Infections of the Head and Neck
Srikar Adhikari
INTRODUCTION
Head and neck infections are common presentations to the emergency department (ED) and vary in their need for urgent treatment. Common conditions such as pharyngitis, tonsillitis, cellulitis, uncomplicated sialoadenitis, and lymphadenitis can be treated with outpatient oral antibiotics or symptomatic therapy. Other conditions such as peritonsillar abscesses, dental abscesses, suppurative sialoadenitis, and neck abscesses often require urgent treatment in the ED and may require imaging to diagnose and characterize them, and to determine involvement with surrounding structures. Physical examination findings in patients with head and neck complaints are not always sufficient. Most of the structures and conditions in this region lie between 1 and 5 cm below the skin, making them well suited to evaluation by ultrasound (1). Ultrasound can detect abscesses not identified on clinical examination and is very reliable in identifying lymphadenitis, sialoadenitis, thyroid masses, and infected congenital cysts. Ultrasound can successfully differentiate between cellulitis, abscess, and adenitis, and is very accurate in distinguishing cystic from solid masses, benign from malignant lymphadenopathy, and intra- from extraglandular abnormalities of the salivary glands. The sensitivity and specificity for detecting some of these lesions have been found to be comparable to other imaging modalities such as computerized tomography (CT) and magnetic resonance imaging (MRI) (2). Ultrasound has a number of advantages in comparison with x-ray, CT, and MRI: It is readily available, noninvasive, repeatable, rapid, inexpensive, and nonionizing.
In recent years, the role of point-of-care head and neck ultrasonography in the ED has expanded dramatically. Bedside ultrasound is being increasingly used in the evaluation of head and neck soft tissue masses, paranasal sinuses, and detection and treatment of peritonsillar abscesses (3). Head and neck ultrasound has moved from being an imaging modality confined to the radiology department to an active bedside diagnostic and therapeutic tool available to the clinicians at the point of patient care. Clinician-based ultrasound allows emergency physicians to evaluate patients with suspected head and neck infections in a rapid and cost-effective manner.
THE PARANASAL SINUSES
Clinical Applications
Rhinosinusitis is a common disorder affecting more than 30 million adults in the United States every year (4). Antibiotics are generally considered beneficial in the treatment of acute bacterial sinusitis; however, only 50% of patients presenting to the ED with sinus symptoms actually have acute bacterial sinusitis (5). Accurate diagnosis of acute sinusitis is challenging since signs and symptoms of bacterial sinusitis are nonspecific and distinguishing between rhinitis and sinusitis is not always simple (6). Although imaging studies such as CT and MRI improve diagnostic accuracy, these are not routinely used for diagnosing uncomplicated sinusitis in ambulatory settings due to additional costs, time, and radiation risk.
Ultrasound has become a tool for diagnosing acute maxillary sinusitis during the last two decades. It is safe, quick, noninvasive, inexpensive, and repeatable. It is very sensitive in detecting fluid in sinus cavities. Accuracies exceeding 90% for diagnosing maxillary sinusitis have been reported in Otolaryngology (ENT) practices (6,7). Results from ENT practices may not be generalizable to other settings, due to differences in patient populations and severity of disease. When bedside ultrasound performed by emergency physicians is compared to CT in ED patients with suspected maxillary sinusitis, the sensitivity and specificity are 81% and 89%, respectively (8). Ultrasound is an accessible imaging alternative to the more expensive or invasive diagnostic modalities.
Clinician-performed sinus ultrasound can be used to:
Evaluate patients with suspected maxillary sinusitis.
Distinguish rhinitis from acute maxillary sinusitis.
Detect nosocomial sinusitis as an occult cause of fever in intubated patients in intensive care settings.
Image Acquisition
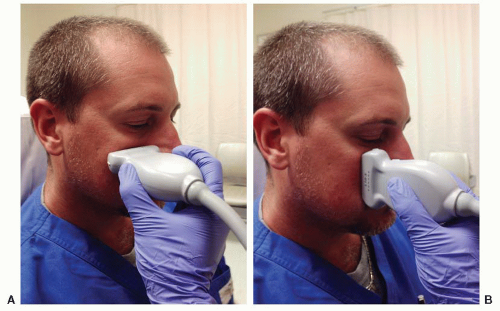
The paranasal sinuses that are amenable for bedside scanning are maxillary and frontal sinuses. However, frontal sinuses are not well seen on ultrasound due to the thick anterior surface of frontal bone. A high frequency (7 to 13 MHz) linear array transducer is typically used to perform an ultrasound examination of the maxillary sinus. Alternatively, a phased array or a micro convex transducer can also be used. The examination is done with the patient in an upright position with the head bent slightly forward so that sinus fluid, if present, will layer in the floor of the sinus against the anterior wall (Fig. 24.1). A large amount of ultrasound gel is applied to the maxillary area. The transducer is placed in a transverse plane, beneath the orbit and lateral to the nose. Without applying any pressure, the maxillary area is scanned both in sagittal and transverse planes between the nose and the zygoma to demonstrate the full extent of the sinuses. The scanning hand should be stabilized over the facial bones to prevent sliding. The scan is performed initially in a transverse plane, angling the probe from the orbital floor to the floor of the sinus. This is followed by rotating the transducer 90 degrees and scanning in a sagittal plane, from the medial to the lateral wall of the maxillary sinus. The depth setting should be appropriately adjusted so that the sinus fills approximately three-quarters of the screen and the posterior wall of the sinus is visualized well. The contralateral side should be scanned routinely for comparison.
Normal Anatomy
The pyramidal-shaped maxillary sinus is located within the body of the maxilla bounded by the orbital floor superiorly, the hard palate inferiorly, the zygoma laterally, and the nasal cavity medially. It is 2 to 4 cm deep anteroposteriorly. The normal maxillary sinus is filled with air that prevents the transmission of ultrasound. Normally, aerated sinuses
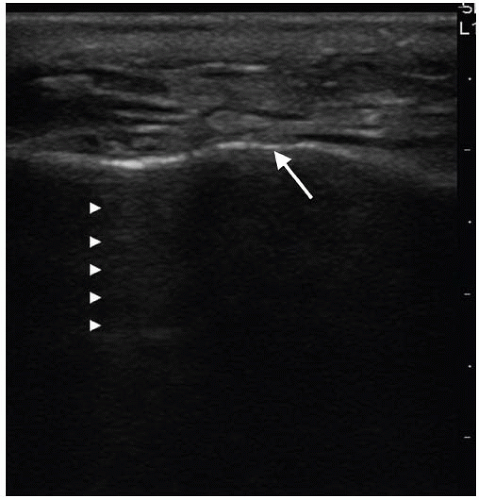
reflect most of the ultrasound signal, preventing visualization of structures deep to the air. The anterior wall of the maxillary sinus is seen as a bright echo, behind which rever-beration artifact is seen. Reverberation artifact generates a series of evenly spaced horizontal echogenic lines parallel to the anterior surface of the maxilla that diminish in intensity at increasing depth (Fig. 24.2). This gives a snowstorm appearance to a normal air-filled sinus. The posterior wall of the sinus is not visualized in a normal nonopacified sinus (9).
reflect most of the ultrasound signal, preventing visualization of structures deep to the air. The anterior wall of the maxillary sinus is seen as a bright echo, behind which rever-beration artifact is seen. Reverberation artifact generates a series of evenly spaced horizontal echogenic lines parallel to the anterior surface of the maxilla that diminish in intensity at increasing depth (Fig. 24.2). This gives a snowstorm appearance to a normal air-filled sinus. The posterior wall of the sinus is not visualized in a normal nonopacified sinus (9).
Pathology
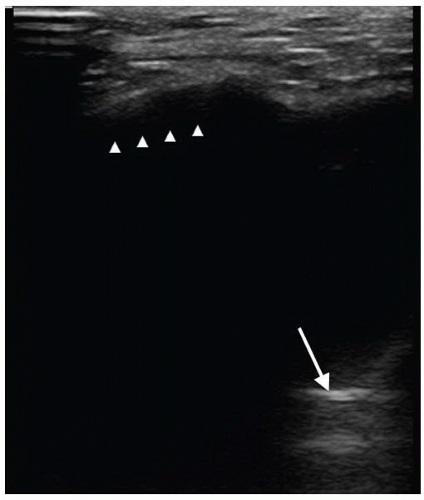
Acute maxillary sinusitis is characterized by edema, mucosal thickening, and fluid collection within the sinus cavity. When the sinus cavity is filled with fluid, the ultrasound signal penetrates the anterior wall, travels through the fluid-filled sinus cavity, strikes the posterior and lateral walls, and returns to the transducer, resulting in an image of the entire sinus cavity. The fluid-filled maxillary sinus is seen as a triangular hypoechoic cavity with well-defined lateral, medial, and posterior walls. This creates an image referred to as a sinusogram. The total opacification of the completely fluid-filled maxillary sinus results in a complete sinusogram where the posterior wall of the sinus is clearly seen and no reverberation artifacts are visualized (Fig. 24.3). However, if the sinus is only partially filled with fluid, partial visualization of the walls can occur due to the presence of an air-fluid level within the sinus cavity. This is called a partial sinusogram, where all walls are not well defined (Fig. 24.4). This appearance is also seen with mucosal thickening (10). Postural scanning maneuvers can help in differentiating acute sinusitis from mucosal thickening.
Lichtenstein et al. prospectively investigated the significance of sinusograms in critically ill patients who underwent maxillary sinus CTs. The maxillary sinus ultrasound was always positive (complete or partial sinusogram) when the CT revealed complete opacification of the sinus. The ultrasound was always negative when CT showed a normal sinus. The sensitivity of ultrasound was 67% and the specificity was 87% for the diagnosis of maxillary sinusitis (total opacification or air-fluid level within the maxillary cavity on CT). The specificity of complete sinusogram was 100% for the diagnosis of total opacification of the sinus (10).
Artifacts and Pitfalls
The thickness of the anterior wall of the sinus can limit the ability of ultrasound to penetrate fluid-filled sinus cavities.
Air bubbles near the anterior wall of the sinus can degrade the ultrasound signal, resulting in the appearance of an incomplete or partial sinusogram.
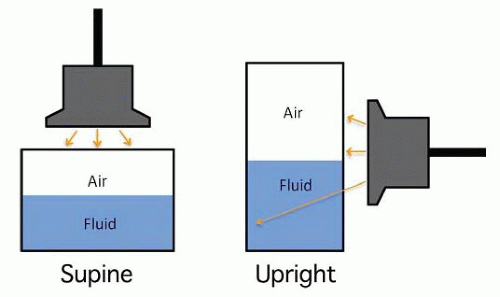
A partial sinusogram cannot differentiate sinusitis with a partially fluid-filled sinus cavity from that with mucosal thickening. However, dynamic scanning maneuvers can help make this distinction. The patient’s position while scanning influences the appearance of the sinus fluid in a partial sinusogram. In the supine position, fluid can layer out away from the anterior wall and create an airfluid interface. Ultrasound cannot penetrate the overlying air, resulting in either acoustic shadowing or a partial sinusogram. The partially aerated sinus may not allow visualization of the posterior wall when the patient is supine. In contrast, when the examination is performed in an upright position, the fluid will layer out inferiorly in the floor of the sinus and come into contact with the anterior wall. On ultrasound, this results in either a partial or complete sinusogram, depending on the amount of fluid present in the sinus cavity and the orientation of the transducer (Figs. 24.4 and 24.5) (9). In sinusitis, the posterior wall of the sinus is seen in the fluid-filled portion of the sinus cavity, and reverberation artifact is seen in the air-containing region of the sinus. In mucosal thickening there is no significant change in the appearance of the image in the upright position since there is no fluid in the sinus cavity.
Reverberation artifacts located deep in the sinus cavity can be confused for the posterior wall of the sinus.
Sonographic findings of sinusitis are not helpful in differentiating between a viral or bacterial etiology. Similar abnormalities (partial or complete sinusogram) are noted with both conditions. Other conditions such as polyps, cysts, and mass or blood in the sinus masses can also produce the appearance of a sinusogram.
The sensitivity of ultrasound for maxillary sinusitis is approximately 85% (11). If clinical suspicion is high, other imaging modalities or consultation should be considered.
Use of the Image in Clinical Decision Making
In daily clinical practice, the diagnosis of acute maxillary sinusitis is most often based on symptoms and clinical examination findings, although these have been shown to be unreliable in differentiating acute sinusitis from upper respiratory infection. As a result, it is likely that a significant number of patients receive antibiotics for viral respiratory tract infections leading to the alarming global threat of increasing antimicrobial resistance. Conversely, undiagnosed sinusitis can lead to pain, return ED visits, and other complications such as pneumonia, meningitis, and intracerebral abscesses. Maxillary sinus ultrasound is a safe, rapid, painless, noninvasive bedside procedure to detect fluid in the maxillary sinus cavity. If sinusitis is diagnosed or excluded using bedside ultrasound, unnecessary antibiotic use could be potentially reduced. If a complete sinusogram is seen, further imaging studies can be avoided, and the patient can be treated with antibiotics for sinusitis. Appropriate consultation can be obtained for a drainage procedure if necessary.
Correlation with Other Imaging Modalities
Imaging modalities used for the diagnosis of maxillary sinusitis include x-ray, CT, and MRI. Standard x-rays are rarely used in current clinical practice because of low sensitivity. CT is highly sensitive for sinusitis, and is generally considered the imaging procedure of choice for the diagnosis of sinusitis. Common CT findings for sinusitis include air-fluid levels, mucosal edema, and air bubbles within the sinuses. Because of radiation exposure with this imaging technique, CT should be considered only in situations such as recurrent sinusitis, chronic sinusitis, and treatment failures. MRI is not routinely used in the evaluation of patients with suspected sinusitis. MRI provides better visualization of soft tissue than CT and is useful in the assessment of complications of acute sinusitis when extra sinus involvement is suspected. While CT is more sensitive than plain x-ray, and MRI is more sensitive than CT, the specificity of these studies is unclear. In both children and adults without symptoms of sinusitis, the prevalence of sinusitis on CT and MRI is 45% and 42%, respectively (12). In patients with no symptoms of sinusitis, 32% to 60% had mucosal thickening, opacification, fluid, or polyps in their sinuses (13). Hence, the use of CT and MRI is limited by false-positive findings seen in
healthy, asymptomatic individuals. Additionally, both imaging modalities are expensive and time-consuming. A positive culture from fluid obtained on sinus puncture is the true gold standard for diagnosing bacterial sinusitis, but it is an invasive procedure not readily accepted by all patients and rarely utilized.
healthy, asymptomatic individuals. Additionally, both imaging modalities are expensive and time-consuming. A positive culture from fluid obtained on sinus puncture is the true gold standard for diagnosing bacterial sinusitis, but it is an invasive procedure not readily accepted by all patients and rarely utilized.
Ultrasonography is a rapid, inexpensive, and readily available tool for evaluation of maxillary sinuses, features that make it an optimal diagnostic method in the ED. In a comparative study done by Puhakka et al., ultrasound and plain x-rays of the paranasal sinuses were performed on 197 young adults within 48 hours of the onset of symptoms of the common cold (11). Forty randomly selected patients also received MRI. A diagnosis of acute maxillary sinusitis was made in 24% of the sinuses by plain x-rays, and in 28% by MRI. Compared with MRI, the sensitivity and specificity of ultrasound for detection of maxillary sinusitis were 64% and 95%, respectively. Based on these study findings, positive ultrasound findings can be regarded as evidence of maxillary sinusitis. In a systematic review conducted by Varonen et al., the efficacies of clinical examination, ultrasound, and radiography as diagnostic measures for acute maxillary sinusitis were evaluated (7). Ultrasound findings were considered positive for sinusitis if scans showed the presence of a posterior echo ≥3.5 cm from the anterior echo. Seven studies compared ultrasonography to sinus puncture and revealed a sensitivity of 85% and specificity of 82% for ultrasound. In another study done by Varonen et al., the overall sensitivity of ultrasound compared to x-rays was 92% and specificity was 95% when results were calculated per patient as unit of analysis (14).
Ultrasound is easy to perform, nonionizing, and provides an alternative to CT and MRI in the diagnosis of maxillary sinusitis. While ultrasound is less sensitive than CT and MRI in detecting mucosal changes and identification of fluid in sinus cavity, it is probably more specific in diagnosing clinically significant disease since a significant amount of sinus fluid is required to produce sonographic abnormalities.
PHARYNGITIS
Clinical Applications
Acute pharyngitis accounts for approximately 12 million ambulatory visits per year in the United States (15). The differential diagnosis for pharyngitis includes parapharyngeal space infection, peritonsillar abscess, submandibular space infection (Ludwig angina), Lemierre syndrome, and epiglottitis. Peritonsillar abscess (abscess in the area between the palatine tonsil and its capsule) is the most common deep space infection of the head and neck, with an incidence estimated at 30 cases per 100,000 annually in the United States (16). Peritonsillar abscess is often described as part of a spectrum of disease beginning with tonsillitis, progressing to peritonsillar cellulitis, and culminating in peritonsillar abscess. The abscess develops as a complication of acute follicular tonsillitis with the infection spreading from the tonsillar crypts, penetrating the capsule, and localizing in the peritonsillar region (17). The diagnosis of peritonsillar abscess can be challenging. History and clinical examination alone cannot be used to reliably differentiate peritonsillar cellulitis from peritonsillar abscess. The sensitivity and specificity of physical examination to diagnose a peritonsillar abscess has been shown to be around 75% and 50% respectively (18). It is, however, important to distinguish between these two conditions since they require very different treatments. Peritonsillar cellulitis is generally treated with antibiotics, whereas a peritonsillar abscess usually requires aspiration or incision and drainage in combination with antibiotics. If not treated promptly, peritonsillar abscess can lead to complications such as parapharyngeal abscess, retropharyngeal space and mediastinal extension, jugular vein thrombophlebitis, cavernous sinus thrombosis, brain abscess, meningitis, or pneumonia (19). Traditionally, emergency physicians have used anatomic landmark-based blind needle aspiration in patients with clinically suspected peritonsillar abscess. Blind needle aspiration has a reported false-negative rate of 10% to 12%, (17) and has been associated with injuries to the carotid artery, jugular vein, and parotid gland. In the recent years, bedside ultrasound has emerged as an extremely valuable tool in the diagnosis and management of peritonsillar abscess in the ED. Lyon et al. used intraoral ultrasound to diagnose and treat bilateral peritonsillar abscesses (3). Blaivas et al. also reported the use of intraoral ultrasound by emergency physicians to diagnose and successfully aspirate peritonsillar abscess and found ultrasound to be 100% accurate in their series (20). In a recent prospective randomized controlled study involving 28 patients with suspected peritonsillar abscess, intraoral ultrasound established an accurate diagnosis more often than a landmark approach, resulted in more successful aspiration of purulent material, and decreased the need for specialty consultation and CT scan (18).
Ultrasound is helpful in determining the presence, size, and anatomic location of a peritonsillar abscess, and in identifying the relationship of the abscess to the carotid artery. The main clinical indications for the use of ultrasound in the evaluation of peritonsillar infections in the ED are:
To distinguish peritonsillar abscess from peritonsillar cellulitis.
To provide real-time guidance to aspirate peritonsillar abscess.
To evaluate other complications such as Lemierre syndrome.
Image Acquisition
Sonographic evaluation of suspected peritonsillar abscess is usually performed with a high frequency (4 to 9 MHz) curved array intracavitary transducer, as is used for transvaginal sonography. A small amount of gel is applied to the transducer, followed by a protective sheath such as a condom. Gel may be placed on the outside of the probe sheath; however, moist oropharyngeal mucosa allows transmission of ultrasound without gel. A topical anesthetic should be sprayed in the posterior pharynx prior to the exam for patient comfort to reduce gagging. The scanning approach is shown in Figure 24.6. The tonsillar tissue should be scanned systematically in two orthogonal planes to determine the size and presence or absence of a fluid collection. The soft palate is interrogated in both the sagittal and the transverse planes with the goal of identifying the superior and inferior extent of the abscess cavity, its depth, and its position relative to the carotid artery. Doppler should be used to identify the carotid artery if it is not readily apparent. The inferior portion of the pharynx should be scanned carefully because pus
accumulates adjacent to the mid and lower pole of the tonsil in up to 40% of cases (which correlates with false-negative needle aspiration) (21). Comparison to the contralateral side may be helpful. If the patient tolerates it, gentle pressure should be applied to assess the motion of contents within the abscess cavity.
accumulates adjacent to the mid and lower pole of the tonsil in up to 40% of cases (which correlates with false-negative needle aspiration) (21). Comparison to the contralateral side may be helpful. If the patient tolerates it, gentle pressure should be applied to assess the motion of contents within the abscess cavity.
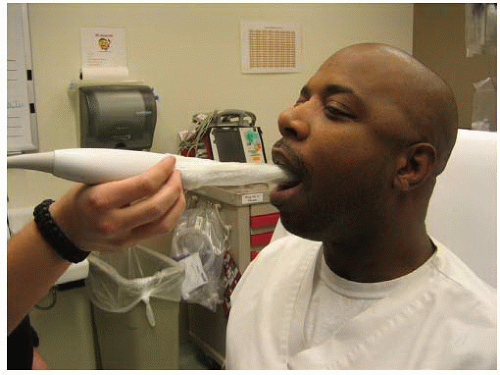 FIGURE 24.6. Intra-Oral Approach. A sheathed endocavitary transducer is inserted orally to scan the peritonsillar region after application of topical anesthesia to the posterior pharynx. |
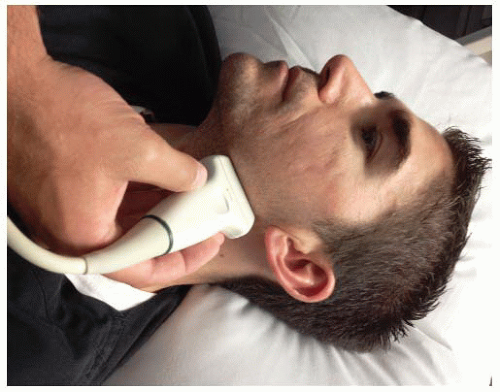
In patients with significant trismus, intraoral ultrasound with an endocavitary probe can be challenging. A transcutaneous approach has been described using a high frequency (5 to 10 MHz) linear transducer to scan the pharynx. The transducer is placed inferior and adjacent to the angle of the mandible directing posteriorly and cranially (Fig. 24.7). This approach does not require an open mouth or direct probe contact with the tonsils (22).
Normal Anatomy
The anatomy of the peritonsillar area is somewhat complex, and it is unrealistic to expect to identify all the structures in this region. These include the palatine tonsil, the margin of the bony hard palate and styloid process of the temporal bone, the medial pterygoid muscle, and various fascial planes. However, it is important to locate the internal carotid artery (anechoic tubular structure), which courses anterior to the jugular vein in the carotid sheath, and is usually located posterolateral to the tonsil within 5 to 25 mm of a peritonsillar abscess (23). Typically, the normal tonsil is seen as a small (10 to 20 mm), oval structure with homogeneous lowlevel echoes (Figs. 24.8 and 24.9).
Pathology
Peritonsillar abscess
On ultrasound, peritonsillar cellulitis appears as an enlarged tonsil (>20 mm) with a homogeneous or striated echo texture (Fig. 24.10) (17). A peritonsillar abscess usually appears as a hypoechoic, heterogeneous mass, but like all abscesses, the appearance is variable depending on the composition of the purulent material. The abscess may be isoechoic compared with the surrounding tissue in one-third of cases; however, posterior acoustic enhancement is a consistent finding (Figs. 24.11, 24.12 and 24.13;  VIDEO 24.1) (24). If the necrosis is minimal, there is less acoustic transmission, resulting in a more isoechoic pattern. Sometimes, central hypoechogenicity with an echogenic rim is seen. Any complex fluid collection inseparable from the tonsil with a mass effect regardless of the echo-pattern is more likely an abscess than cellulitis.
VIDEO 24.1) (24). If the necrosis is minimal, there is less acoustic transmission, resulting in a more isoechoic pattern. Sometimes, central hypoechogenicity with an echogenic rim is seen. Any complex fluid collection inseparable from the tonsil with a mass effect regardless of the echo-pattern is more likely an abscess than cellulitis.
 VIDEO 24.1) (24). If the necrosis is minimal, there is less acoustic transmission, resulting in a more isoechoic pattern. Sometimes, central hypoechogenicity with an echogenic rim is seen. Any complex fluid collection inseparable from the tonsil with a mass effect regardless of the echo-pattern is more likely an abscess than cellulitis.
VIDEO 24.1) (24). If the necrosis is minimal, there is less acoustic transmission, resulting in a more isoechoic pattern. Sometimes, central hypoechogenicity with an echogenic rim is seen. Any complex fluid collection inseparable from the tonsil with a mass effect regardless of the echo-pattern is more likely an abscess than cellulitis.Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree