There is a wide variety of causes of diffuse lung disease in the intensive care unit patient, of which adult respiratory distress syndrome is the commonest clinical consideration. Plain radiography, computed tomography, and ultrasound can be used synergistically to evaluate patients with diffuse lung disease and respiratory impairment. Imaging is not limited to characterization of the cause of diffuse lung disease but also aids in monitoring its evolution and in ventilator setting management.
Key points
- •
There is a wide variety of causes of diffuse lung disease in the intensive care unit patient, of which adult respiratory distress syndrome is the commonest clinical consideration.
- •
Plain radiography, computed tomography, and ultrasound can be used synergistically to evaluate patients with diffuse lung disease and respiratory impairment.
- •
Imaging is not limited to characterization of the cause of diffuse lung disease but also aids in monitoring its evolution and in ventilator setting management.
Introduction
Clinical evaluation of the intensive care patient is multifactorial but relies to a great extent on pulmonary imaging. Numerous primary pulmonary diseases or systemic disorders may affect the lung independently or may superimpose on a preexisting lung disorder. Clinical assessment can be complex in the intensive care unit (ICU) setting, making the interpretation of lung disease contribution challenging. However, determining the cause of the diffuse lung disease (DLD) is crucial because characterizing the mechanisms can optimize both the etiologic and the symptomatic treatment. The principal cause of DLD is the clinical syndrome of adult respiratory distress syndrome (ARDS), which often constitutes a common challenging radiological pattern in the ICU population; however, DLD is not limited to ARDS. The main causes of DLD and diffuse lung injury are pneumonia, aspiration, nonpulmonary sepsis, major trauma, pulmonary contusion, acute exacerbation of idiopathic pulmonary fibrosis (AE-IPF), inhalational injury, severe burns, noncardiogenic shock, pancreatitis, drug overdose, multiple transfusions, or transfusion-associated acute lung injury (TRALI), pulmonary vasculitis, and near drowning.
Imaging plays a significant role in the detection and characterization of DLD. However, the role of modern radiology is not limited to this remit. Applications of multimodality imaging also include respiratory management and monitoring during lung recruitment and lung protection strategies. Current and novel imaging modalities aim to evaluate the effectiveness of the therapeutic interventions by providing functional information optimizing lung assessment during ventilator management.
This article focuses on the clinicoradiological aspects of the detection, characterization, and radiologically assisted management of the principal causes of diffuse interstitial lung disease (ILD) presenting as clinical management issues in the adult ICU patient, with a particular focus on ARDS and its differentiation from other common similarly presenting causes of DLD.
Adult respiratory distress syndrome: direct and indirect lung injury
ARDS is the most frequently associated clinical entity to DLD in the ICU patient. It is characterized by an acute inflammatory lung injury in a heterogeneous group of patients with respiratory insufficiency hours to days after a severe local or systemic insult. Three overlapping pathologic phases have been described following direct insult to the alveolar epithelium (eg, pneumonia or gastric acid) or indirect to the pulmonary capillary endothelium (eg, pancreatitis, extrapulmonary sepsis). The exudative or early phase, which lasts for the first week after the onset of symptoms, is histologically characterized by diffuse alveolar damage (DAD). The proliferative or intermediate phase occurs from day 5 to 7 onwards and can last for a further week, characterized by organization of the exudates. In patients who do not recover, a final fibrotic or late phase can begin as early as day 10 after the initiating injury and is histologically characterized by fibroplasia.
Following the first description of ARDS by Ashbaugh and colleagues, there have been several attempts to describe and clarify the syndrome with a reliable definition. The 1994 American-European Consensus Conference definition of ARDS was the first to become globally accepted. However, there were several concerns regarding the timing, origin of edema, oxygenation, severity, and imaging description criteria of the syndrome. The most recent 2012 “Berlin” international expert consensus panel addressed these limitations. Specifically, the acute timeframe was specified; 3 subgroups of ARDS by severity were created (mild, moderate, and severe); the acute lung injury (ALI) term and pulmonary artery wedge pressure requirement were removed; a ventilation minimal positive end-expiratory pressure (PEEP) level was incorporated; and imaging criteria were clarified ( Table 1 ).
| Timing | Onset of ARDS must be acute, defined as within 7 d |
| Imaging | Bilateral opacities, not fully explained by effusions, lobar/lung collapse, detected on chest radiograph or CT |
| PAWP: origin of edema | There is no need to exclude heart failure in the new ARDS definition |
| Oxygenation Pa o 2/ Fi o 2 | 3 subgroups by severity/degree of hypoxemia Mild (<300 mm Hg), moderate (<200 mm Hg), severe (<100 mm Hg) |
ARDS reflects a clinicoradiologically diverse spectrum of disease, course, and prognosis, influenced by the etiologic mechanism. ARDS cause is generally classified as due to direct causes of lung injury, such as pneumonia or aspiration, and indirect causes of lung injury, such as nonpulmonary sepsis or transfusion. Accordingly, these pulmonary and extrapulmonary causes result in different pathophysiology, with resultant varying radiological patterns and consequent effects on respiratory mechanics and responses to ventilator settings.
The radiological description of ARDS in daily practice remains often confusing regarding the appropriate terminology. Although ARDS is a clinical diagnosis, it is often used in the radiology reports interchangeably with ALI and with the histopathologic and pathophysiology terms of DAD and increased permeability edema. Because the diagnosis remains a clinical determination, and radiology has a supportive role, the radiology report should be descriptive and indicate appearances suggestive of ARDS and, if appropriate, the cause, infective or extrapulmonary, to direct clinical corroboration and appropriate treatment and management.
Despite optimized therapy, ARDS is associated with appreciable morbidity and mortality. In a large observational study, based on the 2012 Berlin criteria, a 28-day mortality of 30%, 35%, and 43% was observed for mild, moderate, and severe ARDS, respectively.
Acute interstitial pneumonia
Acute interstitial pneumonia (AIP), previously known as Hamman-Rich syndrome, is reserved for ARDS of unknown cause. It is a rapidly progressive idiopathic clinical disorder associated with DAD. AIP radiologically resembles ARDS with similar clinical presentation. However, the different clinical management and the poor prognosis with greater than 70% mortality at 3 months despite mechanical ventilation make the determination of AIP versus other causes of ARDS of paramount importance. Open lung biopsy is, therefore, frequently indicated to confidently confirm AIP and exclude other causes.
Ventilator-associated pneumonia
Ventilator-associated pneumonia (VAP) is defined as pneumonia that occurs more than 48 hours following endotracheal intubation. It is the most common nosocomial infection in mechanically ventilated patients in the ICU. A combination of clinical criteria, the Clinical Pulmonary Infection Score (CPIS), has been proposed for VAP diagnosis. These clinical criteria include radiological evaluation on a chest radiograph (CXR). New findings of pulmonary infiltrates in a patient with fever or hypothermia, leukocytosis or leukopenia, purulent tracheal secretions, and impaired oxygenation are highly indicative of VAP ( Table 2 ). To detect these pulmonary infiltrates, current American Thoracic Society guidelines recommend CXR and computed tomography (CT) for VAP diagnosis. However, in mechanically ventilated patients, such pulmonary infiltrates are frequent and may be associated with multiple causes. Therefore, imaging determination of VAP in the critical care setting remains problematic.
| Criteria | CPIS Points |
|---|---|
| Temperature | ≥36.5 or ≤38.4 = 0 point ≥38.5 or ≤38.9 = 1 point ≥39 or <36.5 = 2 point |
| Leukocyte count | ≥4000 or ≤11.000 = 0 point <4000 or >11.000 = 1 point Band forms ≥50% = add 1 point |
| Tracheal secretions | Absent = 0 point Tracheal secretion with less purulence = 1 point Abundant purulent secretion = 2 points |
| Oxygenation | Pa o 2 /Fi o 2 <200 = 0 point Pa o 2 /Fi o 2 , mm Hg ≤240 or ARDS = 2 points |
| Chest radiograph | No infiltrate = 0 point Diffuse infiltrates = 1 point Local infiltrates = 2 points |
| Chest radiograph progression (day 2–3) | No progression (−) = 0 point Progression (+) (after the exclusion of heart failure and ARDS) = 2 points |
| Microbiological culture (day 2–3) | No growth or few pathogenic bacteria = 0 point Moderate or high levels of pathogenic bacteria = 1 point Pathogenic bacteria seen on Gram staining = add 1 point |
Acute exacerbation of interstitial lung disease
Patients with fibrotic lung disease can develop acute respiratory failure because of an exacerbation of their underlying disease. Identifying and managing this type of respiratory failure remains clinically challenging. The diagnostic workup includes imaging with high-resolution computed tomography (HRCT) as part of an initial assessment identifying signs of fibrosis and most typically a background pattern consistent with usual interstitial pneumonia pattern. According to an international multidisciplinary working group consensus, the recently updated diagnostic criteria of acute exacerbation of IPF have been defined as an acute (<1 month in duration) and clinically significant respiratory deterioration in a previously diagnosed IPF patient, associated with the presence of new widespread alveolar abnormality on HRCT and exclusion of alternative causes. Because respiratory failure in IPF has a poor prognosis, imaging plays a significant role in the distinction of acute exacerbation of IPF from infection to guide appropriate management demanding increased immunosuppression rather than antimicrobial treatment.
Imaging
Chest Radiography
For several decades, CXR evaluation was the only imaging modality in the assessment of DLD in critically ill patients to assess progression, stability, or regression in concordance with direct or indirect pulmonary insults. However, the radiographic appearance is recognized to be frequently nonspecific, including bilateral, symmetric, or asymmetric airspace consolidative opacification with air bronchograms that may reflect infection, or ARDS. The coexistence of septal lines and pleural effusions makes interpretation more challenging, favoring the coexistence of cardiogenic pulmonary edema, a common confounder in the ICU setting. Volume loss may be appreciated in the later phases of interstitial pulmonary fibrosis, indicating a background of ILD in a patient with potential acute exacerbation. However, the volume loss of IPF is frequently basilar and, therefore, may overlap in appearance with the basilar volume loss of hypoinflation atelectasis, which is common in ventilated patients.
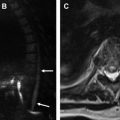
ARDS is the commonest consideration for DLD on ICU chest radiographs. The radiographic findings vary depending on the phase of the disease mirroring the histopathologic phase. The CXR may be normal in the first hours of the syndrome. The progression of the disease during the early exudative phase (1–2 days) is typically of bilateral patchy alveolar airspace opacities with progression to confluent consolidation in the late exudative phase (3–7 days) ( Fig. 1 A). Thereafter, in the proliferative phase (day 5–7 onwards), the consolidation becomes progressively extensive and dense ( Fig. 1 B). If the syndrome persists for at least 7 to 10 days, early fibrotic changes with a coarse reticular pattern begin to evolve ( Fig. 1 C–E). An exception to the generally bilateral progressive appearance is if ARDS is triggered by a direct lung injury (eg, pneumonia), in which case early asymmetric focal or multifocal consolidation may be observed.

Undoubtedly, chest radiographs are of assistance in determining the presence, and monitoring the evolution, of cardiogenic edema and fluid overload, differentiating these common causes for diffuse parenchymal abnormality in the ICU patient from ARDS. The typical features of cardiogenic edema are well recognized: progressing from septal lines and central peribronchovascular interstitial edematous changes to alveolar edema with diffuse airspace abnormalities that may resemble infection or ARDS. Typically, effusions may be present, although these are a nonspecific feature also seen in infection and other conditions. Similarly, the heart is usually enlarged, although this feature may be absent in patients with acute cardiogenic shock, acute renal impairment, or acute fluid overload. Asymmetry of appearances may be postural or indicate noncardiogenic edema, particularly in cases of opiate overdose. The role of chest radiography has also been investigated as a possible guide for fluid management, measuring the changes of a simple anatomic landmark, such as the vascular pedicle width. According to a study by Rice and colleagues, the vascular pedicle width measurement on a CXR appears to correlate highly with pulmonary artery occlusion pressure distinguishing cardiogenic from noncardiogenic edema and suggesting a fluid management protocol. In a recent study, a radiographic severity score of lung edema (RALE score) has been developed quantifying the severity of pulmonary edema in ARDS. The study showed that the RALE score is associated with ARDS severity, response to conservative fluid management, and clinical outcomes.
Daily routine CXR for DLD, and more specifically ARDS, remains a common practice in most ICU departments. Indeed, the American College of Radiology’s Appropriateness Criteria recommend daily routine CXRs for patients with mechanical ventilation. CXRs are also recommended immediately following the placement of tubes, catheters, and other monitoring devices to check their position and detect procedure-related complications. In a study by Henschke and colleagues, the routine use of daily CXR detected malposition of tubes and lines in 12% and 1%, respectively, and provided useful information affecting patient management in 65% of studies. However, more recent metaanalysis data suggest that daily routine CXRs can possibly be eliminated because the observed daily variations are minor and are unlikely to alter clinical management and decision making.
The use of daily chest radiographs is supported by the new definition of ARDS, whereby radiographic criteria are more explicitly stated, defining the syndrome by the presence of bilateral opacities consistent with pulmonary edema not fully explained by effusions, lobar collapse, or nodules. However, specificity, even in the context of ARDS, remains low. The Berlin definition statement also underscores the limits of CXRs, recommending that CXR criteria should be clarified by creating a set of example radiographs. The limitations of chest radiography in ARDS include not only a lower accuracy compared with other image modalities but also a high interobserver variability in the radiographic definition of ARDS. Figueroa-Casas and colleagues demonstrated that the accuracy of anteroposterior chest radiograph in the diagnosis of ARDS is limited, resulting generally in underrecognition of ARDS, particularly when nondiffusely distributed, but also in other circumstances, overdiagnosis of the syndrome. Indeed, in daily practice, it remains difficult to differentiate ARDS from infection and cardiogenic and noncardiogenic pulmonary edema because they frequently coexist. Although this limitation has been partially addressed with the new definition, ICU CXR interpretation remains a consistent challenge for radiologists attempting to appropriately guide ICU clinicians. Compared with other modalities, several studies have demonstrated the lower-diagnostic accuracy of chest radiography for alveolar consolidation, pleural effusions, and alveolar or interstitial pathology compared with CT and ultrasound (US). In practice, CXR, CT, and lung US should be used in a complementary fashion rather than used interchangeably.
Computed Tomography
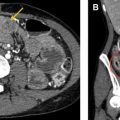
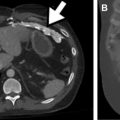
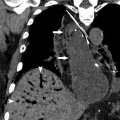
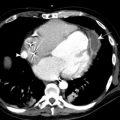
CT is perhaps the most consistently useful imaging tool in the evaluation of DLD and ARDS in the ICU patient. A progressive understanding of CT imaging patterns has offered insights into both clinical aspects and the pathophysiology of acute lung illness in critical patients. Several studies have illustrated the superiority of CT in the imaging and follow-up of DLD in the ICU context. In 1 study, the imaging findings provided by CT compared with CXR frequently yielded additional information (66%), with direct influence on patient treatment in 22% of cases. CT is also important in providing further information regarding complications, such as iatrogenic line or tube insertions and ventilation-associated complications (barotrauma) ( Fig. 2 ). The improved imaging characterization by CT, and in particular HRCT reconstructions, can assist in the differentiation of ARDS from pulmonary edema and other clinical causes of DLD.