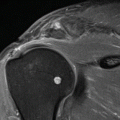
Fig. 39.1
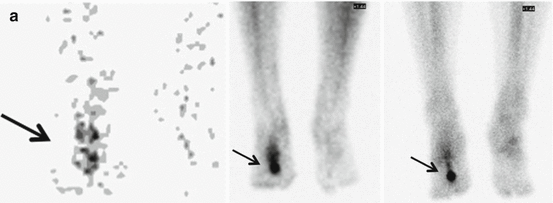
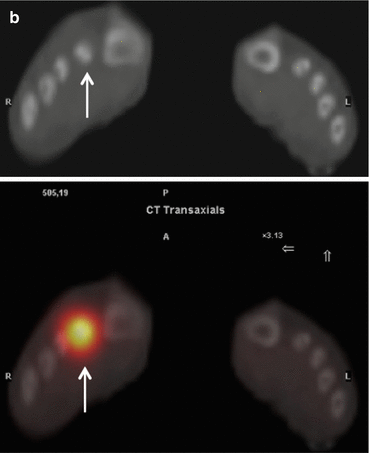
SPECT – (high resolution) CT images (left to right: transverse, sagittal, and coronal) of the left foot of a 21-year-old female with an os tibiale externum in both feet and a history of fixation of the os tibiale externum at the left side, with persistent pain. SPECT-CT shows high focal activity in the os tibiale externum at the left side, indicative of nonunion. No increased activity is found at the side of the right os tibiale externum (not shown) (Images provided by J. Lavalaye, St. Antonius Hospital Nieuwegein, The Netherlands)
39.2 Tendinopathies
All tendons in the foot are at risk for tendinopathy due to overuse. Most common tendinopathies in the foot are related to muscles of the lower leg. For instance, overuse of the peroneal and tibial muscle groups can result in tendinopathy in the foot near the insertion (enthesopathy) but also near the ankle because of friction in its fibro-osseous groove between the retinaculum and the bones of the ankle. Examples of frequently involved tendons are the posterior tibial tendon, the peroneal tendon (Fig. 39.2), the flexor hallucis longus tendon, and the anterior tibial tendon. The most common soft tissue injuries of the foot in athletes are Achilles paratendinopathy and insertional Achilles tendinopathy.
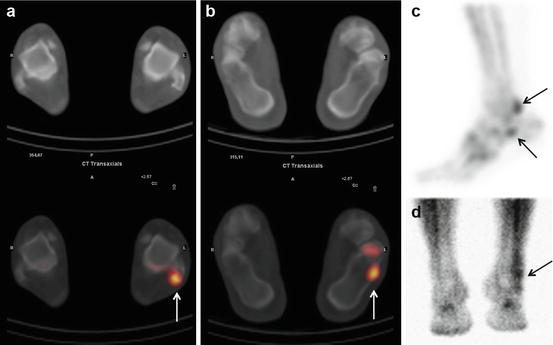

Fig. 39.2
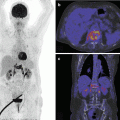
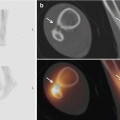
Transverse SPECT-CT images (a, b), maximum intensity projection (c), and planar soft tissue phase images from the anterior (d) of a 26-year-old male with pain and swelling at the lateral side of the left ankle. The early images show hypervascularity and increased soft tissue uptake at the lateral side of the left ankle along the anatomical course of the peroneal tendon; SPECT-CT shows focal increased tracer uptake at the posterocaudal side of the lateral malleolus and in the area of the trochlea peronealis calcanei (arrows) due to friction between the retinaculum and the calcaneus, suggestive of peroneal tendinitis
The cause of tendinopathy is still not clear. Multiple risk factors, including genetic factors, are implicated in the etiology of soft tissue injuries including Achilles tendon injury (Collins and Raleigh 2009). These injuries are related to relative overuse (Tan and Chan 2008), secondary to an imbalance between intensive training leading to repetitive mechanical and chemical microtrauma and (inadequate) recovery leading to a breakdown in tissue reparative mechanisms (Cosca and Navazio 2007). Eventually, this may result in the formation of ectopic bone deposits in tendon tissue. Although acute injury may lead to true tendinitis, histopathologic studies have shown that overuse tendinopathies are degenerative rather than inflammatory (Cosca and Navazio 2007). The histopathological findings in athletes with overuse tendinopathies are consistent with those in tendinosis, which is a degenerative condition of unknown etiology (Khan et al. 1999). Tendinopathy is a clinical diagnosis. Additional imaging may be conducted to validate the diagnosis. In heel pain, lateral X-rays of the foot may show a Haglund’s deformity, which is an enlargement of the posterosuperior prominence of the calcaneus, frequently associated with insertional Achilles tendinopathy. However, Kang and coworkers showed in a retrospective radiographic review of 44 patients with insertional Achilles tendinopathy that a Haglund’s deformity was not indicative of insertional Achilles tendinopathy and was also present in asymptomatic patients (Kang et al. 2012). Three-phase bone scintigraphy may be helpful in confirming the diagnosis. In tendinopathy, increased activity in the early phase is seen because of hyperemia, related to angiogenesis at the tendon and/or to a secondary inflammatory reaction during active resorption of the calcific deposit. In the delayed phase, bone scintigraphy shows increased uptake at the insertion of the tendon (Fig. 39.3).
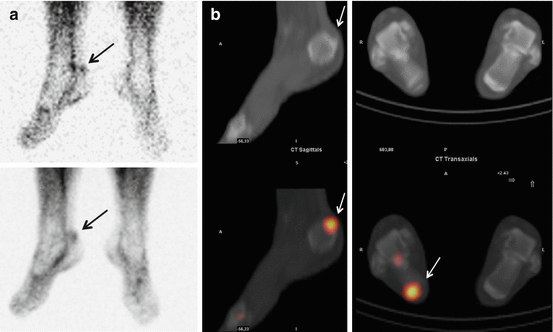

Fig. 39.3
Early images (a, vascular phase (upper) and soft tissue phase (lower)) and SPECT-CT (b) with a sagittal image of the right foot (left) and a transverse image of both feet (right) of a 70-year-old female with pain at the dorsal side of the right heel. The early images show focal hypervascularity and increased soft tissue uptake at the dorsal side of the right calcaneus (arrow); SPECT-CT shows a Haglund’s deformity at the right side and focally increased bone activity at the insertion of the tendon (arrow)
39.3 Plantar Fasciitis
Plantar fasciitis is thought to result from microtrauma of the plantar fascia related to overuse. As in tendinopathy, histological studies show no evidence of inflammation but the characteristics of a fasciosis (Lemont et al. 2003; Cutts et al. 2012). A better definition for this condition is plantar enthesophytosis or inferior calcaneal enthesophytosis. However, the fact that many patients react to local corticosteroid injections or oral anti-inflammatory drugs suggests that inflammation may play a role in a subgroup of patients, possibly triggered by the microscopic tears in the plantar fascia (Woolnough 1954; Cutts et al. 2012).
As is the case with tendinopathy, plantar fasciitis is a clinical diagnosis, which can be supported by additional imaging. Plain lateral radiographs may show a calcaneal spur. Studies have demonstrated a significant association between plantar fasciitis and calcaneal spur formation: a calcaneal spur is present in 85–89 % and 32–46 % of patients with plantar fasciitis and controls, respectively (Osborne et al. 2006; Johal and Milner 2012). But it is not clear whether this association is causal; the spur is not related to the plantar fascia and is the attachment of the quadratus plantae muscle. So, the heel spur could represent an unrelated incidental finding. Osborne and coworkers demonstrated that the key radiological features that differentiate patients with plantar fasciitis from controls were not spurs but rather changes in the soft tissues like plantar fascia thickness and fat pad abnormalities (Osborne et al. 2006), which can be measured by ultrasonography (Kane et al. 2001). Three-phase bone scintigraphy shows (focal) hyperemia and a focal accumulation anteromedially in the calcaneus in patients with plantar fasciitis. Ultrasonography and bone scintigraphy have shown to be equally effective in the diagnosis of plantar fasciitis (Kane et al. 2001). Frater and colleagues demonstrated that especially focal hyperemia in the early phase of bone scintigraphy seems to correlate well with response to treatment (Frater et al. 2006).
39.4 Sprains
In sports activities, direct or indirect trauma can result in all kinds of sprains. Most sprains involve the ligaments of the ankle and not the foot. Sprains involving ligaments of the foot are, for example, located in the midfoot and in the first metatarsophalangeal joint (see Sect. 39.5). In the situation that these sprains are the only trauma, three-phase bone scintigraphy will show hyperemia in the early phases and almost no activity in the third phase, except discrete diffuse uptake due to the hyperemia. In more severe sprains, the bone in the adjacent joints is often also traumatized resulting in bone bruising or even small fractures. This will give rise to focal uptake in the third phase of a bone scan. Examples are the Lisfranc and Chopart injuries (see Sect. 39.7.1).
39.5 Injuries Involving the First Metatarsophalangeal Joint and Hallucal Sesamoids
The sesamoid complex is located centrally and plantar to the first metatarsal head, where the sesamoids are imbedded within the tendon of the flexor halluces brevis. Several injuries and pathologic conditions can involve the hallucal sesamoidal complex and plantar capsular structures of the first metatarsophalangeal joint. The hallucal sesamoids are crucial to normal weight bearing and foot mechanics; during push-off, the complex can transmit loads of more than 300 % of body weight (Dedmond et al. 2006). These high stresses may lead to both acute and chronic pathologies of the hallucal sesamoids, including, stress fracture, avascular necrosis, osteochondral fractures, and chondromalacia. In addition, the abnormal motion range of the metatarsophalangeal joint during sports activities (Riley et al. 2012) can lead to the so-called turf toe injury, a plantar capsuloligamentous sprain of the first MTP joint (McCormick and Anderson 2010).
As the clinical presentation and physical findings of the different pathologic entities may be identical, imaging plays an important role in the diagnostic process and in directing appropriate therapy. Radiographs are often normal in the first six months following onset of symptoms. In contrast, bone scintigraphy is a highly sensitive technique demonstrating radiotracer uptake in an early phase of the pathologic process. The combination with SPECT-CT makes it possible to locate the pathology with high accuracy. The simultaneously acquired functional and anatomical data can clarify the nature of the pathology and distinguish, for example, fractured sesamoids from other causes of sesamoid pathology or even an anatomical variant (Fig. 39.4). One should be aware of the fact that tracer uptake in the first metatarsophalangeal joint is frequently observed in asymptomatic patients with beginning, age-related arthrosis (O’Duffy et al. 1998). Although the intensity of uptake in such cases is usually mild, the specificity of the bone SPECT abnormalities in this area needs to be further elucidated.
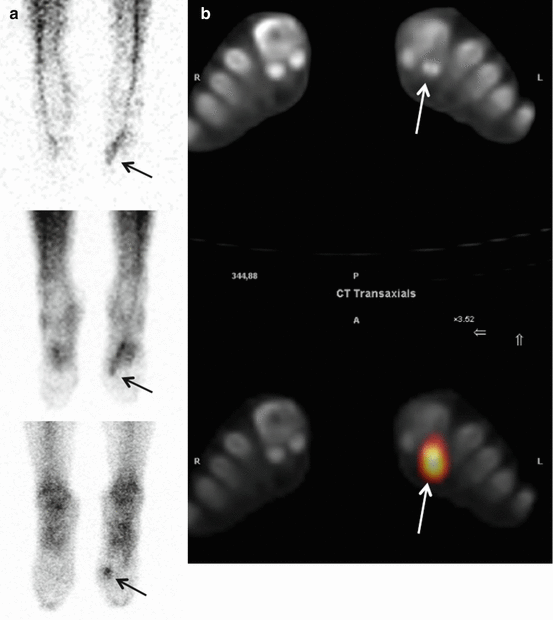

Fig. 39.4
Planar images of the feet from anterior (a, vascular phase (upper), soft tissue phase (middle) and delayed phase (lower)) and transverse SPECT-CT image (b) of both feet of a 23-year-old female with pain and swelling at the left forefoot. The early images show focal hypervascularity and increased soft tissue uptake in the region of the first metatarsophalangeal joint of the left foot and increased tracer uptake at this site in the delayed phase (arrows). SPECT-CT images locate the increased uptake at the lateral sesamoid ossicle (arrow); the concomitantly acquired CT shows a fractured lateral sesamoid
MRI offers little in the direct evaluation of sesamoid pathology, but may be helpful in differentiating sesamoid pathology from other conditions affecting the hallucal sesamoid complex such as plantar plate injury, since it can better delineate soft tissue injuries in this complex region of the foot (Sanders and Rathur 2008; Mohan et al. 2010). Bone SPECT-CT may be helpful in the initial evaluation of turf toe injuries, but MRI is the method of choice in grading the extent of plantar plate injury (Sanders and Rathur 2008).
39.6 Tarsal Coalition
Tarsal coalition is a condition in which there is an abnormal bony or fibrous bridging across two or more tarsal bones, most frequently concerning calcaneonavicular and talocalcaneal fusions. These abnormal connections cause abnormal stress on the hindfoot, resulting in painful deformity of the hindfoot with restricted motion. Due to varying projection angles, plain radiographs may not be sufficient for thorough evaluation of a complex subtarsal coalition, and false-negative and false-positive findings with radiographs can occur (Scharf 2009). MRI and CT are considered to be the gold standard techniques (Newman and Newberg 2000), but are not able to differentiate between asymptomatic and symptomatic joints (De Lima and Mishkin 1996; Scharf 2009). Bone scintigraphy with SPECT-CT is superior to CT alone because of the addition of supplementary functional information, demonstrating the location of the stress forces on this abnormal connection between the bones (Fig. 39.5). This information may be helpful in further decision-making as in guiding intra-articular injections (Mohan et al. 2010).
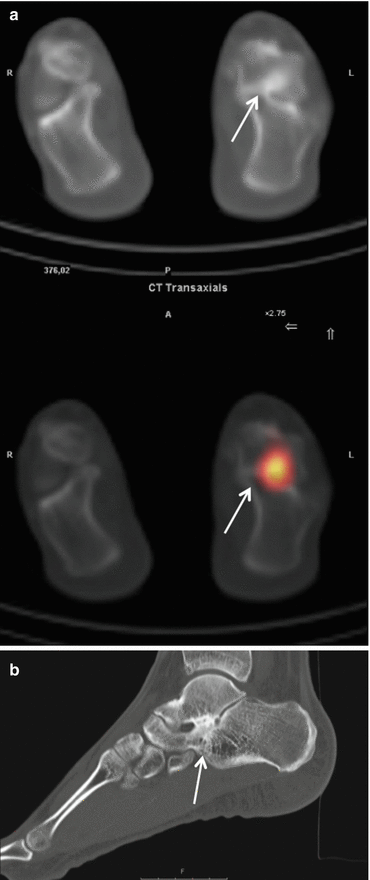

Fig. 39.5
Transverse SPECT-CT images of both feet (a) and sagittal high-resolution CT image (b) of the left foot of a 31-year-old male who complained of persistent pain in the left foot and heel. Plain radiographs showed mild degenerative abnormalities in the talonavicular joint (not shown). SPECT-CT reveals the presence of a bony coalition between the talar and calcaneal bone and also a bony coalition between the calcaneal and navicular bone, which was confirmed with high-resolution CT. The focally increased tracer uptake on the SPECT-CT images (arrow) demonstrates the location of the stress forces on this abnormal connection between these bones
39.7 Stress Fractures
Stress fractures in athletes concern fatigue fractures caused by unusual, repeated physical activity, which initiates focal bone remodeling and results in failure of the bone. Stress fractures can be classified as at-risk or less critical fractures according to their location and relative importance in clinical treatment (McBryde 1995). Most stress fractures in the foot are found in the metatarsal bones. Less common are the tarsal navicular bone, talar body (Rossi and Dragoni 2005), calcaneus, and sesamoids. Especially fractures of the navicular bone and second and fifth metatarsals require additional treatment because of tendency to develop delayed union or nonunion. In the majority of stress fractures, there is no obvious abnormality on plain radiographs because of the lack of dislocation. Bone scan and MRI have demonstrated high sensitivity in identifying early stress injury (Rupani et al. 1985; Ammann and Matheson 1991; Sijbrandij et al. 2002). The three-phase bone scan shows focal hyperemia, increased soft tissue uptake, and a sharply delineated focal area of increased uptake in the involved bone in an early stage of accelerated remodeling (Fig. 39.6). SPECT-CT is helpful in locating the injury and to distinguish a stress reaction from a stress fracture (Brukner and Bennell 1997). The role of SPECT-CT could become even more prominent since it has been suggested that the earliest finding of abnormal repetitive stress may be osteopenia, which can only be demonstrated by high-resolution CT imaging (Gaeta et al. 2005).