13 Infections Definition: Maternal infection with the spirochete Treponema pallidum, which can be transmitted to the fetus. Incidence: There is regional variation, about one in 100 000 births, most frequently in maternal stage II. Origin: Contrary to many assumptions, this pathogen can cross the placental barrier at any time during the course of pregnancy. Ultrasound findings: Hydramnios, enlarged placenta, hepatosplenomegaly, ascites; in severe cases, fetal hydrops, bent long bones. Clinical features: Skin and bones are affected. Meningitis, nephritis, hepatosplenomegaly. In untreated cases, fetal demise or stillbirth occur in 50% of cases. Differential diagnosis: Cytomegalovirus infection, meconium peritonitis, parvovirus, trisomy 21, Turner syndrome. Clinical management: Maternal blood for serological testing (FTA-ABS). The pathogen can be identified either in amniotic fluid or in fetal blood samples. The mother should be treated with antibiotics. Fetal damage that may already have occurred is irreversible. Procedure after birth: Cardiac and respiratory difficulties are often present. Blood and other secretions are highly infectious. Penicillin is given for 10 days. Prognosis: At the time of birth, the neonate may appear clinically normal, but may show signs and symptoms of syphilitic disease at a later stage. Mental impairment, blindness, and sensorineural deafness are possible late sequelae. Infants with hydrops have a particularly unfavorable prognosis. References Conde-Agudelo A, Belizan JM, Diaz-Rossello JL. Epidemiology of fetal death in Latin America. Acta Obstet Gynecol Scand 2000; 79: 371–8. Crino JP. Ultrasound and fetal diagnosis of perinatal infection. Clin Obstet Gynecol 1999; 42: 71–80. Gust DA, Levine WC, St Louis ME, Braxton J, Berman SM. Mortality associated with congenital syphilis in the United States, 1992–1998. Pediatrics 2002; 109: E79–9. Hollier LM, Harstad TW, Sanchez PJ, Twickler DM, Wendel GD Jr. Fetal syphilis: clinical and laboratory characteristics. Obstet Gynecol 2001; 97: 947–53. Narducci F, Switala I, Rajabally R, Decocq J, Delahousse G. Maternal and congenital syphilis. J Gynecol Obstet Biol Reprod (Paris) 1998; 27: 150–60. Newell ML, Thorne C, Pembrey L, Nicoll A, Goldberg D, Peckham C. Antenatal screening for hepatitis B infection and syphilis in the UK. Br J Obstet Gynaecol 1999; 106: 66–71. Vieker S, Siefert S, Lemke J, Pust B. [Congenital syphilis after reactivation of “healed” maternal primary infection; in German.] Klin Pädiatr 2000; 212: 336–9. Walker GJ. Antibiotics for syphilis diagnosed during pregnancy [review]. Cochrane Database Syst Rev 2001; 3: CD001143. Zelop C, Benacerraf BR. The causes and natural history of fetal ascites. Prenat Diagn 1994; 14: 941–6. Definition: Infection with varicella zoster virus. This is a DNA virus belonging to the family of herpesviruses. The primary infection causes chickenpox; reactivation of the virus at a later stage from the sensory roots of the posterior horn of the spinal cord is responsible for the clinical symptoms of herpes zoster. Incidence: Maternal infection during pregnancy, one in 2000–10 000. The risk of congenital infection to the fetus is low; congenital malformations result in less than 5% of cases. Origin: The virus affects the nervous system, causing neurological impairment of fetal structures. Infections in the first trimester cause the most severe damage. Clinical features: Focal ulceration of the skin and anomalies described in the following section. Ultrasound findings: Rarely, the following are detected: growth restriction, hydramnios, microphthalmia, hydrocephalus, or microcephaly; ascites, pleural effusions and even full-fledged fetal hydrops; hepatic calcification, club feet and other limb anomalies, reduction in fetal movements. These anomalies develop only in the most severely affected cases, about 3–12 weeks after maternal infection. Clinical management: Serology of maternal blood; fetal IgM is detectable from 20 weeks, amniotic fluid culture, chorionic villus sampling and polymerase chain reaction, regular scanning controls (is hydrocephalus developing?). IgG may be given to the mother within 72–96 h if the mother has been in contact with an infected individual and is not immune. Procedure after birth: Acyclovir may be given after birth. Prognosis: The infants usually do not show any symptoms. Fetal anomalies appear in 1–2% of cases if infection occurs before 20 weeks of gestation. About one-third of the most severely affected infants die in the early neonatal stage; in the surviving infants, mental impairment and fits may occur. References Dufour P, de Bièvre P, Vinatier D, et al. Varicella and pregnancy. Eur J Obstet Gynecol Reprod Biol 1996; 66: 119–23. Harger JH, Ernest JM, Thurnau GR, et al. Frequency of congenital varicella syndrome in a prospective cohort of 347 pregnant women. Obstet Gynecol 2002; 100: 260–5. Kerkering KW. Abnormal cry and intracranial calcifications: clues to the diagnosis of fetal varicella-zoster syndrome [review]. J Perinatol 2001; 21: 131–5. Lecuru F, Taurelle R, Bernard JP, et al. Varicella zoster virus infection during pregnancy: the limits of prenatal diagnosis. Eur J Obstet Gynecol Reprod Biol 1994; 56: 67–8. Mets MB. Eye manifestations of intrauterine infections [review]. Ophthalmol Clin North Am 2001; 14: 521–31. Petignat P, Vial Y, Laurini R, Hohlfeld P. Fetal varicellaherpes zoster syndrome in early pregnancy: ultrasonographic and morphological correlation. Prenat Diagn 2001; 21: 121–4. Pons JC, Vial P, Rozenberg F, et al. Prenatal diagnosis of fetal varicella in the second trimester of pregnancy. J Gynecol Obstet Biol Reprod (Paris) 1995; 24: 829–38. Taylor WG, Walkinshaw SA, Thomson MA. Antenatal assessment of neurological impairment. Arch Dis Child 1993; 68: 604–5. Yaron Y, Hassan S, Geva E, Kupferminc MJ, Yavetz H, Evans MI. Evaluation of fetal echogenic bowel in the second trimester. Fetal Diagn Ther 1999; 14: 176–80. Definition: Infection with parvovirus B19, a DNA virus causing erythema infectiosum. The disease is often asymptomatic in both children and adults. Infection of the fetus may lead to fetal anemia and hydrops. Incidence: Some 50–75% of adult women are immune. There is a 10–20% risk of transmission to the fetus through the placenta, and it is most likely to occur in the first and second trimesters. Clinical history: Joint pain and small areas of erythema may be the only clinical symptoms of this infection. Origin: The infection destroys host cells, particularly those that have a high rate of mitosis and divide quickly, such as erythrocyte precursors. Ultrasound findings: Severe cases show hydramnios, placentomegaly, ascites, pleural effusions, cardiomegaly, possibly reduced fetal movements. In addition, there may be hepatosplenomegaly and fetal hydrops. These findings are detected 3–13 weeks after maternal infection. If untreated, fetal demise or neonatal death results. Differential diagnosis:
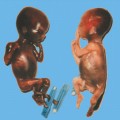
Congenital Syphilis
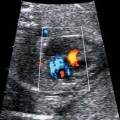
Congenital Varicella
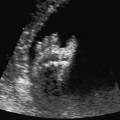
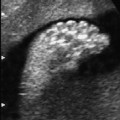
Parvovirus B19
![]()
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree