Fig. 23.1
Normal PA wrist radiographs. (a) Ulnar deviation, (b) radial deviation. A normal wrist shows no discontinuity in Gilula lines I, II, and III and neutral, ulnar, and radial deviation. In ulnar-sided wrist deviation, the scaphoid shows its longest diameter (a double-sided long arrow); in radial deviation the scaphoid rotates volarly out of the coronal plane with foreshortened projection on PA view producing a signet ring appearance at its distal half (dotted line); the superposition of the lunate and capitate bone is increased due to solidarity of motion of the scaphoid and lunate bone (b small double arrow)
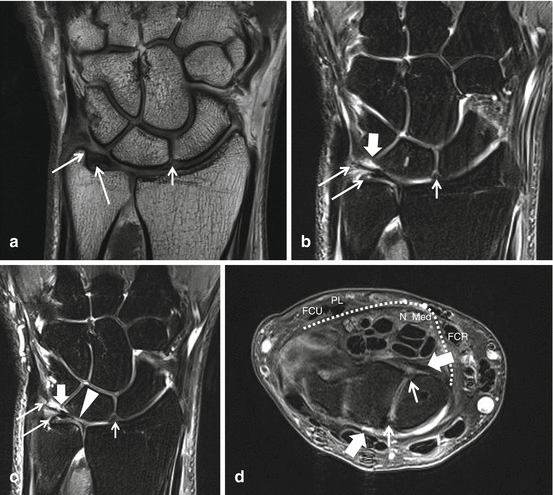
Fig. 23.2
Wrist 3 T MRA images after IV gadolinium administration (indirect arthrography), (a) coronal SE T1, (b) coronal intermediate TE FS, (c) coronal SE T1 FS (d) axial intermediate TE FS at proximal row. Intrinsic SL (small arrow) and LT (thick arrow on (b, c)) ligaments and dorsal and volar components of intrinsic SL ligament demonstrated on axial images only. Intermediate SI connection between the TFC and the low SI bone lamella of the radius is best demonstrated on c. Two ulnar attachments of TFC on coronal images (long arrows) are best demonstrated on b, and c. c shows broad perforation (arrowhead) at the central part of the TFC with minor chondromalacia (increased SI at the cartilage over the distal ulna epiphysis) (palmer type II C). Extrinsic radiocarpal volar and dorsal ligaments (thick arrows on axial image only). At the volar aspect the transverse ligament (dotted line) covering the flexor digitorum profundus and superficialis tendons, the flexor pollicis longus and median nerve is demonstrated. The median nerve (N Med) is located between the flexor carpi radialis tendon (FCR), palmaris longus tendon (PL) and flexor carpi ulnaris tendon (FCU)
23.3 Functional Anatomy
The wrist, hand, and fingers have the most complex human musculoskeletal anatomy. Excellent knowledge of this anatomy and its function is a condition sine qua non for radiological evaluation of wrist and finger pathology.
23.3.1 Bones, Joints, and Ligaments of the Wrist and Hand
The bones consist of the distal radius and ulna, two rows of four carpal bones, metacarpal bones, and proximal, middle, and distal phalanges (Fig. 23.1). The wrist articulations are grouped in functional entities, including: the radiocarpal, distal radioulnar (DRU), pisiform-triquetral, midcarpal, scapho-trapezio-trapezoid (STT), first carpometacarpal (CMC), intermetacarpal, and interphalangeal (IP) joints. The proximal carpal row is starting at the radius or lateral aspect formed by the scaphoid, lunate, triquetrum, and pisiform. At the radiocarpal (RC) joint, this proximal carpal row functions as an integrated entity or ellipsoid ball that articulates with the socket at the distal end of the radius and the TFCC. The radiocarpal joint has a wide multidirectional range of motion. The distal carpal row is formed by the trapezium, trapezoid, capitate, and hamate and articulates with the distal surfaces of the proximal row which is called the midcarpal joint and the proximal surfaces of the metacarpal bones also called the CMC joints. The midcarpal joint has a wide range of motion especially serving flexion and extension and to a lesser range radial and ulnar deviation; the widest range of motion is located at the lateral (radial) aspect or STT joint. The 2nd to 5th CMC joint spaces are gliding joints with very restricted range of motion (ROM) due to the shape of the epiphyseal end plate and due to the fortification by a strong ligamentous apparatus. The CMC 1 is a single joint compartment and functions as a saddle joint providing a multidirectional wide range of motion. The CMC 1 and STT joints are prone to overuse osteoarthritis (OA) related to the wide range of motion. The ulna does not articulate directly with the carpus but does with the distal radius at the DRUJ. The MCP and IP joints are hinge joints with unidirectional movement restricted to flexion and extension due to radial and ulnar collateral ligaments. Extension in these joints is restricted to 180° by the very strong palmar plate that is a ligamentous thickening of the volar capsule in these joints. The carpal bones are held together by ligaments, including the intrinsic (or interosseous) and extrinsic ligaments (Figs. 23.2 and 23.3). These strong ligaments are essential stabilizers of the wrist. The dorsal ligaments are weaker than the volar ligaments, resulting in dorsal dislocation being more common. The intrinsic (or interosseous) ligaments connect pairs of carpal bones and divides the midcarpal and RC joint compartments. In the proximal carpal row, the scapholunate (SL) and lunotriquetral (LT) ligaments join the proximal, dorsal, and volar margins of these carpal bones and separate the RC from the midcarpal compartments. Especially the volar and dorsal parts of these, SL (Fig. 23.4) and LT intrinsic ligaments are essential in the stabilization of the centrally located lunate bone; perforations at the proximal part of these interosseous ligaments have no functional consequence. The dorsal and volar extrinsic ligaments are thickenings of the inner surface of the joint capsule (Fig. 23.4). The main dorsal extrinsic ligaments are the radiotriquetral, triquetrotrapezial, and triquetroscaphoid ligaments. The main volar extrinsic ligaments are the radioscapholunate (RSC) and the radiolunotriquetral (RLT) (long radiolunate) and the short radiolunate ligaments. The TFCC is an important stabilizer of the DRUJ. Its main central component is the TFC disk, which separates the RC compartment from the DRUJ. The low SI on MRI of the TFC disk is attached to the intermediate MRI SI of the hyaline articular cartilage of the ulnar side of the distal radius and connects to the ulnar styloid through two fibrous bands (Fig. 23.2). The intermediate SI on MRI of the hyaline cartilage at the radial junction of the TFC should not be confused with a tear (Fig. 23.2c). The central and radial aspects of the TFC disk are “white” avascular, while the peripheral and ulnar aspects “red” have a blood supply. The latter regions hence have the potential to heal following injury with elongation or tear, either conservatively or after surgical repair (Bednar et al. 1991). Multiple variants of the ulnar adherence of the two ulnar connections are described, located from the top of the ulnar styloid process up to the distal ulnar epiphysis making the radiological evaluation difficult and less accurate; radiologists should carefully search for and recognize two separate ulnar TFC insertions to increase the accuracy of ulnar TFC avulsions (Palmer and Werner 1981; Benjamin et al. 1990; Totterman and Miller 1995). Other components of the TFCC are the dorsal and volar radioulnar ligaments, prestyloid recess, meniscal homologue (a fibrostyloid fold that extends into the prestyloid recess), ulnar collateral ligament, subsynovial sheath of the extensor carpi ulnaris (ECU) tendon sheath, and volar ulnotriquetral and ulnolunate ligaments (Fig. 23.2). The DRUJ consists of an articular surface that covers two-thirds of the circumference of the distal ulnar epiphysis, which in turn articulates with the sigmoid notch of the distal radius (Fig. 23.5). The DRUJ is a pivot joint with unidirectional movement providing rotation only of the radius around the ulna; this is the distal component of supination and pronation movement of the forearm. The DRUJ is stabilized intrinsically by the TFCC and extrinsically by the interosseous membrane, extensor carpi radialis (ECR) and flexor carpi ulnaris (FCU) tendons, and the pronator quadratus muscle.
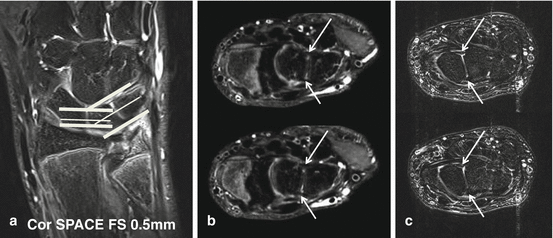
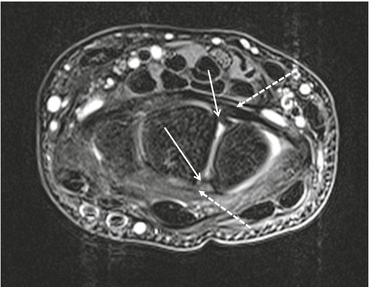
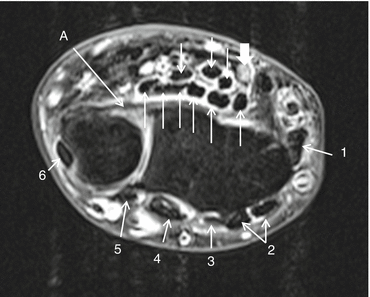

Fig. 23.3
MR demonstration of volar and dorsal components of the LT (b) and SL (c) intrinsic ligament. (a) Native coronal image, 3D TSE (SPACE, Siemens) intermediary TE FS, thin slice (0.5 mm), demonstrating oblique axial reconstruction plane perpendicular to the articular surface at the LT compartment of the midcarpal joint (b) and axial imaging plane perpendicular to the SL compartment of the midcarpal joint on TSE intermediary TE FS images (C). Arrows point to the dorsal and volar intrinsic ligament components. (b) Oblique axial multiplanar reconstruction with 0.5 mm slice thickness. (c) Axial TSE intermediary TE with FS images

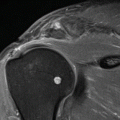
Fig. 23.4
MRI normal SL ligament. Axial TSE intermediary TE MRI at the level of the proximal carpal row. Low SI dorsal and volar functional important components of the intrinsic SL ligament (arrows) connecting the lunate and scaphoid bones are demonstrated on axial images only, extrinsic dorsal and volar radiocarpal ligaments (dotted arrows)

Fig. 23.5
Axial TSE intermediate SE FS at level of DRUJ in pronated joint positioning. Semicircular distal ulna epiphysis (left) fits in the distal radial epiphysis sigmoid notch (right); the volar radioulnar ligament is stretched and demonstrated as a low signal band connecting the radius and ulna (arrow A). Dorsal compartments numbered 1–6 (arrows 1–6). Volar flexor digitorum profundus and superficialis tendons with flexor pollicis longus tendons (arrows) and median nerve (thick arrow) proximal to the carpal tunnel
23.3.2 Tendons, Arteries, and Nerves of the Wrist and Hand
The tendons of the hand originate primarily in the forearm and pass over the wrist. The dorsal aspect of the wrist is covered by the extensor retinaculum that covers the extensor tendons and attaches to the distal radius and ulna to divide the extensor aspect in six type II tendon compartments, each containing one or more finger or wrist extensor tendons within a synovial sheath (Fig. 23.3). The flexor tendon compartment in the volar aspect at the level of the carpus is also called the carpal tunnel. The carpal tunnel is bounded superficially by a strong flexor retinaculum, the transverse carpal ligament (Fig. 23.2d), and contains the nine finger and long thumb flexor tendons, the distal part of the FCR tendon, the median nerve, and the radial artery but not the wrist flexor tendons and ulnar artery. The superficial and deep finger flexor tendons are surrounded by a single compartment synovial sheath at the level of the carpal tunnel; the long thumb flexor is surrounded by an independent synovial sheath at the level of the carpal tunnel up to the level of the distal phalanx. The palmaris longus and FCU tendons are located superficially to the carpal tunnel and not covered by retinaculum; they are type I tendons without synovial sheath (Fig. 23.2d). The flexor carpi radialis tendon (Fig. 23.2d) pierces the flexor retinaculum at its distal half and is therefore surrounded by a synovial sheath; it runs over the volar aspect of the scaphoid, the STT joint, subsequently in a fibro-osseous groove of the trapezium bone and inserts at the base of the second metacarpal bone. The latter tendon and tendon sheath are prone to impingement in this fibro-osseous tunnel related to overuse and STT osteoarthritis with osteophytosis, tenosynovitis, and tendinopathy. Resisted flexion at the carpus nicely demonstrates the FCR and palmaris longus tendons at the skin surface; the level of the median nerve deeply located at the carpal tunnel is between these two tendons (Fig. 23.2d). Blind infiltrations of the carpal tunnel therefore are performed at the ulnar aspect of the palmaris longus tendon to avoid median nerve injury. Guyon’s canal lies superficial to the transverse carpal ligament and radial to the hook of hamate and contains the ulnar nerve, artery, and veins. The ulnar nerve runs deep to the FCU tendon and palmaris brevis muscle in Guyon’s canal. The flexor FCU tendon is surrounded by a synovial sheath and inserts into the pisiform bone; it is the only tendon that inserts into one of the wrist bones. The median nerve splits distal to the carpal tunnel into the palmar common digital nerves of fingers 1–4 (radial aspect of ring finger) and branches to the thenar muscles (except flexor pollicis brevis caput profundus and adductor pollicis) at the level of the carpal tunnel. A bifid median nerve is a variant with split of the median nerve at or proximal to the carpal tunnel, an associated persistent median artery may exist, and these variants are easily detected on ultrasound with Doppler and MRI and have to be described by the radiologist as in these cases blind infiltration of the carpal tunnel may cause injury of the median nerve (Propeck et al. 2000). The ulnar nerve splits into the ramus profundus to the flexor pollicis brevis caput profundus and adductor pollicis of the thenar and hypothenar and ramus superficialis to the palmar and volar common digital nerves for the little finger and ulnar aspect of the marriage finger. The superficial branch of the radial nerve is located at the subcutaneous tissue over the radial aspect of the wrist and distal forearm and branches into the dorsal common thumb and digital nerves of the fingers 2 and 3 and radial aspect of the ring finger. The deep branch of the radial nerve also called the posterior interosseous nerve (PIN) follows the extensor digitorum tendons into the extensor digitorum fibro-osseous tunnel of the wrist together with the extensor indicis proprius tendon (extensor compartment 4) and ends into the dorsal RC joint capsule. Blood supply of the wrist and hand is very variable and complex with anastomosis at multiple levels: volarly its most important supply is via the ulnar artery, and secondary supply is via the radial artery; both arteries anastomose distally in a superficial and deep palmar arc and at the dorsal aspect via the posterior interosseous artery that ends in a dorsal arterial anastomosing network. This dorsal network connects to the deep palmar arc at the radial and ulnar side through dorsal carpal arterial branches. The scaphoid bone receives its blood supply via its distal third through a superficial palmar and dorsal branch part of the radial artery; because of this blood supply, fractures of the middle and proximal third of the scaphoid are prone to AVN. The fingers have four arteries at the four corners: the dorsal digital arteries arise from the dorsal network, the ventral digital arteries from the deep and superficial arc, and the latter anastomose at the level of the distal phalangeal tuft.
23.3.3 Anatomy and Biomechanics of Fingers, Tendons, and Ligaments
The finger joints and MCP joints are hinge joints, with full flexion capacity but extension motion restricted to 180° related to action of the volar plate that is a major thickening of the volar joint capsule. Rather thick radial and ulnar collateral ligaments resist varus or valgus deviation at these joints, the collateral ligaments have a palmar extension, the ligamentum palmaris.
Flexor digitorum superficialis musculotendinous unit (MTU) is responsible for flexion of the PIP joint and inserts on the base of the phalanx media; the flexor digitorum profundus tendon crosses the superficialis tendon at the proximal phalanx and inserts on the phalanx distalis; thus it is responsible for flexion of the DIP joint. Bowstringing of the flexor tendons relative to the phalanges is prevented by specific finger retinacula, the pulley system, annular (A) and cruciate (C) pulleys are located along the phalangeal course of the flexor tendons (Fig. 23.6). The biomechanically important annular pulleys are numbered (1–5) from proximal to distal. The odd annular pulleys (A1–3 and 5) insert on the volar plates of the MCP and IP joints; the even pulleys A2 and A4 insert on the phalanx proximalis and media, respectively; these are the strongest and most important functional pulleys (Fig. 23.6a, b). Pulley lesions are associated with overuse in climbing sports and acute trauma in baseball and in PIP dislocation (Fig. 23.6c).
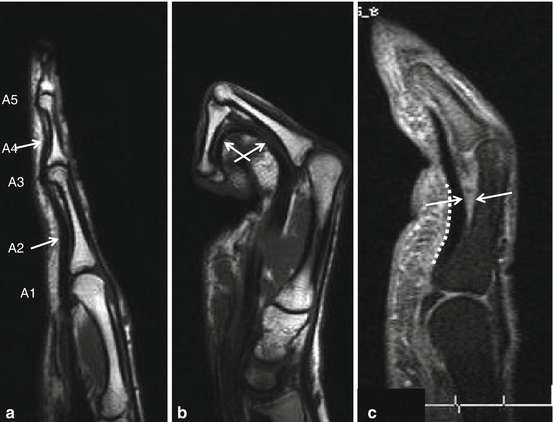

Fig. 23.6
Function of the finger pulleys. Middle finger, sagittal MR T1WI with extension (a) and flexion (b) of the finger. Bowstringing of the flexor tendons during flexion is prohibited by the pulley system on MRI demonstration of contact of the flexor tendons and the phalanx in both finger positions at the level of the A2 (proximal phalanx arrow) and A4 (phalanx media arrow) pulleys. Partial distal A2 pulley lesion (c) with dissociation of flexor tendons and proximal phalanx at the distal third of the A2 pulley after volar PIP dislocation (dotted line: extension of the A2 pulley)
The extensor apparatus of the long fingers is very complex. Extensor digitorum muscle tendons are inserting on the phalanx media 2–5; they are called the central slips and responsible for extension at the PIP joint. At the index an additional MTU, the extensor indicis proprius, is responsible for the independent extension at the PIP; also at the little finger, an additional MTU, the extensor digiti minimi, is responsible for the independent extension at the PIP. The dorsal hood is responsible for extension movement of the DIP joints 2–5; this tendinous structure is formed by the aponeuroses and tendons of the lumbrical muscles and dorsal and volar interossei muscles that run to the dorsal aspect of the phalanx on radial and ulnar side. Proximally at the level of the metacarpal heads, the dorsal hood forms a sling around the central slip; this part is called the sagittal bands; they keep the central slip centered to the central axis of the MCP joint in flexed position. The dorsal hood runs over the phalanx at radial and ulnodorsal aspect and inserts on the distal phalanx, thus responsible for the extension of the DIP joint. Lumbrical muscles with their origin at the flexor digitorum profundus tendons at metacarpal level connect the flexor and extensor apparatus of the fingers and are responsible for the complex action of the finger joints with combined flexion and extension.
At the MCP joint of the thumb, the ulnar collateral ligament is covered by the aponeurosis of the adductor pollicis; this aponeurosis is comparable to the dorsal hood of the long fingers and thus part of the extensor mechanism that forms a sling around the extensor pollicis longus tendon. Thus, the adductor pollicis muscle has a similar action to the interosseous muscles and is consequently called the missing interosseous (Mardel and Underwood 1991). The adductor pollicis tendon has a second, commonly known, insertion on the ulnar sesamoid of the first metacarpal.
23.3.4 Biomechanics of the Wrist and Hand in Sports Injuries
The wrist is a complex intercalated segment that biomechanically transmits forces generated at the hand to the forearm. An important motion component is located at the ellipsoid ball and socket radiocarpal joint; a secondary motion component is located at the midcarpal joint; the only restricted motion is located at the CMC joints 2–5. DRUJ is involved in rotation with pro- and supination. The radial side of the wrist carries 80 % of the axial load, and the ulnar side the remaining 20 %. Radial deviation of the wrist results in ventral angulation of the distal pole of the scaphoid (Fig. 23.1b) producing a round sclerotic circular line on the distal third of the scaphoid producing a signet ring aspect on radiographs; SL ligament causes solidary movement of the lunate with increased superposition of lunate and capitate (Fig. 23.1b small arrow). In neutral position and ulnar deviation, the scaphoid rotates with its long axis in the coronal plane producing the longest projection of the scaphoid on radiographs (Fig. 23.1a long arrow). In SL ligament dysfunction, a lack of solidary motion of scaphoid and lunatum results in a sustained ventral angulated position during ulnar deviation with increased scapholunate distance (SL dissociation) (Fig. 23.7).
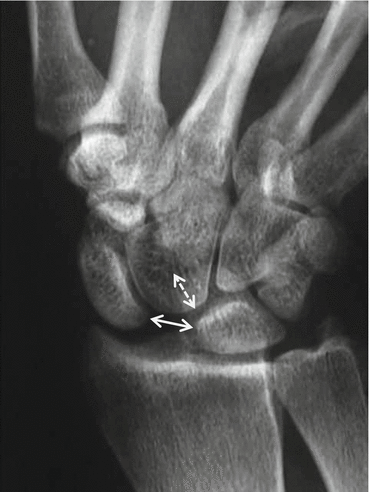

Fig. 23.7
CR in neutral position with clenched wrist demonstrating carpal instability dissociative. CR posteroanterior view with clenched wrist. Late findings with increased scapholunar distance in neutral position (double arrow), increased superposition of lunate and capitate (dotted double arrow): Terry Thomas sign in carpal instability dissociative (CID)
23.4 Fractures
23.4.1 Scaphoid and Distal Radial Fractures
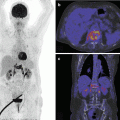
Radial, scaphoid fractures and scapholunar ligament lesions are common in sports, usually occurring during a fall on the pronated outstretched hand (FOOSH). The type of lesion depends on the patient’s age, bone density, reaction time, and the angle at which the wrist hits the ground. The more dorsiflexed the wrist is, the more likely the scaphoid bone will break. With less wrist dorsiflexion, it is more likely that the radius will break. On striking a hard surface, the hand becomes fixed, while the momentum of the body produces two forces: a twisting force causing excessive supination of the forearm and a compression force which acts vertically through the carpus to the radius. The type of fracture is also dependent on whether the hand is in radial or ulnar flexion at the moment of impact. Distal radial fractures are often associated with ulnar fractures. Distal radial fractures may be extra- or intra-articular and displaced or nondisplaced. These fractures are primarily examined radiographically; complex intra-articular fracture components are evaluated with multiplanar or cone beam CT with multiplanar two-dimensional reconstructions in three orthogonal planes and three-dimensional reconstructions. Despite the fact that nondisplaced scaphoid fractures are a radiological challenge and occult fractures are frequent (Fig. 23.8a), radiography with specific scaphoid series remains the first imaging modality in the initial evaluation and follow-up of scaphoid fractures. If clinically suspected for scaphoid fracture, i.e., FOOSH with pain on palpation at the anatomical snuff box and normal radiographs, additional examinations are mandatory, whether repeated radiographs of the scaphoid after 1 week of immobilization, or bone scintigraphy, or MRI with coronal TSE FS T2 or intermediate TE sequence (Fig. 23.8c). Because of its sensitivity, specificity, absence of radiation exposure, and lower cost, MRI without contrast is the imaging modality of choice over nuclear imaging techniques (bone scintigraphy, SPECT-CT) for depiction of radiographic occult scaphoid fracture, bone contusion, and associated soft tissue injury. Multislice CT and cone beam CT with its high spatial resolution and multiplanar two-dimensional reconstructions in three orthogonal imaging planes improve visualization and characterization of the fracture line and the amount of displacement and angulation of the fracture fragments or staging that is necessary for appropriate treatment (Taljanovic et al. 2012). Malunion, nonunion, and AVN of the proximal part of the scaphoid are associated to insufficient immobilized scaphoid fractures. Increased density of the proximal part of the scaphoid on radiographs (Fig. 23.9a) is a late sign of AVN; MRI shows demarcation line between normal bone of the distal half and bone marrow edema and fat replacement in the early phases with low SI on T1 (Fig. 23.9b) and increased SI on T2WI at the proximal half of the scaphoid; in very early phases, SI on T1WI and T2WI is normal; in these cases subtracted T1WI before and after IV gadolinium administration proves absent gadolinium enhancement in the necrotic part. Contrast-enhanced MRI aids in the assessment of scaphoid fracture nonunion, AVN, fracture healing after bone grafting, and revitalization of the necrotic bone after bone grafting. Stress fractures of the scaphoid have been reported to be due to repetitive loading of the wrist in dorsiflexion, occurring to sportsmen such as gymnasts and shot-putters (Hanks et al. 1989). These stress fractures are recognized late on radiographs related to endosteal spongious callus with bandlike increased bone density. On MRI they are early and easily demonstrated as a transverse low SI on T1- and T2-weighted coronal images of non-complete fracture line surrounded by major bone marrow edema. On MRI, the presence of edema without a visible fracture line may represent a bone bruise or a stress reaction recognized as forestage of stress fracture.
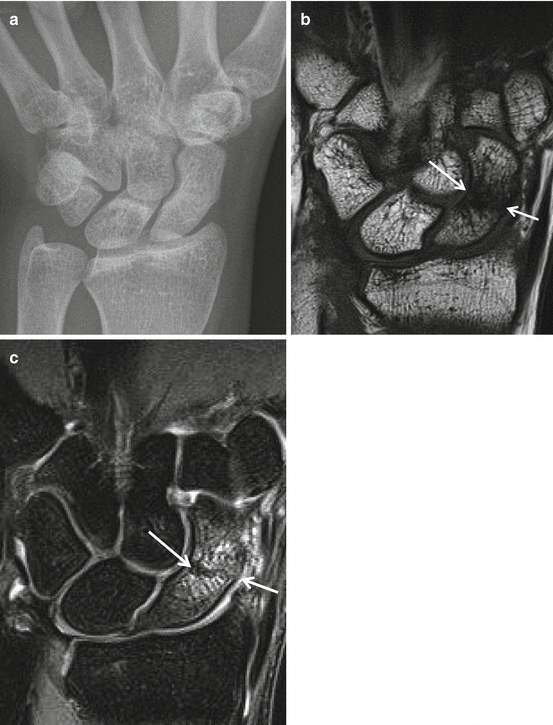
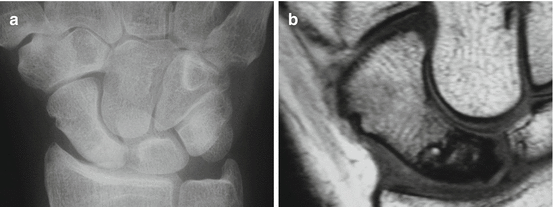

Fig. 23.8
Occult midportion scaphoid fracture. (a) Normal PA radiograph. (b) Coronal SE T1WI and C coronal TSE intermediate TE FS images demonstrating the cortical disruption (arrows) and fracture line surrounded with bone marrow edema with reduced SI on T1 (b) and increased SI on intermediate TE with FS (c)

Fig. 23.9
Midportion scaphoid fracture with AVN of the proximal half. (a) PA radiograph demonstrating relative increased density of the proximal half related to absence of osteopenia. (b) Coronal SE T1WI shows decreased SI at the proximal necrotic half of the scaphoid with sharp demarcation line with the vital distal half
23.4.2 Hamate Fractures
Hamate fractures are relatively common wrist fractures in athletes. They may be either isolated or in complex injury associated with carpometacarpal dislocation or pisiform fracture. They are commonly classified into hook or body of hamate fractures. A fractured hook of hamate is typically isolated and is the most common hamate fracture but less common compared to scaphoid fractures. This fracture is typically occult on radiographs and easily demonstrated on axial and sagittal multiplanar CT reconstructions or water-sensitive FS MRI sequences (Fig. 23.10). It occurs when a patient falls while clenching firm objects, and the object lands between the ground and ulnar side of the palm. Falling on an outstretched hand that impacts the ulnar side of the wrist may also result in fracture of the hamate hook. This injury occurs in individuals who are involved in a sport involving a racquet, club, or bat and is caused by the impact against the hook of the hamate. The fracture may also be through indirect force when a racquet is swung, when a golf club catches the ground, or when a bat hits a ball (Futami et al. 1993). There is some controversy as to whether these fractures result from shear forces transmitted through ligament insertions as the wrist is forcibly hyperextended while gripping an object. In racquet sports, fractures affect the dominant hand. In golf, hockey, and baseball, hamate fractures usually occur in the nondominant hand. Isolated fracture to the body of the hamate is less common and also often occults on radiographs. It is due to a direct force such as a punch-press injury, falling on a hyperdorsiflexed and ulnar-deviated wrist, or posterior dislocation or subluxation of the fourth and/or fifth metacarpal.
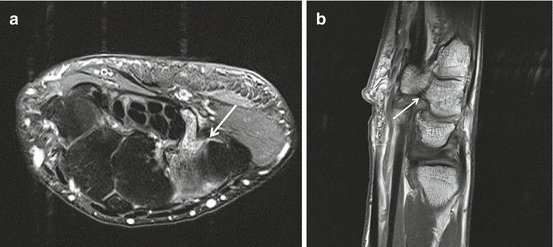

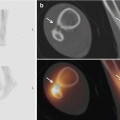
Fig. 23.10
MRI fracture hook of hamate. Axial TSE intermediate TE with FS (a) and sagittal TSE T1WI after intervenous gadolinium administration. Bone marrow edema surrounding the fracture (arrow) is well demonstrated on water-sensitive images (a). Fracture line (arrow) at the base of the hook of the hamate is demonstrated on T1WI (b)
23.4.3 Lunate Fractures
The lunate, being the fulcrum of the proximal carpal row, is frequently exposed to traumatic forces to the wrist. Kienbock’s disease, osteomalacia, or osteonecrosis of the lunate is thought to be due to repetitive microtrauma and is associated with ulna minus. Early radiological diagnosis of Kienbock’s disease is challenging as the lunate as a whole is involved, and thus the pathognomonic sign of demarcation line with double contrast that defines the necrotic bone on T2WI (well known in hip AVN) is not demonstrated. Relative homogeneous increased bone density of the lunate on radiographs (Fig. 23.23) and diffuse bone marrow edema on fluid-sensitive MRI sequences are rather late findings at a subacute stage (Fig. 23.11e) that is followed by collapse and secondary osteoarthritis. The absence of gadolinium enhancement in the very early stage of Kienbock’s disease is best demonstrated by subtracting pre- and post-IV gadolinium-enhanced T1WI (Fig. 23.11c, f). Acute lunate fractures are uncommon; body fractures of the lunate are caused by axial compressive force between the radius and capitate. When occurring through one of the horns, they are due to intrinsic SL or LT ligamentous avulsion. Lunate fractures are typically occult on radiographs and may be an incidental finding on US (Fig. 23.12a); additional imaging (CT or MRI) is indicated in clinical suspicion of lunate fractures (Fig. 23.12c, d, e).
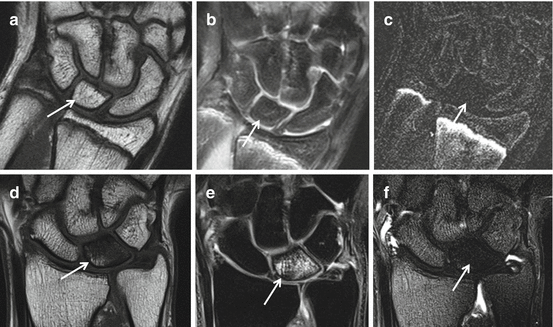
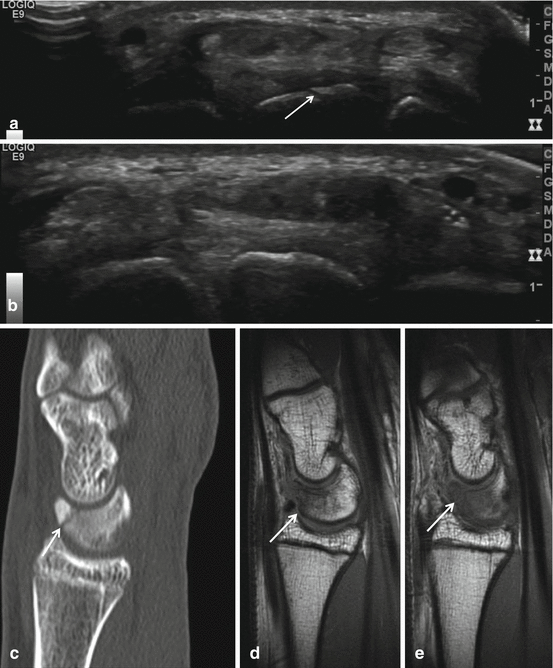

Fig. 23.11
MRI lunatomalacia, Kienbock’s disease, early and later findings. Early findings AVN of the right os lunatum, coronal images (a–c) of an adolescent patient. SE T1WI (a), TSE intermediary TE (b), and subtraction image (c) of T1WI before and after IV gadolinium administration. No abnormalities are detected on TSE and SE WI, normal fat signal and morphology of the os lunatum on T1WI (a), no bone marrow edema on water image (b). Absence of enhancement after gadolinium administration is best demonstrated on subtracted gadolinium-enhanced image (c). Subacute findings of AVN of the left os lunatum, images (d–f) of an adult patient. SE T1WI (d), TSE intermediary TE (e), and subtraction image (f) of T1WI before and after IV gadolinium administration. Wide spread reduced SI on T1WI (d) with diffuse BME on water image with FS (e) and absence of gadolinium enhancement (f)

Fig. 23.12
Occult left lunate fracture. Incidental finding on ultrasound (a, b) and confirmation on CT (c) and MRI (d, e). Seventeen-year-old elite male tennis player with tennis-related chronic pain at the dorsal aspect of the wrist. Fracture line at the dorsal aspect of the os lunatum is demonstrated on axial ultrasound of the left wrist (a arrow), not demonstrated at the right wrist (b). Sagittal multiplanar CT reconstruction with confirmation of the fracture at the dorsal distal surface of the lunate bone (c arrow), low SI on SE T1WI sagittal MRI images surrounding the fracture line (d, e arrows)
23.4.4 Other Fractures
A subcapital metacarpal five fracture is typically related to axial trauma on the clenched wrist in boxing sports. Fractures may also be caused by direct trauma, e.g., impact with a helmet during American football. Radiography is the primary imaging technique in these fractures. Additional imaging (MRI or CT) is indicated in suspicion for occult fracture or in fracture distention into the joint.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree