Imaging Presentation
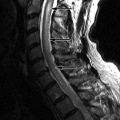
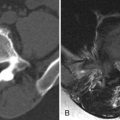
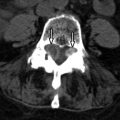
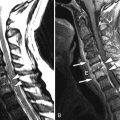
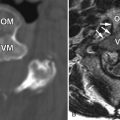
Magnetic resonance (MR) image of the spine revealed a large enhancing intradural mass extending from the tip of the conus medullaris (mid T12) to the superior L2 level. A smaller intradural mass is located within the thecal sac at the L2-3 level ( Figs. 50-1 to 50-5 ) . The patient’s symptoms eventually resolved and he delayed surgery until his symptoms returned 3 months later. Surgery consisted of L1-L5 decompressive laminectomy, intradural exploration, and gross total removal of the multilobulated tumor. Radiologic and pathologic diagnosis was myxopapillary ependymoma.





Discussion
Of all intramedullary cord tumors, 95% are gliomas (astrocytomas or ependymomas); 65% of cord gliomas are ependymomas in adults. Myxopapillary ependymomas comprise 30% of all ependymomas and 13% of spinal ependymomas. They represent the most common intradural tumor involving the conus medullaris and cauda equina. Approximately 90% of tumors involving the conus medullaris/cauda equina junction are myxopapillary ependymomas. They are histologically benign tumors, classified as World Health Organization (WHO) grade I, and although they may recur locally after surgery, rarely disseminate in the central nervous system (CNS). They usually manifest in middle-aged adults, usually in the fourth decade of life, with back pain, lower extremity weakness, and radiculopathy and may produce loss of bladder and bowel control. The symptoms are usually slowly progressive because these tumors usually grow very slowly. Hemorrhage into the tumor can rarely cause rapid increase in tumor size, resulting in a cauda equina syndrome. Myxopapillary ependymomas can rarely arise in the subcutaneous tissues posterior to the sacrococcygeal junction. Such tumors are believed to arise from the coccygeal medullary vestige or subcutaneous ependymal rests.
Imaging Features
Typically, these lesions are relatively well circumscribed, lobulated masses that usually extend 1 or 2 vertebral levels, but may be multiple or more extensive, filling the entire lumbar spinal canal. They usually grow very slowly, so they may not be detected until they are quite large. Plain radiographic (plain X-ray) findings are present in 60% of patients, more common with tumors occurring in the lumbar region. They can produce expansion of the spinal canal and posterior vertebral body scalloping and also medial erosions/remodeling of the pedicles. MR imaging is the procedure of choice for evaluating spinal cord tumors. On MRI, these masses are usually T1 isointense (see Fig. 50-1 ) but can be T1 hyperintense, because of the presence of intratumoral mucin. Mucin is not usually present in cellular ependymomas of the cervical cord. Myxopapillary ependymomas are predominantly T2 hyperintense with respect to the cord (see Fig. 50-2 ). They may contain small tumoral cysts or areas of necrosis and intratumoral hemorrhage (see Fig. 50-3 ) is common, as with cellular intramedullary ependymomas in the cervical region. Myxopapillary ependymomas usually display intense heterogeneous enhancement (see Figs. 50-4 and 50-5 ). These tumors can produce subarachnoid hemorrhage, but this is rare. The presence of superficial siderosis can be secondary to a myxopapillary ependymoma. Myxopapillary ependymomas generally enhance intensely although somewhat heterogeneously after IV contrast ( Figs. 50-5 and 50-6 ). Myxopapillary ependymomas have an extremely low tendency to metastasize. However, ependymomas involving the conus or cauda equina may be secondary to ependymomas elsewhere in the CNS. Therefore, the entire spinal axis should be imaged if a spinal ependymoma is discovered, regardless of location. Calcifications rarely occur in spinal ependymomas.