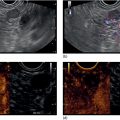
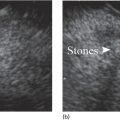
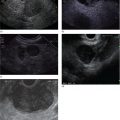
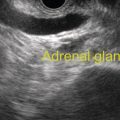
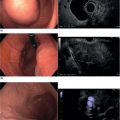
Indraneel Chakrabarty and Ann Marie Joyce Tufts University School of Medicine and Lahey Clinic Medical Center, Burlington, MA, USA The most common liver pathology seen using endoscopic ultrasonography (EUS) includes cirrhosis, fatty liver, hepatic cysts, and neoplasms. Dilated intrahepatic, extrahepatic, and common bile ducts with or without stones are often seen as well. Endoscopic ultrasonography of the liver can be frustrating as it is often difficult to determine if the liver was viewed in its entirety depending on the patient’s body habitus and anatomy. For optimal imaging, the echoendoscope should be set to the lowest possible frequency for maximal hepatic penetration. There are three primary positions for viewing the liver. The duodenal bulb is the best position to evaluate the right lobe of the liver. The balloon over‐inflation technique can be used to help lock the scope into the duodenal bulb. From here the scope should be advanced and withdrawn and torqued clockwise and counterclockwise accordingly for maximal views of the right lobe. This should be repeated until the ultrasonographer feels that he or she has viewed the liver to the best of their ability given the patient’s size and anatomy. After completion of this exam, the balloon should be deflated and the scope positioned in the antrum. This will give views of both the right and left hepatic lobes. The same technique of torque and advancing the scope forward and backwards should be applied until all views of the liver have been exhausted. The last position is the gastric fundus, which gives optimal views of the left hepatic lobe. It is usually initiated from the gastroesophageal junction using the same techniques as in the latter position until all views are achieved to the ultrasonographer’s satisfaction. The endosonographic description of liver pathology is reviewed in this chapter. The two leading causes of cirrhosis in the United States is alcohol abuse followed by hepatitis C. Combined they are the twelfth leading cause of death in the United States as of 2000, accounting for over 25 000 deaths. In addition, approximately 75–85% of acutely infected hepatitis C individuals progress to chronic infection, with up to 20% developing cirrhosis over 20–25 years. Other etiologies include hepatitis B, non‐alcoholic steatohepatitis, primary biliary cirrhosis, primary sclerosing cholangitis, autoimmune hepatitis, hereditary hemochromatosis, Wilson’s disease, and α1‐antitrypsin deficiency. All patients with cirrhosis are at increased risk of developing hepatocellular carcinoma. In general, cirrhosis is characterized by the replacement of normal hepatic tissue with permanent scar tissue, which leads to disruption of organ function and blocks portal blood flow through hepatic parenchyma leading to the various clinical features of cirrhosis. This scar tissue can often be visualized under EUS as nodular tissue characterized by coarse, diffuse, heterogeneous, echoic parenchyma (Figure 28.1a). The outer wall of the liver often loses its smooth border and can appear irregular or nodular (Figure 28.1b). One of the complications related to cirrhosis is ascites. Ascites can be seen as anechoic areas adjacent to intra‐abdominal organs (Figure 28.1c). A sample of the fluid can be obtained through a fine needle aspiration (FNA).
28
Liver Pathology
Introduction
Cirrhosis
Fatty liver disease
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree