Meniscus surgery is common, and surgical indications and techniques continue to evolve. After highlighting relevant anatomy and emerging magnetic resonance (MR) imaging techniques, this article reviews the current indications and techniques used for meniscus surgery, evaluates the use of MR imaging protocols with and without arthrography, and focuses on MR imaging interpretation of the postoperative meniscus, with particular attention to clinical outcomes and diagnostic criteria.
Key points
- •
To correctly interpret magnetic resonance (MR) imaging findings in the postoperative meniscus, physicians must understand the surgical techniques applied to the meniscus: the “3 Rs,” namely resection, repair, and replacement, each resulting in a different MR imaging appearance of the postoperative meniscus.
- •
Resection (most often partial meniscectomy) is by far the most common procedure, but there is an increasing body of literature questioning its clinical efficacy. Consequently, meniscus preservation is increasingly emphasized, and repair techniques may become more common in the coming years.
- •
Repair techniques generally are subdivided into 3 types: inside-out, outside-in, and all-inside. After surgical repair, the meniscus can be categorized as healed (ie, no fluid signal in the repair), partially healed (ie, fluid signal extending into <50% of the repair site), or not healed (ie, fluid signal extending into >50% of the repair site).
- •
Meniscus replacement can be performed for postmeniscectomy syndrome in appropriate young to middle-aged patients. In the United States, this usually takes the form of a cadaveric meniscus allograft. In Europe and elsewhere, there is increasing experience with synthetic meniscus implants.
Introduction
Meniscus surgery is one of the most commonly performed orthopedic procedures, with an estimated 1 million meniscus surgeries and US$4 billion in direct medical expenditures each year.
Magnetic resonance (MR) imaging of the knee commonly is indicated to investigate the cause of unresolved or recurrent pain that can occur in patients after meniscus surgery.
The objectives of this article are to review selected highlights of (1) basic science (normal anatomy and emerging MR imaging techniques), (2) meniscus surgery (indications and techniques), (3) MR imaging protocols (with vs without arthrography), and (4) postoperative MR imaging interpretation (clinical outcomes and diagnostic criteria).
Basic science: implications for knee MR imaging
Like articular (hyaline) cartilage, the fibrocartilaginous meniscus plays several roles, including load bearing, load distribution, joint stability, and joint lubrication. Compared with articular cartilage, the meniscus has a higher collagen content (15%–25% vs 10%–20%), lower proteoglycan content (1%–2% vs 5%–10%), and lower water content (60%–70% vs 68%–85%).
Although the most important principles of meniscus anatomy are covered elsewhere in this issue by Rosas and colleagues, a few basic science concepts regarding the meniscus deserve to be highlighted here to emphasize our evolving understanding of this surprisingly heterogeneous tissue. Indeed, the meniscus structure varies both radially (peripheral to central) and also with depth (superficial to deep). Current research is providing insights into the various constituents within the meniscus, including cells, collagen, vascularity, and innervation.
Meniscus Cells: Do Meniscus Cells Die?
Meniscus cell degeneration and death (apoptosis) is significantly associated with meniscus tears and prognosis for successful meniscus repair.
Meniscus cell (fibrochondrocyte) subpopulations show marked regional variation, with concomitant zonal variation in the surrounding matrix (pericellular and extracellular) that they produce. Indeed, rather than being a homogeneous tissue, recent work indicates that this wedge-shaped tissue varies consistently from the thin, cartilage-like free edge, where compressive forces predominate and proteoglycan content is high, to the thicker, more peripheral region, where circumferential tensile loads predominate and proteoglycan content is low.
In addition to zonal variation in the proteoglycan matrix produced by the cells, there is also a zonal variation in the density of meniscus cells and their phenotypes (chondrocytic inner zone versus fibroblastic outer zone).
MR imaging with T1rho mapping and delayed gadolinium enhancement, known to be sensitive to changes in proteoglycan loss in cartilage, recently has been used to show differences between normal and degenerated menisci.
Given that the anatomy and mechanisms that drive meniscus degeneration may be zonally dependent, future treatments such as gene therapy may use a targeted therapeutic approach for inner versus outer zones of the meniscus.
Collagen: Can MR Imaging Evaluate Collagen?
Collagen fibers are primarily responsible for tensile strength. In the classic description, collagen fibers are arranged for transferring vertical (compressive) loads into circumferential hoop stresses. In particular, the hoop stresses are contained via a belt of peripheral circumferential fibers, and these circumferentially oriented fascicles are secured together by radially oriented tie fibers. With aging, there tends to be an increase in connective tissue stiffness related to processes such as elastin degradation and collagen rigidification.
Although the collagen architecture is often presented in a stylized fashion in diagrams, recent work indicates that the highly ordered microstructure is even more complex, and exquisite, than appreciated previously ( Fig. 1 ).

For example, there are 2 major types of collagen fascicle organization: braided and woven.
- •
The braided fascicle organization is analogous to that seen in rope. With stretching in an axial orientation, the braided fascicles compress against adjacent fascicles, thus increasing stiffness.
- •
The woven arrangement is analogous to the pattern seen in fabrics or other flat structures that can convert compressive loads into tensile forces in the weave, sharing loads with adjacent supporting structures such as the ligamentous attachments to the tibial plateau. This arrangement may be relevant to normal meniscus movement and abnormal extrusion observed with conventional and dynamic MR imaging techniques.
MR imaging T2 mapping has been used to detect changes in collagen structure and water content, which are associated with degeneration. After meniscus repair, preliminary results suggest that quantitative T2* values correlate with collagen structural integrity, and are sensitive to temporal and zonal differences of meniscus repair.
Recent study of the architectural subdivisions within the meniscus conclusively demonstrates the 3-dimensional nature of sheets of collagen tie fibers surrounding blood vessels. These sheets are oriented along the transverse plane of the meniscus, which may explain a propensity for horizontal-cleavage plane tears commonly seen with MR imaging and arthroscopy ( Fig. 2 ).

Vascularity: If the Inner Meniscus Is Avascular, How Does It Receive Nourishment?
The geniculate arteries, which are branches of the popliteal artery, supply the meniscus. Although the meniscus is diffusely vascularized during early life, by approximately 10 years of age only the outer 10% to 30% of the meniscus remains vascularized. Indeed, in adults, the inner portion of the meniscus is not only avascular, it is aneural and alymphatic! The inner portion of the meniscus receives nourishment from diffusion or mechanical pumping of synovial fluid, likely via canal-like structures opening deep into the surface of the menisci.
Vascularization of the meniscus is directly related to its healing potential. Well-vascularized, peripheral (red zone) tears have a propensity for healing, whereas tears at the avascular, inner aspect (white zone) of the meniscus are not expected to heal spontaneously. Tears at the transition between the red and white zones are said to be in the red-white zone.
In a recent study of 86 peripheral vertical tears, almost all (>94%) tears of the medial meniscus at the posterior meniscocapsular junction healed spontaneously, whereas most (∼80%) other peripheral vertical tears did not heal. For the peripheral vertical tears not located at the meniscocapsular junction, however, several MR imaging findings were significantly associated with spontaneous healing: thin tear (width <2 mm), tear visualized on only proton-density (PD)-weighted (but not T2-weighted) imaging, and thin horizontally oriented strands bridging the tear on T2-weighted images. Conversely, a wide gap between torn edges that is filled with fluid signal intensity on T2-weighted images did not heal with nonoperative therapy.
MR imaging performed with intravenous injection of contrast material is not helpful for differentiation of vascularized from nonvascularized zones of the meniscus.
Innervation: If Most of the Meniscus Is Aneural, Do Meniscus Tears Cause Pain?
The primary goals of any meniscus surgery are to help alleviate pain and optimize function. Both pain and function are influenced by meniscus innervation.
The meniscus is well innervated only in vascularized areas. Thus, when a tear occurs in the vascularized, innervated area at the meniscus periphery, some pain may result from direct nerve insult and bleeding.
When tears occur at the inner noninnervated meniscus, pain presumably occurs via other mechanisms, such as secondary stimulation of nociceptive fibers in the adjacent subchondral bone, synovium, or joint capsule as sequelae of osteoarticular pathomechanics, in addition to meniscus neovascularity, sensory nerve growth, and perimeniscal synovitis (defined as enhancing synovium >2 mm in thickness on MR imaging), and premature osteoarthritis.
- •
Symptomatic tears. MR imaging findings significantly associated with knee symptoms include meniscus tears that are vertical or complex, and tears associated with bone marrow edema and joint-capsule thickening. Specific tear types may be associated with particular symptoms at higher frequencies. Examples cited in the literature include: flap tears associated with pain on standing and a catching sensation; posterior root tears associated with popliteal pain; and radial tears in the middle segment associated with nocturnal pain on rolling over in bed.
- •
Asymptomatic tears. Meniscus tears with a horizontal or oblique configuration on MR imaging are not significantly associated with knee symptoms.
In addition to nociceptors (causing pain), the meniscus also contains several types of mechanoreceptors (converting physical stimuli into electrical nerve impulses) that may be involved in sensorimotor control of the knee.
In the normal medial meniscus, mechanoreceptors may be crucial in a reflex arc that stimulates the semimembranosus to contract, including the segment that pulls the medial meniscus posterior horn posteriorly, thus preventing the meniscus from being trapped and injured with knee flexion. By contrast, derangements and some surgeries involving the meniscus posterior horn may contribute to the inhibition of semimembranosus muscle activation and alter meniscus mobility, thus changing the internal joint forces. In a subset of patients, symptoms of giving way or buckling of the knee may be due to an alteration in stretch-reflex excitability rather than ligamentous laxity.
Meniscus surgery: indications and techniques
Nothing has changed so much in knee treatment and surgery as the meniscal treatment algorithms…
Meniscus tears may be managed nonoperatively or operatively, depending on the type of tear and the clinical context ( Box 1 ). Besides clinical history, other factors dynamically influence treatment algorithms, including recent sensational advancements in clinical outcomes research, treatment techniques, and musculoskeletal imaging.
In a patient with a meniscus tear, relevant clinical history includes:
- •
Age and functional demands
- •
History of prior meniscus surgery and trauma
- •
Features of acute injury/trauma
- •
Significant mechanical symptoms (eg, locking)
- •
Concomitant injuries (eg, anterior cruciate ligament tear)
- •
Malalignment
- •
Articular cartilage status
Important specific examples of clinical research expected to affect management choices include:
- •
The recent trials finding lackluster clinical outcomes after meniscectomy for nontraumatic tears, with or without osteoarthritis
- •
The recent literature on acceptable healing rates for augmented repairs of tears in the red-white zone
- •
The evolving recommendations that some stable tears be left in situ (sometimes with healing on follow-up MR imaging and second-look arthroscopy)
To interpret MR imaging findings in the postoperative meniscus correctly, one must understand the surgical techniques applied to the meniscus. Although treatment algorithms are debated and continue to evolve, there are 3 general surgical strategies (known as the 3 Rs), resection, repair, and replacement (or reconstruction). Each of the 3 techniques results in a different MR imaging appearance for the postoperative meniscus. Repairs and partial replacements are often performed with augmentation techniques to enhance healing, which might promote meniscus regeneration (or rejuvenation), a fourth “R.”
Resection
Indications
The general indication for partial meniscectomy is a meniscus tear not amenable to repair. Irreparable tears conventionally include nonperipheral tears with a horizontal, oblique flap (vertical flap, parrot beak) or a complex configuration, especially nontraumatic tears in middle-aged or older patients ( Fig. 3 ).


Technique
The damaged, loose meniscus tissue is removed using arthroscopic instruments until solid tissue is reached; these instruments include manually operated scissors and baskets and mechanical shavers that use suction to draw tissue into a rotating window, which then severs its connection. The remaining meniscus is tapered and contoured, preserving as much meniscus tissue as possible. Debridement of a meniscus tear most often results in partial meniscectomy. Rarely is a complete meniscectomy performed. Unless otherwise specified, the authors use the term “meniscectomy” here to refer to partial resection of the meniscus, because total meniscectomy is so rare in practice.
Repair
Indications
Indications for meniscus repair traditionally have included posttraumatic vertical (longitudinal) peripheral tears located at or near the joint capsule, ideally in younger patients (<40 years).
Compared with meniscectomy, repair procedures are more technically demanding for the surgeon, cost more (in terms of time and equipment), and traditionally have required longer rehabilitation to allow for successful healing of the repair.
Techniques
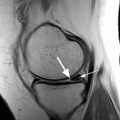
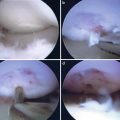
Repair techniques generally are subdivided into 3 types: inside-out, outside-in, and all-inside. Meniscal repair is analogous to operative repair of a fracture nonunion; the surgeon commonly assesses vascularity of the tear, debrides/rasps the edges, aligns the edges, and applies stable fixation with sutures or bioabsorbable implants at approximately 5-mm intervals, sometimes with biological adjuncts in an attempt to improve healing ( Fig. 4 ).


Inside-out
The inside-out technique with vertical mattress sutures is the gold standard with which other repair techniques are compared. Although to date it has been the most common technique, comparable results are reported with other techniques that are less technically demanding.
For example, in a review of 767 meniscus repairs involving the red-white zone, clinical healing was reported in 81% (of 470) inside-out repairs and 86% (of 297) all-inside repairs.
The inside-out technique deploys sutures from inside the joint across the meniscus tear and through the capsule to the exterior surface, using a cannulated needle under arthroscopic visualization. To visualize passage of the needles and avoid injury to neurovascular structures adjacent to the knee joint, a 2- to 3-cm length incision with dissection to expose the external joint capsule is necessary.
Outside-in
The outside-in technique has evolved since its original description in 1985, with healing rates and functional scores comparable with those of other meniscus repair techniques.
The outside-in technique is most applicable to tears in the anterior and adjacent middle segments of the meniscus. With a recent modification, this technique also can be recommended as an alternative method for repair of the middle segment and the posteromedial or posterolateral corner of the meniscus.
All-inside
The all-inside technique has progressed dramatically and has become increasingly popular since its first description in 1991.
An all-inside repair technique is suitable for most reparable meniscus tears, especially vertical (longitudinal) posterior horn tears. The all-inside technique also can be combined with other techniques, especially the outside-in method, to repair tears extending the entire axis of the meniscus. In addition, recent innovations may facilitate the repair of radial, horizontal, and root tear patterns that were previously considered difficult or impossible to suture ( Figs. 5 and 6 ). Relative contraindications include meniscocapsular separations and anterior horn tears.


Although there are numerous vendors that manufacture different devices, the current fourth generation of all-inside techniques commonly uses an arthroscopic needle to deploy backstop anchors across the meniscus tear to the outer surface of the joint capsule (extra-articularly), followed by a pre-tied sliding-locking knot that compresses the tear margins.
Replacement
Indications
Meniscus replacements can be performed via arthroscopic or mini open procedures, particularly when extensive meniscectomy is performed for significant tears that cannot be repaired.
Surgical candidates for synthetic meniscus implants may include skeletally mature, nonobese adults younger than 50 to 55 years with substantial unicompartmental tibiofemoral postmeniscectomy pain, a stable joint, normal alignment (eg, mechanical tibiofemoral angle ≤3°), and the ability to commit to a postoperative physical rehabilitation program. Contraindications generally include advanced chondrosis (eg, International Cartilage Repair Society [ICRS] grade 3 or 4 ipsilateral compartment lesions, <50% joint space narrowing), inflammatory arthritis, and infection.
The algorithm for selecting any particular procedure can vary depending on numerous factors, including the surgeon, geography, and available resources.
- •
Allograft transplants are most appropriate for extensive meniscus defects.
- •
Partial meniscus implants can be used to fill partial meniscectomy defects, which should be greater than two-thirds of the meniscal width, measuring less than 5 cm, with intact anterior and posterior horn/roots, and a stable rim at the popliteus hiatus. Total meniscus implants are still under clinical investigation; these prostheses are not available outside of clinical trials.
Techniques
Two general techniques are the subjects of intense interest to patients with postmeniscectomy syndrome: (cadaveric) meniscus allograft transplantation and (synthetic) meniscus implantation.
Allograft
Meniscal allografts are harvested from human donors and then transplanted, most commonly with attached bone as anchors using double bone plugs or a single bridge of bone placed in a tibial slot technique. In addition, soft-tissue fixation of the allograft to the joint capsule is necessary, but the meniscotibial attachments are not usually reconstructed.
Meniscus allograft transplantation may be performed as an isolated procedure but is more commonly combined with another procedure, such as anterior cruciate ligament (ACL) reconstruction, cartilage repair procedure, or high tibial osteotomy.
Accurate preoperative sizing of the allograft to match the recipient’s knee is critical to maximize the likelihood of a successful outcome. For a mismatch of even 10%, significantly increased contact forces occur on the articular cartilage in the setting of an oversized, extruded meniscus allograft or on the transplanted meniscus tissue because of an undersized meniscus allograft. Although sizing is usually performed with radiographs, MR imaging may be more accurate.
Implants
Unlike cadaveric allografts that require the sacrifice of any normal residual meniscus tissue that a patient might have, the synthetic scaffold implants can be customized to fit the size of a patient’s meniscus defect. The surgery for suturing one of these scaffolds into place is similar to repairing a bucket-handle tear (eg, a hybrid of all-inside and outside-in sutures), a less complex process than meniscus allograft transplantation.
The synthetic meniscus scaffolds for partial meniscus replacement are highly porous, acellular, bioresorbable implants manufactured with the aims of supporting ingrowth of meniscus-like tissue, alleviating postmeniscectomy pain, and preventing premature arthrosis.
Although the 2 available scaffold products are used in similar ways, they have very different compositions: one is polyurethane-based (Actifit; Orteq Ltd, London, UK) and the other is collagen-based (Menaflex Collagen Meniscus Implant; Ivy Sports Medicine LLC, Gräefelfing, Germany). The collagen-based product is processed type-I collagen from bovine Achilles tendon (97%) that is augmented with glycosaminoglycans to enhance ingrowth of meniscus fibrochondrocytes.
Another implant, currently in clinical trials, is a nonanchored, free-floating, disc-shaped interpositional prosthesis composed of a composite polymer (ie, polycarbonate-urethane reinforced with ultra–high-molecular-weight polyethylene fibers: NUsurface; Active Implants LLC, Driebergen, The Netherlands). In contrast to the scaffolds, the target population for this “total meniscus prosthesis” is currently middle-aged adults who have meniscus dysfunction and early osteoarthritis in the medial compartment.
Many other implants have been conceived and patented, such as a partial meniscus patch, coated with a protein cross-linking reagent and biocompatible adhesive to enhance surgical repair, and various complete meniscus implants, typically containing a reinforcing network of fibers embedded in the scaffold.
Augmentation (Regeneration)
With all meniscus repair techniques, there is intense research into augmenting the healing of both peripheral and nonperipheral tears. The fundamental paradigm in regenerative tissue engineering is that 3 factors act in concert to orchestrate a successful outcome: cells (to synthesize new extracellular matrix), scaffolds (for mechanical support of cells), and growth factors (to stimulate cell function).
Although specific MR imaging features are not widely reported, some techniques have been used for decades, including fibrin clot augmentation and mechanical stimulation, such as meniscus trephination, meniscus rasping, and synovial rasping. Such techniques may improve the success of meniscus repair substantially. For example, complete radial tears repaired with fibrin clot augmentation reportedly show high rates of healing at follow-up MR imaging and second-look arthroscopy. Another study found that intra-articular injection of human stem cells is associated with improved knee pain and meniscus regeneration on MR imaging.
Numerous other substances also may promote healing of fibrocartilage, but specific MR imaging findings are not widely reported. Such agents include platelet-rich plasma, bioadhesives such as those containing chondroitin sulfate, numerous growth factors such as myoblasts expressing recombinant cartilage-derived morphogenetic protein 2, and scaffolds such as gelatin hydrogel scaffold. Not all surgical techniques are successful, and MR imaging refinements may allow for objective, noninvasive diagnostic evaluation of surgical techniques at anatomic, cellular, and biochemical levels.
MR imaging protocols
Regardless of the particular imaging protocol chosen for one’s practice, the authors affirm that an optimal MR imaging interpretation has 3 prerequisites:
- •
A pre–MR imaging “history form” completed by the patient, including the site and duration of symptoms
- •
An operative note, including the timing and type of surgical procedure
- •
Preoperative imaging examination(s) for comparison ( Figs. 7 and 8 )

Fig. 7
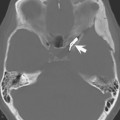
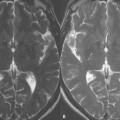
New meniscus tears. New medial and lateral meniscus tears in a 35-year-old snowboarder with new pain and mechanical symptoms 3 years after an anterior cruciate ligament (ACL) reconstruction. Postoperative PD ( A ) and fat-suppressed T2-weighted ( B ) coronal images reveal an intact ACL graft and a new horizontal tear of the body segment of the lateral meniscus ( small arrows ). There is also a new vertical peripheral tear of the body segment of the medial meniscus ( large arrows ) with a thin 5-mm displaced flap of the posterior horn seen just medial to the medial tibial spine ( arrowheads ). Having access to the baseline scan and the operative history made interpretation of this postoperative scan straightforward. The horizontal tear and the displaced flap were treated with a partial meniscectomies. The vertical peripheral tear was trephined and then repaired.

Fig. 8
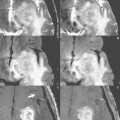
New tear after surgery. New tear of the posterior horn of the lateral meniscus in a 15-year-old girl with a recurrent injury 1 year after an ACL reconstruction. Preoperative PD ( A ) and fat-suppressed T2-weighted ( B ) sagittal images reveal a normal posterior horn of the lateral meniscus on the initial scan at the time of the acute ACL tear. The lateral meniscus was also normal at the time of ACL reconstruction 4 weeks later. Postoperative PD ( C , E ) and fat-suppressed T2-weighted ( D , F ) sagittal images reveal an intact, but vertically oriented ACL graft ( thick arrow ) and a new tear of the posterior horn of the lateral meniscus ( thin arrows ). Having access to the baseline scan and the operative history made interpretation of this postoperative scan straightforward. This new tear was treated with a partial meniscectomy.

Based on the MR imaging findings, the radiologist can verify independently that prior knee arthroscopy has been performed by looking for validated findings of characteristic fibrosis along portal tracts in and adjacent to the Hoffa fat pad. Less commonly, findings associated with meniscus repair may include susceptibility artifact at the joint line and findings of arthroscopic deep medial collateral ligament pie-crusting release, which is performed for expansion of the medial joint space in the case of a tight medial compartment.
Choice of Advanced Imaging Technique
The best technique for imaging the postoperative meniscus is a matter of active controversy.
- •
In some practices, an elaborate algorithm is used before scheduling 1 of 4 types of imaging examination: conventional MR imaging, indirect MR arthrography, direct MR arthrography, or computed tomographic (CT) arthrography. This algorithm includes several variables, including the presence or absence of a joint effusion (ie, minimal vs large), the type of prior meniscus surgery (ie, resection, repair, or replacement), and the extent of any prior partial meniscectomy (ie, more vs less than 25%).
- •
Other practices focus on the timing of prior meniscus surgery, opting for direct MR arthrography if surgery has been performed within the past 1 to 2 years.
- •
In the authors’ practices, the approach is simpler: we routinely begin with conventional MR imaging.
In particular, preference is to begin with a screening examination of paired fast spin-echo (FSE) PD and fat-suppressed T2 images in all 3 planes. If there is substantial postoperative metallic artifact, the technologist is instructed to perform a metal-artifact reduction protocol that includes optimized FSE PD and FSE inversion recovery pulse sequences ( Fig. 9 ). Experience has shown that these conventional MR images do a good (albeit imperfect) job in evaluating the post-operative knee; arthrographic techniques (also imperfect) are reserved for uncommon cases in which additional problem solving is deemed necessary.

Rationale for Conventional MR Imaging
The accuracy of conventional MR imaging for postoperative menisci is generally less than the accuracy achieved for menisci without previous surgery, and arthrographic techniques can aid in the diagnosis of some meniscus tears. However, as discussed by others, the authors routinely begin with conventional MR imaging to screen the postoperative knee, for the following reasons:
- •
Arthrographic techniques are associated with additional time, cost, discomfort, and risk, such as urticaria, vasovagal reaction, anaphylactic reaction, and septic arthritis. Primum non nocere.
- •
In the United States, the intra-articular administration of gadolinium-based contrast agents is off-label (ie, not specifically approved by the US Food and Drug Administration [FDA]).
- •
With MR arthrography, some tears do not fill with contrast material: the signal contacting the surface of a recurrent meniscus tear may be equal to or less than that of adjacent intra-articular gadolinium contrast material. Of note, when conventional MR imaging findings are consistent with a meniscus retear, but contrast material does not extend into the meniscus on MR arthrography, a meniscus retear is likely ( Fig. 10 ).

Fig. 10
True positive conventional MR imaging, with false-negative MR arthrography. Recurrent horizontal tear of the posterior horn of the medial meniscus 2 years after a partial meniscectomy in a 42-year-old woman. Postoperative PD ( A ) and fat-suppressed T2-weighted ( B ) sagittal images reveal a new horizontal tear of the posterior horn of the medial meniscus ( arrow ). A fat-suppressed T1-weighted sagittal image ( C ) after an arthrogram 1 week later with dilute gadolinium contrast shows linear increased signal at the site of the tear ( small arrow ), but no definite filling of the tear with high signal intensity that is as bright as the dilute gadolinium contrast within the joint space. The arthrogram was interpreted as negative (although some studies suggest this finding indicates a tear). At arthroscopy 3 weeks later, a new horizontal tear was found and was again treated with a partial meniscectomy.
- •
With MR arthrography, it can be difficult to determine whether mild or moderate increased signal intensity in a postoperative meniscus represents contrast material in a tear, unless precontrast MR imaging also is performed, requiring additional time and scheduling challenges.
- •
With MR arthrography, the imbibition of contrast material into a repaired meniscus tear does not necessarily indicate that the tear is unstable or responsible for symptoms. In fact, some surgeons leave small stable tears alone to maximize meniscus preservation.
- •
With MR imaging, the development of a parameniscal cyst is a specific, albeit insensitive, finding of a meniscus tear ( Fig. 11 ), but these cysts often do not fill with contrast material on arthrographic examinations.

Fig. 11
Recurrent horizontal tear with parameniscal cyst. Recurrent horizontal tear 6 years after a partial meniscectomy with trimming of a free-edge radial tear of the medial meniscus in a 53-year-old golfer. Postoperative PD ( A ) and fat-suppressed T2-weighted ( B ) sagittal images of a horizontal tear of the posterior horn of the medial meniscus ( arrow ) communicating with a tiny parameniscal cyst ( arrowhead ).
- •
With a substantial internal derangement, a native joint effusion is often present (defined as anteroposterior distension of the suprapatellar recess by >5 mm or the lateral parapatellar gutter by >10 mm), which tends to mildly increase the accuracy of nonarthrographic MR imaging examinations.
- •
When less than 25% of the meniscus has been resected, the literature indicates that there is no significant benefit of MR arthrography over MR imaging. Such low-grade partial meniscectomies are much more common than high-grade meniscectomies or meniscus repairs ( Fig. 12 ).

Fig. 12
Expected postmeniscectomy findings. No recurrent tear of the lateral meniscus 5 years after a partial meniscectomy with free-edge trimming of a horizontal tear of the body segment of the lateral meniscus in a 56-year-old physician complaining of vague knee pain. Preoperative PD ( A ) and fat-suppressed T2-weighted ( B ) coronal images reveal a horizontal tear of the body segment of the lateral meniscus ( arrow ). Postoperative PD ( C ) and fat-suppressed T2-weighted ( D ) coronal images reveal an intact meniscal remnant without evidence of a new tear.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree