CHAPTER 20 Endoscopy of the upper and lower gastrointestinal tract
Indications
Types of endoscopy
Upper gastrointestinal endoscopy
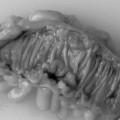
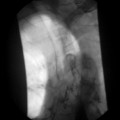
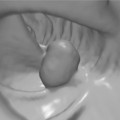
To prepare for upper gastrointestinal endoscopy patients are asked not to eat or drink for 4–6 hours prior to the procedure. The procedure can be done under local anesthetic to the throat or under sedation. The gastroscope is passed via the mouth, through the cricopharyngeal sphincter and into the esophagus. Once intubation is achieved the examination of the esophagus, stomach and duodenum is relatively straightforward (Figures 20.3, 20.4 and 20.5, see color insert). There are several blind spots that merit special attention. The view of the esophageal mucosa is often lost at the point of passage through the sphincter and lesions can be missed. If this is suspected, the patient should undergo a barium swallow or a rigid esophagoscopy. Another potential blind spot is the superior part of the gastric antrum and angulus. It is important to retroflex the gastroscope in the antrum to gain a good view of this area.
Small bowel endoscopy
Enteroscopy is used to examine mainly the proximal small bowel. This is a much more involved procedure than gastroscopy. Enteroscopy is indicated for diagnosis of small bowel diseases including obscure gastrointestinal bleeding, malabsorption, obtaining tissue biopsies following abnormal fluoroscopic studies as well as therapeutic procedures for treating small bowel bleeding or polyps.
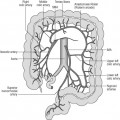
Colorectal endoscopy
Visualization of the lower bowel can be performed using a rigid or flexible endoscope. Rigid sigmoidoscopy and proctoscopy usually occur in the outpatient clinic. The Association of Coloproctology of Great Britain and Ireland recommends that a patient referred for barium enema should have had at least a rigid sigmoidoscopy prior to referral (Guidelines for Management of Colorectal Cancer, 2007). The reason for this is that lesions very low down in the rectum may be missed on barium enema but seen on proctoscopy or rigid sigmoidoscopy. A rigid examination is especially important in patients presenting with bright red rectal bleeding as common pathologies such as distal proctitis or hemorrhoids may not be demonstrated on barium enema.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree