, Valery Kornienko2 and Igor Pronin2
(1)
N.N. Blockhin Russian Cancer Research Center, Moscow, Russia
(2)
N.N. Burdenko National Scientific and Practical Center for Neurosurgery, Moscow, Russia
The term “demyelinating disease” (DD) of the central nervous system refers to primary, usually idiopathic, abnormal processes that cause the destruction of the normal myelin development. Such diseases currently include multiple sclerosis in the classical form, its atypical variants (Marburg disease, Balo sclerosis, Schilder’s disease), and inflammatory demyelinating pseudotumor (IDP). In addition, demyelinating diseases include diseases with secondary demyelination and destruction of myelin, such as acute disseminated encephalomyelitis (ADEM), progressive multifocal leukoencephalopathy (PML), HIV leukoencephalopathy, and some slowly demyelinating leukoencephalitis of viral etiology. It must be emphasized that demyelinating diseases are characterized by focal, multiple, and asymmetric white matter lesions, due to which it can often acquire an MRI picture similar to that with secondary tumor lesions.
Demyelinating diseases are characterized by specific MR signal changes on T1-weighted, T2-weighted, and T2-FLAIR MRI. The entire group of demyelinating diseases, in contrast to other processes accompanied by contrast enhancement, is characterized by a specific and often unique sign allowing to make the correct diagnosis: a so-called “partial” type of contrast enhancement observed in some lesions, in the form of “half-rings” or “incomplete rings.”
41.1 Multiple Sclerosis
It is a chronic, progressive autoimmune disease of the central nervous system, manifested by diffuse neurological symptoms and having a relapsing-remitting course in its initial stages in typical cases (Adams and Victor 1993). The history of the disease study begins in 1835, when the French pathologist J. Kruvelie described “spotted” or “insular” sclerosis. MS is considered the best understood in the group of demyelinating diseases, but its etiology is still unclear. Etiological hypotheses consider an infection, autoimmunity to normal myelin, a combination of infectious and autoimmune processes, and toxic and metabolic causes of MS. Currently, the most common is the hypothesis of multifactorial etiology of MS, according to which the disease develops, when a certain combination of external factors affects genetically susceptible individuals, causing chronic inflammation, autoimmunity, and demyelination of the white matter in the CNS. The genetic predisposition to MS remains unproven; however, the development of MS has been established to be most strongly associated with HLA class II DR2 haplotype. The role of other genes in the etiology of MS, as well as the possibility of a combination of different genetic factors, is still discussed.
In the majority of cases, these lesions have a relatively homogeneous MR signal and clear limits with the white matter. The form of MS plaques may be the most diverse, varying from round to irregular one. However, rounded lesions are encountered more often; they are identified mainly in the periventricular region and semioval centers and less frequently in the corpus callosum and subcortical structures. Individual plaques can be located in the projection of the brainstem and cerebellar hemispheres. On T1-weighted MRI, in relapsing-remitting MS, the plaques are not visible in most cases and only individual lesions are identified, which are characterized by a slightly hypointense MR signal. This group is also characterized by the absence of visualization of subtentorial plaques in T1-weighted images.
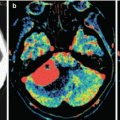
MS plaques may accumulate the contrast agent, reflecting transient BBB disorders. Contrast enhancement is used in MS to identify more or less specific features in the hyperintensity picture of multiple foci in T2-weighted images. It is known that the simultaneous detection of both contrast-enhanced and non-contrast-enhanced lesions is a characteristic of MS and puts in question other diagnoses (Fig. 41.1).
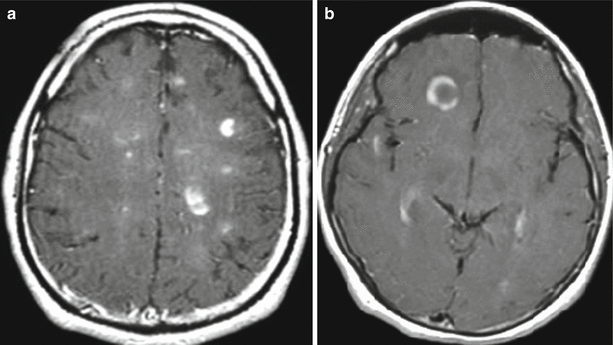

Fig. 41.1
Multiple sclerosis. a, b On T1-weighted MRI with contrast enhancement, multiple areas of its abnormal accumulation are observed. In “active” MS lesions, diffuse and annular types of contrast enhancement (a, b), as well as the partial type, half-ring accumulation, are observed
The diffuse type of contrast enhancement is characterized by opacification of an entire plaque. This type of contrast enhancement is a characteristic for multiple, small demyelination foci (a few millimeters in size). The annular type of contrast enhancement is observed with the accumulation of contrast agent in peripheral portions of larger foci—in the form of a ring. The dimensions of these lesions usually approach 1 cm or more. This type of contrast enhancement is a characteristic for plaques with the presence of a perifocal edema detectable in T2-weighted and DW images. This partial type of contrast enhancement, from our point of view, is the most pathognomonic for demyelination foci in MS, in general, and is manifested in the form of partial CA accumulation within the area of abnormal changes in the intensity of an MR signal detected by T2-weighted MRI. At the same time, the attention should be drawn to contrast enhancement of MS plaques in the form of a “half-ring” or a “half-moon,” when an increase in the MR signal intensity on post-contrast T1-weighted images is observed only in a limited area on the plaque periphery, not confined to annular opacification (Fig. 41.2).
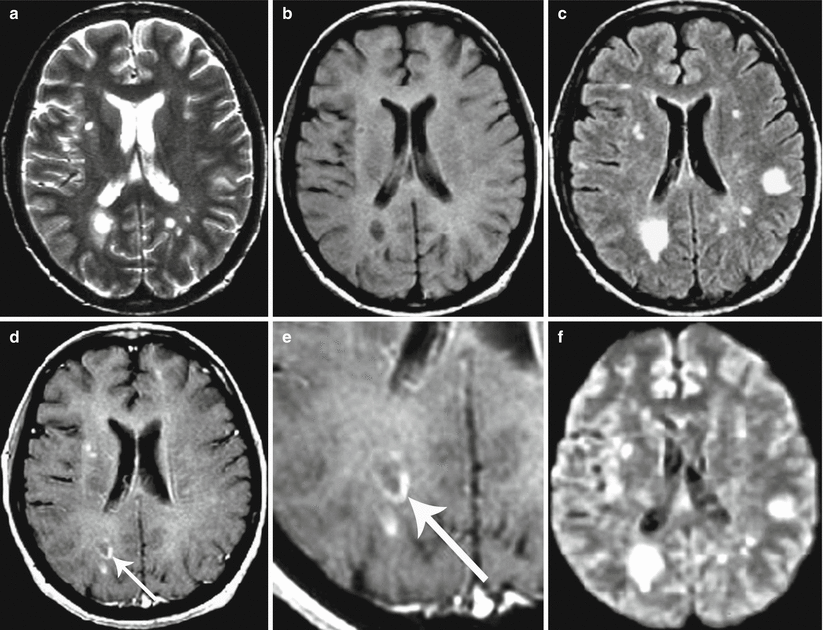

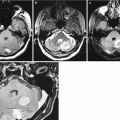
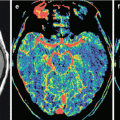
Fig. 41.2




Multiple sclerosis. On T2-weighted (a), T1-WI (b), T2-FLAIR (c), and T1-weighted MRI after intravenous contrast enhancement (d, e), there are multiple areas with an altered signal. Contrast enhancement in the form of a “half-ring” is observed along the edge of one of the portions (indicated by the arrow). All lesions are hyperintensive on T2-FLAIR (c). On DWI (f), the signal from demyelination foci is increased
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree