Chapter Outline
Small Intestine as an Immunologic Organ
Hookworm Infestation (Ancylostomiasis)
Tapeworm (Cestode) Infestation
Trematode (Flukes) Infestation
Inflammatory Disease in Immunodeficiency
Selective Immunoglobulin A and Common Variable Immunodeficiency
Gastrointestinal Infections in AIDS
Human Immunodeficiency Virus Enteritis
Isosporiasis and Other Intracellular Protozoans
Mycobacterium Avium-Intracellulare Complex
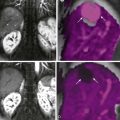
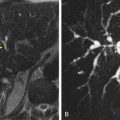
With increasing immigration, tourism, and globalization of the economy, infectious conditions of the small bowel are more likely to be encountered. Some of these patients with acute infectious diseases may undergo imaging studies for symptoms such as diarrhea or right lower quadrant pain ( Figs. 42-1 and 42-2 ). This chapter presents a review of the wide spectrum of inflammatory and infectious disorders involving the small bowel other than Crohn’s disease. Inflammatory disorders that cause malabsorption are discussed in Chapter 43 , and Crohn’s disease is given special treatment in Chapter 41 .


Small Intestine as an Immunologic Organ
The microflora of the upper gastrointestinal (GI) tract originates from swallowed food and from the oral cavity. Small amounts of bacteria and yeasts are present in the esophagus, stomach, and duodenum—about 10 6 bacteria/mL compared with 10 11 to 10 12 bacteria/mL in the distal small bowel and colon.
A variety of mechanisms prevent bacterial colonization of the small intestine. Secretion of water, electrolytes, and mucus by epithelial cells is an important component of host protection. Mucous secretions help prevent adherence of infectious agents to epithelial cells or penetration of toxins into these cells. Intestinal motility and fluid flow also impede bacterial colonization of the small bowel. Diarrhea caused by increased secretion of fluid and electrolytes also facilitates the passage of infectious agents out of the small intestine. Bacterial colonization may occur if there is small bowel stasis because of a motor disorder, diverticulosis, or strictures.
The small intestine is one of the largest immunologic organs in the body because it has an enormous surface area that is constantly exposed to foreign antigens. In healthy individuals, the small intestine is in a chronic state of low-grade inflammation and immune activity. In most people, foreign antigens are eliminated without producing clinical symptoms. The small intestine can exclude foreign antigens without inducing autoimmune intestinal disease caused by cross-reactivity of foreign and host antigens.
The immune system includes intraepithelial lymphocytes, lymphoid tissue in Peyer’s patches in the lamina propria, neutrophils, macrophages, and mast cells. Peyer’s patches are unencapsulated lymphoid clusters spanning the lamina propria. A specialized epithelium overlies the Peyer’s patches; M cells in this specialized epithelium transport antigens to the underlying lymphoid tissue.
B cells in the lamina propria synthesize immunoglobulin A (IgA) and, to a lesser degree, IgM, IgG, and IgE. Intraluminal secretion of IgA inhibits bacterial adherence to the epithelium, preventing bacterial colonization. IgA also neutralizes bacterial toxins, minimizing any deleterious effects on epithelial cell function. IgA also blocks absorption of intraluminal antigens. IgA helps neutralize intracellular pathogens but does not cause their destruction.
Intraepithelial lymphocytes are primarily T cells. These cells lie in the basal epithelium, secrete cytokines, and are involved with antigen recognition and tolerance to oral antigens. They also perform immunosurveillance against abnormal epithelial cells. T cells are markedly increased in number in graft-versus-host disease, celiac disease, and protozoan infections.
Polymorphonuclear neutrophils differentiate in the bone marrow, leave the peripheral circulation, enter the lamina propria, and traverse the epithelium to enter the intestinal lumen. Neutrophils recognize and phagocytize antibody-coated bacteria. Macrophages in the lamina propria are derived from monocytes produced in the bone marrow. They also pass through the epithelium into the lumen and are important in bacterial phagocytosis and killing. Mast cells are found in all layers of the bowel wall. They contain granules with preformed mediators of inflammation such as histamine and 5-hydroxytryptamine and are important in the defense against intestinal parasites and food antigens.
Parasitic Infestations
Worms and protozoa infect more than 25% of the world’s population. Helminths (worms) are divided into roundworms (nematodes), tapeworms (cestodes), and flukes (trematodes). Nematodes are round and unsegmented. They have a body cavity and are divided into separate sexes. Cestodes are tapelike and segmented and are hermaphrodites. Trematodes are leaf-shaped and unsegmented and are also hermaphrodites.
Ascariasis
Ascaris lumbricoides is the most common intestinal worm, infecting about 25% of the world’s population, most frequently people living in the tropics and subtropics. Ascariasis is acquired by ingesting mature eggs from contaminated soil, food, or water. Two to 3 weeks after ingestion of eggs, larvae develop in the small intestine. The larvae penetrate the mucosa, enter vessels in the bowel wall to reach the portal venous system, and migrate through the liver and heart to the lungs. The larvae then penetrate the alveoli, enter the tracheobronchial tree, and are swallowed. Development is completed in the small intestine, where the worms attach to the mucosal surface of the midjejunum. Worms may grow up to 40 cm in length.
Symptoms include abdominal pain and malabsorption. If the worms are present in large numbers, ascariasis can cause small bowel obstruction resulting from luminal obturation or intussusception. Mature worms that migrate into the bile or pancreatic ducts may cause cholangitis or pancreatitis.
Ascaris can be identified on plain abdominal radiographs, barium studies, and computed tomography (CT) scans. Long, smooth, convoluted tubular filling defects are seen in the intestinal lumen on barium studies ( Fig. 42-3 ) or CT. If barium enters the worm’s intestinal tract, a long, thin line of barium will be present within the tubular radiolucent filling defect caused by the worm (see Fig. 42-3 ). Small bowel folds are usually of normal size but may be enlarged. Small nodules reflect submucosal cysts surrounded by fibrotic tissue. The radiographic diagnosis can be confirmed by detection of ova in stool specimens.

Hookworm Infestation (Ancylostomiasis)
Hookworms are small (8-10 mm) nematodes that infect almost 1 billion people worldwide. The incidence of hookworm disease has decreased markedly in the southern United States with improved sanitation. Ancylostoma duodenale is found in southern Europe, the Mediterranean region, and the western coast of South America. Necator americanus causes hookworm infestation in the southern United States, the Caribbean, and South America. Both species are found in India and southeast Asia. Near adult stage larvae and adult worms attach to the small intestinal mucosa. Ova are secreted into the feces. Infection results primarily from filarial invasion of the feet (in people who walk barefoot) or hands.
Although hookworm infestation can cause abdominal pain, diarrhea, or acute GI bleeding, iron-deficiency anemia is the most common clinical presentation. Peripheral eosinophilia is present in most patients.
The jejunal mucosa is edematous and hemorrhagic at sites of intestinal attachment. Hookworms have not been demonstrated on barium studies. Jejunal fold thickening and irritability may be present. Ileal strictures have also been reported. Regional lymphadenopathy may be present. A definitive diagnosis requires the GI demonstration of ova in stool specimens or worms in jejunal aspirates or biopsy specimens.
Strongyloidiasis
Strongyloides stercoralis is a nematode usually found in the tropics and subtropics and in areas of poor sanitation or areas in which human waste is used as fertilizer. In the United States, strongyloidiasis is found in people living in Appalachia, military personnel returning from endemic regions, and patients who are immunocompromised because of malnutrition, steroid use, AIDS, or other causes.
Filariform larvae about 0.5 mm long penetrate the skin, migrate through the venous system to the lungs, penetrate the alveoli, enter the tracheobronchial tree, and are swallowed. The larvae are transformed into adult worms in the small intestine. The females penetrate the mucosa of the duodenum and proximal jejunum and live in the superficial layers of the proximal small bowel. Male worms are expelled. Female worms are about 2 mm in length.
Strongyloidiasis differs from other nematode diseases because autoinfection may occur; these infections may be life-threatening in an immunocompromised host. Eggs released into the intestinal lumen form rhabditiform larvae that develop into infective filariform larvae in the intestinal lumen or in the soil. The filariform larvae may reinvade intestinal mucosa or perianal skin. Most larvae die in lymphatics in the wall of the small bowel or in the mesentery.
Strongyloidiasis may cause a wide variety of clinical symptoms. These include abdominal pain, diarrhea, weight loss, and malabsorption.
Mild infestation by strongyloidiasis cannot be detected on imaging studies. With chronic infection, thickened folds are seen in the duodenum and jejunum on barium studies. With severe infection, the small bowel folds are effaced or obliterated, and the jejunum can assume a narrowed, tubular configuration ( Fig. 42-4 ). Strongyloidiasis is also a cause of papillary stenosis and small intestinal dilation. A definitive diagnosis can be made by duodenal aspiration or biopsy.

Anisakiasis
Members of the Anisakidae family are nematode parasites of marine mammals. Anisakis larvae are found in intermediate hosts such as squid and fish (e.g., salmon, cod, anchovy, tuna, mackerel, Pacific pollock, Pacific red snapper, herring). Human infection is acquired by eating raw, inadequately cooked, or pickled fish. Anisakiasis is most common in areas in which raw fish such as sushi or sashimi is frequently eaten. Ingested larvae usually attach and invade the stomach, but small or large bowel involvement may occur. Edema and inflammation develop at the site of attempted larval penetration. Ulceration and perforation with the formation of inflammatory masses have been reported. Symptoms of small bowel involvement can mimic those of acute appendicitis, Crohn’s disease, or small bowel obstruction.
Anisakis larvae have been detected on double-contrast studies of the stomach and colon as thin, curved, 5-mm filling defects in the shallow barium pool. Focal, irregular fold thickening may be seen in the small bowel. Strictures and short, ulcerated lesions have also been described. Perforation with mesenteric abscess formation may lead to a mesenteric mass or abscess detected on cross-sectional imaging studies.
Tapeworm (Cestode) Infestation
Cestodes live as adults in the GI tract of definitive hosts and as cysticerci in the tissue of intermediate hosts. Humans are the definitive hosts for Taenia saginata (beef tapeworm), Taenia solium (pork tapeworm), Hymenolepis nana (dwarf tapeworm), and Diphyllobothrium latum (fish tapeworm). Humans are intermediate hosts for Echinococcus granulosus, Echinococcus multilocularis, and Taenia solium. These worms attach to the intestinal mucosa by a scolex. A connecting region is followed by the strobila and a ribbon-like chain of developing segments (the proglottids). The number of proglottids varies from 3 to 4000, and the length of the cestode varies from several millimeters to several meters.
Humans are infected by eating inadequately cooked beef, pork, or fish (e.g., pike, salmon, trout, whitefish, turbot). After infected flesh is ingested, the cysticercus breaks down, releasing a scolex that attaches in the upper jejunum. The adult worm develops, and proglottids and ova are released into the lumen. Tapeworm infection usually causes no symptoms. Because of its long length (up to 4-6 m), T. saginata may cause obstructive symptoms. In contrast, D. latum may cause vitamin B 12 deficiency and macrocytic anemia.
Trematode (Flukes) Infestation
A variety of flukes may involve the liver, biliary tract, and intestines. The genus Schistosoma infects more than 150 million people worldwide. S. mansoni is endemic in Africa, the Middle East, and Latin America, S. japonicum is endemic primarily in Asia, and S. haematobium is endemic in the Middle East and Africa . S. haematobium mainly causes genitourinary disease but is occasionally found in the appendix. Because colonic infection by schistosomiasis is more common than small bowel infection, this disease is discussed in Chapter 58 .
Giardiasis
Giardiasis is the most common parasitic disease worldwide. In the United States, giardiasis is usually found in the Rocky Mountain states. Surface water contaminated by feces from wild animals is the principal source of infection. Cysts remain viable in cold water for 1 to 3 months and can also survive the chlorine levels of many municipal water systems. Giardiasis is transmitted primarily by fecal-oral transmission from contaminated food and pets and occasionally by oral-anal contact. The risk of infection is greater in patients with immunodeficiency states and hypochlorhydria.
After cyst ingestion, trophozoites emerge in the duodenum and proximal jejunum. The trophozoites remain in the intestinal lumen or penetrate the mucus gel layer of the proximal intestine to attach to the glycocalyx of the enterocytes. The trophozoites do not invade the epithelium. Mature cysts are excreted in the stool.
The infection varies from the asymptomatic carrier state to self-limited diarrhea or chronic, watery diarrhea. Because the infection is patchy, biopsy specimens may be normal in infected patients. Some patients may have villous atrophy with crypt hyperplasia and variable inflammation, and others may have lymphoid hyperplasia.
The small intestine frequently appears normal on small bowel follow-through studies. In about 50% of patients, there is increased intraluminal fluid and rapid small bowel transit. Some reports have described thickened folds and irritability in the duodenum and jejunum ( Fig. 42-5 ). Because barium studies are abnormal in fewer than 50% of infected patients and radiographic findings are nonspecific, the diagnosis depends on the detection of cysts and trophozoites on stool examinations, detection of trophozoites on duodenal biopsies or aspirates, or positive fluorescent antibody test.

Trypanosomiasis
Chagas’ disease is caused by the protozoan Trypanosoma cruzi, spread by the bite of the reduviid bug. Chagas’ disease is endemic in central Brazil, northern Argentina, and Venezuela but has also been reported in southern areas of the United States. It is estimated that 350,000 people in the United States are seropositive for this infection. T. cruzi produces a neurotoxin that attacks autonomic ganglion cells throughout the body, including those in the heart, GI tract, urinary tract, and respiratory tract. The esophagus, duodenum, and colon are the GI organs most commonly affected, resulting in secondary achalasia, megaduodenum, and megacolon. Involvement of the mesenteric small bowel leads to dilation of the small bowel, with delayed transit.
Bacterial Infections
Traveler’s diarrhea and foodborne diseases are common problems related to tainted water supplies and improperly prepared or stored food. Bacteria are the organisms usually responsible for traveler’s diarrhea, which explains why prophylactic use of antibiotics decreases the incidence of traveler’s diarrhea. Chemicals, viruses, and parasites are less frequent causes of traveler’s diarrhea. Enterotoxigenic Escherichia coli is the most common cause of traveler’s diarrhea. Enteroadherent and enteropathogenic E. coli are less frequent causes. Shigella and Campylobacter jejuni are the next most common pathogens, but these bacteria usually involve the colon. This infection is rarely diagnosed on imaging studies, because acute watery diarrhea develops during or shortly after a period of travel.
Tuberculosis
Tuberculosis is endemic in Asia. Intestinal tuberculosis is uncommon in the West, usually occurring in the homeless, alcoholics, inmates, farm workers, immigrants, or people infected with human immunodeficiency virus (HIV). With the rise of AIDS and immigration, intestinal tuberculosis has become more common in developed countries. In one hospital in London with an extensive population of Asian immigrants, new diagnoses of tuberculosis were almost as common as new diagnoses of Crohn’s disease. The proposed mechanisms of infection of the GI tract include the ingestion of infected sputum or milk and hematogenous spread to submucosal lymphatics. Intestinal tuberculosis frequently occurs without radiographic evidence of pulmonary disease.
Intestinal tuberculosis primarily occurs in the ileocecal region. The distribution of tuberculosis parallels the distribution of the lymphatics. In one autopsy series of over 1000 cases, 90% of patients had ileal disease and 75% had cecal disease. Other sites were not infrequently involved, however, including the ascending colon in 51%, transverse colon in 33%, descending colon in 23%, and appendix in 33%. Skip lesions may be present.
The three classic forms of GI tuberculosis are the ulcerative, hypertrophic, and ulcerohypertrophic forms. Sloughing of mucosa overlying submucosal tubercles results in ulceration. These ulcers usually appear as short (3-6 mm in length) collections perpendicular to the longitudinal axis of the bowel. The ulcers may be stellate or longitudinal. Extensive inflammation and fibrosis of the bowel wall result in the hypertrophic form of tuberculosis associated with extensive mesenteric lymphadenopathy and adhesions. Bacilli are found primarily in necrotic mesenteric lymph nodes rather than the intestinal wall. Endoscopic biopsy specimens and tissue cultures are frequently negative. In one study, acid-fast bacilli and caseating necrosis were found in only 32% and 50% of patients with GI tuberculosis, respectively. In some cases, laparoscopic diagnosis with cultures and histologic examination of ascitic fluid may be helpful. Not infrequently, however, the diagnosis of tuberculosis is made only by pathologic examination of resected surgical specimens.
Complications of small bowel tuberculosis include strictures and obstruction, fistulas, enteroliths, and chronic appendicitis.
Barium studies may reveal perpendicular, stellate, or longitudinal ulcers of varying size with heaped-up margins in the colon or ileum (usually the terminal ileum). Short or long strictures may be associated with nodular mucosa. A narrow, contracted cecum associated with a gaping ileocecal valve and disproportionate inflammation of the ascending colon are findings that help distinguish ileocecal tuberculosis from Crohn’s disease ( Fig. 42-6 ). However, longitudinal ulceration, sinus tracts, and fistulas in the terminal ileum may be indistinguishable from those in Crohn’s disease on barium studies.

CT often reveals thickening of the ileocecal valve. The medial wall of the cecum is disproportionately thickened and is often associated with a soft tissue mass that engulfs the terminal ileum. Wall thickening may be uniform or heterogeneous. Lymphadenopathy predominates in the pericecal region but may extend into the mesentery.
Historically, radiologic differentiation of tuberculosis from Crohn’s disease was facilitated by predominance of the tuberculous inflammatory process in the cecum and ascending colon, with a patulous ileocecal valve lumen and thickened ileocecal valve lips in patients with tuberculosis. Barium studies showing disease predominantly in the cecum and ascending colon with cecal contraction and CT showing low-attenuation lymph nodes indicative of caseous necrosis should suggest tuberculosis rather than Crohn’s disease as the diagnosis in these patients. However, tuberculosis and Crohn’s disease may have a similar lymphatic distribution and overlapping radiographic findings. The clinical history and patient demographics should therefore be considered before suggesting the diagnosis of Crohn’s disease.
Yersiniosis
Yersinia are gram-negative cocci acquired after the ingestion of contaminated food or water. Yersinia enterocolitica is more frequently encountered than Yersinia pseudotuberculosis in the United States. Yersinia invades epithelial cells, enters Peyer’s patches in the lamina propria and submucosa, and spreads to mesenteric lymph nodes. Ileitis, colitis, mesenteric adenitis, periappendicitis, and hemolytic uremic syndrome have been reported. Bacterial multiplication in Peyer’s patches and regional lymph nodes can result in distant infections, including chronic hepatitis, ankylosing spondylitis, and lung and kidney infections.
Yersinia infection leads to the development of aphthoid ulcers overlying hyperplastic lymph follicles in the bowel. Hyperplasia of follicular and interfollicular regions results in massive lymphadenopathy. Acute vasculitis may cause ischemia.
The radiographic appearance in Yersinia enterocolitis depends on the course of infection. Early in the disease, aphthoid ulcers and thickened folds may be the predominant findings in the terminal ileum. Later in the disease, the ulcers disappear but thickened undulating folds persist ( Fig. 42-7 ). The inflammatory process is distinguished from Crohn’s disease by the absence of luminal narrowing, fissures, or fistulas. The inflammatory process usually resolves in 4 to 6 weeks.

Salmonellosis
Salmonella infections in the GI tract may have distinct clinical forms, including gastroenteritis, typhoid fever, and an asymptomatic carrier state. Foodborne outbreaks resulting in diarrhea are usually caused by Salmonella enteritidis and Salmonella typhimurium, found in a wide variety of sources, including eggs, poultry, and livestock. Diarrheal outbreaks caused by fecal-oral spread from human reservoirs are less common. Salmonella enter and multiply in M cells and enterocytes and then disseminate to lymphoid tissue and macrophages in the submucosa and mesenteric lymph nodes. The diarrheal form of salmonellosis varies from a few loose stools to a severe, watery, diarrheal state. The diarrhea usually lasts from 3 to 7 days. Bacteremia is uncommon, occurring in 6% to 8% of patients.
Typhoid fever is usually caused by Salmonella typhi and Salmonella paratyphi . Humans are the reservoir for S. typhi. The organism is transmitted by the fecal-oral route, so this disease is usually found in regions with contaminated water and poor waste treatment. In most patients, a brief episode of diarrhea precedes the febrile illness. A systemic, acute febrile illness then lasts for 3 to 5 weeks, accompanied by nonspecific symptoms such as headaches, malaise, abdominal discomfort, and arthralgia. Complications of Salmonella include GI bleeding and perforation related to a lymphoid reaction in the ileocecal region. Bacteremia can lead to other infections, including meningitis, pericarditis, orchitis, and splenic or liver abscesses. Hepatosplenomegaly may be present. Perforation or peritonitis may cause an adynamic ileus.
Salmonella may be manifested on barium studies by longitudinally oriented ulcers in the distal ileum overlying Peyer’s patches. Prominent lymphoid hyperplasia may be present, and vascular thrombosis may be seen. The disease is sometimes detected on CT performed to evaluate hepatosplenomegaly, right lower quadrant pain, and fever. CT may reveal circumferential thickening of the terminal ileum. Barium studies may demonstrate nonspecific fold thickening in the terminal ileum.
Campylobacteriosis
Campylobacter comprises a group of gram-negative rods, including Campylobacter jejuni, Campylobacter fetus, and Campylobacter coli. These organisms may cause an acute enteritis or colitis, or affected individuals may remain in an asymptomatic carrier state. Colonic infections may be severe, resulting in fulminant colitis with GI bleeding or toxic megacolon. Systemic manifestations (e.g., arthritis, endocarditis, genital infections, urinary infections) may occur. Cross-reactivity of C. jejuni and neural antigens may result in Guillain-Barré syndrome.
When the small intestine is involved, multiple superficial ulcers may develop in the distal ileum and region of the ileocecal valve. Barium studies may reveal thickened folds and aphthoid ulcers in the distal ileum and terminal ileum. The radiographic findings are indistinguishable from those of yersiniosis or early Crohn’s disease.
Fungal Infections
Histoplasmosis
Histoplasma capsulatum is a dimorphic fungus commonly found in the Mississippi and Ohio River valleys. This fungus occurs in a mycelial form at ambient temperature and in a yeast form at body temperature. The fungus usually infects older patients or immunocompromised hosts. Small bowel infection is common in patients with disseminated disease, but clinical symptoms are usually minimal. Ileocecal disease is characterized by ulceration, mucosal nodularity, strictures, and lymphadenopathy. Intestinal perforation and peritonitis may also be seen.
Viral Infections
Numerous viruses may infect the small intestine, resulting in an acute diarrheal state. Radiologic studies are rarely performed in this clinical setting. The diagnosis can be made by viral cultures or by enzyme-linked immunosorbent assay (ELISA) or electron microscopy of stool specimens. Cytomegalovirus involving the small bowel is described later (see “ Cytomegalovirus Infection ”).
Drug-Induced Disorders
Drugs may cause a variety of abnormalities in the small intestine. Ischemia can result from systemic hypotension and hypovolemia, mesenteric arterial vasoconstriction, and slow mesenteric flow with venous thrombosis ( Box 42-1 ). Ischemia is discussed in Chapter 47 . Anticoagulants may cause GI bleeding. Small bowel hypomotility can be caused by narcotics, drugs with anticholinergic properties, or neurotoxic side effects ( Box 42-2 ). Drugs may cause malabsorption by a number of mechanisms, including interference with fat digestion and absorption; decreased gastric, pancreatic, and biliary secretions; increased intestinal transit; and small bowel mucosal injury ( Box 42-3 ). Alcohol may also cause malabsorption by damage to intestinal crypts and villi. Metals such as aluminum, lead, gold, cadmium, mercury, zirconium, and iron may also damage small bowel epithelium.