- •
Neurofibromatosis (type 1—vasculopathy-associated)
- •
Stress-associated
- •
Sleep deprivation (72 hours)
- •
Depression
- •
Emotional stress
- •
- •
Sexual intercourse
- •
Blunt chest trauma
- •
Clinical Presentations of Spontaneous Dissections
- □
Chest pain
- □
Stable angina (likely due to organization/evolution of dissection into a coronary artery stenosis or occlusion)
- □
Acute coronary syndrome
- □
Myocardial infarction (MI)
- •
ST-elevation myocardial infarction (STEMI)
- •
Non-STEMI
- •
- □
Transient ST elevation
- □
Sudden death
- □
Atrial fibrillation and tamponade due to rupture of the dissected artery
- □
Tamponade due to rupture of the dissected artery
- □
Aortic dissection–like
- □
Stroke (due to coronary dissection resulting in MI)
Ischemic presentations dominate. It has been suggested that inadvertent use of thrombolytics for STEMI due to spontaneous coronary dissection may predispose the coronary dissection to extension. Arrhythmic presentations and sudden death are relatively common for this diagnosis. Rupture of the artery with tamponade has been described, as have other indirect complications or presentations. Multivascular occurrences (e.g., stroke, renovascular disease) should prompt consideration of vasculitides, including the inheritable variants and fibromuscular dysplasia.
Diagnostic Testing for Coronary Dissections
Conventional angiography has been and remains the standard diagnostic test to diagnose coronary artery dissections, although, unfortunately, it may also cause coronary dissection. IVUS, performed at the time of angiography, is able to visualize a subset of coronary dissection cases that are ambiguously represented on angiography. Transesophageal echocardiography (TEE) has detected spontaneous coronary dissection, but would be expected to have very limited ability to interrogate the coronary tree. TEE would be able to image dissection of the aorta extending into a coronary artery, or coronary dissection extending into the aortic root.
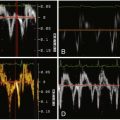
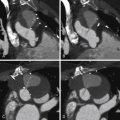
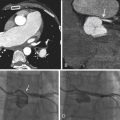
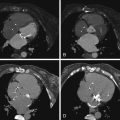
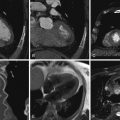
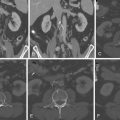
Coronary CT angiography (CTA) has been used to image coronary artery dissections (see Figures 12-1 through 12-10 ).