, Valery Kornienko2 and Igor Pronin2
(1)
N.N. Blockhin Russian Cancer Research Center, Moscow, Russia
(2)
N.N. Burdenko National Scientific and Practical Center for Neurosurgery, Moscow, Russia
Meningioma is the most common intracranial tumor among neoplasms of non-glial origin (Buetow et al. 1991; Osborn 2004). Benign forms of meningiomas are histologically characterized by a uniform arrangement of cells with moderate polymorphism of nuclei, lack of necrosis and mitoses. In this group, there are the following meningiomas: fibroblastic, meningotheliomatous, secretory, transitional, psammomatous and other meningiomas. Atypical (usually meningotheliomatous and mixed) meningiomas are characterized by pronounced polymorphism of cells and nuclei, presence of necrosis and mitotic figures, which results in the characteristic radiographic manifestations similar to those in metastases.
Meningiomas occur most frequently in the falx cerebelli and parasagittal area (up to 50%) and in the ACF base region (up to 10% of all intracranial meningiomas). The neoplasm grows from the dura mater covering the intracranial surface of the skull or dural sleeves extending to some cranial nerves. Classic bone hyperostosis is detected in about 5% of cases, however, the majority of patients are examined by MRI, and, therefore, many examinations do not clearly visualize and evaluate hyperostotic bone changes. Bone erosion can occur in all types of meningiomas; they can also cause bone destruction, but still hyperostoses are more frequently observed.
By their appearance, meningiomas are subdivided into two main forms. The first group includes tumors with a spherical, lobular shape. The second group is characterized by a flat form infiltrating the adjacent meninges and often the bone (Fig. 31.1).
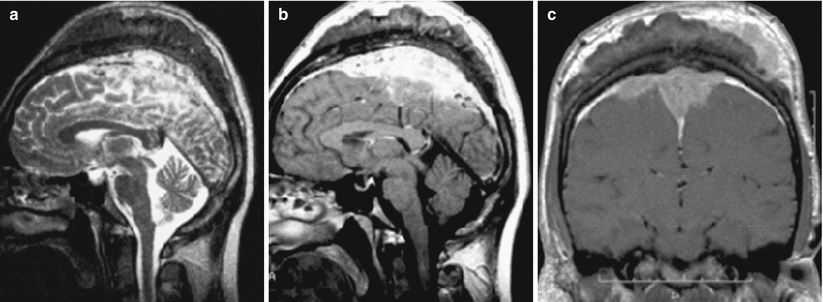

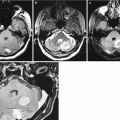
Fig. 31.1
Meningioma. In the fronto-parietal convexital area on T2-weighted (a) and T1-weighted MRI after intravenous CA administration (b, c), a flat space-occupying lesion is detected, intensely accumulating the contrast agent, infiltrating the adjacent bone, meninges and soft tissues of the fronto-parietal region. The tumor that has V-type spread along the falx completely invades the superior sagittal sinus
Meningiomas are usually well separated from the adjacent brain substance. The surface of most tumors is smooth or lobular. There is often a pronounced arachnoid (CSF) cleft containing dislocated vessels and elements of the dura mater between the brain substance and the surface of the meningioma.
CT with contrast enhancement is one of the main methods of primary visualization for meningiomas, allowing to diagnose at least 95% of intracranial neoplasms (Konovalov and Kornienko 1985a, b). Meningiomas are most often identified as lesions with well-differentiated contours due to intense (40–45 HU) contrast agent accumulation. Therefore, the use of contrast enhancement is one of the principal constituent elements of CT diagnosis of meningiomas. In a quarter of cases, meningiomas weakly accumulate the contrast material. In general, in up to 75% of all cases, meningiomas have more or less hyperdense characteristics. Up to 25% of meningiomas contain calcifications in their structure, which can be individual or multiple, punctate and very large. 3D CT reconstructions are useful in hyperostotic meningiomas to estimate the extent of bone destruction (Fig. 31.2).
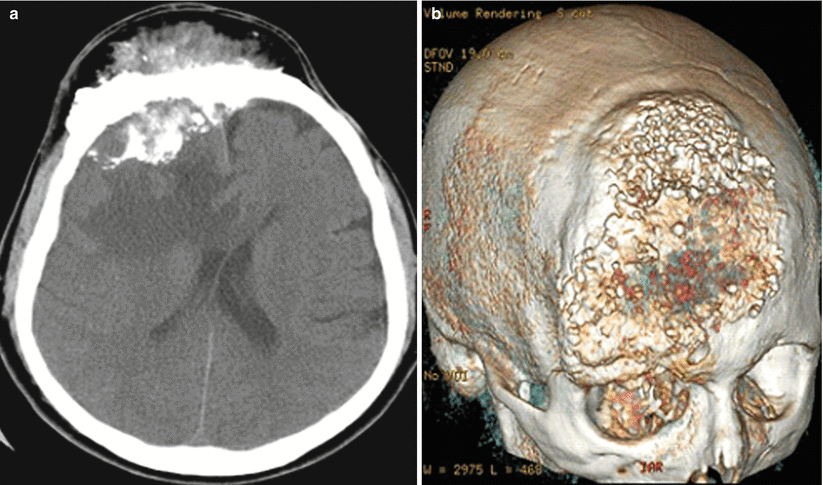

Fig. 31.2
Meningioma. On CT, in the area of the squama of the frontal bone (more on the right), there is a large lesion with hyperostotic inclusions. In the axial projection (a), there are tumor structures with increased density, extending both intra- and extracranially. On 3D-reconstruction (b) the extent of destruction of the bone tissue can be clearly determined
On perfusion-weighted CT images, meningiomas are divided into three main types based on their hemodynamic manifestations that correlate well with the results of direct cerebral angiography. We distinguished the following hemodynamic types of tumors:
Type 1—low CBV (2.5–5.0 ml/100 g) and CBF (25–30 ml/100 g/min) values with or without tumor vasculature minimally visualized on AG;
Type 2—a moderate increase in CBV, CBF (10–11 ml/100 g and 70–80 ml/100 g/min, respectively) with a moderately expressed vascular spot in the capillary phase of AG;
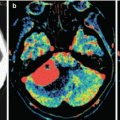
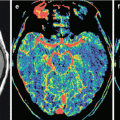
Type 3—a pronounced increase in meningioma hemodynamics (CBV—21–24 ml/100 g, CBF—110–125 ml/100 g/min) in the presence of a highly vascularized tumor on angiograms (Fig. 31.3).

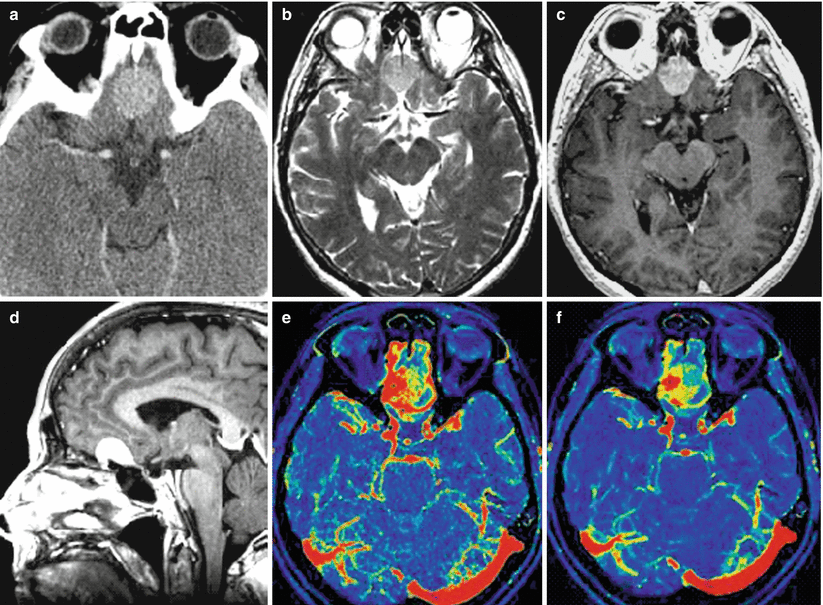
Fig. 31.3
Meningioma. In the projection on the olfactory fossa, on axial CT (a) with contrast enhancement, on T2-weighted (b) and T1-weighted MRI after CA administration (c, d), a lenticular tumor lesion is determined with homogeneous contrast accumulation. On CT perfusion of CBF (e) and CBV (f), there are areas with both high and average blood flow values
The nature of MR signal changes in different histological forms of meningiomas is ambiguous. On T1-weighted MRI, most meningiomas, regardless of their histological type, appear as iso- or hypointense space-occupying lesions as compared to the cerebral cortex. Changes in MR signal on T2-weighted MRI can correlate with histologic subtypes of meningiomas. Thus, up to 90% of fibroblastic and transient subtypes, as well as psammomatous meningiomas have lower signal intensity in T1- and T2-weighted images as compared to the white matter of the brain, while two thirds of meningotheliomatous tumors are hyperintense in T2-weighted images.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree