Children with neuromuscular disorders have primarily ventilation rather than oxygenation impairment as a result of inspiratory muscle insufficiency. When the respiratory muscles are not assisted, this leads to hypercapnic ventilatory failure or acute respiratory failure mostly owing to ineffective cough during otherwise benign upper respiratory tract infections. Most patients with Duchenne muscular dystrophy (DMD), infantile spinal muscular atrophy (SMA), and other pediatric neuromuscular diseases die prematurely because of failure to use respiratory muscle aids. In large part for this reason, respiratory failure continues to be the most common cause of death for children with severe myopathies, anterior horn cell disorders, and high-level spinal cord injury. The use of inspiratory and expiratory muscle aids can prevent or reverse ventilatory failure, preserve quality of life, and prolong survival for most of these patients. This chapter briefly reviews clinical physiology, presents a diagnostic approach to these diseases, describes some common clinical entities, and concludes with a discussion of the prevention of respiratory failure caused by neuromuscular disease.
Physiology
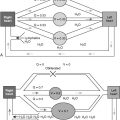
The three basic components of the respiratory control system are as follows: (1) sensors , which gather afferent information and feed it to (2) a central controller in the brain, which processes afferent information and sends efferent impulses to the (3) effectors (respiratory muscles), which cause ventilation or cough.
The afferent information for ventilation comes from central chemoreceptors located in the medulla, carotid and aortic bodies, and stretch receptors in the lungs. The brainstem is the primary center for the central control of respiratory muscle activity. This control occurs at a subconscious level. The cortex can temporarily override the automatic nature of this mechanism if voluntary control is desired.
For the central commands controlling respiration to operate the ventilatory mechanism, the motor units of the respiratory muscles also must be functioning properly. A motor unit consists of an anterior horn cell, its peripheral nerve axon, the neuromuscular junction, and the muscle fibers it innervates. Normally, when an anterior horn cell fires, the peripheral nerve causes the release of acetylcholine at the terminal axon. Acetylcholine diffuses across the neuromuscular junction, where it binds to receptors on the postjunctional membrane and opens channels for the passage of calcium and sodium ions. The ion influx depolarizes the muscle membrane, which triggers contraction of the myofibrils. Neuromuscular diseases are caused by disorders of the anterior horn cells, peripheral motor nerves, myoneural junction, and muscle fibers.
The muscles of respiration include four groups: the diaphragm, the chest wall muscles, the abdominal muscles, and the muscles of the upper airway (bulbar-innervated). The diaphragm is the principal muscle of inspiration. The phrenic nerves from cervical segments 3, 4, and 5 supply it. The chest wall muscles consist of the internal and external intercostals (T1-T12); the parasternal intercostals (T1-T12); the scalenes (C4-C8); and the accessory inspiratory muscles, including the sternocleidomastoids (cranial nerve XI, C1-C2), trapezoids (cranial nerve XI, C2-C3), and pectoralis major (C5-C7). The abdominal respiratory muscles include the rectus and transverse abdominis and the external and internal obliques (T7-L1). They are the most important muscles of expiration.
The muscles of the upper airway include the muscles of the mouth (cranial nerves IX and X), uvula and palate (XI), tongue (IX and XII), and larynx (C1). Although these muscles do not have a direct action on the chest, they are essential for keeping the upper airway patent, and they affect airway resistance and airflow.
During normal respiration, the most important muscles for breathing in addition to the diaphragm are the parasternal intercostals. Postural muscles such as the external and internal intercostals and the accessory muscles such as scalenes and sternocleidomastoids affect breathing significantly only at high rates of ventilation. Expiration is passive during quiet breathing. The lungs and chest wall are elastic and tend to return to their equilibrium positions after being actively expanded during inspiration. The abdominal muscles are not used during quiet expiration to functional residual capacity. These muscles are contracted during forceful exhalation that deflates lungs to residual volume.
Assessment of Respiratory Muscle Function
Clinical Evaluation
Clinical and laboratory evaluation of the chest wall can provide essential information with regard to chest wall function in a particular patient ( Table 9-1 ). The chest wall configuration and pattern of spontaneous breathing, including rate and amplitude of breathing, thoracic or abdominal breathing, coordinated or paradoxical thoracic and abdominal expansion, maximal variation in chest circumference, maximal diaphragmatic excursion during inspiration, and cough effectiveness, are evaluated.
| Clinical Evaluation |
|
| Laboratory Evaluation |
|
Careful bedside observation of an at-risk patient usually allows the recognition of clinical signs and symptoms indicating progressive respiratory muscle fatigue. These signs and symptoms include loss of nonbreathing functions of the respiratory system, increased respiratory rate, and pattern of breathing, and other warning signs ( Table 9-2 ).
|
For an infant and small child, inspection is the most important, and usually the only, evaluation tool that is necessary. The normal movement of chest and abdominal wall is directed outward during inspiration. Inward motion of the chest wall during inspiration is called “paradoxical breathing.” This motion is seen when the thoracic cage loses its stability and becomes distorted by the action of the diaphragm. Most infants who present with neuromuscular conditions have paradoxical breathing with a seesaw type of thoracoabdominal motion owing to severe intercostal muscle weakness. This is true for all children with SMA type 1 and about 40% with SMA type 2 and for many with severe congenital myopathies and muscular dystrophy.
Respiratory rate is important to monitor. As the work of breathing increases, the patient may opt to use less force per breath, reducing tidal volume with shallow breaths and compensating by taking more breaths per minute to avoid fatigue. A very rapid breathing rate cannot be sustained indefinitely, however, and can lead to respiratory muscle exhaustion. The pattern and regularity of breathing also are helpful to observe for risk of fatigue. Breathing that becomes increasingly more rapid and shallow and is interrupted by a deep breath with a brief pause to rest the muscles can be a sign of fatigue for certain patients with central nervous system disorders. Although pauses are normal in healthy children, they can signal respiratory distress, as does nasal flaring, nocturnal flushing, and perspiration. Cyanotic spells or cyanosis with brief cough or brief pause, sustained paradoxical thoracic/abdominal movement, drooling in the absence of airway obstruction (cannot pause to swallow), and confusion also can be signs of impending respiratory arrest.
Laboratory Evaluation
Longitudinal evaluation of lung function should be obtained in patients older than 6 years of age. Measurements of lung function include forced spirometry, static lung volumes, end-tidal carbon dioxide (CO 2 ), and oximetry. Measuring maximal inspiratory and expiratory pressures at the mouth also can assess respiratory muscle strength, whereas cough efficacy can be evaluated by measuring peak cough flows (PCFs) using a simple peak flowmeter.
The forced vital capacity (FVC) should be measured in the sitting position. If FVC is less than 80%, it should be measured again in the supine position to investigate for diaphragm weakness. A greater than 20% decrease in FVC when going from sitting to supine indicates diaphragm weakness out of proportion to chest wall muscle weakness. Although FVC less than 60% indicates a low risk for nocturnal hypoventilation, FVC less than 40% or diaphragm weakness indicates a significant risk for nocturnal hypoventilation. Continuous overnight pulse oximetry and end-tidal or transcutaneous CO 2 should be obtained annually in children too young to perform the FVC maneuver or when FVC is less than 60%, or more often when FVC is less than 40%.
Full overnight polysomnography should be obtained when overnight pulse oximetry is not diagnostic in the presence of symptoms suggestive of hypoventilation or sleep-disordered breathing, and a trial of nocturnal noninvasive ventilation (NIV) is clearly warranted. Polysomnograms are programmed to interpret all abnormalities as being due to central/obstructive apneas and not due to respiratory muscle weakness. For these patients, this is similar to “blaming the brain and throat for what the diaphragm cannot do.” It too often results in patients being prescribed continuous positive airway pressure or bilevel positive airway pressure (BiPAP) at inappropriately low spans, rather than sufficient pressure or volume support to correct hypoventilation and rest inspiratory muscles more fully. A nocturnal desaturation pattern, often a smooth one, may indicate alveolar hypoventilation. When the patient has a respiratory tract infection, a sudden nocturnal or diurnal severe desaturation usually indicates mucous plugging.
Arterial blood gases are not routinely needed because of the adequacy of end-tidal CO 2 /transcutaneous CO 2 measurement. Pulse oximetry should be reserved for intensive care management only.
PCF also should be measured annually during a steady state and at any episode of respiratory infection; values less than 160 to 200 L/min may indicate that cough is ineffective and may place patients at risk for recurrent respiratory infections and respiratory failure. The assisted PCF–unassisted PCF difference also is an excellent measure of glottic integrity.
Spirometry is equally important for the measurement of maximum insufflation capacity (MIC). The MIC is the measure of the maximum volume of air that the glottis can hold in the lungs by “air stacking” volumes of air consecutively delivered from a volume-cycled ventilator or manual resuscitator. The MIC–vital capacity difference is a direct function of glottic integrity and an objective measure of bulbar-innervated muscle function. Unassisted PCFs are measured. Then the patient air stacks as deeply as possible, and an abdominal thrust is applied, timed to the glottic opening of a cough effort.
Other qualitative and quantitative measures of respiratory muscle function can be obtained, although they are rarely needed (see Table 9-1 ). These include electromyographic studies of various respiratory muscles, chest radiographs in supine position, and real-time ultrasonography. Chest radiographs are useful for diagnosing pneumonia and gross atelectasis, but they lag behind oximetry as an indication of these problems (see later). Diaphragmatic strength also can be invasively assessed by measuring transdiaphragmatic pressure and by using a manometer for measuring maximum inspiratory and expiratory pressures at the mouth. The measurement of maximum voluntary ventilation, when possible, can be helpful in determining respiratory muscle endurance. The most important and practical measures continue to be spirometry for FVC and MIC, peak flowmeter for unassisted and assisted PCFs, end-tidal CO 2 , and pulse oximetry. The last two also are useful for nocturnal monitoring because they relate to inspiratory muscle dysfunction.
Clinical Manifestations of Respiratory Muscle Fatigue
Acute respiratory muscle fatigue is characterized by exhaustion leading within minutes or hours to respiratory failure. Chronic fatigue is not as easily identified. Symptoms of chronic fatigue are often subtle, and the diagnosis is frequently missed unless specifically considered. Infants with severe neuromuscular disorders often present with tachypnea, nocturnal flushing, profuse perspiration, and frequent arousals. After 6 months of age, these infants develop otherwise benign respiratory tract infections that result in airway mucous plugging because of their ineffective cough. This mucous plugging causes decreases in oxyhemoglobin saturation (Sa o 2 ) to less than 95%, which, if not quickly reversed by effective assisted coughing, results in pneumonia and respiratory failure with persistent hypoxemia.
In older children, symptoms and signs of chronic respiratory insufficiency include general fatigue and dyspnea on exertion. The first manifestations of chronic respiratory muscle impairment often are symptoms of sleep hypoventilation, however, either nocturnal (frequent nightmares, enuresis, perspiration, frequent awakenings) or daytime symptoms (morning headaches, hypersomnolence, chronic fatigue, impaired concentration, dyspnea, tachycardia, difficulty awakening in the morning, right ventricular failure, peripheral edema, irritability, polycythemia, impaired cognition, anxiety, depression, weight changes, muscle aches, memory impairment), and poor control of upper airway secretions and exacerbation of swallowing difficulties. Often, because many of these patients are wheelchair-bound and inactive, only fatigue, anxiety, and sleeplessness are noted. Small children exhibit increased paradoxical breathing and tachypnea and nasal flaring, and appear distressed.
Neurologic versus Muscular Disease
Some neuromuscular diseases include upper motor neuron involvement. Upper motor neuron lesions result from pathology in the cerebral cortex, brainstem, or spinal cord and are signaled by an increase in muscle tone (spasticity), hyperreflexia, and the persistence or reappearance of primitive reflexes, such as the extensor plantar response (Babinski sign). These patients also may have reflex deep breaths (“sighs”) and coughs despite having very low vital capacity and PCFs. Lesions above the foramen magnum also may produce contralateral hemiplegia. Lesions in the cortex or subcortical areas often are associated with disorders of speech or other cortical functions. Lesions in the brainstem usually affect cranial nerve function ipsilateral to the lesion and contralateral hemiplegia. Abnormalities in the spinal cord typically cause bilateral weakness because of the close proximity of the descending tracts. Upper motor neuron disorders can be identified and differentiated further by imaging studies such as computed tomography, magnetic resonance imaging, and myelography.
The lower motor neuron system includes the anterior horn cell, the peripheral nerve, the neuromuscular junction, and muscle. Manifestations of lower motor neuron involvement include flaccidity, depressed reflexes, fasciculations, and muscle atrophy. Anterior horn cell diseases cause distal weakness without sensory symptoms, whereas disorders of peripheral nerves are almost always accompanied by sensory loss secondary to the involvement of sensory nerves, hyporeflexia, and usually distal weakness. Peripheral nerve weakness can result from damage to either the core axon (axon neuropathies) or the myelin sheath that coats the nerve (demyelinating neuropathies). Disorders of the neuromuscular junction are characterized by fluctuating weakness and frequently involve the extraocular and bulbar-innervated muscles. Sensory symptoms are lacking.
Muscle disorders usually manifest with proximal weakness manifested by inability to rise from a chair or to comb the hair. Sensory symptoms are absent, and reflexes are usually decreased. Serum levels of creatine kinase are frequently elevated. Electrodiagnostic testing may be used to differentiate between anterior horn cell disorders, peripheral neuropathies, neuromuscular junction disorders, and muscle diseases.
Clinical Entities
Table 9-3 lists causes of respiratory muscle dysfunction.
| SITE OF DEFECT | CAUSES |
|---|---|
| Central Drive of Breathing | Congenital or acquired |
| Upper Motor Neuron | Hemiplegia |
| Cerebral palsy | |
| Quadriplegia | |
| Lower Motor Neuron | Poliomyelitis |
| Spinal muscular atrophies | |
| Guillain-Barré syndrome | |
| Tetanus | |
| Friedreich’s ataxia | |
| Traumatic nerve lesions | |
| Phrenic nerve paralysis | |
| Neuromuscular Junction | Myasthenia gravis |
| Congenital myasthenic syndromes | |
| Botulism | |
| Drugs | |
| Respiratory Muscles | Muscular dystrophies |
| Congenital myopathies | |
| Metabolic myopathies | |
| Steroid myopathy | |
| Connective tissue disease | |
| Diaphragmatic malformation | |
| Nonmuscular, Chest Wall Structures | Scoliosis |
| Congenital rib cage abnormality | |
| Overinflated rib cage | |
| Connective tissue disease | |
| Thoracic burns | |
| Obesity | |
| Giant exomphalos |
Upper Motor Neuron
Quadriplegia and respiratory compromise can result from acute cervical spinal cord trauma, spinal artery infarction, or compression by tumor. Injuries at or above C3 to C5 involve the phrenic nerves and can cause partial to complete bilateral hemidiaphragmatic paralysis. Intercostal muscle paralysis below the level of the lesion limits the normal outward expansion of the middle and upper rib cage, compromising inspiration further. Expiration also can be reduced because of paralysis of the abdominal and other expiratory muscles. High-level quadriplegics may be unable to generate adequate tidal volumes, and the accompanying hypoventilation and atelectasis can result in hypoxemia. Low-level cervical quadriplegics with intact phrenic nerves are able to contract their diaphragms. They, too, lack the intercostal muscle activity necessary to stabilize the rib cage for optimal inspiratory function, however. These patients also may lose the use of the abdominal and other expiratory muscles. Combined inspiratory and expiratory weakness can prevent them from effectively coughing and clearing secretions and place them at high risk for pneumonia. Initially, with spinal cord injury, the vital capacity, maximum inspiratory pressure, and maximum expiratory pressure are reduced. As the initial phase of spinal injury passes, chest wall flaccidity is replaced with spasticity, and there is an improvement in the vital capacity as the more rigid chest wall resists collapse.
Anterior Horn Cell Disorders
SMAs comprise a group of autosomal-recessive degenerative disorders of lower motor neurons classified as type I (Werdnig-Hoffman disease), type II, and type III (Kugelberg-Welander disease), based on the age of onset of muscle weakness and clinical severity. These disorders often manifest in infancy and childhood with an estimated incidence of 1:5000. SMAs are due to a mutation of the survival motor neuron gene located on chromosome 5q13. This mutation is responsible for primary degeneration of the anterior horn cells of the spinal cord and often of the bulbar motor nuclei, which leads to skeletal muscle paralysis and atrophy.
Werdnig-Hoffman disease manifests in the first 6 months of life. Infants with this disease lack head control and are nearly always unable to sit and walk. There is severe hypotonia, generalized weakness, and thin muscle mass. All of these patients have paradoxical inward rib cage movement with each inspiration, the diaphragm being relatively spared. Unless provided with nocturnal high-span BiPAP, they develop pectus excavatum and severe undergrowth of the lungs and chest wall, showing on chest radiography reduced lung volume and a bell-shaped thorax. Unless supported by respiratory muscle aids (described later), more than 90% of patients die by 2 years of age.
In SMA type 2, affected patients are usually able to suck and swallow, and respiration is adequate in early infancy. Swallowing difficulties or choking with feeds becomes apparent in the preschool years, predisposing these patients to recurrent pneumonia and chronic suppurative lung disease. These patients can sit but not walk. About 40% of these patients have paradoxical breathing and require nocturnal high-span BiPAP.
Kugelberg-Welander disease is the mildest SMA (type 3), and patients may appear normal in infancy. The progressive weakness is proximal in distribution, particularly involving shoulder girdle muscles. In the adult-onset form, SMA type 4, patients can walk for some period of time. An X-linked adult-onset type 5 SMA (which affects only men), otherwise known as Kennedy disease, is associated with gynecomastia, temporal atrophy, and endocrine disturbances and hypospermia.
Preliminary data obtained from phase 1 human studies have suggested that sodium valproate may improve anterior horn cell function in SMA. Pharmacologic therapy or gene therapy is unlikely to have a major effect on the course of the disease in older patients with advanced disease, but NIV is effective in many of these patients and may buy time for medical therapies to take effect or even undergo development.
Poliomyelitis is a poliovirus infection of young children that begins with fever and upper respiratory symptoms that are followed by signs of meningeal irritation and asymmetric, flaccid paralysis that can involve the skeletal, respiratory, and bulbar-innervated musculature. The respiratory motor nuclei can be directly involved, resulting in diaphragmatic and accessory respiratory muscle dysfunction. Involvement of lower cranial nerve nuclei can result in upper airway obstruction, pooling of secretions, and aspiration. The medullary respiratory center also can be affected, resulting in irregular respirations and apnea. Many of these patients require ventilatory and hemodynamic support during the acute phase of the illness. Although most patients show substantial muscle recovery over time, they gradually relapse to require ventilatory assistance again later in life with the senescent aging and dropping out of overworked anterior motor neurons with aging.
Disorders of Peripheral Nerves
Hereditary motor and sensorimotor neuropathies are common. The former is often confused with and can be as severe as SMA. The most common is Charcot-Marie-Tooth disease, a demyelinating neuropathy. Almost 15% of patients are left with residual weakness, and an additional 5% experience chronic relapsing (dysimmune) polyneuropathy. Some patients are never weaned from ventilatory support.
Acute idiopathic polyradiculitis, also known as Guillain-Barré syndrome, is the most common peripheral neuropathy causing respiratory failure. It is considered to be an autoimmune disease precipitated by a preceding viral or bacterial infection, such as cytomegalovirus, Epstein-Barr virus, Mycoplasma pneumoniae , and Campylobacter jejuni . In 80% of these patients, there is a history of a nonspecific viral illness preceding weakness by 2 to 3 weeks. Diagnosis is mainly based on clinical grounds. It usually begins with fine paresthesias in the toes or fingertips followed by progressive muscle weakness in the lower extremities, trunk, upper limbs, and, finally, bulbar-innervated and respiratory muscles. Muscle involvement is relatively symmetric. Facial and oropharyngeal weakness are often impending signs of respiratory failure. Muscle pain is common in the initial stages. Daily bedside evaluation of vital capacity and arterial blood gases is essential for appropriate decisions regarding the need of mechanical ventilatory support, which is required in 20% of affected children. Acute respiratory failure can be avoided with the use of noninvasive aids when bulbar-innervated muscle function is adequate to prevent continuous aspiration of saliva or oxyhemoglobin desaturation. Otherwise, patients need to be intubated for ventilator use and airway secretion management. Early use of high-dose intravenous immunoglobulins or plasma exchange induces a more rapid resolution of the disease. Corticosteroids are now used sparingly because they seem to predispose to the chronic relapsing form of the disease.
Among other peripheral neuropathies leading to respiratory failure, Lyme disease can manifest with a syndrome identical to Guillain-Barré syndrome. In endemic areas, serologic testing for Lyme disease is indicated. Acute intermittent porphyria can cause a neuropathy severe enough to result in respiratory failure. Postdiphtheritic neuropathy, toxic neuropathies (thallium, phosphate, and lead) avitaminosis, paralytic shellfish (saxitoxin) poisoning, and the polyneuropathies associated with systemic lupus erythematosus and polyarteritis nodosa also can cause ventilatory failure.
Disorders of the Neuromuscular Junction
Myasthenia gravis is the most common disorder of the neuromuscular junction. It affects any age group, although clusters of cases are found in adolescent girls. Myasthenia gravis is characterized by fluctuating weakness with a predilection for the ocular muscles (ptosis, diplopia, blurred vision) and bulbar-innervated muscles (dysphagia, dysphasia, and aspiration). The pupillary response to light is preserved. Similar to the adult form, juvenile myasthenia gravis is an acquired immunologic disorder of neuromuscular transmission associated with circulating antibodies against postsynaptic acetylcholine receptors. These antibodies can be detected in the serum of 90% of patients with generalized myasthenia gravis.
Diagnosis of juvenile myasthenia gravis is based on clinical symptoms, electrophysiologic studies, a positive finding of circulating acetylcholine receptor autoantibodies, and transient improvement with anticholinesterase medication. Most patients in whom this disease is suspected but undiagnosed show a dramatic response to intravenous edrophonium chloride, a short-acting acetylcholinesterase inhibitor. Benign thymic hyperplasia or thymoma occurs in 90% of these patients. Management is primarily based on anticholinesterase medication (pyridostigmine bromide). Improvement with anticholinesterase medication is often incomplete, however, and most patients require further therapeutic measures, including thymectomy, which results in improvement or remission in 80% of patients without thymomas. Immunosuppressive drugs (prednisone, azathioprine, or cyclosporine) are frequently recommended. Other autoimmune diseases, such as rheumatoid arthritis, systemic lupus erythematosus, and thyrotoxicosis, commonly complicate the clinical picture.
Transient neonatal myasthenia gravis is a syndrome that affects 30% of infants born to mothers with autoimmune myasthenia gravis. Clinical features are usually noted within hours of birth and include feeding and respiratory difficulties, hypotonia, weak cry, facial weakness, and palpebral ptosis. Respiratory difficulties are related to feeding problems causing aspiration pneumonia, upper airway obstruction owing to inability to handle oropharyngeal secretions, or respiratory muscle weakness. Some patients may require ventilatory support during this period. After the abnormal antibodies disappear, the infants have normal strength and are not at increased risk for developing myasthenia gravis in later childhood. The syndrome of transient neonatal myasthenia gravis is to be distinguished from a rare, often hereditary, and often permanent, congenital myasthenia gravis not related to maternal myasthenia gravis. This disorder is characterized by an abnormality of the acetylcholine receptor, manifested as high conductance and excessively fast closure, and is probably due to a mutation affecting a single amino acid residue. Therapy for acute attacks (myasthenia crisis) includes mechanical ventilation in combination with plasma exchange, acetylcholinesterase inhibitors (pyridostigmine), and corticosteroids or other immunosuppressants.
Botulism is a rare disorder of the neuromuscular transmission blockade caused by the binding of one of the neurotoxins (A, B, E, and F) produced by Clostridium botulinum . The toxin that is carried in the bloodstream prevents the release of acetylcholine from the presynaptic terminal and affects nicotinic and muscarinic synapses. Botulism occurs in three forms: infantile botulism, the most common, in which the organism and its spores are ingested in honey or other foods, or from the environment; food-borne (classic) botulism, in which preformed toxin is ingested in nonacidic home-canned or factory-canned vegetables or meat; and wound botulism (very rare), in which C. botulinum and its spores contaminate traumatic or surgical wounds.
Infant botulism is most commonly seen in the first 4 months of life. Constipation is usually the first symptom; thereafter, neuromuscular dysfunction results in progressive descending muscle weakness, with early bulbar involvement and hypotonia. Acute respiratory failure develops in 90% of affected infants. Respiratory failure results from respiratory muscle weakness and paralysis, causing hypoventilation; bulbar palsy and upper airway muscle weakness, leading to aspiration pneumonia or upper airway obstruction; and inability to clear secretions, resulting in pneumonia and atelectasis. Endotracheal intubation is performed as soon as depression of the gag reflex is noted.
In older children with food-borne or wound botulism, the onset of neurologic symptoms follows a characteristic pattern of diplopia, blurred vision, ptosis, dry mouth, dysphagia, dysarthria, decreased gag reflex, and decreased corneal reflex followed by flaccid descending paralysis that often progresses to affect the respiratory muscles. The diagnosis should be considered if a previously healthy infant, usually younger than 6 months, has a history of constipation and then acutely develops weakness with difficulty in sucking, swallowing, crying, or breathing. It is suggested by electromyographic changes of brief, small, abundant motor unit potentials in response to high rates of stimulation similar to that seen in aminoglycoside toxicity. The diagnosis is confirmed by showing neurotoxin in the serum, stool, or contaminated food. Treatment includes positioning the head backward to open the airway and improve respiratory mechanics. Respiratory muscle aids are often required, and pneumonia is a common complication and a major cause of death. Antibiotic therapy is not part of the treatment of uncomplicated infantile or food-borne botulism because the toxin is primarily an intracellular molecule. Antibiotics are reserved for the treatment of complications. Wound botulism requires aggressive use of antibiotics and antitoxin.
The neuromuscular junction is perhaps the most common site adversely affected in drug-induced neuropathies. Several drugs have been reported to produce or potentiate unwanted neuromuscular blockade, including aminoglycosides, clindamycin, polymyxin, colistin, propranolol, calcium channel blockers, quinidine, lidocaine, corticosteroids, chlorpromazine, and lithium.
Disorders of Muscles
DMD is the most common and severe of the muscular dystrophies that affect humans. Inherited as an X-linked recessive trait, it has an estimated incidence of 1:3000 male births. The gene responsible for DMD and Becker muscular dystrophy has been localized on the short arm of the X chromosome (Xp21). The dystrophin gene regulates the expression of dystrophin, a protein that links the normal contractile apparatus to the sarcolemma in skeletal muscle. DMD usually manifests in boys with proximal muscle weakness at 2 to 4 years of age. Poor head control in infancy may be an early sign of weakness. Clinical diagnosis is made after consideration of history, physical findings, and elevated serum creatine kinase level. Diagnosis is confirmed by finding an abnormality in the dystrophin gene by mutation analysis of blood leukocyte DNA. By inducing specific exon skipping during messenger RNA splicing, antisense compounds were shown to correct the open reading frame of the DMD gene and to restore dystrophin expression in vitro and in animal models in vivo .
Respiratory disease in DMD is the major cause of morbidity and mortality. Loss of lung function progresses linearly after the initiation of wheelchair use; increasing hypoxemic dips are seen during sleep in subsequent teenage years, and respiratory failure occurs between 18 and 20 years of age. Unless properly managed with respiratory muscle aids, these patients invariably die before age 30. The deterioration in pulmonary function in DMD parallels the progression of the disease. A FVC of less than 1 L is a predictor of poor outcome, with a 5-year survival rate of only 8% if assisted ventilation is not provided. Death is due to respiratory failure in 80% of cases or to cardiac failure in 10% to 20% of cases.
A restrictive syndrome secondary to muscle weakness characterizes the pulmonary compromise in patients with DMD. When daytime hypercapnia develops in DMD patients, life expectancy without noninvasive ventilatory assistance is approximately 9 to 10 months. Chest wall muscle weakness and contractures, spinal deformity, and vertebrocostal ankylosis also occur. When assisted PCF decreases to less than 300 L/min, a pulse oximeter and Cough-Assist TM (JH Emerson Company, Cambridge, MA) are prescribed for the oximetry protocol as described subsequently. Patients with DMD eventually require 24-hour use of noninvasive inspiratory muscle aids, but can live well into their 40s using them.
Congenital myotonic dystrophy is the second most common muscular dystrophy. Myotonic dystrophy is an autosomal dominant inherited disease that occurs with an estimated frequency of 1:7500 to 1:18,500. The mutation responsible is an expansion of trinucleotide (CTG) repeats in the region of the myotonic dystrophy protein kinase ( DMPK ) gene, on the long arm of chromosome 19. Myotonia, a very slow relaxation of muscle after contraction, and muscle weakness are the prominent clinical features, but many organ systems can be affected, including the cardiac, endocrine, and ophthalmologic systems. Involvement of the respiratory system is the major contributor to morbidity and mortality.
Neonatal myotonic dystrophy is a severe form of myotonic dystrophy that develops in a few infants born to mothers, and rarely to fathers, with myotonic dystrophy. Prominent manifestations include hypotonia without myotonia, feeding difficulties, and respiratory distress. Respiratory failure is common and may result in death in the neonatal period. Examining the parents and finding the repeat segment of DNA on the myotonic dystrophy gene can confirm the diagnosis. Polyhydramnios and decreased fetal movements are common. Prematurity, hydrops fetalis with pleural effusions, and pulmonary hypoplasia can increase respiratory difficulties owing to diaphragmatic weakness at birth. Fifty percent of neonates with congenital myotonic dystrophy need respiratory support at birth.
The diagnosis of this disease is suspected when the newborn is recognized to be difficult to wean from the ventilator for unknown reasons. Thin ribs and an elevated right diaphragm on the chest radiograph may hint at the diagnosis. The breathing pattern of these patients is similar to that of any patient with a restrictive syndrome secondary to respiratory muscle weakness—increased rate with small tidal volumes at rest. Myotonia and weakness of the respiratory muscles and the muscles of deglutition, decreased ventilatory drive, and failure of myotonic muscles to benefit from inspiratory muscle support (ventilatory assistance) make these patients very prone to chronic hypoventilation and cor pulmonale.
Sleep Evaluation in Neuromuscular Diseases
Neuromuscular diseases are frequently associated with sleep-disordered breathing and alveolar hypoventilation. Onset of respiratory insufficiency can be subtle. Symptoms of sleep hypoventilation include gradually increasing headache, somnolence, and, rarely, vomiting. Patients with some neuromuscular disorders also are at risk for upper airway obstruction.
Children with DMD may go through an early phase of latent or occult nocturnal hypoxemia before there is evidence of daytime respiratory impairment. Such episodes of hypoxemia can result in a disrupted sleep pattern and impair daytime cognitive performance. The sleep laboratory is an ideal site to diagnose occult episodes of nocturnal hypoxemia in patients with most types of significant restrictive lung disease.
The timing and necessity of polysomnography to detect sleep hypoventilation have not been determined in patients with neuromuscular disorders. Sleep hypoventilation correlates with an awake PaCO 2 of 45 mm Hg or greater and a base excess 4 mmol/L or greater. Ambulatory monitoring at home with recording of cardiac and respiratory variables has been suggested as the first diagnostic step in testing for sleep-disordered breathing in patients with DMD. These devices can detect the presence of decreases in sleep-related oxyhemoglobin saturation. A negative test result does not rule out the diagnosis of sleep-disordered breathing and must be followed by polysomnography.
It is recommended to review sleep quality and symptoms of sleep-disordered breathing at every patient encounter, and an annual evaluation for sleep-disordered breathing should be obtained in patients with DMD starting from the time they are wheelchair users or when clinically indicated. Overnight pulse oximetry with continuous CO 2 monitoring provides useful information about nighttime gas exchange, although central or obstructive events not associated with desaturation or CO 2 retention would not be detected. A simple capillary blood gas measurement on arousal in the morning can show CO 2 retention, although not as sensitively as continuous capnography.
Cardiac Involvement
Cardiac involvement is universal in individuals with DMD. Cardiac disease is the second most common cause of death in individuals with DMD. Dilated cardiomyopathy primarily involves the left ventricle, and can lead to dyspnea and other symptoms of congestive heart failure. Conversely, right ventricular failure can result from respiratory failure and pulmonary hypertension. Individuals with DMD also are at risk for ventricular arrhythmias. Although some studies have suggested that the respiratory and peripheral muscle weakness tend to be inversely related to the risk of cardiac failure, other studies suggest that left heart and respiratory failure tend to occur in parallel. It is recommended that all individuals with DMD obtain regular cardiac evaluation with annual electrocardiograms and echocardiograms, starting at least by school age.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree