Fig. 35.1
(a) Radiograph showing an ankle effusion. (b) Ultrasound showing an ankle joint effusion
The conventional radiograph is still the main stay in initial trauma imaging. There are several classification methods: in common use are the Weber classification, the Lauge-Hansen classification and the AO system (Fig 35.2). These are of particular value in research projects. Some will use the classification to assist in determining the best treatment pathway. Their use and application depend on local practice.
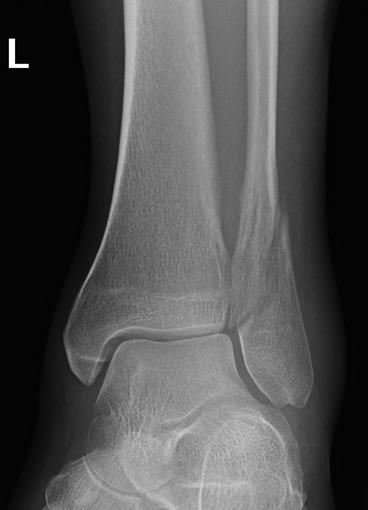

Fig. 35.2
A radiograph of a Weber type B ankle fracture
35.4.2 Ligament Tears
Ligaments may tear in their mid-substance or avulse from their bone insertions. Sometimes, a fragment of bone is pulled away with the ligament. The mildest type of injury is a sprain where some fibres are torn internally without complete separation. This may include cases where the ligament is stretched and not split.
Given the complex three-dimensional structure of some of the ligaments (spring and deltoid), the tears may be partial or complete. Rupture of part of a ligament is worse than a simple sprain where there is no macroscopic or imaging disruption of fibres.
It has been argued that less severe ligament injuries may lead to scar tissue and adhesion to adjacent structures and that the long-term symptoms exceed the apparent damage using imaging. This may be particularly important where tendon sheaths abut ligaments (e.g. medial and lateral tunnels). Ligament tears can be detected by ultrasound and MRI (Perrich et al. 2009; Peetrons et al. 2004) (Figs. 35.3 and 35.4). Neovascularisation may be seen at the site of ligament damage with Ultrasound.
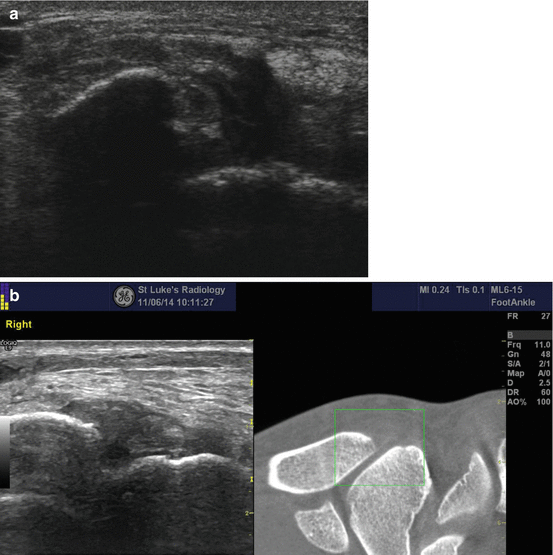
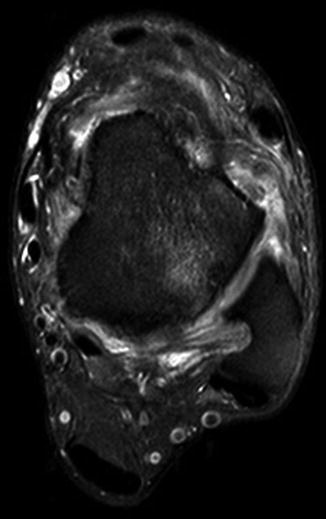

Fig. 35.3
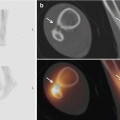
Anterior talofibular ligament rupture. (a) An ultrasound of a ruptured anterior talofibular ligament. There is discontinuity of the ligament fibres. (b) Cone-beam CT with ultrasound fusion imaging showing the anterior talofibular ligament tear on the ultrasound with a tiny periosteal lift of the distal fibula seen on the CT and ultrasound images

Fig. 35.4
An MRI of a ruptured anterior talofibular ligament. There is discontinuity of the ligament fibres and a gap where the ligament should be
35.4.3 Tendon Injuries
Tendons and their insertions are at risk from partial or complete rupture due to sudden overload in their direction of action. An outside force or excessive muscle contraction may be the cause. Chronic tendinopathy may increase the risk but age is also a major factor.
Dysfunction, pain and abnormal physical signs are important diagnostic features. However, the clinical signs may be misleading especially in patients with concomitant diseases such as arthropathy or adjacent fractures. On occasion, overlap of function of intact tendons may prevent adequate clinical examination. An intact plantaris muscle, which is a variant or vestigial structure, may mislead the examiner to consider a completely ruptured Achilles tendon to be intact.
Complete rupture normally leads to retraction of the tendon ends, sometimes by a considerable distance.
When a tendon tears, blood and fluid may fill the vacant tendon sheath. However, this fluid will resolve with time, and the empty tendon sheath or paratenon will fill the gap. Care should be taken not to confuse this with an intact tendon. Here, dynamic imaging is especially useful using both the patient’s efforts to move the limb and passive motion applied by the examiner. Ultrasound is therefore the best way of imaging as dynamic movement can be performed whilst imaging. With extended field-of-view imaging, the precise location of the tendon tear can be demonstrated in a manner that may be easier for the observer reviewing the images to appreciate (Fig 35.5).
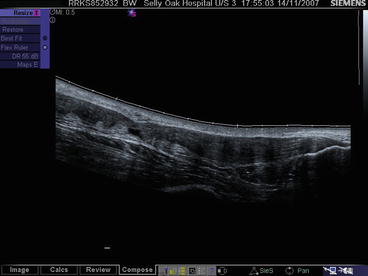

Fig. 35.5
Extended field-of-view ultrasound image of a complete Achilles tendon tear
In children, the tendons are strong, and the bone or enthesis are weaker. Avulsion injuries are more common. Epiphyseal plates are especially weak and tend to break before the tendon does. The role of imaging is to detect the avulsion and assess the size of the separated bone fragment. This will help when considering the efficacy and potential outcome of surgical reattachment.
35.5 Chronic Injuries
35.5.1 Stress Injuries
The bone remodels in response to load surprisingly quickly. In a matter of weeks, the bone and ligament or tendon insertions will strengthen whatever the age of the patient. This remodelling makes the bone fit for purpose and is why a skeleton gives clues to the lifestyle and activity of the person. Overload occurs when the bone is diseased or does not have time to respond to the load. Stress injuries result. In the first instance, the bone reacts with local oedema in the marrow and sometimes with an increased blood supply and a thin layer of oedema in the periosteum. If the load continues, trabeculae give way, and the microfractures start to repair. This gives more local bone oedema but also will show linear oedema and then sclerotic repair. This is best seen using MRI when the STIR sequence will show the bone stress response as high signal, and the fracture if present will be of low signal on a T1 SE sequence (Figs. 35.6 and 35.7). A break in the cortex with periosteal oedema can also be identified by ultrasound examination (Fig 35.8). Continued load leads to a true fracture that separates one and then both cortices.
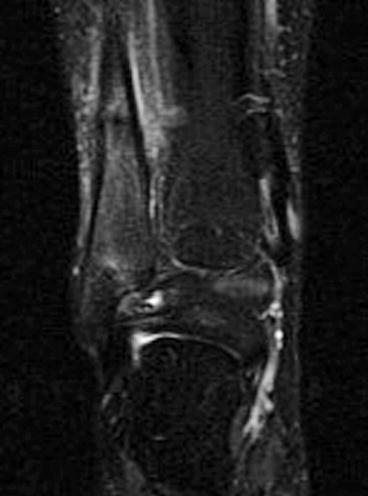
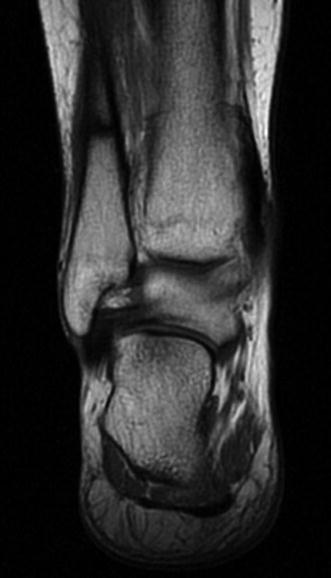
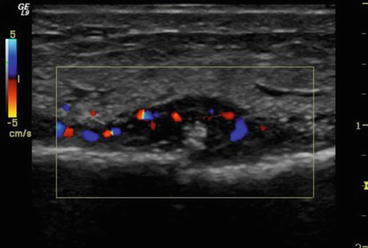

Fig. 35.6
MRI coronal STIR showing a stress fracture of the distal fibula

Fig. 35.7
MRI coronal T1SE showing a stress fracture of the distal fibula which has become a complete fracture

Fig. 35.8
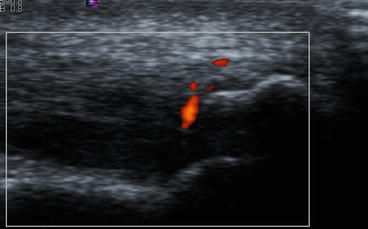
Ultrasound with colour Doppler showing a stress fracture of the distal fibula
35.5.2 Tendinopathy
Overuse of a tendon due to repetitive activity especially when this is unaccustomed may lead to tendinopathy. There is a degenerative element to this disorder that is more evident in older patients. Early signs are pain and dysfunction with tenderness and swelling. Symptoms will be exacerbated by the causative activity, but the worsening may be delayed by hours or even a day. Imaging will reveal fluid in the tendon sheaths in type II tendons, oedema in the paratenon and adjacent soft tissues in type I tendons with increased vascular supply. Continued overuse will lead to internal tendon degeneration and delamination. The tendon may thicken due to repetitive small injuries and fibrotic repair processes. Areas of fibrosis and calcification may become permanent features. When impingement of bony spurs or implanted metal is the cause, then rupture may ensue. The tendon will show fluid in the tendon sheath and mucoid degeneration. This is visible using both ultrasound and MRI. The ultrasound will also show neovascularisation which is a sign of tendon degeneration and also often correlates with the amount of pain the patient is experiencing (Reiter et al. 2004; Calleja and Connell 2010) (Figs 35.9 and 35.10).
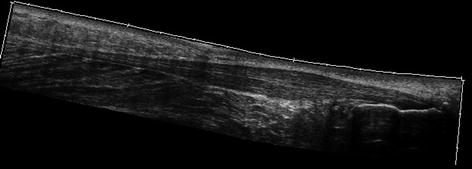
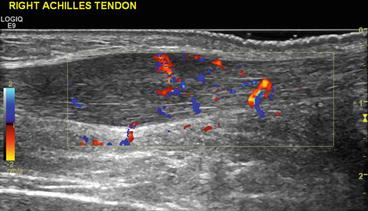

Fig. 35.9
Extended field-of-view of the Achilles tendon showing a fusiform swelling in keeping with chronic tendinosis

Fig. 35.10
Ultrasound with colour Doppler showing an Achilles tendinosis
35.5.3 Enthesiopathy
Enthesiopathy is a traction injury of the tendon insertion and adjacent bone due to repetitive load, the tendon thickens locally, and there will be neovascularisation in the tendon and adjacent tissues. There will be focal bone oedema and some soft tissue swelling also with increased local blood supply. The bony enthesis may distort due to minor partial avulsion and repair. The enthesis may enlarge with bony overgrowth as a result. This is often seen in distal insertion Achilles tendinosis but can sometimes also be associated with an underlying inflammatory arthropathy in the athlete (Fig 35.11). A common example in the ankle is plantar fascia insertion enthesiopathy; not strictly a tendon, but the signs are the same.