Fig. 12.1
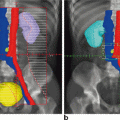
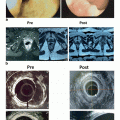
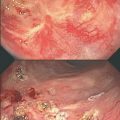
Sacral insufficiency fracture. 86-year-old male with a history of T3 N0 M0 adenocarcinoma of the rectosigmoid colon who received neoadjuvant chemoradiation therapy including 45 Gy administered at 1.8 Gy per fraction. CT images of the pelvis were obtained 1 month after completion of the radiation therapy. There was a baseline of mildly decreased bony mineralization diffusely which was thought to be related to the patient’s age. a Axial CT image of the pelvis at the level of S1 demonstrates no sacral ala fractures. b A sagittal reformation of the pelvis shows that the sacral alignment is preserved. Similarly acquired CT images of the pelvis respectively were obtained 8 months after the initial postradiation therapy CT study. c Axial CT image of the sacrum at the level of S1 demonstrates focal discontinuity of the anterior cortices of the bilateral sacral ala with small fractures tracking posteriorly (ARROWHEADS). d Sagittal reformation of the sacrum demonstrates a small minimally displaced fracture through the anterior cortex of S3 (ARROW), propagation of the fracture through the neural arch (Arrowhead) and subtle kyphotic angulation at the fracture site. e A nuclear medicine bone scan was performed 13 months after the initial postradiation therapy CT study using Tc-99m MDP. This study shows delayed posterior planar image of the entire body demonstrates focal radiotracer uptake longitudinally along the bilateral sacral ala with band of transverse uptake at the level of S3—the so-called “Honda sign” named for the similarity of the radiotracer uptake pattern to the H-shaped corporate logo. The transverse band of radiotracer uptake at S3 is partially obscured by the prominent amount of radiotracer present within the overlying urinary bladder (CIRCLE). f shows a right posterior oblique image which better demonstrates the H-shaped distribution of the radiotracer uptake along the sacrum when the radiotracer in the urinary bladder (CIRCLE) is rotated away from the sacrum by altering patient position. An MRI of the pelvis was performed 15 months after the initial postradiation therapy CT. g A coronal T1-weighted image of the sacrum demonstrates the H-shaped pattern of low signal which delineates the morphology of the sacral insufficiency fractures through the bilateral sacral ala and transversely crossing the superior margin of the S3 vertebral body. h A coronal STIR sequence of the sacrum shows abnormal increased signal suggestive of edema about the fracture planes. CT images of the pelvis were obtained 28 months after the completion of radiation therapy. i Axial CT image of the superior sacrum at the level of S1 show progression of fracture planes along the sacral ala bilaterally without extension into the sacroiliac joints or adjacent S1 neural foramina. There is no discrete osseous bridging along the fracture planes however there is reactive bone formation along the fracture margins. j Sagittal reformation of the sacrum demonstrates similar reactive bone formation along the margins of the transverse S3 fracture site without osseous bridging across the fracture planes. There has been progression of the compression deformity at the S3 fracture site with worsening of the associated kyphotic angulation. STIR Short T1 Inversion Recovery
Positron emission tomography/CT (PET/CT) using 2-[F-18] fluoro-2deoxy-D-glucose (FDG) has also been used in the evaluation of pelvic fractures in patients with a history of pelvic malignancy who have received prior radiation therapy with the aim of differentiating radiation-induced insufficiency fractures from fractures occuring through recurrent or metastatic bone neoplasms. Maximum standardized uptake values (SUVmax) measured at fracture sites as well as the distribution of uptake at the fracture site (cortical vs. intramedullary) have been used to differentiate insufficiency from pathologic fractures [16]. However, in the setting of radiation-induced pelvic insufficiency fractures, the SUVmax alone has not been shown to reliably differentiate between pathologic and insufficiency fractures [8,16]. It should be noted, however, that the distribution of increased FDG uptake in radiation-induced pelvic insufficiency fractures of the sacrum may appear as an incomplete variant of the H-shaped pattern described on 99mTc-MDP bone scans [8, 17]. Often, the CT component of the PET/CT scan can offer crucial information regarding the presence of a fracture line, reactive bone formation about a nondisplaced fracture or the presence of an underlying pathologic lesion.
Treatment Overview
The vast majority of patients with pelvic insufficiency fractures can be treated medically; although, early consultation with an orthopedic surgeon is recommended. The orthopedic surgeon will be able to assess the stability of the fracture pattern, help determine weight bearing and activity restrictions, as well as follow the patient’s course and determine if surgical intervention is indicated. Although some patients with acute fractures may require a short hospital stay for initial evaluation, pain control, and to facilitate a safe rehabilitation plan, this is not the norm. Most patients can be evaluated and managed on an outpatient basis.
Patients often require a brief period of narcotic analgesics for comfort, but the treatment goal should be that of early transition to nonnarcotic analgesics as to avoid side effects and dependence. An orthopedic surgery consultation should be sought to evaluate the stability of the fracture pattern and to offer weight-bearing recommendations. Stability is generally defined as the ability of the structure involved to maintain alignment under physiologic loading. These assessments are best made by orthopedic surgeons comfortable with fracture management. After weight-bearing recommendations are made by the orthopedic surgeon, a physical therapy consultation should be sought. The physical therapist can perform a functional assessment and determine the patient’s ability to safely mobilize given their restrictions. The therapist will then be able to provide gait training with an assistive device that fits the patient’s needs. In patients with unstable pelvic or periarticular fractures around the acetabulum or femoral head, toe-touch weight-bearing (enough for balance only) is recommended for several weeks to months. Elderly patients and those with coordination or muscle deficits may not be able to comply with these restrictions and may fully weight bear if permitted to mobilize with restrictions. If there is sufficient concern for fracture displacement, this type of patient may require a wheelchair. Alternatively, if a patient has a stable fracture pattern, they may be allowed to fully weight bear. Although they are cleared to walk without fear of displacement, pain may preclude walking without some type of assistive device such as a walker, crutches, or a cane.
Next, an investigation into the patient’s risk factors such as vitamin D deficiency and underlying osteoporosis should be performed and acted upon. Many would argue that this investigation should be done prior to or during radiation therapy; although, the concept of prescreening and treating hypovitaminosis D patients in hopes of reducing pelvic insufficiency fractures has not yet been investigated. Treatment of patients with pelvic insufficiency fractures should include, at the very minimum, adequate analgesia and calcium/vitamin D supplementation. Additionally, bisphosphonate and teraparatide therapy could be indicated in certain scenarios.
Although bisphosphonate therapy is heavily studied in fragility fractures including pelvic fractures, the same level of investigational interest has not occurred in patients who have fractured through irradiated bone. However, animal research has shown that prophylactic treatment of irradiated mice with a bisphosphonate prevented a rise in osteoclast number, bone loss, and impaired microarchitecture when compared to controls [18]. Despite laboratory data, we cannot directly apply this animal model to human subjects nor can we determine if the difference observed would be clinically significant. It remains unknown if prophylactic treatment with bisphosphonates prior to pelvic irradiation would reduce pelvic insufficiency fractures. Clinical investigation is clearly needed in this area.
Although clinical study of direct treatment with bisphosphonates after fracture through irradiated bone has not been conducted, the sentinel event of a pelvic insufficiency fracture often prompts an investigation leading to a diagnosis of osteoporosis. Many of these patients will eventually be treated with bisphosphonates in order to prevent additional fragility fractures. Bisphosphonate therapy is certainly reasonable in such cases; however, bisphosphonate treatment for patients with radiation-induced pelvic insufficiency fractures in the absence of osteoporosis is not indicated.
Parathyroid hormone (PTH) is the newest treatment modality in the armamentarium for pelvic insufficiency fractures. PTH is a systemic regulator of calcium homeostasis [19]. It is released from the parathyroid gland in response to hypocalcemia and increases serum calcium concentration by promoting osteoclast-mediated bone resorption, calcium reabsorption in the kidneys and intestinal absorption of calcium through the production of the active vitamin D metabolite 1,25-dihydroxy vitamin D. Continuous exposure to PTH is catabolic and results in hypercalcemia and a decrease in bone volume [20]. Intermittent exogenously administered PTH leads to an anabolic effect on bone. Two preparations for intermittent therapy are available in Europe: PTH 1-84 and PTH 1-34. Naturally occurring PTH is a polypeptide containing 84 amino acids, while recombinant PTH (PTH 1-34), also called teraparatide, consists of the first 34 amino acids of the human PTH. Only teraparatide is currently available in the United States of America. Extensive scientific analysis in various skeletal repair models in animals including fracture repair have demonstrated the importance of PTH in mesenchymal cell proliferation and differentiation, enchondral bone formation, membranous bone formation, and callus remodeling [20].
Human studies have been performed as well. Treatment of distal radius fractures in postmenopausal women and elderly osteoporotic women with pubic bone fractures have been reported. There are several reports of level IV data as well, including the successful treatment of patients with tibial and humeral delayed unions, which are very promising [20–23]. Most pertinent for this discussion, is the effect of PTH on the clinical and radiographic outcome in elderly osteoporotic women with pubic fractures. Treatment resulted in a mean time to fracture union in the treatment group of 7.8 weeks compared to 12.6 weeks in the control group [20]. Visual analog scale pain scores and functional testing also significantly favored PTH treatment group. These findings suggest that use in the radiation-induced pelvic insufficiency fracture cohort may be indicated.
In very rare circumstances, surgical intervention may be considered. Given the low energy mechanism associated with pelvic insufficiency fractures, it is extraordinarily rare to have an unstable pelvic ring fracture that meets operative criteria. If operative intervention is to be considered, a more likely scenario would be that of a periarticular fracture of the acetabulum that results in joint incongruity, posttraumatic degenerative joint disease, femoral head osteonecrosis with associated subchondral fracture, or a femoral neck fracture. Shared decision making between the orthopedic surgeon and patient may result in pursuance of a total hip arthroplasty with or without a stabilization procedure for the acetabulum. It is important to set appropriate expectations in these patients because the outcomes in this scenario are not the same as for patients with primary arthritis. Joint replacement in irradiated bone is fraught with complications such as increased incidence of wound healing issues, infection, and component loosening. The result is a prosthetic joint replacement with longevity that is inferior to total hip arthroplasty in the nonirradiated patient.
Sacral Insufficiency Fracture s
Nearly 80 % of patient’s sustaining pelvic insufficiency fractures associated with pelvic irradiation have sacral involvement, making this the most common site of fracture. They occur in about 15 % of patients treated with radiation therapy, with a wide range of 3–45 % reported in the literature [1, 2, 24]. The most common site within the sacrum is the sacral ala, which is lateral to the sacral foramina and medial to the sacroiliac joints. An example of this fracture pattern is illustrated in this 44-year-old female with cervical cancer treated with 45 Gy external beam radiation therapy and an additional 5 Gy brachytherapy at the vaginal cuff (Fig 12.2). There is no laterality predilection and half will have bilateral sacral ala involvement. Over 60 % will have multiple fractures, such as a sacral fracture with an associated pubic ramus fracture [1, 2].
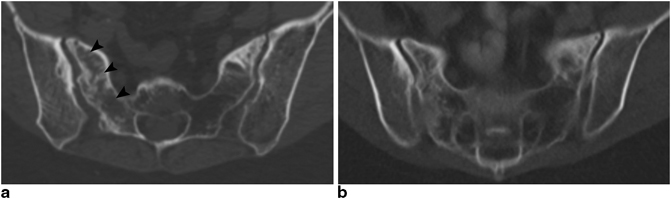

Fig. 12.2
Sacral insufficiency fracture. 44-year-old female with a history of stage Ib squamous cell carcinoma of the cervix status postradical hysterectomy with pelvic lymph node dissection and postoperative chemoradiation therapy which included cisplatin as well as external beam radiation therapy involving a total dose of 45 Gy administered over 5 weeks with additional 5 Gy brachytherapy to the vaginal cuff. a CT axial images of the pelvis at the level of the S2 vertebral body obtained 3 years after completion of radiation therapy demonstrate an irregular longitudinal fracture (ARROWHEADS) obliquely traversing the right sacral ala medial to the right sacroiliac joint and lateral to the S1 and S2 neural foramina. Heterogeneous bony mineralization about the sacroiliac joints and along the bilateral sacral ala was thought to reflect a background of underlying osteoradionecrosis. b The right sacral ala insufficiency fracture was managed conservatively. CT axial image of the pelvis at a similar level to (a) obtained 6 years after completion of radiation therapy shows interval healing of the previously demonstrated right-sided sacral alar insufficiency fracture with osseous bridging and bony remodeling along the fracture site
In studies that have concentrated on radiographic screening with clinical correlation, about half of all sacral insufficiency fractures identified on either MRI, CT, or bone scan are symptomatic [1]. Clinical presentation is usually that of low back pain without radicular symptoms but can include reports of hip or groin pain if there is an associated anterior lesion. The traditional thinking is that like any ringed structure, the pelvic ring rarely breaks in just one place, so one should have a high suspicion for the presence of anterior and posterior lesions in patients presenting with low back and hip or groin pain, even if there is only one radiographically visible fracture. Neurologic deficits are exceedingly rare and the presence of a neurologic deficit does not preclude nonoperative treatment.
Although symptoms are usually mild to moderate, narcotic analgesics may be required during the acute period after sustaining a sacral insufficiency fracture. Orthopedic consultation should be sought early so recommendations on weight bearing and activity as well as a discussion on treatment options can commence immediately. There remains debate on whether to treat patients with a short period of bed rest or with early mobilization. There is no evidence implicating early mobilization with extended duration of symptoms or even increased narcotic use. There are however several reports illustrating the deleterious effects of bed rest, especially in the elderly, with respect to the development of deep vein thrombosis and decubiti, decreased muscle strength, as well as cardiopulmonary, gastrointestinal, and genitourinary complications. Despite no clear guidance in the literature in treating this particular cohort, the authors’ treatment preference is early mobilization as to reduce potential complications associated with bed rest. A physical therapy consultation should be arranged as to facilitate a functional assessment of the patient’s ability to protectively weight bear and subsequent pairing of the safest ambulatory assist device for the patient.
There is no role for rigid bracing in this injury pattern and early surgical intervention is rarely indicated. The average duration of symptoms in this group is 20 months but pain can be permanent in some cases. In a study by Ikushima et al., 72 % of patients required analgesics for an average duration of 4 months, while 44 % required inpatient hospitalization for symptom control [4]. The typical medical treatment algorithm is that of acute treatment with narcotic analgesics with early transition to nonnarcotic analgesics or nonsteroidal anti-inflammatory drugs (NSAIDs) and a rehabilitation program. For patients with persistent disabling pain, percutaneous CT-guided sacroplasty could be offered; however, this treatment modality has not been studied extensively.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree