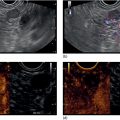
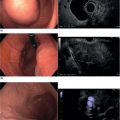
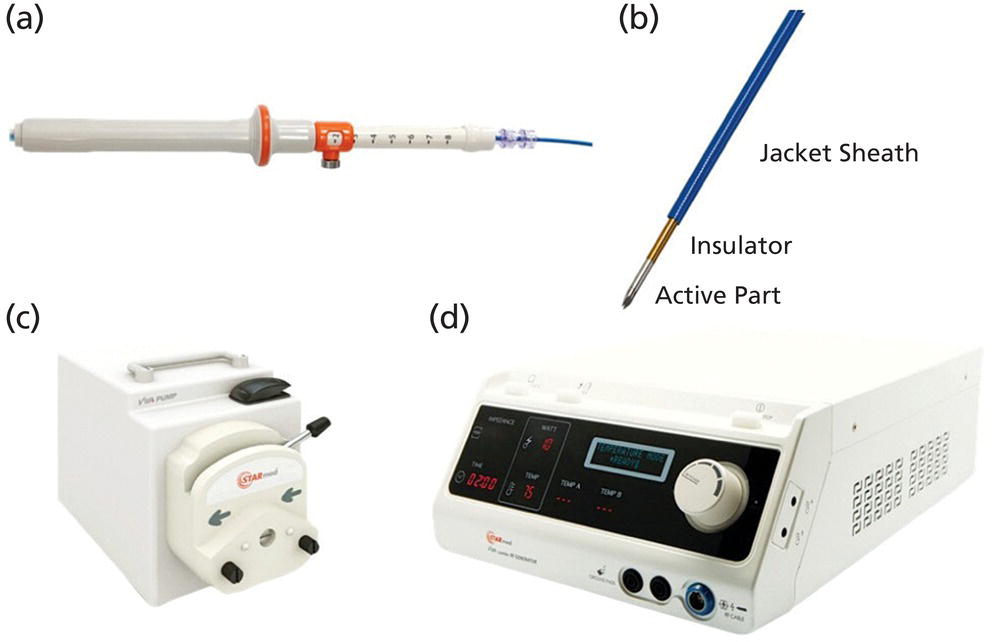
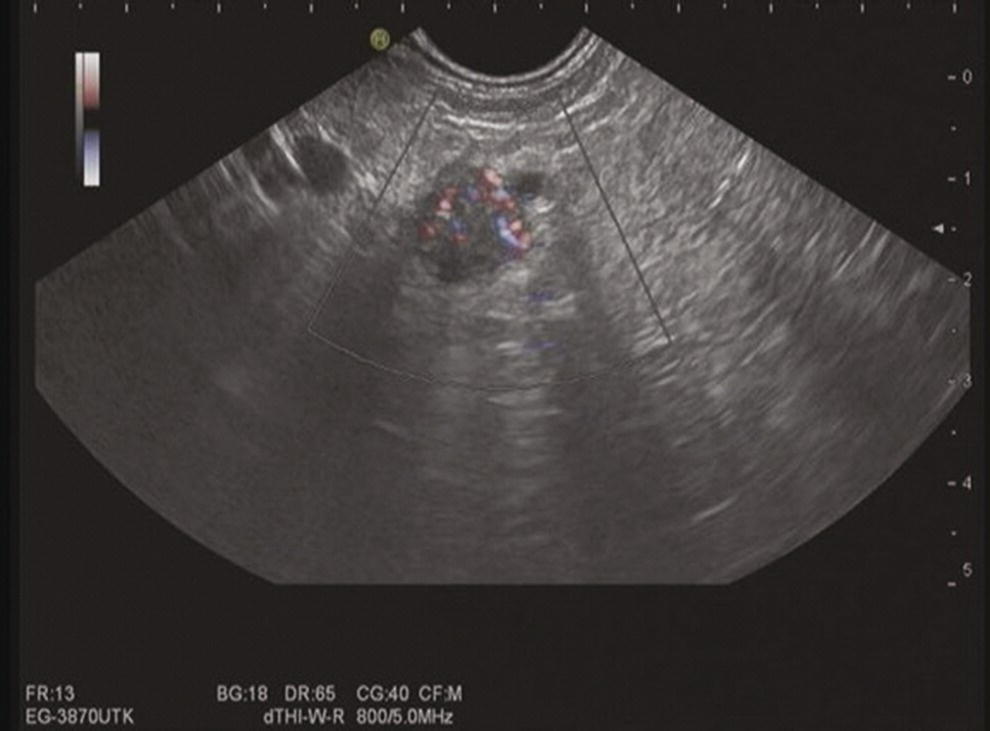
Sabrina Gloria Giulia Testoni, Gemma Rossi, Livia Archibugi, and Paolo Giorgio Arcidiacono San Raffaele Scientific Institute IRCCS, Vita‐Salute San Raffaele University, Milan, Italy In recent years pancreatic neuroendocrine tumors (pNETs) have shown a dramatic increase in terms of incidence and prevalence, especially since the widespread use of imaging studies and their better resolution. pNETs are classified mostly for the ability to secrete hormones and cause a specific syndrome (functional, F‐pNETs, with gastrinoma and insulinoma being the most frequent) or not (non‐functional, NF‐pNETs), and for the expression of Ki‐67. Despite the prominent role of surgery as curative treatment, the complications of pancreatic surgery in this type of disease remain frequent: Jilesen and colleagues reported pancreatic fistula in 14–58% of the cases, delayed gastric emptying in 15–18%, postoperative bleeding in 1–7%, and in‐hospital mortality in 4–6%, depending on the type of surgical resection. It is therefore intuitive how minimally invasive locoregional ablative techniques under endoscopic ultrasound (EUS) guidance can have a prominent role. The factors to be taken into account when deciding the management of the patient with pNET are either patient related (comorbidities, risk of postoperative complications, life expectancy, risk of postoperative endocrine and exocrine insufficiency) or pNET related (F vs. NF, stage, number of lesions, size, grading, location of the lesion), which are also strictly linked to the known risk of progression. It is therefore intuitive to consider ablation of localized lesions with a risk of progression or unfavorable outcome (F‐pNETs, lesions >2 cm, high Ki‐67 index) but at high risk of perioperative/postoperative complications. ENETS guidelines from 2016 reported the possibility of locoregional ablation of localized insulinomas that were not candidates for surgery, despite little evidence. Exclusion of lymph nodes, liver, and other distant metastases is of paramount importance when enrolling a patient for locoregional ablation. For F‐pNETs the goal is to induce necrosis of as many cells as possible in order to reduce the secretion of hormones and therefore abolish the related syndrome. For other pNETs and in other situations (MEN‐1, NF‐pNETs, etc.), there are currently no indications. The two main techniques currently under evaluation for EUS‐guided ablation of p‐NETs are radiofrequency ablation and ethanol injection. Radiofrequency ablation (RFA) works at high temperatures (60 and 100°C), inducing thermally irreversible cellular damage on target tissues, with eventual cellular apoptosis and coagulative necrosis. The ablated area after RFA shows three well‐recognized zones: a central coagulative necrosis, a surrounding peripheral zone with sublethal injury, and an external healthy surrounding zone. Despite numerous clinical oncologic applications (liver, kidney and prostate gland cancers and metastasis), RFA of pancreatic tumors has always been regarded with reluctance by clinicians for fear of serious adverse events (such as pancreatitis, perforation, peritonitis, and adjacent structural injury). However, EUS‐guided RFA could provide undoubted advantages in pancreatic tumor ablation, i.e. real‐time imaging and monitoring during treatment, the ability to reach extremely distant anatomic areas, and minimally invasive technique. Two EUS‐guided RFA monopolar (requiring grounding pads) systems are available on the market. The equipment is composed of an 18‐ or 19‐gauge needle (EUSRA) inserted in the echoendoscope operative channel (length 140 cm, monopolar electrode located on the distal part, available in lengths of 5, 10, 15, 20, 25, and 30 mm), a radiofrequency generator (VIVA, STARmed) releasing the energy, and a peristaltic pump connected to the needle, which is cooled and internally perfused by circulating chilled saline solution during the ablation to avoid tissue charring (and maximizing ablation volume). Ablation power can be set on the generator, and tissue impedance and current are continuously monitored: the system can automatically modulate the power during the ablation if tissue impedance quickly increases or can eventually stop if the impedance (and temperature) rises beyond safety thresholds (impedance ≥500 Ω; temperature >100°C). The equipment is composed of a 1‐Fr wire (0.33 mm, 0.013 inch) catheter (length 190 cm, electrode located on the distal part) that can be inserted in a standard 19‐ or 22‐gauge EUS needle (with stylet removed), a RITA generator (electrosurgical RF generator) releasing the energy and monitoring the temperature in real time, and a remote foot pedal for hands‐free and device activation. Both systems do not have specific ablation settings (power, time) for treating pancreatic solid lesions such as pNETs. Previous experiences has shown heterogeneity in ablation settings (power and time) and results, with no procedure standardization (Table 50.1). Figure 50.1 EUS‐RFA radiofrequency system. a) EUSRA (STARmed, Goyang, South Korea) needle (sizes 18 or 19‐gauge). (b) EUSRA needle tip: terminal part is the “active part” (electrode), available in sizes of 5, 10, 15, 20, 25, and 30 mm. (c) Peristaltic pump connected to the needle, cooled and internally perfused by circulating chilled (0°C) saline solution in order to avoid tissue charring. (d) VIVA radiofrequency generator (STARmed). Source: (a–d) STARmed, Seoul, South Korea. Figures 50.2–50.4 and Videos 50.1 and 50.2 show an EUS‐guided RFA procedure for the treatment of a symptomatic pancreatic tail insulinoma; Figures 50.2 and 50.3 and Video 50.1 show diagnostic evaluation before RFA while Figure 50.4 and Video 50.2 show the appearance of the lesion during the RFA procedure. Patient showed relief of symptoms. EUS‐guided ethanol injection (EI) was first successfully used by Jurgensen and colleagues in 2006 for ablation of F‐pNETs (insulinoma). Ethanol is a low‐viscosity sclerosing agent able to induce cell lysis, denaturation of proteins and vascular occlusion, leading to coagulative necrosis and cell death. Subsequently, EUS‐guided EI was proposed also for treatment of NF‐pNETs in patients not eligible for surgical resection, and various small case series and case reports have been published. However, with a median follow‐up of 20 months (range 2–48 months), the reported outcomes were heterogeneous, with cases where morphologic disappearance of pNET, clinical complete resolution and biochemical normalization were achieved even after only one EI session, and other cases where only a partial response was obtained or there was tumor size reduction only after multiple sessions or injection of large volumes of alcohol leading to a high rate of postprocedural pancreatitis. In fact, this technique is not free from adverse events, with some graded as severe. Among complications reported in the literature are cases of moderate‐graded acute pancreatitis, necrotizing acute pancreatitis, fever, and duodenal wall ulceration. Ethanol volumes in excess of 2 ml and concentration above 98% were most associated with the occurrence of pancreatitis. This therapeutic technique is performed using a 22‐ or 25‐gauge EUS‐FNA needle that is inserted into the pNET, not extending beyond the tumor margins. Needles with multiple side holes are not indicated for EI. Subsequently, a small amount of ethanol is injected inside the pNET, in varying concentrations (40–98%) and volumes (0.1–8 ml) depending on the size of the lesions. If necessary, as for larger lesions, additional injections can be performed during needle withdrawal. Before needle removal, it may be held within the lesion for a short time (approximately 60 seconds) in order to minimize the tracking of ethanol into peripheral normal pancreatic tissue. Depending on tumor size and the degree of spread of ethanol during intratumoral perfusion, multiple injections at different lesion sites may be performed during the same session until the tumor is entirely covered by a hyperechoic “cloud” that visibly expands within the tumor under EUS guidance. The injection should be stopped if the hyperechoic “cloud” extends up to the tumor’s border to prevent leakage of ethanol beyond the tumor. Table 50.1 EUS‐guided radiofrequency ablation for treatment of pNETs: literature review. NA, not available. Multiple sessions of EUS‐guided EI can also be performed if the pNET persists morphologically on imaging controls or symptoms related to F‐pNET are still present. Up to three sessions have been reported, with rates of tumor ablation varying from 54% after one session to 62% after two sessions. In order to avoid procedure‐related adverse events if the pNET is close to a vessel or the main pancreatic duct, it has been proposed that an ethanol volume equivalent to half or one‐third of the calculated tumor volume is injected. Recently, EUS‐EI combined with Lipiodol, an iodized poppy seed oil, was used successfully in treatment of pNETs of less than 2 cm (22‐gauge needle, mean 1.9 sessions per patient and 1.6 sessions per tumor, median mixture volume per session of 1.1 ml, 99% ethanol), obtaining complete ablation in 45% and 60% of tumors after one and two sessions, respectively,with occurrence of mild to moderate pancreatitis in 3.2% of cases. Figure 50.2 EUS‐guided radiofrequency ablation of a pancreatic tail symptomatic insulinoma: Doppler evaluation. Figure 50.3 EUS‐guided radiofrequency ablation of a pancreatic tail symptomatic insulinoma: elastography evaluation. Figure 50.4 EUS‐guided radiofrequency ablation of a pancreatic tail symptomatic insulinoma: EUS aspect of the insulinoma after ablation showing a hyperechoic area covering the center of the lesion. Technical variables reported in different case series and case reports vary widely, and include the needle type and caliber, volume injected, concentration of alcohol, and techniques to minimize the risk of pancreatitis (Table 50.2). Therefore, further studies with technical refinements, larger sample population, and long‐term follow‐up are needed in order to standardize the technical methodology and reduce the reported high rate of postprocedural pancreatitis, and to prove the efficacy of this technique. While for F‐pNETs it is intuitive how ablative techniques could become a standard of care, for NF‐pNETs this is still under debate, especially since it is not entirely clear yet which tumors will progress and which will not. The answer will be reached once new studies regarding both ablative techniques and the actual risk of progression for small NF‐pNETs have been published. The hope is that, in the future, the low risk of complications of such procedures (compared to surgery) and the high rate of success of EUS‐guided ablative procedures will make them a possible first‐line therapeutic method for pNETs at high risk of unfavorable outcome, once solid reliable evidence is obtained.
50
How to do EUS‐guided Ablation of Pancreatic Neurendocrine Tumors
Introduction and indications
Techniques
EUS‐guided radiofrequency ablation
Technical aspects of EUS‐guided RFA
EUS RFA System (STARmed, Goyang, South Korea) (Figure 50.1)
Habib™ EUS RFA (EMcision Ltd, London, UK)
EUS‐guided ethanol injection
Technical aspects of EUS‐guided EI
Study
N
Indication
Patient selection
Device
Thermokinetics
Size (mm)
Outcome
Complications
Rossi et al. (2014)
1
pNET
Refusing or unfit for surgery
Habib EUS‐RFA catheter, Emcision Ltd, London
10–15 W
16
Complete radiologic ablation
None
Lakhtakia et al. (2015)
3
F‐pNETs
Unfit for surgery
EUSRA RF electrode; STARmed, Goyang, Korea
50 W
17.7
Symptom resolution
None
Armellini et al. (2015)
1
pNET
Refusing surgery
EUSRA RF electrode; STARmed, Goyang, Korea
NA
20
Complete radiologic ablation
None
Pai et al. (2015)
2
NF‐pNETs
NA
Habib EUS‐RFA catheter, Emcision Ltd, London
20 W
27.5
Change in vascularity and central necrosis
None
Waung et al. (2016)
1
F‐pNET
Failure of medical therapy, unfit for surgery
Habib EUS‐RFA catheter, Emcision Ltd, London
10 W
18
Complete radiologic ablation
Symptom resolution
None
Bas‐Cutrina et al. (2017)
1
F‐pNET
Unfit for surgery
Habib EUS‐RFA catheter, Emcision Ltd, London
10 W
10
Complete radiologic ablation
Symptom resolution
None
Choi et al. (2018)
8
1 F‐pNET
7 NF‐pNETs
Unfit for surgery
EUSRA RF electrode; STARmed, Goyang, Korea
50 W
20
Complete radiologic ablation
1 abdominal pain, 1 pancreatitis
Barthet et al. (2018)
14
NF‐pNETs
pNET <2 cm, patient unfit or refusing surgery
EUSRA RF electrode; STARmed, Goyang, Korea
50 W
13.1
Complete radiologic ablation
1 mild pancreatitis
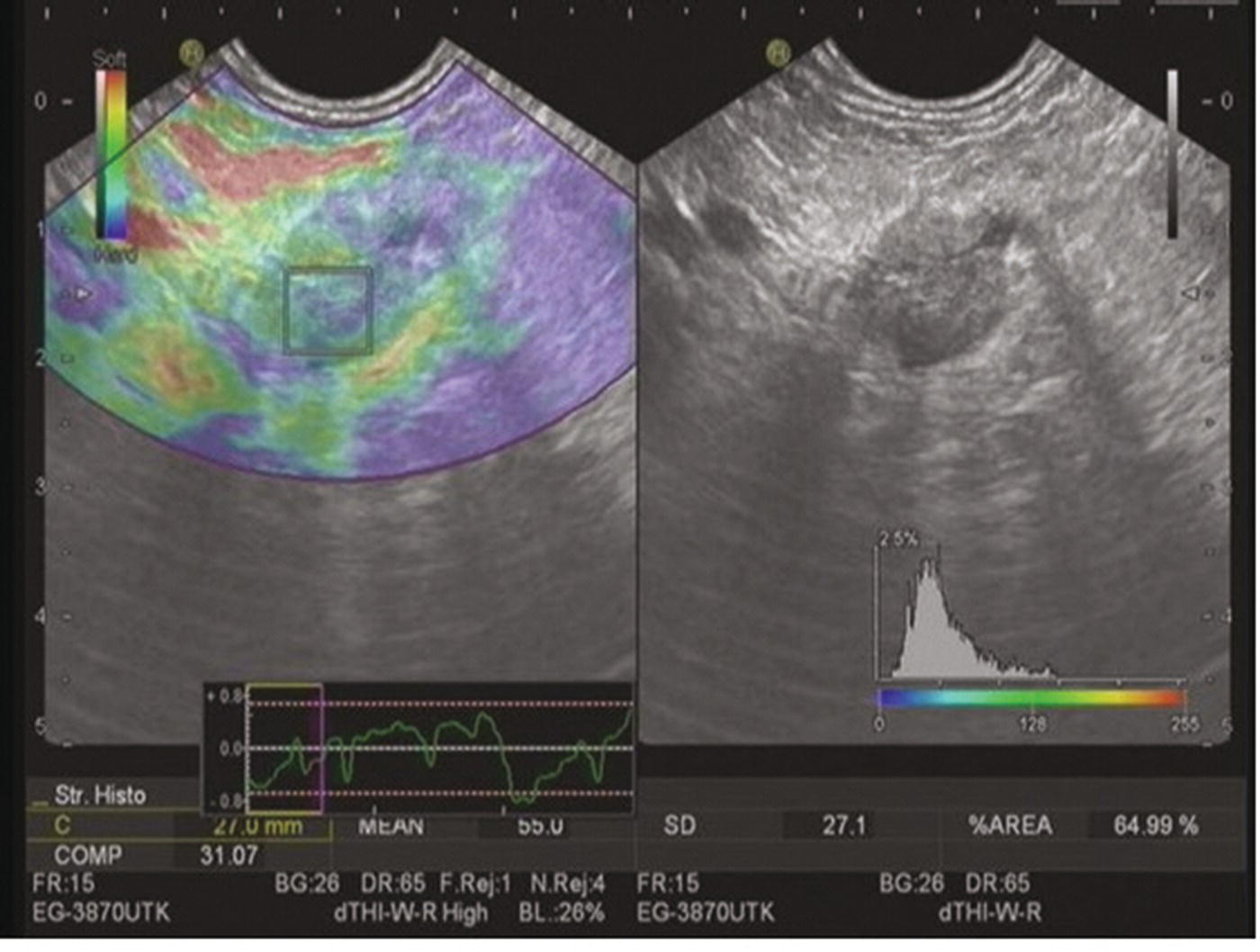
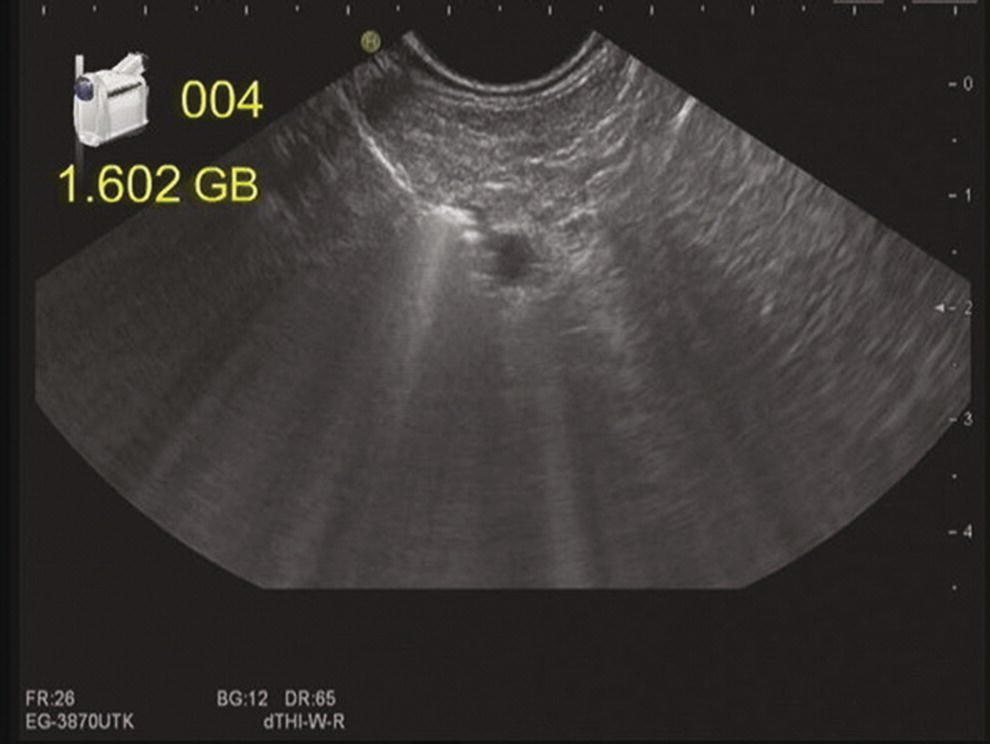
Conclusion and future perspectives
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree